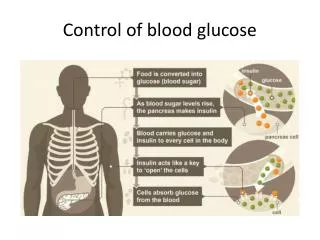
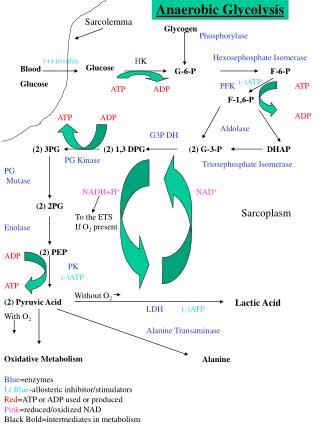
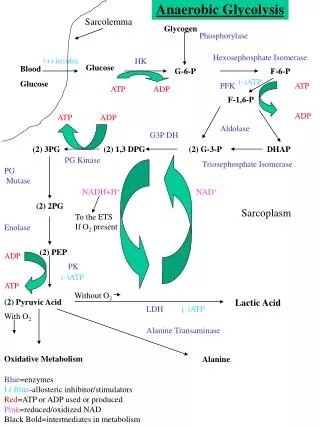
BLOOD GLUCOSE CONTROL
BLOOD GLUCOSE CONTROL. HYPOGLYCEMIA Learning Module. INPATIENT BLOOD GLUCOSE CONTROL. This learning module is required for orientation to Diabetes Care and blood glucose control here at Saint Joseph Health System. This can also be used for periodic reviews as needed.

BLOOD GLUCOSE CONTROL
E N D
Presentation Transcript
BLOOD GLUCOSE CONTROL HYPOGLYCEMIA Learning Module
INPATIENT BLOOD GLUCOSE CONTROL This learning module is required for orientation to Diabetes Care and blood glucose control here at Saint Joseph Health System. This can also be used for periodic reviews as needed. The purpose of this module is: • To describe the hypoglycemia signs and symptoms and causes. • To discuss inpatient treatment of hypoglycemia. At the end of this module, you will take the post-test.
HYPOGLYCEMIA DEFINITION Hypoglycemia protocol now defines hypoglycemia as <70mg/dl.
HYPOGLYCEMIA SIGNS AND SYMPTOMS Hypoglycemia signs and symptoms can be categorized as mild, moderate, or severe. MILD HYPOGLYCEMIA SYMPTOMS = Hunger Tired Headache Sweating Dizzy Nervous Shakiness Light headed Blurred vision Fast/pounding heart beat Numbness/tingling around mouth or lips If this goes untreated it can lead to moderate hypoglycemia.
HYPOGLYCEMIASIGNS AND SYMPTOMS MODERATE HYPOGLYCEMIA SYMPTOMS = Personality change Poor coordination Irritability Difficulty in concentration Confusion Slurred/slowed speech If this goes untreated and the blood glucose continues to drop then severe hypoglycemia can occur.
HYPOGLYCEMIASIGNS AND SYMPTOMS SEVERE HYPOGLYCEMIA SYMPTOMS = Mental status changes Unconsciousness Coma. This could lead to convulsions or death if not taken care of immediately! Whew! We don’t want that to happen!!!
HYPOGLYCEMIA Keep in mind that even though Hypoglycemia can be serious and must be treated right away, it rarely results in any adverse effects.
CAUSES OF HYPOGLYCEMIA Generally, there are 3 main causes: • When the body’s glucose is used up too rapidly, or, • When glucose is released into the blood stream too slowly, or, • When too much insulin is released into the bloodstream
CAUSES OF HYPOGLYCEMIA More specifically, hypoglycemia can be caused by: • Too much insulin • Oral anti-diabetes medications (as sulfonylureas or insulin secretagogues) • Skipped or delayed meals • Renal insufficiency • Liver disease • Gastroparesis • Menstrual Cycles • When TPN or TF is stopped and NPO or low PO intake So, what can we do about hypoglycemia?
HYPOGLYCEMIA TREATMENT Of course prevention is the best intervention. But when hypoglycemia happens, eating or drinking a form of simple carbohydrate that contains glucose is the main treatment. The KEY and challenge to treatment is to not overtreat. Overtreating hypoglycemia causes posttreatment hyperglycemia. Thus potentially putting the patient on a ‘roller-coaster’ of trying to treat high and low swings in blood glucose. And boy that does not feel good!!! So how do we treat hypoglycemia for our patients?
BLOOD GLUCOSE TARGET inpatient target blood glucose for people with diabetes is: Prepradial < 140mg/dl and random <180 for Med/Surg/Tele patients 140-180 mg/dl. for Critical Care patients
HYPOGLYCEMIA PROTOCOL This protocol does not need a physician’s order to implement it. The hypoglycemia protocols are based on the FSBG (finger stick blood glucose) number and the signs/symptoms the patient may be experiencing! For any suspected hypoglycemia, do a FSBG immediately AND if low treat with this protocol. (Remember we already reviewed the signs & symptoms)
HYPOGLYCEMIA PROTOCOL This protocol has the following definitions: Mild/Moderate Hypoglycemia is defined as: FSBG 41 – 69mg/dl whether symptomatic or not Severe Hypoglycemia is defined as: FSBG is 40mg/dl or less OK first let’s discuss mild/moderate treatment in relation to if the patient is eating or not.
MILD/MODERATE HYPOGLYCEMIA TREATMENT Treatment for patients who are eating: If the mealtime tray is available: • Feed the patient immediately • Check FSBG in 15 minutes • Continue to check FSBG and treat with 15-30 grams carbohydrate while FSBG remains <70mg/dl every 15-20 minutes Use your good nursing assessment as to whether you use 15grams (for mild hypoglycemia) or 30grams (for moderate hypoglycemia). Also, don’t assume that the meal will correct the hypoglycemia. . . . . . . it may not! KEY POINT: Do not add sugar to the juice!!! That is considered overtreating.
MILD/MODERATE HYPOGLYCEMIA TREATMENT Treatment for patients who are eating: If it is not mealtime: • Give the patient 15-30 grams of carbohydrate using one of the following: • 3 to 4 glucose tablets • one Glutose gel tube (squeeze tube contents into patient’s mouth and have them swallow) • one-half cup juice (Do Not add extra sugar) • Again keep treating the hypoglycemia every 15 – 20 minutes until the FSBG is >70mg/dl Tablets or gel are preferred treatment since they are a purer form of glucose; these are located in the Accudose. Apple juice is preferred over orange juice since orange juice may be contraindicated in many patients (as renal or cardiac patients). However, if the patient does not like apple juice, then choose tablets, gel, or orange juice.
MILD/MODERATE HYPOGLYCEMIA TREATMENT Re-testing the FSBG and treating EVERY 15-20 minutes with 15 to 30 grams carbohydrate is very important! When you do this you must also document all FSBG and treatment and response to treatment as well! Then the LAST STEP is: Once the hypoglycemia is resolved AND if it is more than an hour before next meal, give one of the following: • 6 crackers and 1ounce cheese, OR, • 6 crackers and 2 Tbsp. peanut butter, OR, • 1 slice bread and 1 ounce meat/cheese, OR, • 1 carton of skim milk with 1 box (serving) of cereal
MILD/MODERATE HYPOGLYCEMIA TREATMENT If after 45 minutes of treatment and hypoglycemia is not resolved, call the doctor who is managing the patients blood glucose for further orders. Special notes: • If the patient is being treated with Acarbose (Precose) or Miglitol (Glyset) treat with only tablets or gel(a purer form of glucose has to be used since these drugs effect the digestive system). • Avoid use of Glutose gel if patient has a decreased swallowing reflex (on aspiration precautions). • Intubated patients should be treated intravenously.
SEVERE HYPOGLYCEMIA TREATMENT Now let’s discuss Severe Hypoglycemia treatment. Remember this is defined as the following: FSBG of 41-69mg/dl with mental status changes, or, Unconscious, or, FSBG of 40mg/dl or less(whether symptomatic or not) For any severe hypoglycemia, obtain a STAT lab blood glucose AND treat the low FSBG! (You are not to wait for the lab results to start the treatment) KEY POINT: Patients who are NPO and have hypoglycemia will be treated as if in severe hypoglycemia if FSBG is less than 70mg/dl. Now, let’s look at IV available versus IV not available.
SEVERE HYPOGLYCEMIA TREATMENT If an IV is available, follow these steps: • Give one (1) amp of D50 (50ml) • Retest FSBG 15-20 minutes after treatment • If adult remains unconscious, give additional one (1) amp (50ml) of D50 slowly • Notify physician • When patient is conscious, follow up with a snack (as discussed earlier)
SEVERE HYPOGLYCEMIA TREATMENT If an IV is not available: (or if the patient is not willing or able to swallow) • Give Glucagon IM (1mg) Retest FSBG 15-20 minutes after treatment • Start an IV with D5W, if the patient remains unconscious • Give one (1) amp D50 slowly • Start D5W at 100ml/hour • Notify physician KEY POINT: Glucagon comes in a kit from the Pharmacy. It has to be reconstituted by the nurse right before giving it.
SEVERE HYPOGLYCEMIA TREATMENT Glucagon was the first step if the IV is not available. Do you know what it is and how to use glucagon? Glucagon is an important hormone in carbohydrate metabolism. It is released from the Alpha cells of the pancreas. It helps maintain the level of glucose in the blood by causing the liver to release its stored glucose. Glucagon is given for severe hypoglycemia as an IM injection which helps to quickly raise the blood glucose. When Glucagon is used, place the unconscious patient on his/her side, supporting the head, give the IM injection, and closely observe the patient. The patient may wake up vomiting and/or feeling sick. Always let the doctor know you’ve had to use Glucagon.
SEVERE HYPOGLYCEMIA TREATMENT REMINDER: Implement seizure precautions (observe for seizures) when patient is experiencing severe hypoglycemia. KEY POINTS: Plan ahead!!! For any patient on insulin, always keep a watch out for hypoglycemia. Have the hypoglycemia protocol readily available on your clip board or in the MAR. Treat immediately and re-treat!!! Teach!!! Document, document, document!!!
HYPOGLYCEMIA OTHER POINTS OF INTEREST: Some patients may have ‘hypoglycemia unawareness’. This is when the patient loses the ability to feel the symptoms of low blood glucose. Frequent monitoring helps to identify that condition and treatment is initiated sooner. This helps the body to recognize the low blood glucose sooner. KEY POINT: It is important to treat the FSBG number whether symptomatic or not. Another point of interest is the timing of FSBGs, Insulin Administration and meals.
TIMING OF FSBG, INSULIN, AND MEALS The timing of checking a patient’s blood glucose is important in relation to the meal. It’s important to check it right before the meal (which is why the order needs to be ac & hs). Then it can be determined whether insulin is needed or not. And depending on the type of insulin, it may be given right before the meal (as Novolog or Humalog insulin) or up to about 30 minutes before the meal (as Regular insulin).
TIMING OF FSBG, INSULIN, AND MEALS Therefore, we often need to encourage the patient to eat especially if he/she is receiving insulin. Sometimes if the patient does not eat enough and insulin is given, then low blood glucose could occur. Monitoring, recognizing hypoglycemia symptoms, and providing replacement foods will help to prevent it!!! A consult to the Dietitian and Diabetes Treatment Center may need to be considered.
HYPOGLYCEMIA KEY POINTS: Physicians base medication changes on how much hypoglycemia or hyperglycemia is occurring. So the Physician won’t know that unless it is accurately documented. DOCUMENT the result, time, and treatment on the MAR; & DOCUMENT the following in the blood glucose section of the patient care flow sheet: • FSBG • Time of hypoglycemia occurrence • If patient is symptomatic or not • Treatment (and if no treatment) • Response to treatment • If Physician was called and why
HYPOGLYCEMIA KEY POINTS cont’d: When a patient experiences hypoglycemia, use this time as a teachable moment. Discuss the signs and symptoms, how to treat and when to call the doctor. If the patient has Type 1 diabetes, verify with the patient and family if someone knows how to give glucagon. If not, once again, a teachable moment has occurred. Use your resources! Remember all the forms, protocols, standing orders, and teaching materials are at your fingertips. . . . . . All located in the SJH intranet (under Departments, then choose Diabetes Treatment center (DTC). And, use the event as a learning experience for yourself; reassess the cause and how it could have been prevented.
HYPOGLYCEMIA Example of documenting hypoglycemia on the Hypoglycemia MAR form. You can document on the patient’s current MAR or you can use this form. This form is located in the Orders & Forms section of the SJHS Intranet, under Endocrinology as the 2nd page of the Blood Glucose Control Protocol.
HYPOGLYCEMIA Whew, that’s a lot of GOOD information!!! Well, let’s see if you can now put it to use! Let’s look at several case studies. Hang in there! This won’t take too long!!!
CASE STUDY #1 Your patient, Mrs. Smith is going for surgery later today. She is NPO and you have just started an IV. She calls out and says she feels light headed. What do you do? Ta da ta duh ta da duh . . . . Well, that’s the computer version of the Jeopardy music!!
CASE STUDY #1 Obviously, the first step is to check her FSBG. When you do, you find that it is 52mg/dl. What is your next step?
CASE STUDY #1 Yes, one amp of D50 is the correct answer! Remember if the patient is NPO & FSBG is less than 70mg, the hypoglycemia is to be treated as if it is severe. And of course Mrs. Smith had an IV available. Then retest the FSBG 15-20 minutes after initial treatment and every 15-20 minutes thereafter. You may have to give an additional one (1) amp of D50 slowly if the hypoglycemia continues. Remember after the initial treatment to notify the patient’s physician who is taking care of the blood glucose for further orders.
CASE STUDY #2 GOOD JOB!!! Let’s look at the next case study. You gave Mr. Jones 70/30 insulin about 0715 this morning. It is now 12noon. You go to check on Mr. Jones and notice he is sweating and seems irritable when you ask how he feels. What should you do?
CASE STUDY #2 Of course, the first step is to check his FSBG. OK, his FSBG is 63mg/dl. What is your first step in treating this hypoglycemia? A HINT . . . It is 12noon and the dietary tray cart is on the unit.
CASE STUDY #2 YES! Feed Mr. Smith. Give him his meal tray! No need to give an extra carbohydrate at this point yet. Then what do you do? YES! Check his FSBG in 15-20 minutes. You’ll need to keep checking his FSBG every 15-20 minutes until it is >70mg/dl.
CASE STUDY #2 Please do not assume that eating his meal will take care of the hypoglycemia. He still might need a bit more carbohydrate, OR, he may not. Do check his FSBG shortly after he has finished his meal! Observe for potential other hypoglycemia occurrences. Remember to document!!!
CASE STUDY #2 One more point of interest with Mr. Jones’ case. Remember he had his scheduled 70/30 insulin about 4 to 5 hours prior to the hypoglycemia occurrence. 70/30 insulin has regular insulin in it which has a peak effect of around 4 to 6 hours. Do pay attention to future insulin doses and monitor for hypoglycemia especially in that 4 to 6 hour period. Because if it does happen again, then perhaps the insulin dose or the time it is given, may need adjustment!
CASE STUDY #3 Your patient Ms. Torres says she feels like her blood sugar is low and would like something to eat. She has no other symptoms of hypoglycemia other than she is hungry. Her FSBG is 74mg/dl. What are you going to do? (Yes, this could be a trick question . . . . :-)
CASE STUDY #3 Let’s think this through . . . . . . . . The in-hospital blood glucose range is 70 – 180mg/dl. The hypoglycemia protocol says to start treatment when the FSBG is less than 70mg/dl. regardless of symptoms or not. Her FSBG is 74mg/dl. She wants something to eat. HHhhmmmm.
CASE STUDY #3 Well, if her diet allows it, give her something to eat! Technically, you are not ‘treating a low blood glucose’. You are just giving her something to eat because she asked for it. However, pay attention to future FSBG’s and other symptoms (just in case she actually does become hypoglycemic).
CASE STUDY #4 OK, let’s do one more case study. You are one of those lucky nurses who has a nursing assistant do all the FSBG’s. She comes to you and says that Mr. Johnson is disoriented (this is a change in his mental status), sleepy, and his FSBG is 44mg/dl. What do you do?
CASE STUDY #4 On your way back to his room, you get a cup of apple juice. When you get to his room, you find Mr. Johnson laying in his bed having pulled out his only IV (he was a hard stick). You try to give the juice but he is not swallowing well and he chokes a bit. What are you going to do?
CASE STUDY #4 Yes, take a deep breath and think GLUCAGON!!! • Ask the nursing assistant to stay with the patient. • Call Pharmacy for a STAT Glucagon injection kit. • Turn the patient on his side and put a pillow under his head. • Give the IM injection in his hip.
CASE STUDY #4 Now, comes the hard part. . . . . wait, observe, and support. Remember after glucagon injection, the patient could get sick and throw up. So be prepared for this. Also get prepared to start another IV as soon as possible. After 15-20 minutes, check his FSBG again.
CASE STUDY #4 OK, let’s say he arouses and is now becoming oriented. You check his FSBG and it is 65mg/dl. He is able to swallow now. Give him either a ½ cup juice, or 4 glucose tablets, or one Glutose gel tube. Keep checking the FSBG every 15-20minutes until it has stabilized above 70mg/dl. and treat as needed.
KEY POINTERS It can not be repeated enough . . . . . When treating hypoglycemia, give 15 to 30 grams of carbohydrate every 15-20 minutes until the FSBG is above 70mg/dl. Do not over treat!!! Follow the protocol. Observe for future hypoglycemia once the patient has one occurrence.
HYPOGLYCEMIA Just remember the following four steps when hypoglycemia occurs: PLAN TREAT TEACH PREVENT DOCUMENT
THE FINISH LINE!!! CONGRATULATIONS! You have just finished the HYPOGLYCEMIA Learning Module If you have any questions, please contact your Clinical Educator, your unit’s Diabetes Champion, or one of the Diabetes Educators.