O r al micro fl o ra Medical oral microbiology, 11th week
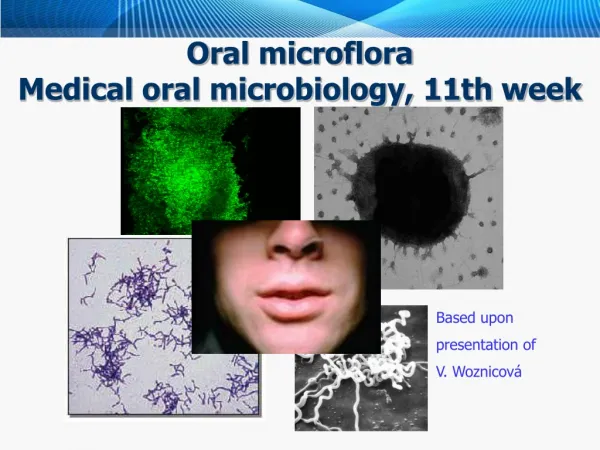
O r al micro fl o ra Medical oral microbiology, 11th week. Based upon presentation of V. Woznicová. History – Leeuwenhoek. (a) Original picture A.L., (b) Campylobacter rectus, (c) Selenomonas sputigena , (d) oral cocci (e) Treponema denticola, (f) Leptotrichia buccalis.

O r al micro fl o ra Medical oral microbiology, 11th week
E N D
Presentation Transcript
Oral microfloraMedical oral microbiology, 11th week Based upon presentation of V. Woznicová
History – Leeuwenhoek (a) Original picture A.L., (b) Campylobacter rectus, (c) Selenomonas sputigena , (d) oralcocci (e) Treponema denticola, (f) Leptotrichiabuccalis
Oral microflora • over700 members (bacteria, parasites) • Ecological system • Biofilm formation • Importantto health • Relationshiptodentalcaries and parodontitis
Sulcus gingivalis anaerobic environment, with sulcarfluid. Bacteria areimportantfor rise anddevelopmentof parodontic illness
Streptococci α-hemolytic streptococci are divided into groups • S. mutans group:S. mutans, lessfrequentS. sobrinus, rare S. cricetus andS. rattus. Change saccharosistosticky glucans and fructans, quicklyformacidsfrom saccharides • S.salivarius group:S. salivarius, S. vestibularis - in salivas and on the tongue surface. Change saccharosisto fructan levan, on solid soils with this sugar growsin mucouscolonies, can cause endocarditis.
S. mitis group:S. mitis ,S. oralis,S. peroris -onmucous membrane, indental plaque.In additon toS. mitiscan this group causesepsis lenta… S. sanguinis andS. gordonii – on tongue, bucalmucose andindental plaque. S. sanguiniscancleave IgA. Can causesubacute bacterial endocarditis (sepsis lenta)! • S. anginosus groupgrowinsmallcolonies - S. anginosus (S. milleri), S. constellatus – S.constellatusand S.pharyngis, andS. intermedius. Location: in nasopharynx, insulci gingivales. Cause dentoalveolar and endodontic infection.
Bacteria of „red complex“ Porphyromonas gingivalis feed, coagregation supportof adhesion and invazion RED COMPLEX + FUSOBACTERIA Treponema denticola Tannerella forsythia adherence Responsibility for parodontitis
Treponema denticola • Spirochatae • Proteolytic bacterium • Inelderchildren (6 – 12 years) andadult • Coagregation with fusobacteria, porphyromonades • Close relationship toP. gingivalis wikipedia.org/wiki/Treponema
T. denticola – factors of virulence • Protease – degradation of bariers, cells and protective macromolecules • Motility • Chemotaxis • Adhezins, invazins • Hemolyzins • Inflamatory starters – starts secretion of cytokins and chemokins
Porphyromonas gingivalis • High proteolytic • Crossfeeding -T. denticola produce succinate, P.g metabolise itandaffordisobutyric acid,proteolytic microorganism – quicklyresides sulcus gingivalis • Fimbria– for adhesis andcolonization • Releasebladderscontainingcompleteparts of surface membrane, bladders transport toxines and ensymes, enable adherence and agregationof bacteria, platelets • Contain black pigment – source of Fe (growing factor of bacteria) www.pgingivalis.org
Tannerella forsythia • Interaction betweenT. forythia andP. gingivalis – supportof adhezionto host cellsandinvazion www.acsu.buffalo.edu Invazion ofT. forsythia intocells, Inagaki 2006, confocal laser microscopy
„Products of metabolism P. gingivalisis susceptible to pH decrease and to O2 Fusobacterium nucleatumform products, who guard P. gingivalisbefore these factors Bakteriocins – natural antibiotics Bacteriocins kill the neighbour, producer and close related bacteria can survive Interactionof microorganism
Other G+ and G- bacteria • N. subflava, N. sicca, N. mucosa –saccharolytic, grow in aerobic condition although they are capnophylic • Staphylococci, micrococci – not commonly found in large numbers • Eikenella– isolated from periodontal disease, fac. anaerobic • Veillonella– dental plaque etiology + dental caries (more in plaque presentation) • other genera – propionibacter, enterococcus – less than 1% - unknown role or teeth specific
Mycoplasmas, actinomyces, lactobacilli • Actinomyces sp. major portion of the microflora of dental plaque – associated with caries, gingivitis (anaerobic) • Lactobacillus – less than 1%, producing lactate or lactate and acetate from glucose, increase in advanced carieer lesions (L. casei, L. oralis...) – microaerophilic • Mycoplasma pneumoniae, M. hominis, M. salivarium - role in dental plaque – unknown
Parasites and fungi in oral cavity • Entamoeba gingivalis, Trichomonas tenax – healthy patients • Candida sp. – colonization occurs either at birth or soon afterwards. Dramatically increases in immunocompromised patients…
Facts • Susceptibilitytophagocytosis is various, depends on microorganism. Some periodontopathogenic bacteriacan rescuebefore immuneresponse • A. actinomycetemcomitans and bacteriaof red-complexaremore resistant tophagocytosisthanother bacteria • Microbesfromoral cavitycan cause metastaticinfection (after teeth extraction - bacterial endocarditis)
Relationship of bacterial communitiesin parodontitis V.parvula A.odontolyticus S.mutans S.oralis S.sanguis P.intermedia P.nigrescens P.micros F.nuc.nucleatum F.nuc.vincentii F.nuc.polymorphum F.periodontium P.gingivalisT.forsythiaT.denticola E.corrodens C.gingivalis C.sputigena C.ochracea A.actinomyc. source: Socransky et al. 1998