Female Reproductive System
760 likes | 771 Vues
Explore the anatomy and functions of the female reproductive system, from oogenesis to childbirth to breast health, along with details on puberty and menopause. Learn about the organs, processes, and hormonal changes that govern this vital system.

Female Reproductive System
E N D
Presentation Transcript
Female Reproductive System • Reproductive Anatomy • Puberty and Menopause • Oogenesis and the Sexual Cycle • Female Sexual Response • Pregnancy and Childbirth • Lactation 28-
Female Reproductive System • Produce and deliver gametes • Provide nutrition and room for fetal development • Give birth • Nourish infant 28-
Sex Differentiation • Male and female are indistinguishable for first 8 to 10 weeks of development • Female develops • no testosterone or müllerian-inhibiting factor • causes degeneration of (male) mesonephric duct • paramesonephric duct • develops into uterine tubes, uterus and vagina • genital tubercle becomes clitoris • urogenital folds develop into labia minora • labioscrotal folds into labia majora 28-
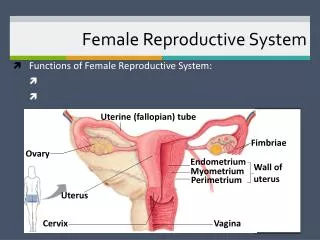
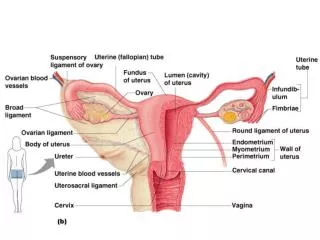
Ovary • Produces eggs and hormones • almond-shaped, 3 cm x 1.5 cm x 1 cm • tunica albuginea capsule like on testes • cortex produces gametes; medulla holds vessels • Each egg develops in its own fluid-filled follicle and is released by ovulation • Ligaments • attached to uterus by ovarian ligament • attached to pelvic wall by suspensory ligament • contains ovarian artery, vein and nerves • anchored to broad ligament by mesovarium 28-
Anatomy of Ovary 28-
Secondary Sex Organs • Internal genitalia • duct system of uterine tubes, uterus, vagina • External genitalia • clitoris, labia minora, and labia majora • occupy perineum • accessory glands beneath skin provide lubrication 28-
Uterine (Fallopian) Tubes • 10 cm long, muscular tube lined with ciliated cells • Major portions • narrow isthmus near uterus • body (ampulla): middle portion • flares distally into infundibulum with fimbriae • Enclosed in superior margin of broad ligament (mesosalpinx) 28-
Uterus • Thick-walled, pear-shaped muscular chamber that opens into vagina and tilts forward over urinary bladder • internal and external os of cervical canal • openings into uterine tubes in two upper corners • Domed fundus above body of organ 28-
Histology of Uterine Wall • Perimetrium - external serosa layer • Myometrium - middle muscular layer • 1.25 cm thick in nonpregnant uterus • smooth muscle • produces labor contractions, expels fetus • Endometrium • simple columnar epithelium with thick layer compound tubular glands • stratum functionalis – superficial, shed each period • stratum basalis - deep layer, regenerates a new stratum functionalis with each menstrual cycle 28-
Vessels of Reproductive Tract Hormonal changes cause spiral artery vasoconstriction, necrosis of stratum functionalis and menstrual flow 28-
Vagina • 8-10 cm distensible muscular tube • allows for discharge of menstrual fluid, receipt of penis, semen and birth of baby • Outer adventitia, middle muscularis and inner mucosa • Epithelium • child - simple cuboidal • puberty - estrogens transform to stratified squamous • bacteria ferment glycogen rich cells producing acidic pH • Tilted posteriorly between rectum and urethra • urethra embedded in its anterior wall 28-
Vulva (Pudendum) • Mons pubis - mound of fat over pubic symphysis; covered by pubic hair • Labia majora - thick folds of skin • Labia minora - medial, thin hairless folds • form vestibule contains urethral and vaginal openings • form hoodlike prepuce over clitoris • Clitoris - erectile, sensory organ • Vestibular bulbs - erectile tissue around vagina • Greater and lesser vestibular and paraurethral glands open into vestibule for lubrication 28-
Breasts • Overlies pectoralis major • conical body, nipple at apex • axillary tail contains many lymphatic vessels • Nipple surrounded by areola • dermal blood vessels closer to surface • melanocytes darken during pregnancy • smooth muscle contracts wrinkling skin and erecting nipple in response to cold, touch and arousal • Suspensory ligaments from skin, muscle • Nonlactating breast has little glandular tissue 28-
Breast Cancer • 1 out of 8 American women • Tumors begin with cells from mammary ducts • may metastasize by lymphatics • Symptoms may include palpable lump, skin puckering, skin texture and drainage from nipple • Most breast cancer is nonhereditary • some stimulated by estrogen • Risk factors include • aging, ionizing radiation, carcinogenic chemicals, alcohol, smoking and fat intake • 70% lack risk factors 28-
Puberty • Begins at age 9-10 (US) • Triggered by rising levels of GnRH • stimulates anterior lobe of pituitary to produce • follicle-stimulating hormone (FSH) • luteinizing hormone (LH) • Follicles develop and begin to secrete estrogen and progesterone 28-
Puberty • Thelarche - development of breasts • Pubarche - growth of pubic and axillary hair; apocrine and sebaceous glands • Menarche - first menstrual period • requires at least 17% body fat in teenager, 22% in adult • leptin stimulates gonadotropin secretion • improved nutrition (↑ body fat) has lowered avg. age of onset to 12 • Female hormones secreted cyclically and in sequence 28-
Climacteric • Midlife change in hormone secretion • due to age related depletion of follicles • occurs with menopause (cessation of menstruation); average age of 52 • Results • atrophy of uterus, vagina and breasts • skin becomes thinner, bone mass declines, and risks of cardiovascular disease increase • hot flashes (sudden dilation of cutaneous arteries) occur several times a day • HRT = hormone replacement therapy 28-
Oogensis and Sexual Cycle • Reproductive cycle - events occurring between fertilization and birth • Sexual cycle - events recurring every month when pregnancy does not occur • ovarian cycle = events in ovaries • menstrual cycle = parallel changes in uterus 28-
Oogenesis • Monthly event produces haploid egg by meiosis • Embryonic development of ovary • female germ cells arise from yolk sac • differentiate into oogonia, multiply • transform into primary oocytes - early meiosis I • most degenerate (atresia) by childhood • by puberty 400,000 oocytes remain • FSH stimulates completion of meiosis I, produces secondary oocyte and 1st polar body • proceeds to meiosis II and ceases until fertilization • after fertilization , releases 2nd polar body 28-
Sexual Cycle • Averages 28 days, ranges from 20 to 45 • Hormone cycle: hierarchy of control • hypothalamus→ pituitary → ovaries → uterus • Follicular phase (2 weeks) • menstruation occurs during first 3 to 5 days of cycle • uterus replaces lost endometrium and follicles grow • Luteal phase (2 weeks) • corpus luteum stimulates endometrial thickening • endometrium lost without pregnancy 28-
Ovarian Cycle - Follicular Phase • Menstruation (day 1) to ovulation(14) (variable) • Difficult to predict date of ovulation • Contains menstrual and preovulatory phases 28-
Ovarian Cycle - Preantral Phase • Discharge of menstrual fluid (days 1-5) • Before follicle develops antrum • primordial and primary follicles 28-
Ovarian Cycle - Antral Phase • Day 6 to 14, one dominant follicle advances to mature (graafian) follicle; secretes estrogen 28-
Ovarian Cycle - Ovulation • Mature follicle ruptures, releases oocyte influenced by LH 28-
Ovarian Cycle - Luteal Phase • Corpus luteum - forms from ruptured follicle, under influence of LH; secretes progesterone 28-
Menstrual Cycle - Proliferative Phase • Day 6-14 rebuild endometrial tissue • mitosis occurs in stratum basalis • result of estrogen from developing follicles 28-
Menstrual Cycle - Secretory Phase • Further thickening of endometrium due to secretion and fluid accumulation -- not mitosis • Due to progesterone stimulation of glands 28-
Menstrual Cycle Premenstrual Phase • Involution of corpus luteum, progesterone falls • spiral arteries constrict causes endometrial ischemia • stratum functionalis sloughs 28-
Menstrual Cycle - Menstrual Phase • Blood, serous fluid and endometrial tissue are discharged 28-
Pregnancy and Childbirth • Gestation (pregnancy) • lasts an average of 266 days from conception to childbirth • gestational calendar measured from first day of the woman’s last menstrual period (LMP) • Birth predicted 280 days from LMP • 3 three month intervals called trimesters 28-
Prenatal Development • Age based terminology • blastocyst is less than 2 weeks old • embryo is from 2 to 8 weeks old • fetus is 9 weeks to birth • neonate - newborn to 6 weeks 28-
Hormones of Pregnancy • HCG (human chorionic gonadotropin) • secreted by trophoblast within 9 days of conception • prevents involution of corpus luteum • Estrogens • increases to 30 times normal before birth • corpus luteum is source for first 12 weeks until placenta takes over • causes uterine, mammary duct and breast enlargement 28-
Hormones of Pregnancy • Progesterone • secreted by placenta and corpus luteum • suppresses secretion of FSH and LH preventing follicular development • prevents menstruation, thickens endometrium • stimulates development of acini in breast • HCS (human chorionic somatomammotropin) • secreted from placenta in direct proportion to its size • ↓ mother’s glucose usage and ↑ release of fatty acids 28-
Hormones of Pregnancy • Aldosterone secretion rises • fluid retention ↑ mother’s blood volume • Endocrine organs • thyroid gland increases 50% in size • ↑ BMR of mother • parathyroid glands enlarge • stimulate osteoclasts to release additional calcium from mother’s bones 28-