Skeletal muscle contraction
290 likes | 424 Vues
Explore the mechanisms of skeletal muscle contraction, including the sliding filament theory, ATP generation, and factors leading to muscle fatigue. Delve into the role of actin, myosin, and ATP in the contraction cycle and learn about force production, tension, and energy requirements. Discover how muscle shortening, Z discs, sarcomeres, and cross-bridges contribute to muscle movement and contraction. Gain insights into the sources of ATP, including phosphocreatine, glucose, fatty acids, and protein catabolism. Uncover the complexities of muscle fatigue through factors like intensity, duration of activity, metabolism, ions, and neurotransmitters. Understand how glycolysis, oxidative phosphorylation, and beta-oxidation fuel muscle activity, and learn how physiological and psychological aspects influence fatigue.

Skeletal muscle contraction
E N D
Presentation Transcript
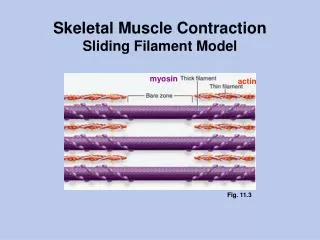
Skeletal muscle contraction • Contraction, force and tension • Sliding Filament Theory of Contraction • Contraction cycle • Regulation of the contraction cycle
Muscle contraction • Movement or resist a load (force) • Load is the weight or force that opposes the contraction of a muscle • Tension is the force created by a muscle • Need ATP to generate tension
Observations during muscle contraction Muscle shortens when it moves a load. (When muscle contracts, it does not always shorten)
Observations during muscle contraction: A band does not shorten during contraction.
Sliding filament theory of contraction: movement and force Resting length How about force without movement?
During contraction • Z discs move closer together • Sarcomere shortens • A band same length • I band reduced • H band reduced
What pushes the actin filaments into the myosin? • Cross-bridges link myosin to actin • Power stroke: myosin head binds to actin myosin head release actin. Repeated many times. • Myosin molecules are flexible • ATP causes movement of myosin molecules
Myosin • A motor protein • Converts chemical bond energy of ATP to mechanical energy of motion • Each myosin as ATPase • Energy from ATP hydrolysis is stored as potential energy in the myosin molecule, and is used to create the power stroke.
Why don’t actin and myosin continuously bind together? • ATP is usually available • Actin’s binding site for myosin is revealed only during cross-bridge (binding). • During relaxation, actin’s binding site for myosin is concealed
Energy for skeletal muscle contraction • ATP sources • The many causes of muscle fatigue • Classification of skeletal muscle fiber types
ATP and muscle contraction • Need ATP for • Cross-bridge formation, power stroke (myosin ATPase) • Ca++ transport to SR (Ca++ ATPase) • Na+/K+ transport across sarcolemma (Na+/K+ ATPase)
Sources of ATP • ATP pool • Phosphocreatine. • At rest, ATP phosphorylates creatine. • During exercise, creatine kinase (creatine phosphokinase) moves phosphate from phosphocreatine to ATP
Sources of ATP • Glucose (glycolysis) to pyruvate citric acid cycle oxidative phosphorylation (about 30 ATP per glucose molecules) • Anaerobic glycolysis: glucose lactic acid (2 ATP per glucose molecule)
Sources of ATP • Beta oxidation of fatty acids. Fatty acids are converted to acetyl CoA citric acid cycle in the mitochondria, need oxygen • Slow • During light exercise
Sources of ATP • glucose catabolism during heavy exercise • carbo loading builds up glycogen stores • Protein catabolism during starvation
Fatigue • Muscle is no longer able to generate sustained expected power output • A variety of contributing factors • depends on the degree of muscle activity
Fatigue: contributing factors • Intensity of muscle activity • Duration of muscle activity • Aerobic/anaerobic metabolism • Muscle composition • Fitness level • Ions • Nutrients • Neurotransmitter
Fatigue during extended submaximal exertion • Not ATP shortage • Glycogen depletion may affect Ca++ release from SR
Fatigue during short duration maximal exertion • Lots of inorganic phosphate from ATP hydrolysis • may slow P release from myosin:ADP:Pi • slows power stroke • Acidosis may inhibit some enzymes
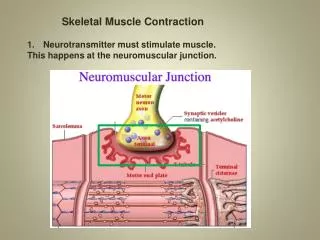
More factors for muscle fatigue • K+ : intracellular K+ lowered during repetitive action potentials affects Ca++ release channels on SR membrane • Acetyl choline depletion at the myoneural junction low end-plate potential (disease)
More factors for muscle fatigue • CNS: • Subjective feelings preceding physiological fatigue • Acidosis may influence perception of fatigue