Vascular Surgery Occlusive Peripheral Vascular Disease
870 likes | 1.75k Vues
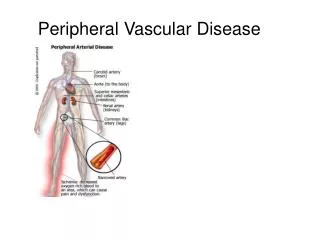
Vascular Surgery Occlusive Peripheral Vascular Disease. Adrian P. Ireland BA(mod) MB MCh BAO FRCS(I). Beaumont Theatre Nurses 13 Jan 2004. Occlusive Peripheral Vascular Disease. Peripheral vascular disease Includes any disease affecting the peripheral vascular system

Vascular Surgery Occlusive Peripheral Vascular Disease
E N D
Presentation Transcript
Vascular SurgeryOcclusivePeripheral Vascular Disease Adrian P. Ireland BA(mod) MB MCh BAO FRCS(I) Beaumont Theatre Nurses 13Jan 2004
Occlusive Peripheral Vascular Disease • Peripheral vascular disease • Includes any disease affecting the peripheral vascular system • Occlusive – essentially blocked arteries
Outline • Review of the circulation • Pathogenesis of blocked arteries • Manifestations of blocked arteries • Monitoring the circulation • Occlusive peripheral vascular disease • Acute Ischemia • Chronic Ischemia
Review Of Circulation • Cells need supply of nutrients and removal of by products • In a unicellular organism this may occur via the cell membrane into say a pond or sea • Multicellular organisms need a circulatory system
William Harvey (1578-1657) On the Motion of the Heart and Blood in Animals (1628)
Problem With Blocked Circulation • Tissues lack adequate supply of nutrients • Tissues suffer build of toxic by products • May cause symptoms and signs particularly when more blood flow is required; • To muscles during exercise • To tissues that are injured (more blood needed)
Pathogenesis Of Blocked Arteries • Atherosclerosis • Genes, hyperlipidemias • Lifestyle • Smoking • High fat diet • Lack of exercise • Co-morbidities • Diabetes, hypertension, hypothyroidism, homocysteine
Manifestations Of Blocked Arteries • Depends on circulation affected • Heart • Stable angina, unstable angina, myocardial infarction • Brain • Transient ischemic attact, stroke • Kidney • Hypertension, renal failure • Legs • Claudication, rest pain, necrosis
Principal causes of death in Ireland (males) Report on Vital Statistics Central Statistics Office Ireland, 1995
Annual Deaths Due toCerebrovascular Disease andIschemic Heart Disease Report on Vital Statistics Central Statistics Office Ireland, 1995
Manifestations Of Blocked Arteries • Depends on speed of development of blockage • Slow blockage • Permits development of collateral blood supply so that occlusion may be asymptomatic • Rapid blockage • No time for development of collaterals • Symptoms/ signs depend on adequacy of preexisting collaterals
Monitoring Circulation • Mottling, colour, temperature, movements, sensation • Palpable pulses, doppler signals • Non invasive pressure studies (Doppler) • Duplex imaging • Angiography (IAA, DSA, MRA)
Occlusive Peripheral Vascular Disease • Classification based upon clinical presentation • Acute ischemia • Chronic ischemia • Anatomic classifcation based upon site(s) of disease
OPVD Anatomic Classification • Aorto-iliac • Le-Riche • Femero-popliteal • Tibio-peroneal
Effects Of Acute Ischemia • Reduced blood flow • Pulseless, pallor, perishing cold • Nerve ischemia • Pain, paralysis, Paresthesia • Muscle ischemia • Rhabdomyolysis • Compartment syndrome • Ischemia reperfusion syndrome
Compartment Syndrome • Pathophysiology • Diagnosis • Management
Compartment SyndromePathophysiology • Strong fascia encases the limb to aid muscle function and return of venous blood • Injury results in swelling • Swelling raises pressure • Pressure occludes lymphatic return, then venous return, then arterial inflow • Result is dead or severly damaged tissues due to pressure and ischemia
Compartment Syndrome Diagnosis • Strong index of suspicion • Nature of injury and duration of ischemia • Clinical manifestations • Nerve and muscle dysfunction • Decreased perfusion • Tense compartment • May measure compartment pressure as adjunct to treatment > 40 mm hg
Compartment SyndromeManagement • Fasciotomy
Acute Ischemia • Causes • Thrombosis • Embolism • The P’s • Thrombosis or embolism? • Clinical assessment of severity • Clinical algorithm
Causes of Acute Ischemia • Trauma • Thrombosis • Embolism • Small print • Aneurysm • Thrombophilia • Paradoxial embolism • Anatomic variation • Csytic adventitial disease
Thrombosis • Occlusive atherosclerosis • Aneurysm • Malignancy • Thrombophilia
Embolism • Macro-embolism • arterial side • venous side (patent foramen ovale) • Micro-embolism • ulcerated atherosclerotic plaques • aneurysm
The P ’s • No flow in artery • Pallor • Pulse absent • Perishing cold • Nerve becomes ischemic • Pain • Paresthesia / anesthesia • Paralysis
Clinical Assessment of Severity • Viable no immediate threat • Threatened • Marginally ok if treated promptly • Immediately ok if treated immediately • Irreversible dead leg
Irreversible Ischemia • Sensory loss Profound,anaesthetic • Muscle weaknessProfound, paralysis • Arterial doppler Inaudible • Venous doppler Inaudible Amputation
Viable no immediate threat • Sensory loss None • Muscle weakness None • Arterial doppler Audible • Venous doppler Audible • Restore perfusion
Clinical Assessment of Severity • Viable No immediate threat • Threatened • marginally Ok if treated promptly • immediately Ok if treated immediately • Irreversible Dead leg
Threatened Marginally • Sensory loss Minimal (toes) to none • Muscle weakness None • Arterial doppler Inaudible • Venous doppler Audible • Restore perfusion
Threatened Immediately • Sensory loss More than toes, Pain • Muscle weakness Mild to moderate • Arterial doppler Inaudible • Venous doppler Audible Restore perfusion
Practical Questions • Is this ischemia? (DDx stroke, TIA, cord) • Is the limb viable, threatened or lost? • If threatened how long can reperfusion be delayed? • Is there a need for duplex or angiography? • Should the patient be immediately heparinised?
acute non traumatic ischemia Irreversible Threatened Viable Clear embolus ?Thrombosis Duplex Adequate Inadequate Angiogram Treat Amputation Embolectomy Thrombolyse +/- PTA Reconstruct
Prognosis • Embolism • Overall 60% dead within three years • One episode 15-20% mortality (in hospital) • Two episodes 40% mortality (in hospital) • Thrombosis • Overall 40% dead within three years
LaFontaine Classification Stage 1 claudication Stage 2 rest pain Stage 3 necrosis/ulceration
Prognosis in Claudicants • About 15% will progress to requiring revasculartion or amputation • Much higher risk of death from IHD and stroke • Rule out diabetes, hypertension and hypercholesterolemia • Exercise, Smoking cessation, Aspirin and a Statin + control of risks
Re-Vascularisation ? • Risk factor control, aspirin, statin • Pain control • Dressing • Sympathectomy (chemical, surgical) • Iloprost • Angioplasty +/- Stent (? Drug elute) • Surgical
Surgical Re-Vascularisation • Embolectomy and Thrombolysis • Patchplasty (synthetic/ autogenous) • Endarterectomy (open/closed/eversion) • Bypass with synthetic material • Bypass with autogenous material
Definition Of Critical Ischemia • Presence of tissue loss OR • Rest pain with ankle pressure less than 50 mm Hg FOR • More than 2 weeks
Acute on Chronic Bypass
J.C. 68 year old male • Emergency admission 24.3.2000 to vascular service SVUH, via A/E • Ischemic right foot