Endocrine System
Endocrine System. Chapters 21, 22, 23, 24, 26. Endocrine System. Endocrine system regulates essential activities of the body Metabolism of nutrients Reproduction Growth and development Adapting to change in internal and external environments. Major Endocrine Organs. Hypothalamus

Endocrine System
E N D
Presentation Transcript
Endocrine System Chapters 21, 22, 23, 24, 26
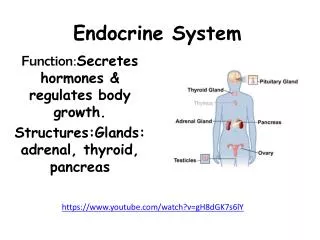
Endocrine System • Endocrine system regulates essential activities of the body • Metabolism of nutrients • Reproduction • Growth and development • Adapting to change in internal and external environments
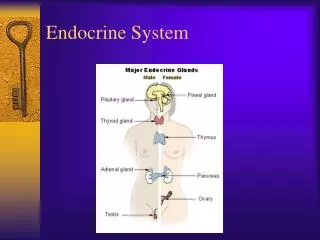
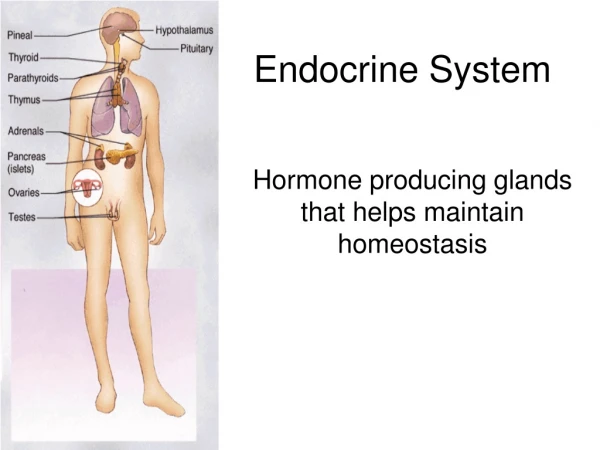
Major Endocrine Organs • Hypothalamus • Pituitary gland • Thyroid gland • Parathyroid glands • Pancreas • Adrenal glands • Ovaries • Testes
Local Tissue Hormones Endocrine like cells in the • Gastrointestinal mucosa – hormones that aid in digestion • Kidneys – erythropoietin – hormone that stimulates bone marrow to produce RBC’s • White blood cells – cytokines – inflammation • Body tissues – prostaglandins and leukotrienes
Tumors • Specific tumors produce hormones • Lungs - ACTH • Kidney – parathyroid hormones Elevation of these hormones would aid in diagnosing the tumors
Endocrine System and Nervous System • Closely connected • Work together to regulate body function • Main connecting link is the hypothalamus – responds to nervous system stimulation by producing hormones • Hypothalamus will initiate the hormone response
What is the Endocrine System? • Endocrine system is in charge of the body processes that happen slowly, such as cell growth. • The nervous system has to do with the faster processes, like breathing and body movement.
Hormones • The bodies chemical messengers • Different hormones circulate throughout the blood stream, but only affects the cells that are genetically programmed to receive and respond to the message.
Hormones • Hormones modify rather than initiate cellular response – stimulated by the hypothalamus / pituitary gland
Hormone Pharmacokinetics • Water soluble hormones, protein-derived hormones have a short duration of action and are inactivated by enzymes in liver and kidneys. • Lipid soluble hormones and thyroid hormones have a longer duration because they are bound to plasma protein – they are broken down in the liver and excreted in bile or urine.
Water Soluble Hormones • Do not enter the target cells – form weak bonds with receptor sites on the cell membrane. • Sometimes called the “second messenger” • Examples: glucagon, adrenalin and parathyroid hormones. • Hormones are be released as needed.
Lipid Soluble Hormones • Steroid and thyroid are constantly present in the blood.
Cellular Response • Up-regulation – receptors may be increased if there are low levels of hormone. • Down-regulation – hormones may be decreased when there are excessive amounts of hormone.
Hormone Disorders • Abnormal secretion and function of hormones can impair physical and mental health. • Malfunction of endocrine organ – • Hypersecretion (too much) • hyposecetion (too little)
What Can Influence Hormone Levels? • Stress • Infection • Fluid balance • Minerals in blood • Structural changes in glands
Glandular Hypofunction • Congenital defect - infant • Damaged or destroyed – inflammation - tumor • Atrophy of gland due to aging – geriatric population • Receptor defects • Intracellular processes malfunction – cellular level
Hormonal Drugs • Potent drugs that produce widespread therapeutic and adverse side effects. • Given when there is hypofunction of a gland. • Need to replace what would naturally be produced by the body.
Two Common Hormonal Drugs • Pancreas dysfunction – insulin needed to regular blood sugar levels. • Diabetes type I and II • Thyroid dysfunction • hypothyroid conditions – need replacement of hormone • hyperthyroid may need to give medication that inhibits excess thyroid produced
In a nut-shell • With hormones the body needs a consistent amount to properly function – too much or too little can be a problem
Hypothalamic and Pituitary Chapter 22
Hypothalamus • Interacts with the pituitary gland to control most metabolic functions of the body. • Controls secretions of the pituitary gland.
Pituitary Gland • The pituitary gland is sometimes called the "master" gland of the endocrine system, because it controls the functions of the other endocrine glands. The pituitary gland is no larger than a pea, and is located at the base of the brain. The gland is attached to the hypothalamus (a part of the brain that affects the pituitary gland) by nerve fibers.
Anterior Pituitary Gland • Anterior pituitary gland – • Growth hormone • Adrenal cortex – ACTH – glucocorticoids • TSH – thyroid stimulating hormone • FSH – follicle stimulating hormone – ovary – estrogen and progesterone • LH - luteinizing hormone – stimulates ovulation • Prolactin – breast tissue – milk production • Testosterone – testes
Medical Conditions • Growth hormone therapy in pediatrics • Delayed development of secondary sexual characteristics - adolescent • Infertility • Thyroid conditions
Growth Hormone Deficiency • In a child what do you think you might see? • Height versus weight • Growth curve • What influences growth? • How do you tell the dug is working?
Posterior Pituitary Gland • ADH – antidiuretic hormone – kidney – regulates water balance • Oxytocin – uterus and breast – labor and breast feeding
Posterior Pituitary Dysfunction • Desmopressin (DDAVP) or vasopressin – synthetic ADH (antidiuretic hormone) • Clinical Diagnosis: diabetes insipidus – characterized by high output of dilute urine – can be idiopathic (do not know the cause) – can occur after head trauma, with tumor of hypothalamus or posterior pituitary • Importance of intake and output and specific gravity
Dysfunction of Posterior Pituitary • Remember the pituitary gland directs function of the antidiuretic hormone in the kidneys which has to do with normal fluid balance.
Specific Gravity • Concentration of urine is measured by density called specific gravity. • Normal specific gravity is around 1.010 • A high specific gravity would reflect dehydration or hypovolemia. • A low specific gravity would reflect over-hydration or disease process such as diabetes insipidus.
Intake and Output • Why important? • How besides urine output can a person lose fluid? • Basic measures of intake and output – ml’s or cc’s
Nursing Considerations • Observe for headache, nasal congestion, nausea • Monitor blood pressure – drug may cause increase in blood pressure • Most serious side effect is water retention and hyponatremia
Posterior Pituitary Hormone • Oxytocin – promotes uterine contractibility • Clinical uses: After delivery of infant and placenta in obstetrics. • In small dosages to stimulate or induce labor in a pregnant woman • When you will be doing your obstetrical rotation you will see oxytocin (Pitocin) given IV after delivery to help the uterus to contract.
Ethical Consideration • Abuse of Human Growth Hormone in athletes to improve performance – older people in search of the “fountain of youth” • Ovary stimulating drugs use to produce numerous ovaries to be artificially inseminated and implanted – may lead to selective abortion of excess embryos after implantation
Corticosteroids Chapter 23
Corticosteroids • Controlled by the hypothalamus • Rate of secretion is kept within a very narrow range • “negative feedback mechanism” when too much is released the mechanism for release shuts down.
Nursing Alert Very important concept when we give steroid to a patient – the higher plasma levels effectively shuts down the bodies production of the drug naturally – this is a drug that cannot be abruptly stopped – needs to be tapered.
Corticosteroids • Produced by the adrenal cortex • Involved in stress response, immune response and regulation of inflammation, carbohydrate metabolism, protein catabolism, blood electrolyte levels and behavior.
Two Types • Glucocorticoids: anti-inflammatory • Mineralocorticoids: aldosterone – controls electrolyte and water levels
Uses of Corticosteroids • Use to treat a number of different disorders especially inflammatory or immunologic disorders • Arthritis • Dermatitis • Allergic reactions • Asthma • Hepatitis • Lupus erythematosus • Inflammatory bowel disease: ulcerative colitis and Crohn’s disease • Uveitis – inflammation of eye
Use in Orthopedics • Cortisone can be injected directly into a joint to reduce inflammation. • Medrol dose pack is often prescribed for chronic back pain.
When not to use Corticosteroids • Fungal infections • Clients who are high risk for infection • Diabetes • Peptic ulcer • Hypertension • CHF • Renal Failure
How Administered • Topical – skin rashes - hydrocortisone • Eye drops / ear drops: cortisone ear drops or ophthalmic suspension • Nasal – Nasonex • Tablet or liquid form – prednisone, Decadron • IV – methyl prednisone or Solu-medrol • Inhaled - asthmatic or COPD
Goals of Therapy • To reduce symptoms to a tolerable level • Total suppression of symptoms may require excessive dosages • Avoid serious side effects
Clinical Pearl • Whenever possible the physician / nurse practitioner will prescribe a topical, nasal spray, eye drops or inhaled dosage before going to an oral route or intravenous route. • Oral and intravenous routes are usually higher dosages and more likely to have side effects.
Effects on the Body • Carbohydrates – increased blood glucose levels • Protein – increase breakdown of protein • Increased in blood pressure • Decrease in natural cortisol production by the body • Decrease in bodies inflammatory response