Cornwall’s Joint Commissioning Strategy
290 likes | 509 Vues
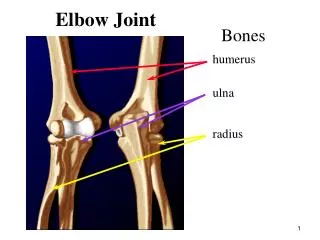
Cornwall’s Joint Commissioning Strategy. Presented by: Carol Williams, Director of Service Improvement Bev Chapman, Clinical Lead & Specialist Dementia Nurse. October 6 2009. Commissioning for Dementia: The last 12 months. 07/08. Joint Strategic Needs Analysis.

Cornwall’s Joint Commissioning Strategy
E N D
Presentation Transcript
Cornwall’s Joint Commissioning Strategy Presented by: Carol Williams, Director of Service Improvement Bev Chapman, Clinical Lead & Specialist Dementia Nurse October 6 2009
Commissioning for Dementia: The last 12 months 07/08 Joint Strategic Needs Analysis Dementia is a shared Council/PCT strategic priority May 08 ClinicalDementiaLead appointed Time Jul 08 Joint Commissioning Plan Aug 08 Service ImprovementProgramme World Class Commissioning Outcome Oct 08 National Dementia Strategy Feb 09
Quantifying Needs • 8,213 people living with dementia in Cornwall and the Isles of Scilly • 2,645 people on GPs dementia registers in August 08 • World Class Commissioning ambition to increase number of people on registers to: • Aug 09 – 3,352 • Aug 10 – 3,724 • Aug 11 – 4,096 • What about carers? Perhaps 4,100 living in Cornwall or 1,500 requiring help by Aug 09? • We need to commission sufficient services for at least the number of people on dementia registers
High Complexity Case Management Medium Complexity Disease / Case Management Low Self Care support / Management Dementia Care Advisors? Care Pathway Segmentation Prevention Awareness Recognition Assessment Opportunities for providers exist all along the pathway Diagnosis Case Mgmt & Treatments Crisis End of Life
Principles of commissioning ‘PEOPLEwith dementia’ • Dementia a long term condition: chronic and progressive • Overlapping physical, mental, health and social needs • Early diagnosis, continuity of care and more choice • Younger people with dementia • People with learning disabilities
Principles of Commissioning (cont) • More community based services promoting independence, delaying or preventing admission to care home/hospital • Integration / joining it up is the only way we can make the best of what we’ve got • Locality commissioning • Low intensity can mean high impact – eg Assistive Technology • Thinking smarter about the connections between different providers – e.g. the relationships between GP practices, a dementia nurse, a social worker and a care home. • Care Homes are people’s homes too.
Long Term Conditions • Understand our population • Early identification of need • Promote self management, • Optimise quality of life and self esteem • More prevention, less crisis management • More responsive • community health and social care
Sacred Cow Philosophy People with dementia have needs that can be labelled: ‘health’,‘social’ ‘primary’ ‘secondary’ Dementia is ‘Older People’s Mental Health’ Older People’s Mental Health are ‘secondary’ care services
Cow slaying logic (1) • Dementia a long term condition: chronic and • progressive • So: overlapping physical, mental, health and social needs • What about younger people with dementia? • What about people with learning disabilities? • Why ‘mental health’?
Primary Care Non- Community Services (People can’t stay In own home) Social Care Health Care Secondary Care Divided by a common language Community Services (People in own home) GPs Locality – eg Newquay
More Bad Language People with dementia are ‘Demented’ ‘Dementing’ ‘Victims’ ‘Sufferers’ ‘Wanderers (without purpose)’
Value the PERSON with dementia “Please don’t call us ‘dementing’ – we are still people separate from our disease, we just have a disease of the brain”. If I had cancer, you would not refer to me as ‘cancerous’ would you? Our labels seem to mean so much – am I Alzheimer’s Disease or fronto-temporal dementia, or simply someone with a ‘dementing illness’. All these terms labels us as someone without capacity, without credibility as a member of the community. How about separating us from the illness in some way? How about remembering we are a person with progressive brain damage” Christine Bryden, “Dancing with Dementia”, 2005
Curing Sacred Cow Disease • Make dementia ‘everybody’s business’ rather than “somebody else’s business” • Focus on prevention – physical health check – vascular checks to prevent vascular events • Improve awareness and recognition of dementia amongst GPs, health and social care professionals, including care homes • Increase the number of people receiving an early diagnosis and an annual health check.
Prevention Awareness Commissioning integrated pathways rather than organisations • The Menu • Information • Books on Prescription • Cognitive Stimulation Therapy • Creative therapies • Peer-Support • Memory Cafes • Assistive Technology • Sensory Therapies • Reminiscence Work • Carer Education • Domiciliary care • Respite Care • Advocacy • Care Home/Hospital Recognition Assessment Diagnosis Case Mgmt Tiered Menu of Interventions Unscheduled Tiered Menu of Interventions End of Life Simple pathways and overlapping services
Work so far • Memory Cafes flourishing • Awareness raising campaign • Education and training • Making it easier to get a diagnosis – 19 Memory Clinics across the county • Newquay Integrated Care Pilot • Dementia Liaison in Care Homes • Carer Education Programme • Advocacy • Arts for Health • Adult Placement for people with dementia Swaps
What does this mean for providers? • Dementia care is a ‘growth market’, but not for more of the same - greater emphasis on early intervention, high volume, low-cost interventions. • Fundamental change essential. Opportunity for existing providers to rethink corporate identities, business models and their role in delivery. • Expect new providers with new types of expertise to enter the market in response to new demands (e.g. Extra Care Housing and GPs) • Competition for business increasing. But, so are opportunities for greater co-operation, collaboration and sharing of resources (knowledge, staff, technology, buildings).
What does this mean for providers? • More emphasis on defining and rewarding quality. • Currency ‘person-centred care’ not ‘units of care’. • New income opportunities for the best providers. • Providers, who can evolve quickly into a new breed of ‘Dementia Specialists’ and who can deliver whole-life, person-centred dementia care in a range of settings will prosper • There has never been a more exciting time to be a dementia care provider in Cornwall
Good opportunity for: • Commissioners informing • Plans • Progress • Business Opportunities • Commissioners LISTENING! • Bringing the experts together: collaboration and best practice sharing • Arts for Health • Assistive Technology
The Newquay Integrated Care Pilot What we did and early learningRegistered Pop 23,000Anticipated Dementia: 361
Dementia Liaison Pilot • Trial the Hospital Liaison model in the community (Care Homes, Community Hospital and GPs) • QOF Health-checks (Community & Care Homes) • 3 month pilot in 12 care homes – led to commissioning of dementia liaison service. Finding the undiagnosed. • Partnership with pharmacists – medication reviews
GP Led Memory Clinic • Education – anticipation of successful Dementia Academy 27th March • Opportunistic screening with flu jab • Recognition, assessment, diagnosing and prescribing cognitive enhancers • Complementary and in addition to existing assessment, diagnosis service, which still provides ‘back-up’ and is partly moving to a Memory Clinic model. • Case management
What did Newquay tell us? • Over 50 patients with undiagnosed dementia identified and registered on QOF registers • 104 QOF Health Checks completed • 27 Psychiatric Medications discontinued (anti-psychotics, night sedation, benzos and depots). • 15 changes to physical medications • 8 Blood Tests • 5 regular blood pressure reviews • 19 pain assessments and treatment • 10 Dietary supplements and weight monitoring • 6 End of Life Care Plans (preventing admission to acute hospital
Dementia Liaison Practitioners’s in Care Homes • Fortnightly review of all care home residents • Providing evidence based education and training • Close working relationship with G.P as decision maker • Annual QOF health check • Crisis prevention • Easily accessible • Acute Hospital admission avoidance • Stabilising needs to avoid distressing move to other care facility • Family support • End of Life care in line with Gold Standard Framework • Reduction of anti-psychotic medication • Risk assessment
Annual QOF Health Check • Blood Pressure • Cognitive Assessment • Medication • Nutrition • Weight • Continence • Activities of daily living • Mobility • Falls • Mood • Pain • End of Life • Difficult to manage behaviours • Plan
IMPROVED HEALTH OUTCOMES Case Study – Mr G End of Life Pathway
Newquay Case Management Outcomes • QOF registers • Prevalence 361 • Sept 08 136 • April 09 207 • Sept 09 244 • 67% of expected prevalence against 37% county wide • Case management 131 with care plan in community • 113 with care plan in care home
2010.... Tele helpline Memory manual Community liaison expansion Case management rollout Increase QoF registration Health checks for all/ health promotion Reduce hospital admissions/crisis Gold standard palliative care. Partnership working social/care all sectors.