Upper and lower limb prosthesis
Upper and lower limb prosthesis. Dr. Hassan El Sharkawy. Definition. Amputation: the surgical removal of a part of the body, a limb or part of a limb. Amputation: Etiology. Trauma Burns Peripheral Vascular Disease Malignant Tumors Neurologic Conditions Infections Congenital Deformities.

Upper and lower limb prosthesis
E N D
Presentation Transcript
Upper and lower limb prosthesis Dr. Hassan El Sharkawy
Definition Amputation: the surgical removal of a part of the body, a limb or part of a limb
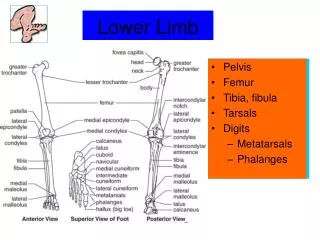
Amputation: Etiology • Trauma • Burns • Peripheral Vascular Disease • Malignant Tumors • Neurologic Conditions • Infections • Congenital Deformities
What is prosthesis? • A device used to replace an absent body part whether due to trauma, disease or congenitally absent ones Types of Upper Limb Prosthesis? • Prosthesis of the upper limb may be cosmetic, functional or combination of both.
WHAT IS THE FUNCTIONS OF THE UPPER LIMBS? • The whole upper limbs function to place hand in adequate position to fulfill a particular task. • Hand tasks: 1- Manipulative tasks. 2- express feeling. 3- Explore environment. • No prosthesis can replace all functionsatisfactory. Selection is based in specific requirement of the amputee.
Cosmetic Upper Limb Prosthesis • This is the simplest and lightest type available. • For transradial (forearm = below elbow) it consists of: 1- Foam filled glove with 2- Wired fingers 3- Fitted to a self suspending socket.
Advantage of this prosthesis • It provides best cosmetic replacement but with minimal functional benefit e.g.: Holding objects steady or carrying things over forearm. • N.B: Individually sculpted silicon hands are available which are excellent cosmetically but expensive and not strong enough for any practical daily tasks.
Functional U.L. Prostheses • These are upper limb prostheses that includes a control mechanism of the hand component (terminal device), and different joint replacement units (either for wrist or elbow joints). • There are two types of control systems namely: • Body- powered control system • Electric control system
A) Body powered: • This prosthesis is the simplest functional prostheses. • Body movement is harnessed to control the terminal device (and elbow). A set of appendages harness the body movement.
Examples • (1) biscapular protraction, (2) shoulder flexion (and elbow extension = in cases of transradial amputation) are used to control terminal device. • Shoulder depression, extension, internal rotation, & abduction operate the elbow lock in trans humeral amputation. • This type of prosthesis is a working tool & it is functional rather than attempting to be cosmetic
Body Powered functional U.L. Prosthesis: Terminal device, Wrist unit, operating cord, suspension loop
Electric control systems: A battery – operated motor moves the hand and/or gripper, wrist or elbow by either: • Myo-electric control. • Servo control. • Switch control. Rechargeable.
1- Myo-electric control • Electrodes pick up microvolts of electricity produced by contractions in the muscles of the residual limb. • Signals are amplified and thereafter they activate the motor. • In operating hand there may be 2 electrodes; one on extensor muscles and one of flexor muscles groups for opening & closing the hand respectively.
Alternatively a single site placement for voluntary opening & automatic closing can be used. • Wrist movement can be controlled myo-electrically using 2 site system. • An electric elbow lock can be activated be a single site placement
2) Servo Mechanisms • The same movements used to control body powered prosthesis, can operate an electric hand but with less shoulder girdle movement. Where mechanical energy is transmitted into electric energy to operate the device motor (s). 3) Switch control • Using harness or touch pads to control electric devices in different ways.
Terminal devices • Used to replace the task of the hand, • It may be cosmetic or functional / passive or active. *** The most commonly used active functional device is the split hook. • It consists of once static – one movable new. • Grip is achieved by elasticated bands holding the two jaws together, and can be increased by increasing number of bands. • The device is activated by harness attached to the lever of the moving jaw as residual limb moves, harness pulls the jaw open, providing good proprioceptive feed back.
If cosmoses are important, a cosmetic hand can be provided. • If patient seeks combination between cosmoses and function, same device as above is used but with mechanical hand same shape as the human hand and body power pulling the thumb and fingers apart.
Mechanical hands have some disadvantages that include: 1- It is harder to operate than the split hook. 2- It has a poorer grip. 3- Bulky & making precision difficult. Despite this it is helpful if an amputee not demands high level of manipulative skill from the prosthesis.
Terminal devices with special tasks: Active: pliers – tweezers- Pen holders (using operating cord). Passive: hammer, fishing red holder tool holder.
Prosthetic Joints • Wrist unit: A cylindrical wrist unit either hand or electrically operated to provide 360° rotation, allow positioning of the terminal device in adequate supination/ pronation range for the required task. Usually wrist units have a disconnect facility allow change of terminal device.
Elbow joint: Several forms of prosthetic elbow joints are in use. Hand operated joints are commonly used with cosmetic prosthesis. In addition, body powered elbow joints, used with body powered prostheses, are utilized. They are operated using operating and elbow lock cords. Operating cord operates the terminal device when the elbow is locked, while with elbow unlocked it operates the elbow joint.
Suspension • For hand amputation and wrist disarticulation self suspension is used that depends on hanging the socket to bony prominences, namely radial and ulnarstyloid processes. • For transradial amputation when using a supra condylar socket, self suspension is applied using medial and lateral humeral epicondyles for hanging the prosthesis.
N.B.: • In case of transradial amputation cup socket is used when amputee need carry heavy objects, with very short residual limb, or bilateral amputation. Supracondylar socket is used with cosmetic and passive terminal devices. • In wrist disarticulation supination /pronation is controlled by wrist unit or by split socket with one section at the wrist and the other at the distal part of the arm, sparing the forearm to perform movement.
Lower Limb Prosthesis Types of lower limbs prostheses : • Types of L.L. prostheses depend on different stages after amputation. There are three types: - Immediate post- operative prosthesis. - Temporary prosthesis - Definitive prosthesis.
The basic components of a lower extremity prosthesis include: the socket, a sock or gel liner, a suspension system, a knee joint (articulating joint), the shank (a pylon), and a foot (terminal device) .
I- Immediate post- operative prosthesis • Used for young patients, usually after a traumatic injury. - Consists of rigid dressing pylon, and foot. - Pylon is usually made of aluminum, steel or plastic. - It helps patient to gain psychological support, early walking (with assistive device 5-12 days post operative) leads to less hospital stay, and reduce phantom pain.
Disadvantages are the possibility of impaired healing & falls due to early ambulation. • Contraindication: • History of slow wounds healing. • Extreme obesity. • Excessive preoperative edema. • Lack of 45 days preoperative ambulation.
II – Temporary prostheses • It is usually used for 3 to 6 month after amputation. • It helps early weight bearing, and reduces edema in the residual limb stamp. • The most common type of temporary prosthesis is adjustable prosthesis. It consists of a socket, pylon, foot. It can be modified so that the foot in moved in medial, lateral, anterior, posterior inversion, eversion direction. These adjustments help to correct gait deviations, increase energy efficiency, and make walking more efficient and cosmetic. Therefore it is used in early stages of gait training. • Temporary prosthesis can be converted to definitive or final prosthesis with cosmetic modifications.
III- Definitive prosthesis • It is used when limb volume becomes stable. • It can be applied 3-9 months postoperative. • Life span 3-5 years. • Changes are needed when there is residual limb atrophy, weight gain or loss., and excessive wear after prosthesis.
Prosthetic foot It should be: 1- Providing stable base of support. 2- Shock absorption. 3- Joint & muscles stimulation. 4- Cosmetic appearance.
I) Conventional a) Articulated Single axis: Have a single Metal axis that allows plantar (15 degree) and dorsiflexion ( 5-7 degree). Internal keel surrounded by foam-rubber outer lining. Loaded with dorsiflexion bumper that replaces eccentric contraction of plantar flexors, and plantarflexion bumper that replaces eccentric contraction of dorsiflexion. It allows level- floor ambulation but does not allow for walking on a steep incline.
Multiple- axis foot • The multiple axis foot has two joints, a rubber rocker block that allows dorsiflexion and plantarflexion and a transverse ankle joint that allows rotation, eversion and inversion. It contains a wood keel and outer cover of foam rubber. It allows walking on level ground and inclines
b) Non articulated 1-Solid Ankle Cashion Heel (SACH) Consists of wood keel that extends forwards to the toe break and is surrounded by molded foam. The SACH Compressible rubber heel simulates plantar flexion. At loading response the heel wedge comprises to simulate plantar flexion.
2- Stationary Attachment Flexible Endoskeletal foot (SAFE) The SAFE foot keel, is composed of rigid polyurethane plate at an angle 45 in the sagittal plane to provide eversion and inversion. To elastic bands extend on the plantar surface that courses the keel to dorsiflex from mid- to terminal stance. At pre swing the keel releases.
II) Dynamic Response 1- Articulated College Park True Step • It has three axes one vertical and two transverse axes. These axes allow mobility in the three planes of motion. Two bumpers, dorsi- and plantar flexion bumpers are included. In front there are two split toes of carbon fibers. • College Park designs, manufactures high quality prosthetic feet and components.
2- Non- Articulated A) SHORT KEEL 1- Stored Energy foot (STEN) The keel is subdivided into compressible and non compressible segments, a structure that allows energy storage from loading response to mid swing and release it at push off.
2- Carbon Copy II Consists of two carbon fiber deflection plates that return energy during walking and running. It has a strong keel covered by polyurethanefoam.
B- LONG KEEL 1- Flex foot: Two elastic carbon fibers attached to a horizontal carbon foot plate. Carbon fibers extend to include the pylon. 2-Springlite foot: Similar to flex foot, but consists of one elastic carbon fibers and one fiber glass filaments surrounded by a soft cover. It is 30% less expensive than flex foot.
Sockets Sockets for below knee amputation is either Patellar tendon bearing or total surface Bearing sockets. • Total surface bearing Complete weight bearing evenly distributing pressure on the contact surface
Suspension Types 1- Supra condylar (medial wedge). 2- Supra condylar- supra patellar system. 3- Supra condylar cuff. 4- Thigh corset. 5- Waist belt.