Claims Follow-up
140 likes | 374 Vues
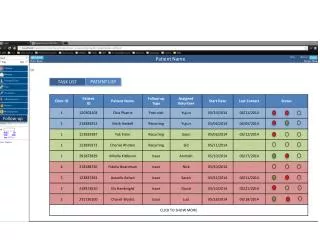
Claims Follow-up. Claim Status Balance Billing Appeals. Once a claim has been filed… . If there is no response within 45 days, contact the plan for claim status or mail a claim tracer form requesting status. There are four general claim statuses:

Claims Follow-up
E N D
Presentation Transcript
Claims Follow-up Claim Status Balance Billing Appeals
Once a claim has been filed… • If there is no response within 45 days, contact the plan for claim status or mail a claim tracer form requesting status. There are four general claim statuses: • Rejected (not processed due to clerical errors. Always correct and resubmit rejected claims!) • Pending (delayed processing – get the reason!) • Denied (payment refused) • Paid (payment made)
The Explanation of Benefits • When a claim has been processed, the insurance company sends and EOB to notify you of the payment amount of denial reason. • Read the EOB carefully to understand the reasons for any unpaid charges. • If you are still unsure, contact the insurer for further explanation.
Credits and Balance Billing • Any insurance payments should be credited to the patient’s account. • Any contractual adjustments should be credited or written-off the patient’s account. • Any deductible, co-insurance or co-payments should be billed to the patient.
Other unpaid amounts… • Do not automatically bill the patient for unpaid charges. Carefully review the EOB for the reason the charges were not paid. • Sometimes these may be contractual adjustments • Sometimes these may be items that need to be appealed for additional insurance payment.
Unpaid Charges - Denials A claim or charge is denied when the insurance refuses to pay. Examples include: • No Eligibility (e.g., coverage ended, coverage not yet begun, etc.) • Policy Exclusion (e.g., cosmetic surgery, pre-exisiting, untimely filing, etc.) • Lack of Medical Necessity or no Authorization (don’t forget to put authorization numbers in block 23) • Duplicate billing (sometimes results from a missing RT, LT, 76 or 77 modifier) • Unbundling (this often results from missing 24, 25, 57 or 59 modifier)
Unpaid Charges • Underpayments are partial denials or reductions in payment. • An underpayment can result from: • Use of the wrong fee schedule or contract rate • Coding or processing error (for example, incorrect use of code or modifier) • Partial denial or application of penalty or discount
Claims Appeals An Appeal is a request for insurance payment of items that were denied or underpaid. • To file an appeal you need to send: • An explanation of how the charge should have been paid and why it should have been paid that way. • A copy of the bill or a corrected bill and the EOB. • Any evidence such as eligibility verification, proof of timely filing, medical records, etc.
Examples of Appeals Arguments • A plastic surgery was incorrectly denied as cosmetic when in reality it was performed as the result of an accident or as reconstruction after a medically necessary surgery such as a mastectomy. • A visit to the doctor was incorrectly denied as bundled into the global surgery period when it was for a condition completely unrelated to surgery. • An emergency service was denied as out of network or not authorized, when obtaining authorization or seeing a network provider would have been impossible or the delay in treatment would possibly have resulted in harm to the patient.
Persistence Pays Off • If the appeals decision is not satisfactory, you have the right to appeal at a higher level. • If you believe the insurance company is “in the wrong,” you can continue to appeal at higher levels until you exhaust your appeals rights. • Higher level appeals are generally reviewed by nurses, doctors or attorneys who may have better medical/legal judgment than the original reviewer.
Regulatory Agencies • When you exhaust your right of appeal or if you notice an unfair insurance practice, you can file a complaint with the appropriate regulatory agency. • Dept. of Insurance: Handles only Indemnity Insurance claims (no HMO or PPO plans). • Dept of Managed Health Care: Handles claims for HMO, PPO or POS insurance plans.
Regulatory Agencies (cont’d) • Dept. of Labor: Handles self-insured group health plans where the employer pays claims out of a bank account funded with employee contributions (rather than paying insurance premiums). These funds are regulated under the Employee Retirement Income Security Act (ERISA).
Medicare Appeals • Medicare is a government plan and is not regulated by the above agencies. • Medicare has five levels of appeal. Some of the higher levels have minimum dollar thresholds. • Each level has a specific deadline for appeals filing. The rules for the appeals process will appear on the Medicare EOB or Medicare Appeals determination letter.