Pneumonia
Pneumonia. Dr Ibrahim Bashayreh, RN, PhD. Pneumonia. Acute inflammation of lung (lower respiratory tract) caused by microorganism, comes with fever, focal chest symptoms, shadowing on CXR Leading cause of death until 1936 Discovery of sulfa drugs and penicillin. Classification .


Pneumonia
E N D
Presentation Transcript
Pneumonia Dr Ibrahim Bashayreh, RN, PhD.
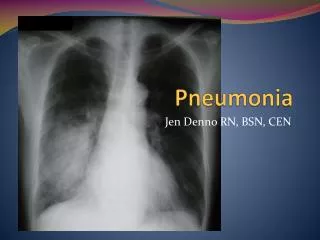
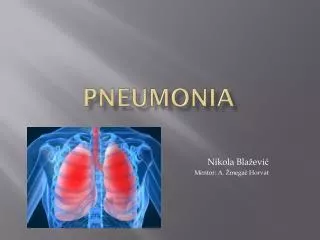
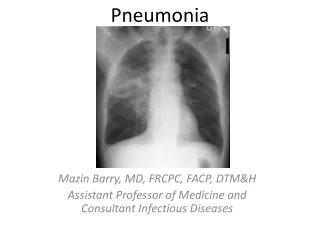
Pneumonia • Acute inflammation of lung (lower respiratory tract) caused by microorganism, comes with fever, focal chest symptoms, shadowing on CXR • Leading cause of death until 1936 • Discovery of sulfa drugs and penicillin
Classification • Community Acquired Pneumonia • Occur within 48 hrs of admission or in patient’s who haven’t been hospitalized in the last 2 wks • Strep pneumonia, mycoplasma pneumonia, influenza A, Haemophilus influenza, and Legionella are more common pathogens • Patients with chronic diseases are more prone to Klebsiella and other gram negative organisms • Highest incidence in winter • Smoking important risk factor
Types of Pneumonia • Hospital-acquired pneumonia (HAP) (Nasocomial Infection) • Develops 2 or more days after admission • Gram negative bacilli (Klebsiella, Pseudomonas, E coli, Proteus) or Staphylococcus are more common pathogens • Aspiration around an ETT/reduced consciousness or difficulty swallowing allows pathogens in the oropharynx to colonize the lungs • Ventilator-associated pneumonia (VAP): in patients on ventilators • Aspiation: follows aspiration of gastric contents • Immunosuppression: chemotherapy/bone marrow transplant/HIV patients susceptible to fungi and viral infections as well as other pathogen • Highest mortality rate of nosocomial infections
Causes of HAP • Pseudomonas • Enterobacter • S. aureus • S. pneumoniae • Immunosuppressive therapy • General debility • Endotracheal intubation
Risk Factors • Aging, 65 years or older • Male • Children under 2 • Having HIV or AIDS • Increased frequency of gram- negative bacilli (leukemia, diabetes, alcoholism) • Smoking • Being around certain chemicals • Living in certain parts of the country • Being hospitalized in ICU & having ETT • Pollution • Malnutrition
Acquisition of Organisms • Aspiration from nasopharynx, oropharynx • Inhalation of microbes • Hematogenous spread from primary infection elsewhere
Signs & Symptoms • Symptoms • Dyspnea • Pleurisy • Cough • Discolored sputum • Signs • Cyanosis • Tachycardia • Tachypnea • Dull percussion • Crepitus • Bronchial breath sounds • Pleural rub • Sweating, cold clammy skin • Non-respiratory features • Confusion, fatigue • Diarrhea, N&V.
Clinical Manifestations • CAP symptoms • Sudden onset of fever • Chills • Cough productive of purulent sputum • Pleuritic chest pain
Pathophysiology: Pneumococcal Pneumonia • Congestion from outpouring of fluid into alveoli • Microorganisms multiply and spread infection, interfering with lung function
Pathophysiology: Pneumococcal Pneumonia • Red hepatization • Massive dilation of capillaries • Alveoli fill with organisms, neutrophils, RBCs, and fibrin • Causes lungs to appear red and granular, similar to liver
Complications • Pleurisy (pain with breathing) • Pleural effusion • Usually is sterile and reabsorbed in 1-2 weeks or requires thoracentesis • Atelectasis • Usually clears with cough and deep breathing
Complications • Delayed resolution • Persistent infection seen on x-ray as residual consolidation • Lung abscess (pus-containing lesions) • Empyema (purulent exudate in pleural cavity) • Requires antibiotics and drainage of exudate
Complications • Pericarditis • From spread of microorganism • Arthritis • Systemic spread of organism • Exudate can be aspirated • Meningitis • Patient who is disoriented, confused, or somnolent should have lumbar puncture to evaluate meningitis
Complications • Endocarditis • Microorganisms attack endocardium and heart valves • Manifestations similar to bacterial endocarditis
Diagnostic Tests • History • Physical exam • Chest x-ray • Gram stain of sputum • Sputum culture and sensitivity • Pulse oximetry or ABGs • CBC, differential, chems • Blood cultures
Collaborative Care • Antibiotic therapy • Oxygen for hypoxemia • Analgesics for chest pain • Antipyretics • Influenza drugs • Influenza vaccine • Fluid intake at least 3 L per day • Caloric intake at least 1500 per day
Collaborative Care • Pneumococcal vaccine • Indicated for those at risk • Chronic illness such as heart and lung disease, diabetes mellitus • Recovering from severe illness • 65 or older • In long-term care facility
Nursing Assessment • History of Predisposing/Risk Factors • Lung cancer • COPD • Diabetes mellitus • Debilitating disease • Malnutrition
Nursing Assessment History of Predisposing/Risk Factors • AIDS • Use of antibiotics, corticosteroids, chemotherapy, immunosuppressants • Recent abdominal or thoracic surgery • Smoking, alcoholism, respiratory infections • Prolonged bed rest
Nursing Assessment • Clinical Manifestations • Dyspnea • Nasal congestion • Pain with breathing • Sore throat • Muscle aches • Fever
Nursing Assessment • Clinical Manifestations • Restlessness or lethargy • Splinting affected area • Tachypnea • Asymmetric chest movements • Use of accessory muscles • Crackles • Green or yellow sputum
Nursing Assessment • Clinical Manifestations • Tachycardia • Changes in mental status • Leukocytosis • Abnormal ABGs • Pleural effusion • Pneumothorax on CXR
Nursing Diagnoses • Ineffective breathing pattern • Ineffective airway clearance • Acute pain • Imbalanced nutrition: less than body requirements • Activity intolerance
Planning • Goals: Patient will have • Clear breath sounds • Normal breathing patterns • No signs of hypoxia • Normal chest x-ray • No complications related to pneumonia
Nursing Implementation • Teach nutrition, hygiene, rest, regular exercise to maintain natural resistance • Prompt treatment of URIs
Nursing Implementation • Encourage those at risk to obtain influenza and pneumococcal vaccinations • Reposition patient q2h • Assist patients at risk for aspiration with eating, drinking, and taking meds
Nursing Implementation • Assist immobile patients with turning and deep breathing • Strict asepsis • Emphasize need to take course of medication(s) • Teach drug-drug interactions
Evaluation • Dyspnea not present • SpO2> 95 • Free of adventitious breath sounds • Clears sputum from airway
Evaluation • Reports pain controlled • Verbalizes causal factors • Adequate fluid and caloric intake • Performs ADLs
Tuberculosis Famous people who have had TB Fredric Chopin* Eleanor Roosevelt* Nelson Mandela Ringo Starr Tom Jones Tina Turner *Died of TB
What is tuberculosis (TB)? • Disease caused by bacteria called Mycobacterium tuberculosis • Chronic bacterial infection • Was once the leading cause of death in US • The number of cases declined in the 1940’s when drugs were developed to treat TB • TB is still a problem worldwide • 8 million people develop TB yearly • 3 million die
Tuberculosis • 5-10% become active • Only contagious when active • Primarily affect lungs but… • Kidneys • Liver • Brain • Bone
How is TB spread? • Through the air from person to person by coughing • Usually attacks lungs • Two stages • Latent TB • asymptomatic and not contagious • can take medication to prevent development of disease • Active TB Disease • May spread to others • May have abnormal chest x-ray • Usually have positive skin test
Symptoms of TB • Chills • Fever • Weakness or fatigue • Sweating while sleeping, Night sweats • Cough that lasts longer than 2 weeks • Pain in chest • Coughing up blood or sputum
Risk Factors • Close contact with someone who is infected with TB • Traveling to a country where TB is common • Foreign-born individuals and minorities have a higher incidence of developing TB • 2002: 50% of US cases were in foreign-born individuals. • 2002: 80% of all US TB cases were in ethnic and racial minorities.
Risk Factors • Immunocompromise • Substance abuse • Indigent (POVERTY) • Living in overcrowded, substandard housing • Health care workers performing high risk activities
Multi-drug resistant TB (MDR TB) • Bacteria become resistant to antibiotics • Arose from improper use of antibiotics in the treatment of TB • Treatment of one case can cost up to $1.3 million • 45 states and Washington, DC have confirmed cases of MDR TB • Treatment is difficult and costly • Can develop from not taking proper course of antibiotics for TB • MDR TB can be spread by an infected person
How to protect yourself • BCG vaccine for TB is given in many countries • Not recommended for healthcare workers unless a high percentage of patients are infected with MDR TB • PPD test if exposure is suspected • USE proper PPE when in contact with patients who may have TB
PPD Skin Test Procedure • Intradermal administration of PPD • L forearm • Must be “read” between 48 and 72 hours • To accurately “read” • Visual inspection for erythema • Tactile inspection to monitor size of induration • 10 mm or > area of induration • Consider positive and must be referred
Tuberculosis Diagnostic exams • PPD • Mantoux skin test • > 10mm in diameter • induration • Indicates: • Latent TB • Read • 48-72 after • Intradermal: 15-degrees • Do not rub
Confirmation of Disease • Positive reaction does not necessarily mean active disease. • May indicate exposure to TB • Diagnosis confirmed by: • Positive smear for AFB and • Sputum culture of Mycobacterium tuberculosis
Interventions • Combination drug therapy • Isoniazid • Rifampicin • Pyrazinamide • Ethambutol or streptomycin • Education • Must follow exact drug regimen • Proper nutrition • Reverse weight loss and lethargy • About disease
Tuberculosis Treatment • INH • Isonicotinyl Hydrazine • Isoniazid • Toxic to the liver • Rifampicin • Turns urine red • Streptomycin • Causes 8th cranial nerve damage • Acoustic nerve
CLASSIFICATION Class 0—no exposure Class 1—exposure, no infection Class 2—latent infection; no disease (positive PPD but no evidence of active TB Class 3—disease; clinically active Class 4—disease; not clinically active Class 5—suspected disease; diagnosis pending
MEDICAL MANAGEMENT Treated with chemotherapeutic agents for 6-12 months Resistance increasing. May be primary, secondary, or multidrug resistant. Primary—resistance to one of first line drugs in those who have not had prior treatment Secondary—resistance to one or more anti-TB drugs in patientsundergoing tx Multidrug resistance—resistance to two agents, INH and Rifampicin.
Tuberculosis Complications • Pleurisy • Pericarditis • Meningitis • Bone infections • Malnutrition • Drug-toxicity
Tuberculosis Nursing Dx • Impaired gas exchange • Ineffective airway clearance • Anxiety • Knowledge deficit • Alt. nutrition
Tuberculosis Preventative measures • Clean well ventilated living areas • Resp. isolation • Vaccine? • BCG • Does not prevent TB • Causes a + PPD • If exposed take • INH
Tuberculosis Summary • Chronic bacterial infection spread through the air • Fever, chills, sweating while sleeping, persistent cough, coughing up blood or sputum • Multi-drug-resistant tuberculosis MDR TB • Use proper PPE and get PPD test if exposed