Shock
Shock. Introduction. Definition of Shock Types and Etiology of Shock Signs and Symptoms of Shock Case Study Body’s Response to Shock Treatment of Shock Prevention How to treat someone in anaphylactic shock Management of anaphylaxis in a hospital setting. Shock, what is it?.


Shock
E N D
Presentation Transcript
Introduction • Definition of Shock • Types and Etiology of Shock • Signs and Symptoms of Shock • Case Study • Body’s Response to Shock • Treatment of Shock • Prevention • How to treat someone in anaphylactic shock • Management of anaphylaxis in a hospital setting.
Shock, what is it? • Shock is a critical condition caused by a sudden drop in blood flowing through the body secondary to circulatory system failure (an inadequate blood flow causing insufficient delivery of oxygen & nutrients to meet the metabolic needs of tissue). • This can damage multiple organs
Types of Shock: • Cardiogenic Shock • Hypovolemic Shock • Vascular/Distributive Shock • Septic Shock • Neurogenic - caused by damage to the nervous system • Anaphylactic - caused by allergic reactions
Cardiogenic Shock • This type of shock is associated with heart problems. It is due to a reduction in cardiac output caused by a primary cardiac disorder. • Example: severe myocardial infarction/ Cardiac failure!
HypovolemicShock • This type of shock is caused by deficiency of intravascular blood volume and the inability to meet the metabolic needs of tissues. • Example: Hemorrhage and dehydration
Vascular/Distributive Shock • This type of shock is characterized by the loss of blood vessel tone, enlargement of the vascular compartment, and displacement of the vascular volume from the systemic circulation. • Venous return is decreased in distributive shock, which leads to a diminished cardiac output but not a decrease in total volume; this type of shock is also referred to normovolemic shock.
Septic Shock • This type of shock is a systemic response to a severe infection.
Neurogenic Shock • This type of shock is caused by decreased sympathetic control of blood vessel tone. This is due to a defect in the vasomotor center located in the brain stem. • Example: Output from the vasomotor center can be interrupted by brain injury, the depressant actions of drugs, general anesthesia, hypoxia, or lack of glucose.
Anaphylactic Shock • This type of shock is considered the most severe systemic allergic reaction. It results from an immunologically mediated reaction in which vasodilator substances such as histamine are released into the blood. • This causes vasodilation or arterioles and venules along with a marked increase in capillary permeability.
Causes of anaphylaxis • Drugs • Penicillin • Foods • Nuts • Shellfish • Environmental • Insect venoms • Latex
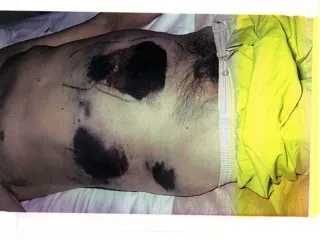
Early signs/symptoms of Anaphylatic shock: • Hypotension • High pulse rate: weak and rapid • Dyspnea, coughing, choking, wheezing, and chest tightness • Tachypnea/ hyperventilation • Dry mucous membranes • Burning & warming sensation of the skin, itching, and urticaria (hives) • Restlessness • Anxiety or agitation • Nausea, abdominal cramps • Thirst • Weakness • WBC - elevated eosinophil count due to allergic reaction
Late symptoms of Anaphylactic shock: • Decreased urinary output • Severe fluid and electrolyte imbalance • Confusion • Hypothermia • Drowsiness • Diaphoresis, moist skin • Lethargy, that can lead to coma
Case Study C.L. is a 35‑year‑old male who is admitted to your floor with a c/c of right flank pain.
9:00 am The M.D. leaves the following orders: R/O right renal calculi V/S q 4 h BR with BRP Strain all urine Strict I & O CBC, SMAC 20, Chest x‑ray, EKG Intravenous Pylogram (I.V.P.) this AM D5 2 N/S 300 cc/hr. Demerol 100 mg IM q 4 h prn for pain
At 9:05 am the nurse clarifies the M.D. orders: R/O right renal calculi V/S q 4 h BR with BRP Strain all urine Strict I & O CBC, SMAC 20, Chest x‑ray, EKG Intravenous Pylogram (I.V.P.) this AM D5 2 N/S 300 cc/hr. Demerol 100 mg IM q 4 h prn for pain
10:00 a.m • You accompany C.L. for his I.V.P. • The tech administers the contrast medium I.V.
10:05 a.m. Within minutes C.L. c/o his lips feeling tingly, his tongue swollen and that he has difficulty swallowing and breathing. He states, "I feel like I'm dying." You place him in semi‑fowlers and take his v/s. R 30 with progressive difficulty and stridor Wheezes heard on auscultation. B/P 80/60 P 120 thready Skin flushed, dry
10:10 a.m. Epinephrine (1:1000) 1.0 ml S/C is given STAT ‑ IV #1 is changed to 0.9% N/S 1000 cc ‑ A second I.V. is initiated with 0.9% N.S. Both IV's are rapidly infusing. ‑ Arterial Blood Gases (ABGs) are drawn and sent stat. ‑ Oxygen at 100% via mask is applied.
10:20 a.m. Vital Signs: B/P: 84/68 PR: 124 bounding RR: 26 S.O.B. noted; decreased stridor, decreased wheezes noted. Dopamine gtt. is hung ‑ to be titrated to maintain systolic > 80 to 110 mmHg.
10:30 a.m. • Vital Signs: • BP:92/68 • HR:120 Reg. • RR:24 • lungs clear throughout • without wheezing or stridor. • Patient c/o that he "feels itchy all over.“ You note urticaria diffusely over his body. • Benadryl 75 mg IM is given STAT with some relief.
10:45 a.m. Vital Signs • BP: 108/170 • PR: 100 Reg • RR: 22 • Patient A & 0 x3. Skin cool, flushed and dry. • Minimal S.O.B. noted without diaphoresis, wheezes or stridor. • Patient states that he is breathing easier and has decreased itching. • Cardiac monitor ‑‑‑> Normal Sinus Rhythm (NSR).
IV #1 0.9% N/S rapidly infusing in the right antecubital space. • I.V.#2 0.9% N/S rapidly infusing in the left antecubital space. • Dopamine gtt @ 4 mcq/kg/min infusing. • ABG results: pH 7.31 PO2 95 CO2 35 HCO2 19 O2Sat 99
Transferred to M.I.C.U. Dr. Jones in attendance. M.Smith, R.N.
Question 1: As the primary nurse in charge of C.L’s care, you check his chart for allergies. You note that he is only allergic to “shellfish”. What, if any, is the connection between an allergy to shellfish and contrast medium?
Differences between a CM allergy and a Shellfish allergy Contrast Medium (CM) Allergy CM is an iodine based substance used in radiology. CM can cause allergic reaction r/t to either Iodine itself or the dye component of CM. Allergy to the IV dye is not a true allergy • The dye causes the direct release of histamine and other chemicals from mast cells without the help of allergic antibodies Shellfish Allergy Shellfish contains iodine, but allergy to shellfish is caused by the protein tropomyosin and NOT the iodine component.
Relation between a Contrast Medium and Shellfish Allergy No Correlation btw Allergy to shellfish and CM ! Allergy to Iodine should be tested independently whether allergy to fish is present or not.
Contrast Medium It is generally used to improve the visibility of internal bodily structures in an x-ray image.
What is the pathophysiology behind Anaphylactic Shock?What chemical mediators are responsible for vasodilation and increased capillary permeability? Question 2 & 3:
Immunologic Disorders • There are three levels of immunologic disorders: • Hypersensitivity – allergy response • Autoimmune Disease – body’s response against self-antigens • Immunodeficiency – the immune response is below normal
Hypersensitivity Hypersensitivity is an immune response that is beyond normal and is damaging rather than beneficial
Hypersensitivity • There are 4 classes of hypersensitivity: • Type I (anaphylactic) reaction • Type II (cytotoxic) reaction • Type III (immune complex) reaction • Type IV (delayed cell-mediated) reaction
Hypersensitivity – Type I (anaphylactic) reaction • Type I (anaphylactic) reaction can be: • Localized • Systemic
Hypersensitivity – Type I (anaphylactic) reaction • Localized anaphylactic reaction: • Usually ingested or inhaled allergens • Symptoms include: • Hives • Asthma • Hay fever
Hypersensitivity – Type I (anaphylactic) reaction • Systemic anaphylactic reaction • Usually injected allergens, but can be ingested • Very quick response • Symptoms include: • coughing • edema • drop in blood pressure • possibly death
Hypersensitivity • Upon the first exposure to an allergen a person will not necessarily develop a response. • Antibodies (Immunoglobins (Ig) will be formed after the first exposure to fight off the same allergen upon a second exposure.
Mechanism of Type I (anaphylactic) Hypersensitivity • Specifically Immunoglobin E (IgE) is found floating around the cell and also bound to basophils and mast cells • When an allergen enters the body the allergen will bind with IgE on the basophils and mast cells
Mechanism of Type I (anaphylactic) Hypersensitivity • A signal transduction pathway will tell the cell to degranulate and release chemical mediators such as histamines, leukotrines, and prostaglandins
Mechanism of Type I (anaphylactic) Hypersensitivity • Chemical mediators cause dilation and leakage of plasma from capillaries, airway constriction, and increased mucus production • This, in turn, can cause itching, swelling, and pain
Mediator Chemical Characteristics Histamine Simple Amine Prostaglandin Simple Amine Platelet-activating factor (PAF) Phospholipid Leukotrienes Acid lipid Neutral Proteases Small protein enzymes Acid Hydrolases Fairly large proteins Heparin Peptide chain bearing long-chain sulfated amino sugars Superoxide dismutase Enzymatic protein Chemical Mediators • Many chemical mediators of inflammation are released by Human Mast Cells and Basophils including:
The three most responsible for vasodilation and increased capillary permeability are: • 1) Histamine • 2) Prostaglandin • 3) Leukotrienes
Histamine • These effects, in turn, help the body rid itself of foreign invaders • Dilation of blood vessels increases circulation to the injured area, washing away harmful bacteria • Proteins also attract other immune cells to the area, such as macrophages. • Once histamines are released into the tissues, they exert a variety of effects: • Contracts visceral smooth muscle • Causes inflammation • Increases permeability of capillaries • Increases respiratory mucous gland activity • Produces sensation of itching • Dilate Blood Vessels • Stimulate gland secretion • Prompt the release of proteins from cells
Leukotrienes • Leukotrienes are inflammatory mediators that cause vasodilation and mucosal swelling, which results in inflammation and congestion. • Leukotrienes are also responsible for: • Prolonged visceral smooth muscle spasm • Increased permeability of venules
Prostalglandin • Prostalglandins are mediators that have strong physiological effects: • Vasodilation • Bronchodilation • GI tract smooth muscle contraction • stimulates constriction and clotting of platelets • Increases mediator release by basophils
Inflammation • Caused by the release of histamine from basophil or mast cells • Directly effects epithelial cells of vessel wall • Pulls the epithelial cells apart from each other • Installs cell adhesion molecules (CAM) on the surface of the vessel wall • Causes leukocytes to stick to the CAM on the sides of the vessel wall • Leukocytes then squeeze through the gaps created by the epithelial cells
Inflammation • When leukocytes reach their target, they secrete more cytokines, which recruit more neutrophils and macrophages • Leukocytes secrete colony stimulating factor, which causes the bone marrow to create more leukocytes