Physician / Investigator Update
Physician / Investigator Update. Charles H. Pierce, MD, PhD Consultant in Pharmaceutical Medicine. Medical Research. Expected Mission: “Quality You Can Count On”. Physician Update Topics. “Phases” of Clinical research “Good Clinical Practice” “Quality Assurance” “Adverse Events”


Physician / Investigator Update
E N D
Presentation Transcript
Physician / Investigator Update Charles H. Pierce, MD, PhD Consultant in Pharmaceutical Medicine
Medical Research Expected Mission: “Quality You Can Count On”
Physician Update Topics • “Phases” of Clinical research • “Good Clinical Practice” • “Quality Assurance” • “Adverse Events” • “Standard Operating Procedures” • “International Conference on Harmonization”
Phase I Clinical Studies • First in man or normal healthy volunteer studies? • Designed to determine all critical clinical safety issues for the drug. • if you double the dose do you double the blood concentration? • effect of food • differences between gender and age
Phase IIa Clinical Studies • Establish the science of the drug in the patients for which the drug is intended • Confirm the mechanism of action of the drug in the target condition or disease • Establish safety in patients with the target condition or disease • Determine the dosage range in patients to manage the condition or disease • Usually confined but not always
Drug Development Statistics • Drug discoverers file patent • Patent exclusivity (no generics) = 17 years • Drug development time = 7 - 10 years • Application review = 2 - 3 years • Market exclusivity = 4 - 8 years • Drug development cost = $250 M - $400M • Target income/drug/year = $250 M - $1B
Investigational New Drug- IND - • Key milestone in drug development! • Signals that the company believes the drug can safely be administered to humans. • Once an IND is filed with the FDA, the company can start their first human study in 30 days; unless the FDA stops the study.
Drug Development Standards • Good laboratory practices (GLP) - Non-clinical safety studies • Good manufacturing practices (GMP) - Production operations - Drug Formulation Quality control • Good clinical practices (GCP) - Clinical studies Phases I to IV
Drug Development • Expensive & time consuming • Race to market • patent life is 17 years (no competition) • $1M - $3M /day for first to market • Safety of the drug is thoroughly tested in laboratory animals and people. • Efficacy of the drug has to be statistically proven efficacious in patients. • MRO’s are important in this process.
“Good Clinical Practice” • Ethics: Informed Consent, IRB • Operational Responsibilities Investigator Sponsor / Client Study Manager etc. • Adverse Events / Reactions • Data Management & Statistics • Quality Assurance
GCP - ICH Definition A standard for thedesign, conduct, performance, monitoring, auditing, recording, analyses, andreportingofclinical trials that providesassurancethat thedataandreportedresultsarecredibleandaccurateand that therights, integrity, andconfidentialityof trial subjects are protected. ICH - GCP Glossary (Final draft, May 1996)
Good Clinical Practice(An Operational View) To: prevent detect correct document Careless errors Violations Fraud / Misconduct Ethical problems
GCP - Objectives • Ethics: Rights of patients • Safety: Protection of patients • Efficacy: Utility of the product
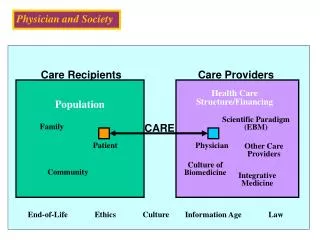
Registration Authorities Notification - Of starting - Of stopping - Adverse events Authorization Sponsor • Preparation of documents • Pharmaceutical products • Data management • Decisions on adverse events • Preparation of reports • Filing and archiving • Audit of systems and data Monitor Protocol, Inv. brochure On site visits information Amendments to protocol Clinical Laboratory - Equipment - Personnel - Certification Quality Investigator - Availability - Knowledge (product, protocol) - Trained team - Acceptance of monitoring - Acceptance of audit & inspection Ethics Committee - Independence - Composition - Written approval - Documented decision Severe Adverse Events Written Approval Product Information Consent Compliance with protocol Patients Ref: A. and T. Spriet, Good Practice of Clinical Drug Trials, Karger, Ed. 1992
GCP in Medical Research Document ! Document ! Document ! “If it is not written, it does not exist.” Dr. Lisook (FDA) Div. of Scientific Investigations Office of Compliance
Adverse Events (AEs) • Adverse experience (AE) • Adverse drug event (ADE) • Adverse drug reaction (ADR) • Adverse drug experience (ADE) • Adverse reaction (AR) • Side effect (SE) • Undesirable reaction (UR) • Unfavorable effect (UE) But not identical !
Adverse Events • Signs- findings eg. BP, temperature, skin rashes or bruises etc. • Symptoms - a change in function as abd. Pain, nausea, headache, lightheadedness • Laboratory Finding - incr. or decr. Abn. • Inter-current Illness - cold, URI etc. • Study Condition - caused by blood draw or ambient temperature
Adverse Event (AE) Defined Any untoward medical occurrence in a patient or clinical investigation subject who is administered a pharmaceutical product and which does not necessarily have to have a causal relationship with this treatment. ICH - GCP Glossary Draft 7 (March 31, 1995)
Adverse Experience vs. Adverse Drug Reaction(FDA Concept) Adverse drug reaction (ADR) is an adverse experience (AE) that is probably / possibly / remotely a reaction to a drug. (Concept of drug-relation.)
Adverse Experience: Attributes • Frequent / Rare • Benign / Serious • Predictable* / Unpredictable • Expected / Unexpected • Early occurrence / Late occurrence *Related to pharmacology / class
Adverse Drug Reaction: Types Type A Type B Pharmacologically predictable Dose-dependent Incidence and morbidity Mortality Treatment + + High Low Adjust dose - - Low High Stop After M.D. Rawlins and J.W. Thompson “Textbook of Adverse Drug Reactions”
Adverse Events Severity Seriousness Severity Intensity of an event (mild - moderate - severe) Seriousness Global evaluation of an event in terms of major consequences for life . .
Quality Assurance All thoseplannedandsystematicactions necessary to provideadequateconfidencethat a productor service will satisfyrequirementsfor“Quality You Can Count On”.
Quality Assurance The goal of a QA is to “minimize correction through early detection” by Monitoring studies and forecasting QA checkpoints to more efficiently utilize resources and minimize delays
Standard Operating Procedures“SOPs” • What are they • How are they defined • How important are they
SOPs - Defined • A set of pre-established written procedures for: - The organization, - The conduct, - The data collection, - The documentation, and - The verification ..… of a clinical trial
SOPs - Defined • A set of pre-established written procedures to ensure that the rights and integrity of the trial subjects are thoroughly protected and to establish the credibility of data and to improve the ethical, scientific, and technical quality of trials.
Standard Operating Procedures“SOPs” WHO does WHAT, WHERE, and WHEN NOT WHY or HOW Instructions Training Policy
Standard Operating Procedures • To establish consistency • To optimize time / manpower • To enhance teamwork • To protect the subject / patient • To assure compliance with GCP • To assure worldwide acceptance • To ensure quality of the data
International Conferenceon Harmonization (ICH) • What is it • How does ICH affect what we do
ICH: Efficacy Groups (GCP) (1) E1A: Extent of population exposure for clinical safety E1B: Prospective/retrospective studies of databases on population exposure • E2A: Expedited reporting: def./standards • E2B: Expedited reporting: format of reports • E2C: Periodic safety updates Clinical safety data management (ADE) :
ICH: Efficacy Groups (GCP)(2) E3: Clinical study reports: format/contents E4: Dose-response information for registration E5: Ethnic factors in acceptability of foreign clinical data E7: Clinical trials in special populations: Geriatrics
ICH: Efficacy Groups (GCP)(3) E6: Good Clinical Practices: consolidated guideline E6A: Addendum: Investigator’s brochure E6B: Addendum: Essential Documents
ICH: Efficacy Groups (GCP)(4) E8: General guidelines for clinical trials E9: Biostatistical issues in planning, analysis, and interpretation of clinical trials to support efficacy and safety E10: Choice of control groups in clinical trials