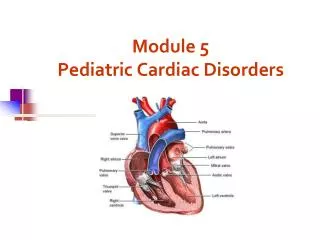
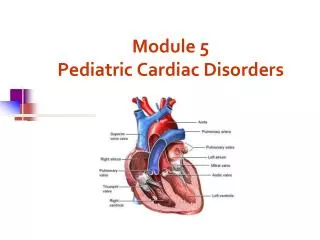
Module 5 Pediatric Cardiac Disorders
Module 5 Pediatric Cardiac Disorders Fetal Circulation What is the main route of blood flow through the fetal heart? Fetal Circulation Why does the blood flow in that route? Fetal Circulation What is the secondary route of circulation? And third route? Fetal Circulation

Module 5 Pediatric Cardiac Disorders
E N D
Presentation Transcript
Fetal Circulation What is the main route of blood flow through the fetal heart?
Fetal Circulation Why does the blood flow in that route?
Fetal Circulation What is the secondary route of circulation? And third route?
Fetal Circulation What is the stimulus for the change in circulation?
Intrauterine to Extrauterine What Happens after the Umbilical cord is Clamped?
Intrauterine to Extrauterine 1. Decreased pulmonary vascular resistance Increased pulmonary blood flow & Closure of ductus arteriosus 2. Increase pressure in left atrium, decrease pressure in right atrium Closure of foramen ovale
Oxygen Saturation • What is oxygen saturation? • What is normal oxygen saturation levels? • What values indicate hypoxemia? • Why is it important for the nurse to know the oxygen saturation levels? question 5
Congestive Heart Failure
Congestive Heart Failure • What is wrong with the heart?
Congestive heart failure • The inability of the myocardium to circulate enough oxygenated blood to meet the demands of the body. • When the heart fails, cardiac output is diminished. Heart rate, preload, contractitility, and afterload are affected. • Peripheral tissue is not adequately perfused. • Congestion in lungs and periphery develops.
Congestive Heart Failure • Why does the pump fail?
Congestive Heart Failure • What does the body do to compensate for this congestion and heart failure?
Compensatory Mechanisms • With a decrease in Cardiac Output • Stimulation of the sympathetic nervous system • Tachycardia - increases venous return to the heart which stretches the myocardial fibers and increases preload.
Compensatory Mechanisms • With a decrease in cardiac output • Decrease perfusion to the kidneys and glomerulus • Increased renin and ADH secretion • Increase in Na and H2O retention to increase intravascular volume
Early Signs of CHF • The earliest signs are often subtle: • Infant will have mild resting tachypnea • Increasing difficulty feeding
Signs and Symptoms • Pulmonary congestion • Tires easily during feeding • Tachypnea, Dyspnea, orthopnea • Signs of respiratory distress • Wheezing, rales and rhonchi • Easily fatigue • Impaired cardiac output • Tachycardia • Extremities cool, capillary refill >2 seconds • Diaphoretic, sweating, hypotension
Signs and Symptoms • Systemic venous congestion • Hepatomegaly • Edema • Weight gain • High metabolic rate • Failure to thrive • Slow weight gain
Treatment of Congestive Heart Failure • Medication Therapy • Digitalis – increases contractility and decreases heart rate. • ACE-inhibitors - arterial vasodilator / afterload reducing agent • Diuretics - enhance renal secretion of sodium and water by reducing circulating blood volume and decreasing preload. • Beta Blocker - increases contractility
Nursing Care How would the nurse recognize digitalis toxicity in an infant or child? What are the pulse rate criteria in administration of digitalis?
Pulse rates for Digitalis administration Infant – 100 BPM or greater Child – 80 BPM or greater Adolescent – 60 BPM or Greater
Digitalis • Digitalization • Given in divided doses • Maintenance • Given daily, usually in two divided doses • Therapeutic vs. Toxicity • Therapeutic range – 0.8 to 2.0 ng/ml • Toxicity • **EKG changes – arrhythmia • Slow pulse • Vomiting – very rare in infants
Digitalis • Hypokalemia potentiates digoxin toxicity
Treatment of Congestive Heart Failure • Diet – low sodium, small frequent feedings • Nursing care: • Measure intake and output – weighing diapers • Observe for changes in peripheral edema and circulation • If ascites present – take serial abdominal measurements to monitor changes. • Skin care • Turning schedule
Feeding the child with CHF • Feed the infant or child in a relaxed environment; frequent, small feedings may be less tiring • Hold infant in upright position; may provide less stomach compression and improve respiratory effort • If child unable to consume appropriate amount during 30-minute feeding every 3 hours, consider nasogastric feeding • Monitor for increased tachypnea, diaphoresis, or feeding intolerance (vomiting) • Concentrating formula to 27 kcal/oz may increase caloric intake without increasing infant’s work
Cardiac Catheterization Measure oxygen saturations and pressure in the cardiac chambers and great arteries Evaluate cardiac output
Cardiac Catheterization • Pre-care: • History and Physical • Lab work – EKG, ECHO cardiogram, CBC • NPO • Vital signs • Preprocedural teaching
Cardiac Catheterization • Post Care: • Check for bleeding or hematoma at insertion site • Keep leg immobilized and straight with bedrest in supine position • Monitor vital signs • Neurovascular monitoring of extremity distal to the catheter insertion • Measure I&O • Provide quiet diversional activities • Provide adequate fluids • Monitor vital signs for
Best Nursing Action • During post procedure assessment, the nurse notes bleeding at the insertion site. • What should the nurse do first?
Ask Yourself? • What is the most common assessment finding indicating a cardiac anomaly? • Answer: an audible heart murmur
Left-to-Right Shunting Defects Patent Ductus Arterious Atrial septal defects Ventricle septal defects
Atrial Septal Defect • Oxygenated blood is shunted from left to right side of the heart via defect • A larger volume of blood than normal must be handled by the right side of the heart hypertrophy • Extra blood then passes through the pulmonary artery into the lungs, causing higher pressure than normal in the blood vessels in the lungs congestive heart failure
Treatment • Medical Management • Medications – digoxin • Cardiac Catheterizaton - • Amplatzer septal occluder • Open-heart Surgery
Treatment • Device Closure – Amplatzer septal occluder During cardiac catheterization the occluder is placed in the Defect
Ventricle Septal Defect • Oxygenated blood is shunted from left to right side of the heart via defect • A larger volume of blood than normal must be handled by the right side of the heart hypertrophy • Extra blood then passes through the pulmonary artery into the lungs, causing higher pressure than normal in the blood vessels in the lungs congestive heart failure
Treatment Surgical repair with a patch inserted
Patent Ductus Arteriosus • Blood shunts from aorta (left) to the pulmonary artery (right) • Returns to the lungs causing increase pressure in the lung • Congestive heart failure
Treatment for PDA • Medical Management • Medication • Indomethacin - inhibits prostaglandin's which help keep the ductus arteriosus open • Surgery • Ligate the • ductus arteriosus
Treatment for PDA • Cardiac Catheterization • Insert coil – tiny fibers occlude the ductus arteriosus when a thrombus forms in the mass of fabric and wire
Cardiac Anomalies - Treatment When is surgery Performed? Why?
Obstructive or Stenotic Lesions Pulmonic stenosisTetralogy of fallotTransposition of the great arteriesTruncus arteriosus
Pulmonic Stenosis • Narrowing of entrance that decreases blood flow • Increases preload causes right ventricular hypertrophy
Obstructive or Stenotic Lesions • Treatment: • Medications – Prostaglandins to keep the PDA open • Cardiac Catheterization • Baloon Valvuloplasty • Surgery • Valvotomy
Aortic Stenosis • The aortic valve is thickened and rigid • Stenosis creates left ventricular hypertrophy • Left ventricle may not be large enough to eject a normal cardiac output.
Aortic Stenosis • Symptoms • Poor peripheral perfusion, feeding difficulties, CHF • Treatment • Balloon valvoplasty • Surgery
Coarctation of the Aorta • Narrowing of Aorta causing obstruction of left ventricular blood flow • Left ventricular hypertrophy
Signs and Symptoms • B/P in upper extremities • B/P in lower extremities • Radial pulses full/bounding and femoral or popliteal pulses weak or absent • Leg pains, fatigue • Nose bleeds
Treatment • Goals of management are to improve ventricular function and restore blood flow to the lower body. • Medical management with Medication • A continuous intravenous medication, prostaglandin (PGE-1), is used to open the ductus arteriosus allowing blood flow to areas beyond the coarctation. • Baloon Valvoplasty