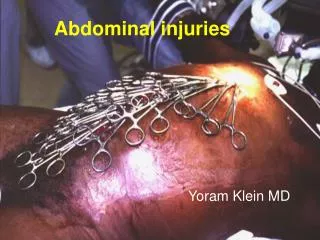
Abdominal injuries
Abdominal injuries. Types Diagnosis Treatment. Types of abd trauma. Blunt Direct blow Deceleration Penetrating: GSW Stab wounds Impalement Often thoracoabdominal. Diagnosis.

Abdominal injuries
E N D
Presentation Transcript
Abdominal injuries Types Diagnosis Treatment Klinika Chirurgii Urazowej Grala
Types of abd trauma • Blunt Direct blow Deceleration • Penetrating: GSW Stab wounds Impalement Often thoracoabdominal Klinika Chirurgii Urazowej Grala
Diagnosis • Determine the presence of abd injury (history, physical examination, USG, CT, DPL, X-ray) – serial examinations indicated • Altered consciousness → major confounding factor for PE • PE: seat belt sign (ecchymotic area at the lower abd. wall – bladder and bowel perforation, L distraction [chance] fr.), Cullen`s sign (periumbilical ecchymosis indicative of intraperitoneal hemorrhage), Grey Turner sign (flank ecchymoses indicative of retroperitoneal hemorrhage) • Indications for laparotomy: is it the cause of hypotension? is peritonitis present? • Posible nonoperative treatment of diagnosed intraabdominal injuries Klinika Chirurgii Urazowej Grala
Diagnosic peritoneal lavage – DPL • Open and blunt technique: decompress UB and stomach gross blood laparotomy 1l warmed normal saline gentle agitation of abd. wait 10min. drain fluid macroscopic evaluation ev. lab testing (positive > 100th RBC/mm3, 500 WBCs/mm3) • Interpretation in context of clinical condition (positive DPL does not mandate laparotomy in stable patient) • In pelvic fractures supraumbilical entry, safe distance from postoperative scars • Complications: false positive, bowel perforation, UB perforation, haemorrhage, wound infection • Contraindications: advanced pregnancy, clotting disorders, obvious indications to laparotomy, planned FAST Klinika Chirurgii Urazowej Grala
ER US Klinika Chirurgii Urazowej Grala
FAST - Focused Assesement with Sonography for Trauma • Limited ultrasound examination directed solely at identifying the presence of free intraperitoneal or pericardial fluid • In the context of traumatic injury, free fluid is usually due to haemorrhage and contributes to the assessment of the circulation Klinika Chirurgii Urazowej Grala
FAST - Focused Assesement with Sonography for Trauma • Perihepatic & hepato-renal space • Perisplenic • Pelvis • Pericardium • Pleural space Klinika Chirurgii Urazowej Grala
FAST - Focused Assesement with Sonography for Trauma • haemodynamic instability and free intra-peritoneal fluid mandates a laparotomy for intra-abdominal haemorrhage. • in the presence of haemorrhagic shock but a negative FAST examination, other sites of haemorrhage must be sought and controlled thoracic haemorrhage may require thoracotomy, pelvic haemorrhage angiographic embolisation; retroperitoneal haemorrhage from vascular injury remains a possibility with a negative FAST. • serial FAST examinations may be required. • positive examination relies on the presence of free intraperitoneal fluid, detects a minimum of 200 mL of fluid; injuries not associated with hemoperitoneum may be missed (not reliable for excluding hollow visceral injury). • cannot be used to reliably grade solid organ injuries - detection of solid organ injury with FAST - 41% (consider CE US). • (in the hemodynamically stable patient a follow-up CT scan should be obtained if nonoperative management is contemplated). more cost-effective when compared with DPL or CT. Klinika Chirurgii Urazowej Grala
Abd CT Klinika Chirurgii Urazowej Grala
Abd. CT • recommended for the evaluation of hemodynamically stable patients with: equivocal findings on PE associated neurologic injury multiple extra-abdominal injuries • under these circumstances, patients with a negative CT scan should be admitted for observation • is the diagnostic modality of choice for nonoperative management of solid visceral injuries • in hemodynamically stable patients, DPL and CT scanning are complementary diagnostic modalities • notoriously inadequate for the diagnosis of mesenteric injuries and hollow visceral injuries (DPL is a more appropriate test) • unique ability to detect clinically unsuspected injuries and ability to evaluate the retroperitoneal structures • requires a cooperative, hemodynamically stable patient that must be transported out of the trauma resuscitation area to the radiographic suite, need for specialized technicians and the availability of a radiologist for interpretation Klinika Chirurgii Urazowej Grala
CT 2006 • One abdominal CT is the equivalent of 500 chest x-rays and will increase the lifetime risk for cancer by 1 in 2000. • Oral contrast is not helpful in liver or spleen injuries, with free fluid or bony injuries. • Oral contrast is not helpful in detecting hollow viscus injuries or duodenal injuries. Instead, adds costs, time delay, and the risk for aspiration. • Additional intangible costs include the risks associated with contrast, electrolytes to check for renal function, longer time in the ED (although CT scanning does save time in complete spinal evaluations), and the cost of working up incidental findings which may in turn lead to more radiation exposure. Klinika Chirurgii Urazowej Grala
Special diagnostic studies Category USCTDPL • Rapid ++ + • Portable ++ + • Non-invasive ++ + • Integration in resuscitation ++ + • Sensitivity + ++ • Specificity + ++ • Quantitative + ++ + • Injury localisation + ++ • Evaluation of retroperitoneum+ ++ • Evaluation of pericardium ++ + • Ease of interpretation + ++ • Ease of repetition ++ + • Radiation exposure ++ ++ • Patient acceptance ++ + • Cost ++ + Klinika Chirurgii Urazowej Grala
Indications for laparotomy • BAT with positive DPL, US, CT • BAT with recurrent hypotension despite adequate resuscitation • Peritonitis • PAT with hypotension, or violation of peritoneum esp. in patients with altered consciousness • PAT with bleeding from the rectum, GU tract or stomach • GSW (except selected flank wounds) • Evisceration • On X-ray: retroperitoneal free air, diaphragmatic inj. Be overaggressive Klinika Chirurgii Urazowej Grala
Diaphragmatic injuries • Difficult to estabilish the diagnosis (CT, DPL, US, chest Xray – miss 30%) Pysical exam: false neg result in 20-45% Explorative laparotomy Explorative thoracoscopy? • Poor healing (chronic hernias): constant motion, relative thinness, pressure gradient (intrathoracic transposition of abd viscera) • Potentially catastrophic consequences (usual delay up to 8 years): strangulation of abd viscera through the defect (20-50% mortality rate) • Usually posterolateral left diaphragm • Chest X-ray: elevation, blurring, hemothorax, abn. gas shadow obscuring the diaphragm Klinika Chirurgii Urazowej Grala
Rupture of the left diaphragm Klinika Chirurgii Urazowej Grala
Rupture of the right diaphragm Klinika Chirurgii Urazowej Grala
Spleen • Receives 5% of cardiac output (splenic a., short gastric aa.) • Accesory s. (between stomach and pancreas) 20% • Functions: removal of aged and deformed RBCs, platelet storage, phagocytosis of bacteria (25% of bodys fixed tissue macrophages), production of IgM (main source) and IgG, opsonins (tuftsin, properdin) • Postsplenectomy complications: atelectasis (drainage, pulmonary toilet), thrombocytosis (up to 3mill, aspirin above 1), granulocytosis, subphrenic abscess, pancreatitis, pancreatic fistula, gastric perforation • OPSI – lifetime risk, majority within first 2ys (flulike symptoms rapidly progressing to fulminant sepsis with consumptive coagulopathy and death within 12-48h) mortality 50-60% encapsulated bacteria (Str. pneum.,Neisseria mening.,H.infl.) are causative – post op. immunization loss of splenic reticuloendothelial cells (clear particulate antigen in the absence of antibody), opsonin synthesis, decrease in lymphocyte T4-T8 ratio → limited responce to infection supportive management, high dose 3rd gen. cephalosporins Klinika Chirurgii Urazowej Grala
Splenic injury CT Klinika Chirurgii Urazowej Grala
Mesh splenorrhaphy Klinika Chirurgii Urazowej Grala
Splenic laceration Klinika Chirurgii Urazowej Grala
Liver trauma • Most commonly injured organ (possible massive haemorrhage) • Initial hemostasis: mobilisation, bimanual compression, Pringle maneuver (oclusion time<45min.) → no↓ → retrohepatic v. cava or hepatic v. inj. → atriocaval shunt (Schrock shunt), Folley catheter, perihepatic packing • Definitive hemostasis: electocautery, parenchymal sutures (horisontal mattress stitches), hepatotomy with selective ligation (finger fracture technique), topical hemostatic agents, omental packing, resectional debridement, hepatic artery ligation • Damage control • Drainage • Blunt trauma: nonoperative approach (observation, selective embolisation). Klinika Chirurgii Urazowej Grala
Posttraumatic biloma Klinika Chirurgii Urazowej Grala
Liver GSW Klinika Chirurgii Urazowej Grala
Mesh hepatorraphy Klinika Chirurgii Urazowej Grala
Femoro-caval (cavo-caval) shunting Klinika Chirurgii Urazowej Grala
Duodenum • Usually unrestrained driver-frontal impact, direct blow (eg.bike handlebars) • Bloody gastic aspirate, retroperitoneal air, leftward scoliosis and blurring of psoas schadow on X-ray, contrast CT • Slow evolution of abd symptoms: back or flank pain • Laparotomy • Kocher maneuver, transverse, double layer closure • Whipple procedure in d. devascularisation with complex bile duct and pancreatic head injury (high complication rate) Klinika Chirurgii Urazowej Grala
Duodenal rupture (750cc blood in ng tube,>50% circumferential tear) Klinika Chirurgii Urazowej Grala
Duodenal acces, incision of the lig. of Treitz Klinika Chirurgii Urazowej Grala
Pancreas • In 0.2% of BAT - direct epigastric blow (compression against VC) and 1.1% of PAT. Penetrating pancreatic injury is usually diagnosed at laparotomy and carries a high mortality because of associated injuries of neighboring major blood vessels. Blunt pancreatic injury is complicated by difficulty in establishing the diagnosis, which can lead to delay in diagnosis and increased morbidity. • Serum amylase levels nondiagnostic • DPL, US, CT often nondiagnostic • ERCP • Celiotomy – associated stomach and liver involvement, Kocher maneuver and gastrocolic and gastrohepatic ligament dissection • Determine presence of ductal injury: L to s. mesenteric vessels → distal pancreatectomy with splenctomy, R → closure of proximal end + distal drainage (Roux-en-Y pancreaticojejunostomy • Extensive injury to the head of pancreas, duodenum, biliary tree → pancreaticoduodenectomy (Whipple procedure) • Parenchymal lesions → drainage Klinika Chirurgii Urazowej Grala
Pancreatic injury BAT CT Klinika Chirurgii Urazowej Grala
Acces to the pancreas Klinika Chirurgii Urazowej Grala
Small bowel • Seat belts, direct blow or penetrating trauma • Minimal bleeding • Peritoneal signs (intoxicated or deeply unconsious patients – absent) • US, CT nondiagnostic • Diagnosis - DPL and laparotomy • Primary repair or segmental resection and anastomosis, close mesenteric defects Klinika Chirurgii Urazowej Grala
Blunt bowel injury Klinika Chirurgii Urazowej Grala
Blunt bowel injury Klinika Chirurgii Urazowej Grala
Large bowel injuriesNo physicalfindings or imaging modalities, no clinically useful combinationof findings that would reliably predict colonic injury. • Colon • Usually penetrating trauma • Diagnosis at laparotomy (although BCI is rare, it ranks 4th among injuries found at laparotomy in BAT and is an independent predictor of hospital and ICU LOS). • Debridement, drainage, wide spectrum antibiotic + : primary 2 layer closure, excision, diverting colostomy and Hartmann`s pouch considered in long operative delay, severe fecal contamination, large transfusion requirements (>4U), prolonged shock, high velocity GSW • Rectum • Historic 3Ds: distal rectal washout, diverting colostomy, presacral drainage – battlefield injuries • Civilian trauma: primary repair, colostomy Klinika Chirurgii Urazowej Grala
RPH • Penetrating trauma – require exploration (uncontained) temoporary control: packing, cross clamping of supraceliac aorta gain acces: division of gastrohepatic lig., L medial visceral rotation (Mattox maneuver), R visceral rotation (Catell maneuver) with Kocher maneuver direct repair, rarely grafting • Blunt trauma – CT, US or laparotomy for diagnosis management determined by location and stability Z I RPH (supramesocolic) – Mattox m. Z II RPH (flank) – unless pulsatile, expanding or ruptured do not explore Z III RPH (pelvic) – as above, packing or angiographic embolisation if required Klinika Chirurgii Urazowej Grala
Cattel maneuver Klinika Chirurgii Urazowej Grala
Mattox maneuver Klinika Chirurgii Urazowej Grala