The Integumentary System
The Integumentary System. Dr Idara . subtopics. Skin (cutaneous membrane) Subcutaneous tissue below the skin Accessory Structures Sweat glands Sebaceous or oil glands Hair Nails. The Integumentary System. Integument is skin Skin and its appendages make up the integumentary system


The Integumentary System
E N D
Presentation Transcript
The Integumentary System Dr Idara
subtopics • Skin (cutaneous membrane) • Subcutaneous tissue below the skin • Accessory Structures • Sweat glands • Sebaceous or oil glands • Hair • Nails
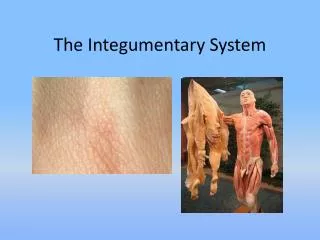
The Integumentary System • Integument is skin • Skin and its appendages make up the integumentary system • A fatty layer (hypodermis) lies deep to it • Two distinct regions • Epidermis • Dermis
Functions of skin • Protection • Cushions and insulates and is waterproof • Protects from chemicals, heat, cold, bacteria • Screens UV • Synthesizes vitamin D with UV • Regulates body heat • Prevents unnecessary water loss • Sensory reception (nerve endings) • The melanocytes contain melanin, which absorbs UV radiation, and also distribute the pigment to neighboring cells. Skin exposed to sunlight becomes wrinkled and creased. Changes seem to be due to disruption of collagen and elastin in dermis, and loss of fibroblasts which make new proteins.
Epidermis • Avascular as it has no blood supply of its own • Oxygen and nutrients diffuse from the underlying dermis • The epidermis is a keratinized stratified squamous epithelium. Oxygen and nutrients diffuse from the underlying dermis. Five structurally different layers can be identified:
Layers (from deep to superficial) • Stratum basale or germinativum – stem cells or mitotic cells. Cells here are constantly dividing and as new cells form, older ones are pushed toward the skin surface. • Stratum spinosum – Consist of prickle cells that interlock to support the skin.
Stratum granulosum- This layer initiates Keratinization. This process starts the death of epithelial cells ( cells that make up the skin) • Stratum lucidum- This layer is made up of translucent cells. This thick layer appears only in frequently used areas used areas such as the palms of the hands and the soles of the feet. • Stratum corneum – horny layer (cells dead, many layers thick). The cells here are filled with keratin which keeps the skin elastic and protects underlying cells from drying out.
Four types of cells • Keratinocytes– deepest, produce keratin (tough fibrous protein) • Melanocytes - make dark skin pigment melanin • Merkel cells – associated with sensory nerve endings for touch sensations • Langerhans cells – macrophage-like dendritic cells, which helps the immune system.
The stratum basale • is the deepest layer of the epidermis (closest to the dermis). • It is found close to the dermal blood supply. • It consists of a single layer of columnar or cuboidal cells which rest on the basement membrane. • Basal cells are the stem cells of the epidermis. • Their mitotic activity replenishes the cells in more superficial layers as these are eventually shed from the epidermis.
stratum corneum • cells are keratinized and form a layer that is about 30 cells thick. • Closest to the surface of the epidermis, • Cells are constantly shed from this part of the stratum corneum. This layer makes up three fourths of the epidermal thickness. The protection of the body by the epidermis is due to the functional features of the stratum corneum.
The renewal of the epidermis takes about 3 to 4 weeks in humans as millions of cells are produced daily. • Cells die as they are pushed away from the source of nourishment. Cells undergo keratinization as a tough protein, keratin, is deposited within the cell. • Keratin hardens and flattens the cells as they move outward and it waterproofs the skin.
Skin color • Three skin pigments • Melanin: the most important • Carotene: from carrots and yellow veggies • Hemoglobin: the pink of light skin
Other Pigments in Skin • Carotene – a yellow pigment in skin usually hidden by the effects of melanin. Asians have little melanin which allows the yellow to show more than other nationalities. • Pinkish color – seen in fair-skinned persons because the vascular dermis is visible.
Cyanosis – blue look to skin due to poorly oxygenated blood • Blushing – caused by dilation of blood vessels • Pale by fright – caused by constriction of vessels
Response to Disease • Jaundice – caused when Bilirubin is deposited in skin because a diseased liver is unable to excrete this pigment • A bruise indicates that blood has escaped from the blood vessels and has clotted under the skin. • Malignant melanoma – a cancerous change in a mole that may metastasize (spread) rapidly and is most difficult to treat. Exposure to sunlight increases risk. • Skin may appear bronzed due to the deposit of excess melanin when a person’s adrenal gland is functioning poorly.
Dermis • The dermis, or corium, consists of dense fibrous connective tissue with numerous collagenous and elastic fibers. • The dermis is much thicker than the epidermis. In thick skin, dermal papillae create a very irregular border between epidermis and dermis. • Blood vessels, nervous tissue, some muscle tissue, certain glands, hair and nails are found in the dermis.
Strong, flexible connective tissue: your “hide” • Fiber types: collagen, elastic, reticular • Critical role in temperature regulation (the vessels) • Nerve endings allow us to sense pain, temperature, pressure, and touch.
Divisions of the Dermis • The Papillary Layer: has loose connective tissue This layer lies directly beneath the epidermis and connects to it via Papillae ( fingerlike projections). Some papillae contain capillaries that nourish the epidermis; others contain Meissner’s Corpuscles( touch receptors). A double row of papillae in finger pads produces the ridged fingerprints on finger tips. 2. The Reticular layer which has dense connective tissue These layers are so closely connected that they are difficult to differentiate.
Exocrine Glands • Sebaceous glands or oil glands are simple branchedareolar glands. They secrete the sebum (seb = oil) an oily product. • Sebum is usually secreted into a hair follicle. Sebum is a natural skin cream: it helps hair from becoming brittle, prevents excessive evaporation of water from the skin, keeps the skin soft and contains a bactericidal agent that inhibits the growth of certain bacteria.
Sebaceous glands are scattered all over the surface of the skin except in the palms, soles and the side of the feet. • When the sebaceous glands oversecretes and bacteria acts on the secretions, a blackhead or pimple results.
SweAT glands • Sweat glands or sudoriferous glands are simple coiled tubular glands. They are divided into two principal types: eccrine and apocrine. • Apocrine glandsare found mainly in the skin of the armpits, of the anogenital areas and of the areola of the breasts. Their secretory portion can be located in the dermis or in the hypodermis. Their excretory ducts open into hair follicles. Their secretion is more viscous than that of the eccrine glands. They start secreting at puberty and may be analogous to the sexual scent glands of other animals.
Eccrine glands are the most common. • Their secretory portion can be located in the dermis or in the hypodermis. They produce sweat, a watery mixture of salts, antibodies and metabolic wastes. Sweat prevents overheating of the body and thus helps regulate body temperature.
Accessory Structures of the Skin Hair • A characteristic feature of the human skin is the apparent lack of hair on most of the body surface. This is actually not quite true. Most of the skin is haired although the hair in most areas is short, fine and only lightly pigmented. • Truly hairless are only the palms of hands and soles of feet, the distal phalanges and sides of fingers and toes and parts of the external genitalia.
Hair development begins in the third fetal month. By the fifth month of fetal life, Lanugo ( fetal hair) covers the fetus. • At 5 months after birth, lanugo disappears from every area except the scalp and eyebrows where coarser hair replaces it. • Vellus( a film of delicate hair) eventually covers the rest of the body. • Terminal hair is the early coarse scalp and eyebrow hair and later armpit and genital hair that grow during puberty.
Accessory Structures of the Skin • In those parts of the skin which we perceive as "hairy" we find terminal hairs. The free part of each hair is called the shaft. • The root of each hair is anchored in a tubular invagination of the epidermis, the hair follicle, which extends down into the dermis and, usually, a short distance into the hypodermis.
The hair that you groom daily is actually dead keratinized cells. • Each hair follicle has an associated bundle of smooth muscle, the arrectorpili muscle. This muscle inserts with one end to the papillary layer of the dermis and with the other end to the dermal sheath of the hair follicle. This makes your hair stand up on its end.
Hair Color and Texture • Hair color is determined by the amount and type of melanin present. • Melanocytes become less active with age (and hydrogen peroxide is produced by hair follicle neutralized by an enzyme). Gray hair is a mixture of pigmented and non-pigmented hairs. • Red hair results from a modified type of melanin that contains iron.
The shape of the hair shaft determines texture. • Round shaft – straight hair • Oval shaft – wavy hair • Flat shafts – curly or kinky hair Alopecia is the term for hair loss. • Functions of hair • Warmth – less in man than other mammals • Sense light touch of the skin • Protection - scalp
Accessory Structures of the Skin • Nails • Plates of stratified squamous epithelial cells with hard keratin • Protect distal ends of phalanges • Cells are keratinized in the nail root • Nail growth occurs in the lunula • Cuticle is a fold of stratum corneum on the proximal end of nail
Disorders of the integumentary system • Burns • Threat to life • Catastrophic loss of body fluids • Dehydration and fatal circulatory shock • Infection • Types • First degree – epidermis: redness (e.g. sunburn) • Second degree – epidermis and upper dermis: blister • Third degree - full thickness • Infections • Fluid loss • Heat loss
Burns First-degree (epidermis only; redness) Second-degree (epidermis and dermis, with blistering) Third-degree (full thickness, destroying epidermis, dermis, often part of hypodermis)
Critical burns Estimate by “rule of 9’s” • Over 10% of the body has third-degree burns • 25 % of the body has second-degree burns • Third-degree burns on face, hands, or feet
How Skin Heals • When your skin gets cut, your body springs into action to heal the wound. First, the body works to limit blood loss by reducing the amount of blood flowing to the wounded area. • For wound healing to occur, certain factors are needed. A good nutritional status which includes adequate blood supply to provide oxygen and nutrients and also remove wastes.
Primary healing ( wound Healingby first intention) This method applies when there is minimal tissue destruction and when the wound edges are apposed. There are three (3) stages which overlap. • Inflammation • Proliferation • Maturation Inflammation: The cut surface becomes inflammedand cell debris and blood clot fills the gap between the cut surfaces in the first few hours. Phagocytes ( neutrophils macrophages) and fibroblasts migrate into the blood clot. The phagocytes begin to remove the clot and cell debris. At the same time, fibroblasts secrete collagen fibers which begin to bind the surfaces together.
Proliferation Epithelial cells proliferate across the wound, through the clot. The epidermis meets and grows upwards until full thickness is restored. The clot above the new tissue becomes the scab and is shed after 3- 10 days. Granulation tissue is secreted by the fibroblasts it consists of new capillary buds, phagocytes and fibroblasts. This invades the clot, restoring blood supply to the wound. Phagocytes remove the debris and bacteria.
Maturation • The granulation tissue is then replaced by fibrous scar tissue. • The collagen fibers are then rearranged and wound strength increases. • The scar becomes less vascular, appearing after a few months as a fine line.
Wound Healing by Secondary Intention This method follows destruction of a large amount of tissue or when the wound edges can’t be apposed. E.g. large ulcers The stages for wound healing are the same in primary healing. Inflammation Inflammation develops on the surface of healthy tissue and the necrotic tissue sloughs off due mainly to the action of phagocytes. Proliferation Granulation tissue is deposited at the base of the cavity and grows upwards towards the surface stimulated by macrophages. Phagocytes prevent infection by ingesting bacteria. Granulation tissue can’t contract like normal skin tissue. When granulation tissue reaches the level of the dermis, epithelial cells at the edges proliferate and grow towards the center.
maturation This occurs by fibrosis, in which scar tissue replaces the granulation tissue. This occurs over several months until the full thickness of the skin is restored. Wound contraction is caused by increased numbers of myofibroblasts. Scar tissue is shiny and doesn’t contain sweat glands, hair follicles or sebaceous glands.
Temperature regulation • In hot conditions • Sweat glands under the skin secrete sweat (a fluid containing mostly water with some dissolved ions) which travels up the sweat duct, through the sweat pore and onto the surface of the skin. This causes heat loss via evaporative cooling however, a lot of essential water is lost.
The hairs on the skin lie flat, preventing heat from being trapped by the layer of still air between the hairs. This is caused by tiny muscles under the surface of the skin called arectorpili muscles relaxing so that their attached hair follicles are not erect. These flat hairs increase the flow of air next to the skin increasing heat loss by radiation. When environmental temperature is above core body temperature, sweating is the only physiological way for humans to lose heat.
Arterioles Vasodilation occurs, this is the process of relaxation of smooth muscle in arteriole walls allowing increased blood flow through the artery. This redirects blood into the superficial capillaries in the skin increasing heat loss.
Cold Temperatures • If the skin temperature drops below 37°C a variety of responses are initiated to conserve the heat in the body and to increase heat production. These include • Vasoconstriction to decrease the flow of heat to the skin. • Cessation of sweating. • Shivering to increase heat production in the muscles. • In lower animals, the erection of the hairs and fur to increase insulation.