Pneumonia
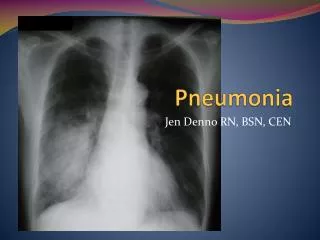
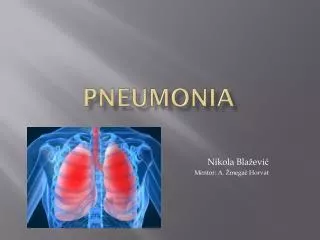
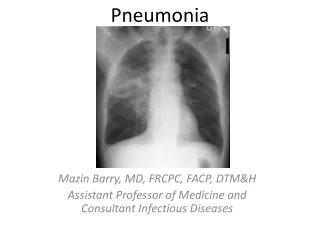
Pneumonia. Definition. • Pneumonia is an acute infection of the parenchyma of the lung( 肺实质 ), caused by bacteria, fungi( 真菌) , virus, parasite (寄生虫) etc. • Pneumonia may also be caused by other factors

Pneumonia
E N D
Presentation Transcript
Definition • Pneumonia is an acute infection of the parenchyma of the lung(肺实质), caused by bacteria, fungi(真菌), virus, parasite(寄生虫) etc. • Pneumonia may also be caused by other factors including X-ray, chemical, allergen
Epidemiology • The morbidity and mortality of pneumonia are high especially in old people.
Etiology • There are two factors involved in the formation of pneumonia , including pathogens and host defenses.
Classification • Classification of anatomy • Classification of pathogen • Classification of acquired environment
Ⅰ.Classification by pathogen Pathogen classification is the most useful to treat the patients by choosing effective antimicrobial agents
Bacterial pneumonia (1) Aerobic Gram-positive bacteria,such as streptococcus pneumoniae, staphy- lococcus aureus, Group A hemolytic streptococci (2)Aerobic Gram-negative bacteria, such as klebsiella pneumoniae, Hemophilus influenzae, Escherichia coli (3)Anaerobic bacteria
Atypical pneumonia Including Legionnaies pneumonia , Mycoplasmal pneumonia ,chlamydia pneumonia.
Fungal pneumonia Fungal pneumonia is commonly caused by candida(念珠菌) and aspergilosis(曲菌). pneumocystis jiroveci(肺孢子虫)
Viral pneumonia Viral pneumonia may be caused by adenoviruses, respiratory syncytial virus, influenza, cytomegalovirus, herpes simplex
Pneumonia caused by other pathogen Rickettsias (a fever rickettsia), (立克次体) parasites(寄生虫) protozoa(原虫)
Ⅱ.Classification by anatomy 1. Lobar(大叶性): Involvement of an entire lobe 2.Lobular(小叶性): Involvement of parts of the lobe only, segmental or of alveoli contiguous to bronchi (bronchopneumonia). 3.Interstitial(间质性)
Classification by acquired environment • Community acquired pneumonia,CAP • (社区获得性肺炎) • Hospital acquired pneumonia,HAP ,NP • (医院获得性肺炎) • Nursing home acquired pneumonia,NHAP • (护理院获得性肺炎) • Immunocompromised host pneumonia,(ICAP) • (免疫宿主低下肺炎)
Diagnosis(诊断步骤) • Give a definite diagnosis of pneumonia • To evaluate the degree of the pneumonia • To definite the pathogen of the pneumonia
Diagnosis • History and physical examination(5W) • X-ray examination • Pathogen identification
Differentiation • Pulmonary tuberculosis • Lung cancer • Acute lung abecess • Pulmonary embolism • Noninfectious pulmonary infiltration
Pathogen identification • Sputum: More than 25 white blood cells (WBCs) and less than 10 epithelial cells. • Nasotracheal suctioning • BAL, ETA, PSB, LA • Blood culture or pleural effusion culture • Serologic testing (immunological testing) • Molecular Techniques
The principal of therapy • Select antibiotics • According to guideline
Therapy • The therapy should always follow confirmation of the diagnosis of pneumonia and should always be accompanied by a diligent effort to identify an etiologic agent. • Empiric therapy,(4-8h) • Combined empiric therapy to target therapy
It is important to evaluate the severity degree of pneumonia • The critical management decision is whether the patient will require hospital admission. It is based on patient characteristics, comorbid illness, physical examinations, and basic laboratory findings.
The diagnostic standard of sever pneumonia • Altered mental status • Pa02<60mmHg. PaO2/FiO2<300, needing MV • Respiratory rate>30/min • Blood pressure<90/60mmHg • Chest X-ray shows that bilateral infiltration, multilobar infiltration and the infiltrations enlarge more than 50% within 48h. • Renal function: U<20ml/h, and <80ml/4h
CAP (社区获得性肺炎) • CAP refers to pneumonia acquired outside of hospitals or extended-care facilities . • Streptococcus pneumoniae remains the most commonly identified pathogen. • Other pathogens include Haemophilus influenzae, mycoplasma pneumoniae, Chlamydophilia pneumoniae, Moraxella catarrhalis and ects. • Drug resistance streptococcus pneumoniae(DRSP)
Clinical manifestation • The onset is accute • Respiratory symptoms • Extrapulmonary symptoms
signs • Consolidation signs • Moist rales • Respiratory rate or heart rate
Laboratory examination • WBC • X-ray features
Diagnosis • Clinical diagnosis • Pathogen diagnosis • Evaluate the severity degree of pneumonia
Therapy • Antiinfectious therapy(Combined empiric therapy to target therapy) • Supportive therapy
Outpatient<60 years old and no comorbid diseases Common pathogens: S pneumoniaes, M pneumoniae, C pneumoniae, H influenzae and viruses A new generation macrolide A beta-lactam: the first generation cephlosporin A fluoroquinolone Empiric therapy (1)
Outpatient>65 years old or having comorbid diseases or antibiotic therapy within last 3 months Common pathogens: S pneumoniae(drug-resistant), M pneumoniae, C pneumoniae, H pneumoniae, H influenzae, Viruses, Gram-negative bacilli and S aureus A fluoroquinolone A beta-lactam / beta-lactamase inhibitor The second generation cephalosporin or combination of a macrolide Empiric therapy (2)
Inpatient : Not severely ill. Common pathogen:S pneumoniae, H influenzae, polymicrobial, Anaerobes, S aureus, C pneumoniae, Gram-negative bacilli. The second or third generation cephalosporin plus A macrolide A beta-lactam/betalactamase inhibitor. A newer fluoroquinolone Empiric therapy (3)
Inpatient severely ill Common pathogens:S pneumoniae, Gram-negative bacilli, M pneumoniae, S aureus and viruses The second or third generation cephalosporin plus A macrolide A beta-lactam/betalactamase inhibitor. A newer fluoroquinolone Vancomycin Empiric therapy (4)
Patients in ICU without Pneudomonas aeruginosa infection The second or third generation cephalosporin plus A macrolide A beta-lactam/betalactamase inhibitor. A newer fluoroquinolone Vancomycin Empiric therapy (5)
Patients in ICU with Pneudomonas aeruginosa infection A antipneudomonas aeruginosa beta-lactam/betalactamase inhibitor plus fluoroquinolone Empiric therapy (6)
HAP(医院获得性肺炎) • HAP refers to pneumonia acquired in the hospital setting. • Enteric Gram-negative organisms, S. aureus, Pneudomonas aeruginosa, ects.
The pathogen of HAP • Gram-negative bacteria (GNB) account for 55% to 85% of HAP infections • gram-positive cocci account for 20% to 30% and some other pathogens.
EPIDEMIOLOGY • General risk factors for developing HAP include age more than 70 years, serious comorbidities, malnutrition, impaired consciousness, prolonged hospitalization, and chronic obstructive pulmonary diseases.
EPIDEMIOLOGY • HAP is the most common infection occurring in patients requiring care in an intensive care unit (ICU), with incidence rates ranging from 6% up to 52%, much higher than the 0.5% to 2% incidence reported for hospitalized patients as a whole. This increased incidence is due to the fact that patients located in an ICU often require mechanical ventilation, and mechanically ventilated patients are 6 to 21 times more likely to develop HAP than are nonventilated patients. Mechanical ventilation is associated
PATHOGENESIS • Aspiration :Microaspiration of contaminated oropharyngeal secretions seems to be the most important of these factors, as it is the most common cause of HAP. • Inhalation • Contamination
Clinical manifestations • The onset is acute or insidious • Respiratory symptoms • Physical signs
Laboratory examinations • Chest X-ray
diagnosis • Clinical diagnosis • Pathogen diagnosis • Evaluate the severity degree of pneumonia
Treatment (1) • Antibiotic therapy: antimicrobial therapy begin promptly because delays in administration of antibiotics have been associated with worse outcomes. • The initial selection of an antimicrobial agent is almost always made on an empiric basis and is based on factors such as severity of infection, patient-specific risk factors, and total number of days in hospital before onset.
Treatment (2) • All empiric treatment regimens should include coverage for a group of core organisms that includes aerobic gram negative bacilli (Enterobacter spp, Escherichia coli, Klebsiella spp, Proteus spp, Serratia marcescens, and Hemophilus influenzae) and gram-positive organisms such as Streptococcus pneumoniae and Staphylococcus aureus.
Treatment (3) • In patients with mild or moderate infections and no specific risk factors for resistant or unusual pathogens, monotherapy with a second-generation cephalosporin such as cefuroxime; a nonpseudomonal third-generation cephalosporin such as ceftriaxone; or a beta-lactam/beta-lactamase inhibitor such as ampicillin/sulbactam, ticarcillin/clavulanate, or piperacillin/tazobactam may be appropriate. • For patients in this low-risk category who have an allergy to penicillin, it is appropriate to initially use a fluoroquinolone
Treatment (4) • Patients with severe infections with specific risk factors should have broadened empiric coverage. • Combination therapy should be employed in these cases because of the high rate of acquired resistance among these organisms. • Appropriate combinations for this group of patients include an aminoglycoside or ciprofloxacin in addition to a beta-lactam with antipseudomonal coverage. • Additionally, vancomycin should be considered if the patient has risk factors that suggest methicillin-resistant Staphylococcus aureus could be a pathogen.