Cardiac Output and Venous Return
541 likes | 1.76k Vues
Cardiac Output and Venous Return. Dr. Amel Eassawi. OBJECTIVES. The student should able to: List the normal at rest values for cardiac output, cardiac index, heart rate, stroke volume, end-diastolic volume, end-systolic volume and ejection fraction.

Cardiac Output and Venous Return
E N D
Presentation Transcript
Cardiac Output and Venous Return Dr. AmelEassawi
OBJECTIVES The student should able to: • List the normal at rest values for cardiac output, cardiac index, heart rate, stroke volume, end-diastolic volume, end-systolic volume and ejection fraction. • List the factors which affect cardiac output and describe the role of each in the modulation of the cardiac output. • List the factors which affect venous return and describe the role of each in the modulation of cardiac output. • Discuss the interplay between stroke volume and heart rate in regulating the cardiac output. • Describe the Frank-Starling law of the heart. • List the methods used to measure cardiac output • Recognize the importance of the venous valves and of the venous pump phenomena. • List the physiological and pathological conditions that affect the cardiac output.
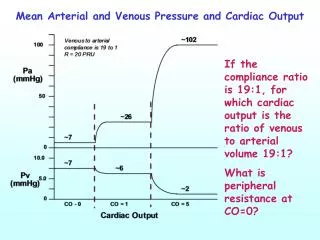
CARDIAC OUTPUT Cardiac Output: The volume of the blood pumped out by each ventricle per minute. About 5 – 5.5 L/min Cardiac Output = Heart rate × Stroke volume = 70 beats/min × 70ml/beat = 4900 ml/min ≈ 5liters/min Cardiac output of each ventricle is the same. Cardiac output increases during exercise, depending on the type of exercise by increasing stroke volume and heart rate(in trained athlete during heavy exercise recorded increase up to 40 L/min). Cardiac Reserve: The difference between cardiac output at rest and the maximum volume of blood the heart can pump per minute. Cardiac Index: Sometimes C.O. is expressed as a cardiac index . Cardiac output per minute per square meter of body surface area (BSA). C.I. ( L/min/M2) = C.O. (L/min) / BSA (M2) Normal Cardiac Index = 3.2 Liter /min/M2.
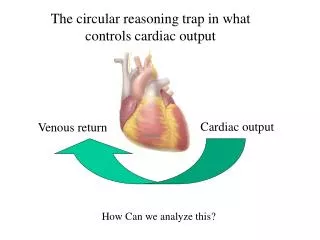
Factors controlling cardiac out put The two determinants of cardiac output is SV and HR
Factors controlling cardiac out put Stroke Volume (SV): Volume of blood pumped out by each ventricle per beat. It is about 70 - 80 ml. Stroke volume (SV) = EDV – ESV End Diastolic Volume (EDV): Volume of blood in each ventricle at the end of diastole. It is about 120 – 130 ml. End Systolic Volume (ESV): Volume of blood in each ventricle at the end of Systole. It is about 50 to 60 ml Ejection fraction (EF): Its the percentage of ventricular end diastolic volume (EDV) which is ejected with each stroke.
Factors controlling cardiac out put EF = Ejection fraction is good index of ventricular function
Factors controlling cardiac output Two types of control influence stroke volume • Intrinsic Control: Related to venous return 2. Extrinsic Control: Related to extent of sympathetic stimulation of heart Both factors( Intrinsic and Extrinsic ) increase stroke volume by increasing the strength of heart contraction.
Factors controlling cardiac output Intrinsic control of stroke volume: • Direct correlation between end diastolic volume & stroke volume. • This depends on length tension relationship of cardiac muscle. • Cardiac muscle resting cardiac length is less than optimum length at which maximum tension develops. • Therefore increasing the cardiac muscle fiber length closer to optimum length, increases the contractile tension of the heart on the following systole .
Frank Starling Law of the Heart • Frank Starling Law of the Heart - the heart will contract with greater force when preload (EDV) is increased. • Preload: diastolic filling volume of the left ventricle (EDV) reflects stretch of the cardiac muscle cells. • Afterload: resistance to ventricular emptying during systole (the amount of pressure the left ventricle must generate to squeeze blood into the aorta. • Myocardial Contractility: the squeezing contractile force that the heart can develop at a given preload.
Factors controlling cardiac output Sympathetic stimulation shift the frank starling’s curve to left
Effects of an Increase in Preload on Left Ventricular Pressure Volume Loop ↑ Ejection Pressure 120 Left Ventricular Pressure (mmHg) ↑ SV ↑ EDV ↑ EDP 6 40 140 Volume (ml)
Effects of an Increase in Afterload on Left Ventricular Pressure Volume Loop ↑ ESV ↑ ESP 120 Left Ventricular Pressure (mmHg) ↓ SV 6 40 140 Volume (ml)
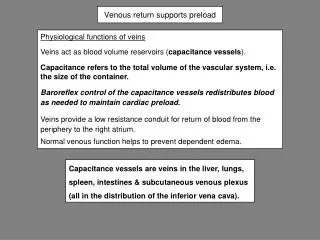
VENOUS RETURN Factors Affect Venous Return 1. Increased Blood Volume: Veins are capacitance vessels and hold about 60 to 70% of blood, when veins store less blood, more blood is returned to the heart. 2. Skeletal Muscle Pump: Muscle contraction compresses the veins. This external venous compression decreases venous capacity and increases venous pressure and moves blood towards the heart. 3. Respiratory Pump: During respiration, intra-thoracic pressure decreases and is less than atmospheric pressure [-5 mmHg]. This negative chest cavity pressure squeezes blood from the lower veins to the chest, increasing venous returns
VENOUS RETURN 4. Increased Sympathetic Activity (Vasoconstriction): Sympathetic Stimulation causes vasoconstriction, which increases venous pressure and drives more blood to right atrium, therefore, more venous returns and increase EDV. 5. Cardiac Suction Effect: Heart plays role in its own filling. During ventricular contraction, AV valves are pulled downward enlarging atrial cavities. Atrial pressure drops below 0 mmHg and increases venous returns. 6. Venous Valves: In the veins, blood can be driven forward only as large veins have one way valve placed at 2 to 4 cm intervals. These valves prevent back flow of blood that tends to occur when a person stands up.
Methods for Determining Cardiac Output • Fick Principle • Indicator-dilution Technique • Electromagnetic Flowmeter • Magnetic Resonance Imaging (MRI) • Doppler Ulrasound Method • Angiogram • Echocardiogram
FICK PRINCIPLE Output of Left Ventricle Oxygen Uptake by lungs ml/min = AO2 - VO2 200 ml / min 200 ml / L – 160 ml / L Art blood – Venous blood [Pul artery] 200 ml/min 40ml / liter = 5 L/min = =
ANGIOGRAM DIASTOLE SYSTOLE
ECHOCARDIOGRAM DIASTOLE SYSTOLE
Conditions which alters the cardiac output Physiological • Muscular exercise • Emotional states • Posture • Pregnancy Pathological • Increase in cardiac out put • Hyperthyroidism • Anemia • Fever • Decrease in cardiac out put • Hypothyroidism • Myocardial damage & cardiac failure • Valvular heart diseases • Arrhythmias • Hemorrhage & shock
HEART FAILURE Heart Failure: • Inability of the heart to pump cardiac output, sufficient to keep pace with the body’s demand. • There may be left ventricular failure or right ventricular failure or biventricular failure. • Most common cause of heart failure is 1. Heart Attack or Myocardial Infarction 2. Working against Increased afterload e.g. hypertension or aortic valve stenosis. Left Ventricular Failure: Pulmonary congestion or pulmonary edema occurs which causes decrease exchange of O2 and CO2 in the lungs. Right Ventricular Failure: Due to back pressure, there is engorgement of neck veins, peripheral edema, liver enlargement.
References • Human physiology, Lauralee Sherwood, seventh edition. • Text book physiology by Guyton &Hall,11th edition. • Physiology by Berne and Levy, sixth edition.