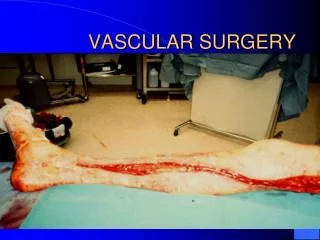
Vascular Surgery Back to Basics
Vascular Surgery Back to Basics. Andrew B Hill MD FACS FRCS Vascular and Endovascular Surgery The Ottawa Hospital. OUTLINE. Acute limb ischemia Claudication Critical limb ischemia Aortic Aneurysm Aortic dissection Varicose veins Chronic venous insuffciency Superficial thrombophlebitis.

Vascular Surgery Back to Basics
E N D
Presentation Transcript
Vascular SurgeryBack to Basics Andrew B Hill MD FACS FRCS Vascular and Endovascular Surgery The Ottawa Hospital
OUTLINE • Acute limb ischemia • Claudication • Critical limb ischemia • Aortic Aneurysm • Aortic dissection • Varicose veins • Chronic venous insuffciency • Superficial thrombophlebitis Acute Limb Ischemia
Mrs. Whitelegg • ID: • 75 yo lady • Active - walks her dog ~2 kms daily • has not needed to see a doctor in the last 10 years. Acute Limb Ischemia
Mrs. Whitelegg PMHx/PMSx: remote TAH-BSO social smoker quit in the 1960’s No: DM HTN hyperlipidemia Acute Limb Ischemia
Mrs. Whitelegg • HPI: • watching TV • sudden onset of numbness in her right leg - “like it went dead” • Unable to walk • constant, severe pain eventually involving the entire right leg. • Called amblance Acute Limb Ischemia
Mrs. Whitelegg What is the diagnosis? Acute Limb Ischemia
Mrs. Whitelegg • Acute limb Ischemia: • abrupt cessation of arterial blood flow • hypoperfusion of tissue • threatened limb viability Acute Limb Ischemia
Mrs. Whitelegg Vital Signs BP:140/90 mmHg HR: 150 bpm irregularly irregular Afebrile Acute Limb Ischemia
Mrs. Whitelegg • Exam Normal heart sounds Chest clear IPPA No pulsatile masses in her abdomen No carotid, abdominal or femoral bruits Acute Limb Ischemia
Mrs. Whitelegg Exam Pulses: Left: + femoral, + politeal, + DP, + PT Right: - femoral, - popliteal, - DP, - PT Acute Limb Ischemia
Mrs. Whitelegg Exam Normal heart sounds good a/e bilat No pulsatile masses in her abdomen No carotid, abdominal or femoral bruits Pulses: L: + femoral, + politeal, + DP, + PT R: - femoral, - popliteal, - DP, - PT R foot is colder and paler than L Decreased sensation in R foot Able to move toes but difficulty with plantar and dorsi flexion Absence of trophic changes in her lower extremities (no hair loss, thickened nails, or thin, flaky or shiny skin) Acute Limb Ischemia
Mrs. Whitelegg Exam R foot is colder and paler than L Decreased sensation in R foot Able to move toes but difficulty with plantar and dorsi flexion Absence of trophic changes in her lower extremities (no hair loss, thickened nails, or thin, flaky or shiny skin) Acute Limb Ischemia
Mrs. Whitelegg • What are the 6 P’s of Acute Limb Ischemia Acute Limb Ischemia
Mrs. Whitelegg 6 P’s of Acute Limb Ischemia Pain Palor Polar/poikilothermia Paraesthesia Paralysis Pulselessness Acute Limb Ischemia
Mrs. Whitelegg • Classify Acute Limb Ischemia. In which category is Mrs. Witelegg? Acute Limb Ischemia
Mrs. Whitelegg • Your working diagnosis is acute limb ischemia. • You order CBC, electrolytes, BUN, Cr, PTT/INR (all of which comes back normal), type and cross-match blood, and a saline infusion is started. • CXR is unremarkable • ECG is as follows: Acute Limb Ischemia
Mrs. Whitelegg • What is the most likely etiology of ALI in Mrs. Whitelegg? • Cardiogenic embolism Acute Limb Ischemia
Mrs. Whitelegg What in her history and physical supports this diagnosis? lack of atherosclerotic risk factors no previous claudication (she walked her dog 2 km/day) atrial fibrillation normal left extremity pulses Acute Limb Ischemia
Mrs. Whitelegg Based on her physical examination, what is the highest point of obstruction of arterial flow? R ileo-femoral region Acute Limb Ischemia
Mrs. Whitelegg How long can a limb be without blood flow before irreversible tissue damage ensues? 4-6 hrs Acute Limb Ischemia
Mrs. Witelegg • What is the surgical management of this condition? • R femoral embolectomy • Can we proceed to the OR without any imaging studies? If not what studies can be perfomed? • Because of the classic history and physical findings, and because of the presence of class 2b ischemia, immediate surgery is indicated without delay for imaging. • Angiography can be performed in certain conditions of ALI • when the suspected etiology is arterial thrombosis (i.e. in preparation for bypass surgery) • when the patient has class 1 or 2a ischemia Acute Limb Ischemia
Mrs. Witelegg • What medical therpay is available for ALI and when is it indicated? • Lytic therapy (i.e. with t-PA) is used to dissolve the clot. It is a good option in the setting of acute arterial or graft thrombosis. It is not indicated in the setting of trauma or when the patient can not wait more than 24-48 hrs, as the therapy requires that period of time for clot dissolution. ( i.e. class 1 or early 2a ischemia) • IV Heparin will not dissolve the clot but will prevent further propagation, and is only indicated if there is a delay to surgery Acute Limb Ischemia
Mrs. Witelegg • The patient is booked for emergency embolectomy • Under local anaesthesia, a small incision is made over the R groin. The femoral artery is exposed and controlled with vessel loops. A small arteriotomy is made and the clot is removed proximally and distally using a fogarty balloon embolectomy catheter. • The arteriotomy is repaired and the foots “pinks up” after blood flow is returned. There is a palpable DP and PT pulse. • The patient is returned to the recovery room. Acute Limb Ischemia
Mrs. Witelegg • At 3 am you get paged by the recovery room nurse. Mrs. W is complaining of significant pain in her leg, it is more swollen and the DP and PT are no longer palpable. • In addition, her urine output has diminished and she is peeing out dark urine which tested positive for “blood” on the urine dipstick. Acute Limb Ischemia
Mrs. Witelegg • What is happening to Mrs. W? • Reperfusion syndrome: occurs as a result of blood flow going back into previously damaged tissue, causing rhabdomyolysis and compartment syndrome.. • Rhabdomyolysis: Liberated myoglobin from dead muscle cells enters the blood stream resulting in renal tubular obstruction and direct nephrotoxicity causing renal failure. Myoglobinuria is a false positive on the urine dipstick test for blood. • Compartment syndrome: Free oxygen radicals are created with reperfusion. These result in increased tissue edema, with in the limited facial compartments of the lower leg, this further decreases capillary blood flow and worsens the ischemia and tissue damage, causing further edema. Pain out of proportion, pain on passive stretch and high pressures in the compartments suggests compartment syndrome. Acute Limb Ischemia
Mrs. Witelegg • How should reperfusion syndrome be managed? • Compartment syndrome is a surgical emergency and is managed by 4-compartment fasciotomies. • Rhabdomyolysis should be managed with aggressive IV fluids, diuresis and alkalinization of urine. Acute Limb Ischemia
Definition • spontaneous tear in aortic intima allowing blood to be driven between the aortic intima and media • acute < 2 weeks • chronic > 2 weeks Aortic Dissection
Classification • DeBakey • Type I - involves ascending and descending aorta • Type II - ascending aorta only • Type IIIA - descending thoracic aorta • Type IIIB - Type IIIA plus abdominal aorta • Standford • Type A - ascending aorta and aortic arch; emergency • Type B - aorta distal to subclavian artery; emergency surgery if complications of dissection Aortic Dissection
Etiology • HYPERTENSION, usually uncontrolled • TRAUMA, usually deceleration injury (falls, MVAs) • other: cystic medial necrosis, atherosclerosis, connective tissue disease (Marfan’s syndrome, Ehlers-Danlos syndromes), congenital conditions (coarctation of aorta, bicuspid aortic valves, PDA), infection, arteritis (Takayasu’s) Aortic Dissection
Epidemiology • incidence 5.2 in 1,000,000 • male:female = 3:1 • small increased incidence in African-Canadians (related to higher incidence of hypertension) • lowest incidence in Asians Aortic Dissection
Clinical Features • SUDDEN ONSET SEVERE CHEST PAIN RADIATION TO THE BACK (INTERSCAPULAR) +/-.... • hypertension • asymmetric BP’s and pulses between arms • ischemic syndromes due to occlusion of aortic branches: coronary (MI), carotid (stroke, Horner’s syndrome), splanchnic (ischemic gut), renal (kidney failure) • “unseating” of aortic valve cusps (new diastolic murmur) • rupture into pleura (dyspnea, hemoptysis) or peritoneum (hypotension, shock) or pericardium (tamponade) • lower limb ischemia (cold legs) Aortic Dissection
Investigations • CT scan is gold standard • CXR • pleural cap • widened mediastinum • left pleural effusion with extravasation of blood • TEE • ECG: LVH (90%), +/- MI, pericarditis, heart block • aortography, MRI Aortic Dissection
Treatment • Type A • EMERGENCY CARDIAC SURGERY • may require putting patient on pump, hypothermic circulatory arrest, valve replacement, coronary re-implantation of aortic root • resection of intimal tear, reconstitution of flow through true lumen, replacement of the affected aorta with graft • Type B • MEDICAL MANAGEMENT • very rarely urgent operation for complications (expansion, rupture, gut/leg/renal ischemia, ongoing pain Aortic Dissection
Definition • localized dilation of an artery that is 2 x its normal diameter • true aneurysm: involving all vessel wall layers • false aneurysm: disruption of aortic wall with containment of blood by some layers of the aorta or a fibrous capsule made of surrounding tissue Aortic Aneurysm
Aortic Aneurysm Aortic Aneurysm
Etiology • DEGENERATIVE (matrix metalloproteinases) • atherosclerosis association • infection • cystic medial necrosis • trauma • vascultitis • connective tissue disease (Marfan syndrome, Ehlers-Danlos) Aortic Aneurysm
Epidemiology • incidence 5 to 32 per 100,000 for AAA • high risk groups: • 65 years and older • male:female = 4:1 • smokers • peripheral vascular disease, CAD, CVD • family history of AAA Aortic Aneurysm
Clinical Features • Vast majority ASYMPTOMATIC • RUPTURE • back pain • hypotension/syncope • pulsatile abdominal mass • ~100% mortality if untreated Aortic Aneurysm
Investigations • abdominal US (100% sensitive) • CT • Aortogram (false negative normal lumen size due to thrombus formation) Aortic Aneurysm
Treatment • Risk of rupture depends on size • <5 cm <5% / yr • 5-6 cm 10% / yr • 6-7 cm 15-20% / yr • >7 cm >20% / yr • Risk of dying from aneurysm surgery = ~5% Aortic Aneurysm
Treatment • Operate when • AAA reaches 5.5 cm in an otherwise healthy individual • >5 mm expansion in 6 months • symptomatic AAA • Rupture • contraindications: life expectancy < 1 year, terminal disease (cancer), significant co-morbidities (recent MI, unstable angina), severe dementia, advanced age Aortic Aneurysm
Treatment: Surgical • Surgical options: • open surgery with graft replacement • Endovascular aneurysm repair Aortic Aneurysm
Ruptured Aortic Aneurysm • EMERGENCY • clinical diagnosis class diagnostic triad (50% cases) • sudden onset back pain • shock (syncope/hypotension) • pulsatile mass • U/S in emerg or CT if stable • IV access, start fluid resuscitation, cross and match • EMERGENCY LAPAROTOMY and CLAMP AORTA • Prognosis • 100% mortality untreated, OR mortality rate 50%; 90%total mortality Aortic Aneurysm
Clinical Features - Claudication • Pain with exertion (usually calves) • relieved by short rest - two to five minutes • reproducible • P/E • hair loss, hypertrophic nails, atrophic muscle • pulses may be absent at some locations
Etiology • blockages in arteries to lower extremities due to atherosclerosis • Risk factors • smoking • DM • HTN • hyperlipidemia • family history • obesity • sedentary • male gender
Investigations • Ankle Brachial Index • Angiogram