Benign Prostatic Hyperplasia
Benign Prostatic Hyperplasia. DR.Gehan Mohamed. Normal Prostate Anatomy. Prostate weights ~20g Measures ~3 by 4 by 2 cm Apex = inferior portion of prostate, continuous with striated sphincter. Base = superior portion and continuous with bladder neck. PROSTATE histology.

Benign Prostatic Hyperplasia
E N D
Presentation Transcript
Benign Prostatic Hyperplasia DR.Gehan Mohamed
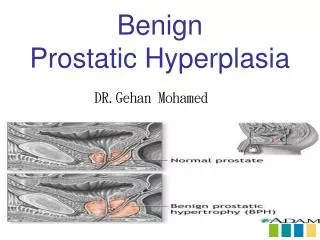
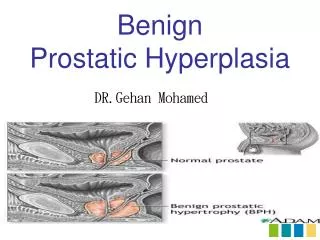
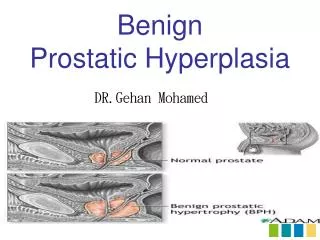
Normal Prostate Anatomy • Prostate weights ~20g • Measures ~3 by 4 by 2 cm • Apex = inferior portion of prostate, continuous with striated sphincter. Base = superior portion and continuous with bladder neck.
PROSTATE histology Prostatic tissue is formed of two components : • fibromuscular tissue (30%) • glandular epithelial cells (70%)
Normal histology of prostate: formed of glands and fibromuscular stroma
Normal histology of the prostate formed of glands and stroma glands: lined by two layers of cells which are inner cuboidal cells and outer basal cells stroma :fibro muscular stroma
Prostate zones Central zone (CZ) • Cone shaped region that surround the ejaculatory ducts (extends from bladder base to the verumontanum) • Only 1-5% of prostate cancer from this region . Peripheral zone (PZ) • Posteriolateral prostate • Majority of prostatic glandular tissue • Origin of up to 70% of prostate adenocarcinoma Transitional zone (TZ) • Surrounds the prostatic urethra • Commonest site for benign prostatic hyperplasia.
What causes BPH? n BPH is part of the natural aging process, like getting gray hair or wearing glasses BPH cannot be prevented BPH can be treated n n
Half of all men over the age of 60 will develop an enlarged prostate. By the time men reach their 70’s and 80’s, 80% will experience urinary symptoms But only 25% of men aged 80 will be receiving BPH treatment
BPHProposed Etiologies • 1-alterations in the testosterone/estrogen balance:enlarged prostate may be caused by lower levels of testosterone (male hormone) production in middle to old age. As men age, the levels of testosterone in their blood decreases, leaving a higher proportion of estrogen (female hormone), so a higher amount of estrogen within the prostate gland can increase activity that promotes cell growth. • 2-Induction of prostatic growth factors. • 3- Increased stem cells/decreased stromal cell death
Benign Prostatic Hypertrophy (BPH)—Pathophysiology • Common in older men; varies from mild to severe • Change is actually hyperplasia of prostate • Nodules form around urethra • Not change to cancer prostate. • Rectal exams reveals enlarged gland • Incomplete emptying of bladder leads to infections • Continued obstruction leads to distended bladder, dilated ureters, renal damage • If significant, surgery required
Abnormal Voiding (obstructive) symptoms Hesitancy Weak stream Straining to pass urine Prolonged micturition Feeling of incompletebladder emptying Urinary retention Storage (irritative or filling) symptoms Urgency:an increasingly strong desire to void) Frequency Nocturia Urge incontinence What’s Lower Urinary Tract Symptoms secondary to prostatic urethra obstruction? LUTS is not specific to BPH – not everyone withLUTS has BPH and not everyone with BPH has LUTS
BPH—Signs and Symptoms • Initial signs • Obstruction of urine flow • Hesitancy : delay between trying to urinate and the flow actually beginning. • dribbling • decreased force of urine stream • Incomplete bladder emptying • Frequency, • nocturia : need to urinate at night • recurrent Urinary Tract Infections
BPH complications • hypertrophy of the prostatedetrussor muscle of the bladder undergo hypertrophy to overcome the obstruction in the prostatic urethra. Later on decompensation occur . • Increase pressure inside bladderdiverticulaformationincreasing urine retentionhydronephrosis renal failure.
Symptom assessment • Digital rectal examination(DRE) • inaccurate for size but can detect shape and consistency • Prostate Volume (PV) determination by ultrasonography • Urodynamic analysis • Measurement of prostate-specific antigen (PSA) • high correlation between PSA and PV, • men with larger prostates have higher PSA levels • PSA is a predictor of disease progression and screening tool for Cancer Prostate. • as PSA values tend to increase with increasing Prostatic Volume and increasing age, PSA may be used as a prognostic marker for BPH. Diagnosis of BPH
BPH : show marked hyperplasia in the number of prostatic glands
When should BPH be treated? BPH needs to be treated ONLy IF: Symptoms are severe enough to bother the patient and affect his quality of life Complications related to BPH n n
Treatment options Medication :α blockers - relax the smooth muscle of prostate and provide a larger urethral opening Surgical approaches 1- Transurethral resection of the prostate (TURP) 2- Open simple prostatectomy n n n
Indication of surgical intervention • Acute urinary retention • Gross hematuria • Frequent urinary tract infection (UTI) • Vesical stone • BPH related hydronephrosis or renal function deterioration • Obstruction
Differential Diagnosisof BPH(i.e from other causes of urinary obstruction) • Urethral stricture • Bladder neck contracture • Carcinoma of the prostate • Carcinoma of the bladder • Bladder calculi • Urinary tract infection and prostatitis • Neurogenic bladder