CONCLUSIONS
Capture of acute myocardial infarctions occurring at non-VA hospitals by outpatient, VA Healthcare System ICD-9 codes .


CONCLUSIONS
E N D
Presentation Transcript
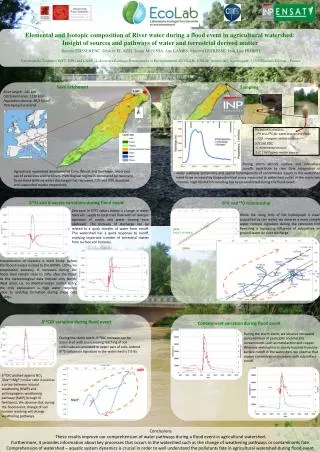
Capture of acute myocardial infarctions occurring at non-VA hospitals by outpatient, VA Healthcare System ICD-9 codes Authors: Travis A Rabbit1,2,3; Amy Justice4; Alberta Warner5; Adeel A Butt1,3; David Rimland6; Sheldon Brown7; Matthew Goetz5; Cynthia Gibert8; Maria Rodriquez-Barradas9; Kathleen McGinnis4; Stephen Gottlieb10; Jason Sico4; Hilary A Tindle1; Heidi Crane11; Matthew S Freiberg1,2,3 1University of Pittsburgh School of Medicine, Pittsburgh, PA; 2University of Pittsburgh Graduate School of Public Health, Pittsburgh, PA; 3VA Pittsburgh Healthcare System, Pittsburgh, PA; 4VA Connecticut Health Care System, West Haven Veterans Administration Medical Center (VAMC), West Haven, CT and the Yale University School of Medicine, New Haven, CT; 5David Geffen School of Medicine, UCLA and the VA Greater Los Angeles Health Care System, Los Angeles, CA; 6Emory University School of Medicine and Atlanta VAMC, Atlanta, Georgia; 7James J. Peters VA Bronx, New York, Mount Sinai School of Medicine, New York , NY; 8George Washington University School of Medicine and the Washington DC VAMC, Washington, D.C.; 9Baylor College of Medicine and Michael E. DeBakey VAMC, Houston, TX; 10 University of Maryland School of Medicine, Baltimore, MD; 11University of Washington, Seattle, WA BACKGROUND The United States Veterans Administration Medical Care system (VA) has a large number of HIV infected and HIV uninfected patients at high risk for acute myocardial infarction (AMI). Whether AMI events occurring at non VAMC hospitals (NVH) in these groups are captured in subsequent outpatient visits within the VA is not clear. Our primary objectives were to: Asses the feasibility and quality of our event ascertainment and capture of non-VA cardiovascular disease (CVD) events. determine whether AMI events occurring at a NVH are captured by outpatient VA ICD-9 codes at post-MI follow-up VA outpatient clinic visits. Figure 1. AMI Event Ascertainment, Capture, Assembly and Adjudication Methods • METHODS • Cohort: The Veterans Aging Cohort Study (VACS) is a • prospective, longitudinal cohort of HIV infected and age, • gender, race/ethnicity, and clinical site matched HIV • uninfected Veterans. • Ascertainment and request of CVD Events: • 3150 Veterans surveyed on prior events including: RESULTS Continued Capture by Physician Notes: All 21 participants with adjudicated AMI NVH events had narrative notes available within the VA EMR. • Veteran self-reported NVH records are requested by coordinators • at all 8 VACS VAMC sites around the U.S.A. • NVH CVD events, all records requested up to 3 times until: • either achieving capture of the outside event, or • receiving notice of no available records. • Coordinators and participants re-contacted when a • NVH had no record of the event or participant. • Obtained records assembled into event packets and de-identified • Triaged NVH possible MIevents by AMI trigger criteria (Figure 1) • VA events accessed through the electronic medical record (EMR) • query- based computer program • assembled based on MI trigger criteria algorithm • NVH events listed as past medical history in the VA EMR persued by site coordinators to gain consent for request. • CONCLUSIONS • NVH records can be successfully captured by thorough investigation, quality event information, and request follow-up. • Ascertaining NVH event occurrence through the EMR, we can assist participant recall, addressing issues with self report. • The VA EMR achieves a high capture of actual NVH AMI events. • 90% by administrative or physician documentation • 80% in entirety and completeness equal to that of the original NVH record, for the purpose of adjudication. • 3. Outpatient VA administrative data reflect events occurring outside the VA, based on preliminary data and a small number of events • Preliminary analysis suggests outpatient VA ICD-9 codes may be an acceptable measure for accounting for NVH AMI events • Future work will focus on sensitivity, specificity, positive and negative predictive values of ICD-9 codes for AMI and other CVD events, once all events have been adjudicated\ • We will also continue to review the VA clinical notes to better understand why physicians used a particular outpatient ICD-9 code (i.e., 410 vs. 414) to document a NVH AMI event. • IMPLICATIONS • Adjudication: • All CVD events meeting MI trigger criteria are adjudicated by 2 members of VACS Central Adjudication Committee • Composed of physicians with expertise in CVD and HIV. • 3rd adjudicator serves as a tie-breaker, if disagreement. • Standardized adjudication protocol criteria adapted from established CHD cohorts, to include: • anginal symptoms, cardiac enzymes, and EKG abnormalities • Assessment of the Adjudicated NVH AMI Event Capture: • Narrative notes and ICD-9 codes reviewed for capture by physician interpretations or of scanned original of NVH records . RESULTS • These preliminary results suggest that cohorts with access to an • electronic medical records system may be able to use similar • methods to ascertain CVD event records from hospitals outside of • their system. • LIMITATIONS • Although promising, the outpatient ICD-9 code data for assessing • NVH AMI events is still very preliminary. Completing the adjudication • process in the VACS cohort will provide a more definitive answer to • this important question. • Within the VA, events occurring prior to the adoption of the EMR may • have no records archived and available. • ICD-9 Code Capture: • Of 21 adjudicated MI events,13 occurred between 1997-2008.* • After reviewing post-AMI VA outpatient EMR ICD-9 codes, 12 of 13 (92%) had outpatient codes consistent with CHD: • * Cleaned data for ICD-9 codes were only available 1997-2008. Data from 2008-present will be available this year. ACKNOWLEDGEMENTS This work was supported by the Department of Veterans Affairs, the National Institute on Alcohol Abuse and Alcoholism (2U10AA13566), and by the National Heart, Lung and Blood Institute (3R01HL095136-03) The University of Pittsburgh School of Medicine and The Center for Research on Health Care