Type 1 Diabetes
Type 1 Diabetes. Karen S. Penko, MD Fellow, Pediatric Endocrinology September 2005. PREP Content Specifications. Recognize signs/symptoms Know how to treat type 1 diabetes Know the value of hemoglobin A1c Know the natural history Counsel patients on self-management


Type 1 Diabetes
E N D
Presentation Transcript
Type 1 Diabetes Karen S. Penko, MD Fellow, Pediatric Endocrinology September 2005
PREP Content Specifications • Recognize signs/symptoms • Know how to treat type 1 diabetes • Know the value of hemoglobin A1c • Know the natural history • Counsel patients on self-management • Differentiate Somogyi & dawn phenomena
PREP Content Specifications • Know how to manage sick days • Know the long-term complications • Know importance of blood glucose control in preventing long-term complications • Recognize the association with other autoimmune disorders
Gary Hall Jr. Olympic swimming medalist Type 1 diabetes
Case 1 • 18 y/o white male, father pages on-call peds endo: • Polyuria, polydipsia x 1 week • 16 y/o brother has type 1 diabetes • Using brother’s supplies, BG “high”, large urine ketones • What should we do? • Leaving for college next week
Serum glucose Venous pH Bicarb UA Serum acetone Electrolytes 497 mg/dl 7.396 27 mmol/l 150 mg/dl ketones, + glucose Negative Na 133, K 4.2, Cl 94, BUN 14, creat 0.8 At WRAMC ED
Diagnostic Criteria • Symptoms of diabetes and a casual plasma glucose 200 mg/dl, OR • Fasting plasma glucose 126 mg/dl, OR • 2-hour plasma glucose 200 mg/dl during an oral glucose tolerance test. • In the absence of unequivocal hyperglycemia, these criteria should be confirmed by repeat testing on a different day.
Presenting Signs/Symptoms • Polyuria, Polydipsia • Nocternal enuresis • Polyphagia • Weight loss • Fatigue, weakness • Blurry vision • Ketoacidosis: abdominal pain, nausea, vomiting, mental status changes
Epidemiology • Prevalence 1:300 • Peak age of diagnosis: 11-13 y/o • Risk for sibling: 6% • Risk for monozygotic twin: 50% • Risk for offspring: 2-10%, higher side if father has diabetes • Highest incidence: Finland, Sardinia
Pathophysiology • Autoimmune destruction of pancreatic -cell • Antibodies: • Islet cell • Insulin • Anti-glutamic acid decarboxylase 65 • T-cell mediated • Lymphocytic infiltration
Pathophysiology • Genetic susceptibility • Association with HLA DR3/4, DQ 2/8 alleles • Environmental triggers • Viruses: congenital rubella, coxsackievirus, enterovirus, mumps • Early exposure to cow’s milk
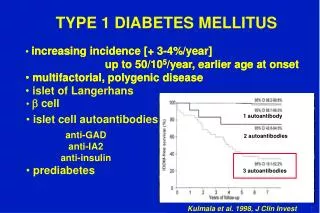
Progression to Type 1 DM Autoimmune markers (ICA, IAA, GAD) Autoimmune destruction Islet Cell Mass Honeymoon 100% Islet loss “Diabetes threshold”
Associated Autoimmune Disorders • Thyroid (Hashimoto’s, Graves’): 5-10% • Celiac Disease: 6% • Addison’s disease: <1%
Nicole Johnson Miss America 1999 Type 1 diabetes
Management • Diabetes team • Insulin • Diet • Exercise • Psychological support
Banting and Best 1923 Nobel Prize for discovery and use of insulin in the treatment of IDDM
The Miracle of Insulin February 15, 1923 Patient J.L., December 15, 1922
Novo Nordisk NovoLog (aspart) NovoLog Mix 70/30 Novolin R Novolin N Novolin 70/30 Sanofi-Aventis Lantus (glargine) Lilly Humalog (lispro) Humalog Mix 75/25 Humulin R Humulin N Humulin 70/30 Humulin 50/50 Lente, Ultralente have been discontinued Insulin Preparations - US
Treatment with Insulin • Total daily requirement: • 0.5-1 unit/kg/day • 1.5 units/kg/day during puberty • Typical Regimens • NPH and Regular • Basal/Bolus: glargine and Novolog/Humalog
Insulin Delivery • Vials and syringes • Pens • Insulin pump
Physiological Serum Insulin Secretion Profile 75 Breakfast Lunch Dinner 50 Plasma insulin (µU/ml) Dawn phenomenon 25 4:00 8:00 12:00 16:00 20:00 24:00 4:00 8:00 Time
NPH and Regular 75 Breakfast Lunch Dinner 50 R R Plasma insulin (µU/ml) N N 25 4:00 8:00 12:00 16:00 20:00 24:00 4:00 8:00 Time
NPH and Regular 2/3 NPH 1/3 Regular AM 2/3 ½ NPH (2/3) ½ Regular (1/3) PM 1/3
NPH and Regular • Regular insulin given 30 min prior to a meal • NPH dose often given at bedtime • Prescribed amount of carbs at meals/snacks
NPH and Regular • AM blood glucoses → Evening NPH • Lunch → AM Regular • Dinner → AM NPH • Bedtime → PM Regular
Basal/Bolus Breakfast Lunch Dinner Aspart Aspart Aspart or or or Lispro Lispro Lispro Plasma insulin Glargine 4:00 8:00 12:00 16:00 20:00 24:00 4:00 8:00 Time
Basal/Bolus • Basal: glargine, 50% total daily dose • Bolus: NovoLog or Humalog • Insulin to carbohydrate ratio • Correction BG – target Correction factor
Basal/Bolus • I:CHO = 450/total daily insulin dose = amount of carbs 1 units will cover • Correction Factor: “1700 rule” = 1700/TDD • Glargine can not be mixed with any other insulins
Basal/Bolus • Glargine dose limited by which blood sugar? • 2 AM and breakfast • Which blood sugar is affected by the I:CHO ratio? • 2 hour post-prandial
NPH and Regular • Advantages • 2-3 shots per day • “Easier” – less carb counting and calculations • Disadvantages • Strict dietary plan • Less flexible • Less physiologic
Basal/Bolus • Advantages • More physiologic • More flexible • Less hypoglycemia • Disadvantages • More labor-intensive (CHO counting, insulin calculations) • At least 4 injections per day
Diet • Healthy, balanced diet • 50-60% total calories from carbohydrate • <30% fat • 10-20% protein • Carbohydrate counting • No forbidden foods - moderation • Eating too much will not cause ketosis
Exercise • Increases sensitivity to insulin • Helps control blood sugar • Lowers cardiovascular risk • Blood sugar usually decreases but may initially increase • Hypoglycemia may occur during, immediately after, or 8-24 hours later
Exercise • Check blood sugar before, during, after • Always have snacks available • May need extra snacks or decreased insulin (learn from experience) • Usually 15 gm CHO for every 30 min vigorous exercise • Do not exercise if ketones are present
Psychosocial Support • Every newly diagnosed family should meet with a psychologist • Guilt • Anger • Fear • Denial • Depression
Case 1: Special Concerns for College Students • Independence • Dining hall food • Alcohol – lowers blood sugar • Roommate aware of diabetes, glucagon • Airline travel – prescription labels
Case 1 • Discharged after teaching complete on • Glargine and Humalog • 0.7 units/kg/day • 3 weeks after diagnosis blood sugars begin going low • What is going on?
Honeymoon Phase • Educate that it may happen • Diabetes is not cured! • Occurs within first 3 months of diagnosis • Insulin requirements <0.5 units/kg/day • Lasts weeks to up to 2 years • Resolution of glucotoxicity, recovery of residual β-cell function
Case 1 • Blood glucoses continue to be so low that pt takes himself off all insulin • Normal blood glucoses for 5 months off insulin • Blood glucoses begin to rise • Homesickness • Depression
Long Term Complications • Retinopathy • Nephropathy • Neuropathy • Cardiovascular disease • Prevention by optimal glucose control
Conventional Therapy 1-2 injections/day Mean A1c 9% Intensive Therapy ≥3 injections/day Mean A1c 7% Diabetes Control and Complications Trial • 1983-1993, early termination given results • Intensive therapy delays onset and progression • of long-term complications in type 1 diabetes
Diabetes Control and Complications Trial • Intensive therapy reduced risk by: • 76% for retinopathy • 54% for nephropathy • 69% for neuropathy • 41% for macrovascular disease • Adverse events • Hypoglycemia • Weight gain
Case 1 – Follow-up visit • Home from college on break • Insulin requirement 0.5 units/kg/day • Physical exam • Monitoring for complications
Physical Exam • Height, weight, BP • Pubertal progression • Thyroid • Abdomen • Shot sites - lipohypertrophy • Feet • Medical alert tag
Prayer Sign Limited joint mobility Associated with: poor control, increased risk of retinopathy, nephropathy
Monitoring • Hemoglobin A1c – every 3 months • Celiac screen – at diagnosis and if ssx • Annually • TSH • Ophthalmology exam - after 10 and 3-5 yrs disease • Urine microalbumin - after 10 and 5 yrs disease • Lipid panel - puberty, unless fam hx, q5 years if normal • Influenza vaccine
Case 1 • Hemoglobin A1c - 6.0% • Ophthalmology exam – no retinopathy • TSH, FT4 – normal • Lipids – cholesterol 143 • Urine microalbumin - negative
Hemoglobin A1c • Reflects blood glucose over the past 3 months • Goal <7 for adults <7.5% for teens <8% for 6-12 y/o 7.5-8.5% for <6 y/o
Case 1 • 1 year after diagnosis, remains diligent about sending blood sugars • Insulin requirements 0.5 units/kg/day • A1c 5.9% • Interested in the insulin pump