Inpatient Asthma
470 likes | 1.07k Vues
Inpatient Asthma. Sangeeta Schroeder, MD Resident Noon Conference. Epidemiology. According to the American Lung Association (2006) Just about 7 million children have diagnosed asthma 3 rd leading cause of childhood hospitalization

Inpatient Asthma
E N D
Presentation Transcript
Inpatient Asthma Sangeeta Schroeder, MD Resident Noon Conference
Epidemiology • According to the American Lung Association (2006) • Just about 7 million children have diagnosed asthma • 3rd leading cause of childhood hospitalization • One of the most common causes of missed school days (about 13 million missed days/year)
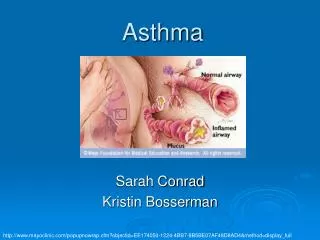
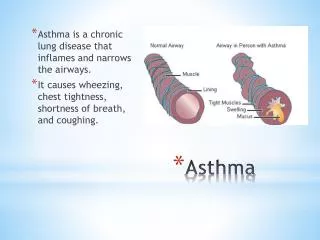
Clinical Features • Shortness of breath • Wheezing • Symptomatic with viral infections, allergens or exercise • Colds that last >10 days • Frequent night-time coughing
Common Triggers • Allergens • Dust, mold, pollen, cats, dogs, etc • Non-Allergens • Cigarette smoke/Smoke • Infections • Exercise • Temp Change • Stress
Initial Assessment • Respiratory Rate • Pulse Ox • Retractions • Dyspnea • Auscultation
LPCH Asthma Scoring Tool: Add Total Points to Give Pediatric Asthma Score (PAS)
Pediatric Asthma Score • Add the Score for the 5 categories together • Mild: PAS < 6 • Mild to Moderate: PAS of 7 or 8 • Moderate to Severe: PAS of 9 or 10 • Severe: PAS > 11
Initial Management • Oxygen • Albuterol • Atrovent • Systemic Steriods • Magnesium Sulfate?
Initial Management • Oxygen
Initial Management - Albuterol • Assessment Q Hour • A. If PAS has not improved by >2, or if it is not <6, REPEAT phase 1 according to current PAS score • B. If PAS has improved by >2,OR PAS <6, ADVANCE to Phase II • C. If PAS has worsened by >2, OR PAS >11, INTENSIFY
Initial Management • Atrovent • Found to decrease rate of admissions • Only if given at least 2 doses • Should be part of phase 1 treatment
Initial Management • Systemic Steroids • Decadron • Can give in office/ER for mild asthma • 0.6mg/kg x1 dose IM/IV/PO • Prednisolone • 1mg/kg/dose BID • NEW GUIDELINES: MAX 60MG/DAY!!!! • Solumedrol • Use only if worried about respiratory distress/aspiration
Initial Management • Magnesium Sulfate • 25-75 mg/kg/dose • Usually give 50mg/kg/dose • Give over 10-20 minutes!
When to Admit? • Oxygen requirement • After Phase 1 with Atrovent • Child is still in resp distress • Needs repeat albuterol dose within 4 hours • Poor PO intake • Poor Follow-up
Continued Management • Albuterol • Systemic Steriods • Inhaled Corticosteroids • Asthma Education
Albuterol • Repeat Phase 1 if child just got admitted • Exception: • If PAS is 1 or 2 on admit, start at Phase 2
Systemic Steroids • Continue for 3-10 days • Mild (no admission): 3 days • Most Admissions: 5 days • If still in hospital on day 4 or 5: 10 days • If use 60mg/day as MAX, no need to taper
Atrovent • Has not been shown to decrease morbidity of admission • Has not been shown to decrease likelihood of PICU transfer • Has not been shown to decrease LOS • NOT USED ON THE FLOOR
Inhaled Corticosteroids • Start inpatient for education • Flovent/QVAR • MDI’s • Pulmicort • Neb • Ensure child uses with mask that does not have holes on top • Risk of Corneal Ulceration
Asthma Education • Review differences btwn preventive and relief meds • Demonstrate and teach proper MDI with Spacer/mask use • Educate on asthma signs and symptoms • Review Home Management Plan of Care
Spacers • All patients with asthma • Holds the “puff” in the chamber
Spacer Use • Insert the MDI into the back end of the spacer • SHAKE BEFORE EACH USE • Use a spacer with mask in a young child
Spacer Use • FIRST: Exhale • SECOND: Create a seal with your mouth and the mouthpiece • THIRD: Inhale slowly as you push the inhaler and hold breath for 10 seconds • FOURTH: Breathe out slowly
Spacer Use - Child • FIRST: Exhale • SECOND: Create a seal with your mouth and the mouthpiece • THIRD: Push the inhaler and keep the seal with the mouthpiece for 8-10 breaths • FOURTH: Breathe out slowly
Spacer Use – Infant/Toddler • FIRST: Use a spacer with mask • SECOND: Create a seal with the infant’s mouth and the mask • THIRD: Push the inhaler and keep the seal with the mask for 8-10 breaths
MDI/Spacer Use • Make sure to repeat all the steps for each puff: Including shaking the inhaler!!!
Discharge Guidelines • Albuterol • System Steriods • ICS • F/U Appointment • Subspecialty Follow-up?
Discharge Guidelines • Albuterol • 4-6 puffs 4 times a day for 1 week • Then per HMPC • Systemic Steroids • 3-10 day course at 60 mg/day max • No need to taper the dose • ICS • Everyday for at least 1 year
Discharge Management • Follow-up Appointment • 1-2 days after hospital discharge • Subspecialty Follow-up? • Max doses of ICS • More than 1 controller • Strong Allergic Component • PCP is not comfortable with asthma • Parents are not comfortable with PCP
Home Management Plan of Care • AKA: Asthma Action Plan • New 4 tier system • Emphasizes home asthma care • Gives consent to school/daycare to administer albuterol
HMPC • Joint Commission Requirement • All fields need to be filled out • Triggers/avoidance • All 4 tiers • Follow-up Appointment • Date/Time and PMD OR • Time frame, PMD Name and Phone Number • Parent’s Signature • Discharging Attending Signature
HMPC • Joint Commission Rates • Quarter 2 of 2009: 64% Compliance • 6/25 patients did not have an action plan in the chart • REMEMBER TO KEEP THE SIGNED COPY IN THE CHART!!! • 3/25 patients had incomplete fields