Fracture Neck Femur
520 likes | 2.15k Vues
Fracture Neck Femur. Dr.Sadeq Al-Mukhtar Consultant Orthopaedic Surgeon. Epidemiology. 97% occurs in patients more than 50 years old. The incidence increases with age.

Fracture Neck Femur
E N D
Presentation Transcript
Fracture Neck Femur Dr.Sadeq Al-Mukhtar Consultant Orthopaedic Surgeon
Epidemiology • 97% occurs in patients more than 50 years old. The incidence increases with age. • 3% occurs in under 50 years age(20-40) due to high energy trauma, sports, industrial & motor vehicle accidents. In 20-40 years most hip fractures are subtrochanteric or basi- cervical. Fractures in elderly are serious injuries, about 250,000 fractures per year in USA & the number is projected to double by the year 2050 & the cost exceeds 6 billion $ per year
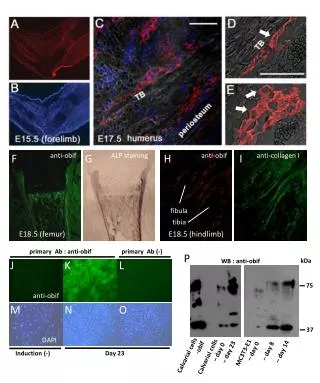
Anatomy • The femoral side of the hip is made of the femoral head with its articular cartilage & the femoral neck which connects the head to the shaft in the region of intertrochanteric area. The synovial membrane incorporates the entire head &the anterior neck but only the middle part of the neck posterior .The neck shaft angle is 130(+_7) degree. The Ante version is 10(+_7).
The diameter of femoral head ranges from 40-60 mm. The thickness of the articular cartilage ranges from 4mm in the apex to 1mm in the periphery. • Blood supply of the head from: • 1- Artery of ligamentum teres that usually originates from anterior obturator artery but it supplies only small area of the head near the attachment of the ligament.
2- Lateral, medial, anterior & posterior Capital vessels. • 3- Lateral, medial, anterior &posterior cervical vessels. • All these 2&3 vessels groups comes from intertrochanteric ring. • Accumulation of intracapsular hematoma interferes with the venous outflow &perhaps the vascular inflow. After 12 hours necrosis of the head starts.
Biomechanics • Falling from standing position leads to direct blow on the greater trochanter. Osteoporosis is the precipitating factor. • In young& middle aged high velocity trauma is needed to induce fracture. • Postmenopausal& senile osteoporosis predisposes to fracture .By the age of 65 years, 50% of women show bone mineral content below the threshold for fracture. By the age of 85 year this will reaches 100% • In elderly it can occur with minor trauma on an externally rotated thigh or the bone is so weak that powerful muscle contraction can lead to fracture.
Classifications • 1- Anatomical classification: • A- Intracapsular: • Subcapital (high risk) • Tran cervical (moderate risk) • Basal (less risk) intracapsular anteriorly, extra capsular posteriorly. • Sometimes, high energy fracture occur in young which involve the shaft of femur then to the base of the neck then to the sub capital area. Usually these are undisplaced.
B- Extra-capsular: • Inter-trochanteric fractures • Per-trochanteric • Notes:Intracapsular fractures carry poor prognosis because of poor blood supply which lead to avascular necrosis & non-union while extracapsular fractures carry good prognosis due to the good blood supply
2- Gardens classification: They are classified according to the degree of displacement of the fracture fragment. 1- Incomplete fracture(abduction& impacted) making the neck in valgus. 2- Complete fracture without displacement; the neck alignment looks normal. 3- Complete fractures with partial displacement. 4- Complete fractures with complete displacement.
1&2 are considered as undisplaced fractures& have good prognosis while 3&4 are displaced fracture& have poor prognosis. Stage 1 can slowly progress to stage 4 if untreated.
Pauwels classification: • They are classified according to the direction of the fracture: • Pauwel s 1: The angle from the horizontal line is 30-49 degree. • Pauwel s 2: The angle from the horizontal line is 50-69 degree . Pauwel s 3: The angle is 70& more.
All the available classifications can not determine the exact displacement that occurred at the time of accident, the degree of vascular damage & the condition of the posterior femoral neck.
Clinical features • Patient is usually old with history of trauma. The patient is unable to stand or walk. On examination the limb is shorter, externally rotated & he is unable to move it. Movement of the hip is tender &limited.
Diagnosis • It is achieved by history,Examination, & X-Ray of the hip, A.P& Lateral views are required. • Differential diagnosis: • Non-traumatic fractures of the neck of femur:- • Pathological fractures: Multiple myeloma, Secondary bone tumors.
Post-irradiation fractures. • Stress fractures: Hair-line fracture with no shortening or deformity.
Treatment • According to the treatment required, the complications likely to occur & the prognosis; patient are divided into three age groups; • Fractures in elderly; over 70 years. • Fractures in young & middle aged. • Fractures in children.
Each group has its own problems but there is one common factor to them ( the danger of injury to the retinacular vessels with end result of avascular necrosis). • This can sometimes be the cause of non-union whatever the method used for immobilization &even in cases where union has occurred late avascular necrosis. Changes in the weight bearing segment of the head can result in a stiff& painful joint .IT IS NOT WITHOUT REASON THAT THE INJURY HAS BEEN LABELLEDE THE UNSOLVED FRACTURE. • There must be rigid lines of demarcation, each fracture must be carefully& individually assessed.
The Aim of treatment • Accurate reduction. • Rigid fixation • Early mobilization to avoid complications.
Causes of avascular necrosis • Interference with blood supply of the head. • No periosteum( some believe there is very thin one) so only endosteal healing will occur resulting in poor callus. • Dissolution of the fracture hematoma by synovial fluid.
Treatment of patients above 70 years • Because of high incidence of AVN &non-union& complications of prolonged immobilization, the treatment is Arthroplasty. • Partial Arthroplasty: Using Austen Moore or Thompson's prosthesis. • Total hip replacement (THR): Indications includes delayed union &secondary osteoarthritis involve acetabulum.
Treatment of young &middle aged patients • Accurate reduction by:- • Closed reduction under anesthesia.or • Open reduction) • Rigid fixation by screws( at least 3 screws), using DHS(dynamic hip screws), or Smith-Petersons nail…..ect.
Treatment in Children • Some prefer conservative but the best method of fixation by multiple pins &immobilization by hip spica for 6 weeks &weight bearing after 8-12 weeks. • Notes: Even undisplaced fractures are not immune from complications like AVN.
Complications • General: • 1- DVT& Pulmonary embolism: It is due to prolonged immoblication, treated by prophylactic early mobilization, if happens give Anticoagulants. • 2- Bed sores: It is due to prolonged immobilization, bad nursing &pressure on the skin& bony prominence leading to necrosis that may be followed by infection. It is treated by prophylactic frequent turning of the patient, talk powder& pneumatic bedes. • 3- Pneumonia, chronic UTI. • 4- Psychological trauma..
Local complications • Avascular necrosis AVN: • Incidence is 10-30% ( 10% in undisplaced fractures, &30% in displaced fractures). It may be partial or complete with consequent collapse of the bone structure leading to fragmentation. It takes months or even 2-3 years to occur. If involved the fracture site it may lead to failure to union whereas collapse at the articular surface leads to O.A & the patient complains of hip pain & inability to walk X-Rays reveal increased bone density, collapse & later an O.A changes.
2- NON UNION • Causes are:- • 1- Interference with blood supply. • 2- Inadequate immobilization& early mobilization. • 3- Dissolution of the hematoma by synovial fluid. • Pathology of non-union: • When there is failure to unite, the fracture undergoes absorption& if it is associated with AVN the head will collapse.
Clinical features: Hip pain, lateral rotation of the limb& inability to walk with shortening. Treatment:- In young patient: If the head is viable to make the fracture line horizontal, the treatment is: Subtrochanteric valgus osteotomy. Rigid fixation &bone graft. In elderly, Arthroplasty. 3- Osteoarthritis.
Fractures of the Trochanteric region • These fractures occur in the region between the greater &lesser trochanters. They are common in elderly especially in women, more than the fracture of neck femur. • Compared to patients with fractured femoral neck, patients with intertrochanteric fractures are significantly older, more likely to be limited to home ambulation& more dependant in their activities of daily living: therefore they tend to have overall poorer prognosis .Because the region is a vascular area so we note blood supply is excessive & AVN is less than 1%.
Classification • 1- Stable fracture:-The the postero-medial buttress remains intact or minimally comminuted& therefore collapse of the fracture fragment is unlikely. • 2- Unstable fracture: The large segment of postero-medial wall is fractured free& comminuted& therefore tends to collapse in varus.
KYLE Classification • 1- Non-displaced stable fracture: without comminution (stable) 21% • 2- Minimal comminution but displaced fracture: once reduced become (stable) 36% • 3- Large postero-medial comminuted area .This is a problem fracture (unstable) 28% • 4- Intertrochanteric & subtrochanteric fracture: It is uncommon (unstable) 15%
Treatment • Types; • 1- Conservative; Traction for 6-8 weeks. • 2- Surgical; Because patients are elderly& complications of such fractures are high so surgery is indicated. • Principles:- • Reduction either closed under screen or open reduction. • Rigid fixation by pin& plate, DHS ,angled plate …etc.
Complications • General; The same as complications of fracture neck femur . • Local; • 1- Malunion; Varus deformity or external rotation which is treated by corrective osteotomy& fixation. • 2- Non-union; rare due to soft tissue interposition, treated by ORIF & bone graft.
Subtrochanteric fracture • These are fractures in the area between lesser trochanter & the junction between proximal and middle 3rd of femur. It occur in all age groups but there are two peak ages of incidence; • 1- Late adolescence & early adulthood; here high energy trauma is needed. • 2-Geriatric; minor trauma to bone lesion like metastatic tumor lung, breast cancer) causing pathological subtrochanteric fracture.
The upper fragment is flexed due to spasm of the iliopsoas& abducted by gluteal muscle while the distal segment is adducted by adductor muscles