Pneumonia
Pneumonia. PBL Presentation 15 April 2011. Definition of Pneumonia. Harrisons: An infection of the pulmonary parenchyma Respiratory tract infections are more frequent than infections of any other organ and account for the most number of workdays lost in the general population


Pneumonia
E N D
Presentation Transcript
Pneumonia PBL Presentation 15 April 2011
Definition of Pneumonia • Harrisons: An infection of the pulmonary parenchyma • Respiratory tract infections are more frequent than infections of any other organ and account for the most number of workdays lost in the general population • Pneumonia can result when any of the normal pulmonary defense mechanisms are impaired or when systemic host resistance is lowered
Defects in Local Defences • Loss or suppression of cough reflex – coma, anaesthesia, neuromuscular disorder, drugs, chest pain • Injury to mucociliary apparatus – cigarrette smoke, inhalation injury, viral disease, genetic defects • Accumulation of secretions – CF, bronchial obstruction • Interference of phagocytic activity – alcohol, tobacco smoke, anoxia, O2 intoxication • Pulmonary congestion and oedema
Epidemiology • In the US, there are 4 million cases of CAP each year. 80% of these are treated as outpatients, 20% in hospital • HAP results in 600,000 hospitalisations, 64 million days of restricted activity and 45,000 deaths annually • The annual cost is $9-10bn USD • The incidence varies, overall in is 12/1000 persons, but it is 12-18/1000 in children <4 years of age and 20/1000 in persons >60 years of age
Morphology • Bacterial pneumonia has two patterns of anatomic distribution. What are they?
Lobular bronchopneumonia is defined by patchy consolidation of the lung. This can be confluent, producing lobar consolidation • Lobar pneumonia is defined by fibrinosuppurative consolidation of a large portion of a lobe, or an entire lobe
Pathology of Typical Lobar Pneumonia (i.e. not viral, Pneumocystis) • 1. Oedema – presence of proteinaceous exudate and often bacteria in the alveoli • 2. Red hepatisation – erythrocytes in intraalveolar exudate, as well as neutrophils • 3. Gray hepatisation – erythrocytes have lysed and been degraded, neutrophils are the predominant cell, fibrin deposition is abundant and bacteria have disappeared. Infection has been contained and gas diffusion improves • 4. Resolution – Macrophage is the predominant cell type. Debris is cleared
The congested septal capillaries and extensive neutrophil exudation into alveoli corresponds to early red hepatization.
Early organization of intra-alveolar exudate, seen in areas to be streaming through the pores of Kohn (arrow).
Advanced organizing pneumonia featuring transformation of exudates to fibromyxoid masses richly infiltrated by macrophages and fibroblasts
Symptoms of Pneumonia • Symptoms depend on progression and severity of the disease • Patient is febrile, tachycardic • Chills and/or sweats • Cough that is either non-productive of productive of mucoid, purulent or blood-tinged sputum • Patient may be shortness of breath • If infection has involved the pleura, Px may experience pleuritic chest pain • 20% of patients have GIT symptoms (nausea, vomiting, diarrhoea) • Fatigue, headache, myalgias, arthralgias
Signs of Pneumonia • Findings depend on the degree of pulmonary consolidation and the presence of absence of pleural effusion • Respiratory rate is increased • Use of accessory muscles is common • Palpation can reveal increased or decreased tactile fremitus • Percussion note is dull or flat, either due to underlying consolidated lung or pleural fluid • Crackles, bronchial breath sounds, pleural friction rub can be heard on auscultation • Severely ill patients with septic shock are hypotensive and have evidence of organ failure
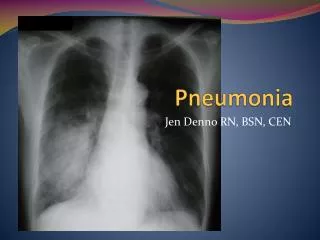
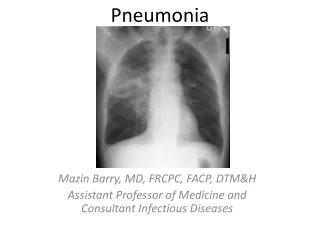
Diagnosis • DDx include: • Acute bronchitis • Acute exacerbations of chronic bronchitis • Heart failure • PE • Radiation pneumonitis • Specificity and sensitivity of findings on examination average 58 and 67% respectively • Chest radiography is required to confirm the diagnosis of CAP, as well as assessing the severity (e.g. cavitation, multilobar involvement) • Radiography can suggest an aetiologic diagnosis (pneumatocoeles suggest S. aureus, upper-lobe cavitating lesion suggests TB) • CT is rarely necessary but can be useful in post-obstructive pneumonia due to a tumour or foreign body • Lab tests are not done on an outpatient basis since results are not available soon enough to influence management, but influenza virus can be diagnosed at point-of-care to guide treatment
Diagnosing the Aetiology • Gram stain and culture of sputum (must have >25 neutrophils and <10 squamous epithelial cells per lpf to be valid). Sensitivity is poor (<50%) • Blood cultures (positive in only 5-14% of hospitalised patients with CAP, usually S. pneumoniae) • Antigen tests for Legionella and pneumococcal agents in urine • PCR • Serology (fourfold rise in IgM between acute and convalescent-phase serum samples)
Prognosis • The CURB-65 criteria include five variables: • confusion (C); • urea >7 mmol/L (U); • respiratory rate >30/min (R); • blood pressure, systolic <90 mmHg or diastolic <60 mmHg (B); • and age >65 years (65). • Patients with a score of 0, among whom the 30-day mortality rate is 1.5%, can be treated outside the hospital. With a score of 2, the 30-day mortality rate is 9.2%, and patients should be admitted to the hospital. Among patients with scores of >=3, mortality rates are 22% overall; these patients may require admission to an ICU
Prognosis • To determine the PSI, points are given for 20 variables, including age, coexisting illness, and abnormal physical and laboratory findings. On the basis of the resulting score, patients are assigned to one of five classes with the following mortality rates: class 1, 0.1%; class 2, 0.6%; class 3, 2.8%; class 4, 8.2%; and class 5, 29.2%. • Clinical trials have demonstrated that routine use of the PSI results in lower admission rates for class 1 and class 2 patients. Patients in classes 4 and 5 should be admitted to the hospital, while those in class 3 should ideally be admitted to an observation unit until a further decision can be made.