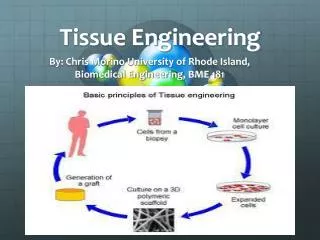
Tissue Engineering
Tissue Engineering. Mouse Ears . http://www.youtube.com/watch?v=PEc7QXAjsL4&feature=related. 1997 MIT. Engineering Tissue . http://www.youtube.com/watch?v=WvSxZ4JKQAY&feature=related. Corneal Tissue Engineering Blood vessel tissue engineering Liver tissue engineering

Tissue Engineering
E N D
Presentation Transcript
Mouse Ears http://www.youtube.com/watch?v=PEc7QXAjsL4&feature=related 1997 MIT
Engineering Tissue http://www.youtube.com/watch?v=WvSxZ4JKQAY&feature=related
Corneal Tissue Engineering Blood vessel tissue engineering Liver tissue engineering Cartilage tissue engineering Bone tissue engineering
Key Factors involving tissue engineering Scaffold( ceramics collagen, polymers) Cell Culture( stem cell, osteoblast, chondrocyte, hepatocyte Tissue/Organ regeneration Signaling Molecules (Growth Factors, proteins
Cell culture Interactive traids of responsive cells Scaffolds Supportive matrix Growth factors Bioactive molecules promoting differentiation and regeneration
Application of tissue engineering • Transplantation • Cellular and tissue • bases product • Alternative to animal • test 3D culture
1st generation 2nd generation 3rd generation Principle approach Performed tissue flaps 3D construct In vivo regeneration and guided tissue repair Autologous cell transplant Important component Delivery substances and scaffold( 體內重新建構) Growth factors and biomaterials(體內再生) Periosteal flaps( 修補組織 骨骼) Developing procedures used in cartilage tissue engineering
Cartilage Tissue Engineering • Autologous chondrocyte • 1. Isolation of tissue sample from patients • 2. Tissue regeneration by precursor cells • or embryonic stem cells • articular cartilage repair, nasal septal • cartilage scaffolds for cartilage for • tissue repair
ECM ( Extra cellular Matrix) ECM interaction directly influence cell signaling via cell adhesion molecules such as integrin and cadhedrin, fibronectin, collagen, laminin….
Extracellular Matrix in relation to epithelium endothelium and connective tissue Epithelial cell Basement membrane Endothelial lining the capillary Connective tissue with interatitial matrix Fibroblast
Steering Stem Cell Differentiation Differentiation of stem cells induced by binding to extracellular matrix components (e.g. proteins such as fibronectin, collagen and laminin)components http://inano.au.dk/organization/research-groups/nanobiointerfaces/research/steering-stem-cell-differentiation/
II. Scaffold for tissue construction 1. Act as shape and guidance template for in vitro and in vivo tissue development 2. Permit 3D immobilization and maintain differentiation materials: hyaluronic acid, collagen, alginate, chutosan, synthetic biodegradable poly( - hydroxy ester) polyacetic acid,( PLIA), polyglycolic acid( PGA), PLGA……
Embedding medium ( hydrogel) Polymer fiber Chondrocyte or Mesenchyma stem cell
Biosynthetic scaffolds Collagen scafold
Cells In vivo transplant Tissue scafold + and Growth factors
Engineering Organs from Scratch http://www.youtube.com/watch?v=0QJh0yc2mAI&feature=related
Tissue in cardiovascular structure • Advantages: • Avoid repeat operation • No rejection by the patients immune system • Cells behave like endothelial cells may have low thrombus formation and low infection • i.e. valves, blood vessels, vascular patches
Basic steps in tissue engineering of a cardiac valve Bone marrow cells harvest Valve scaffold Cell- scaffold construct
Approaches to create a vascular graft Cross linking Exogenous chemicals Mechanical stimulations Endothelial lining Cells + tubular scaffold Smooth muscle cells progenitor cells collagen gel/elastin fibrin Extra cellular matrix Biodegradable polymers Autulogous EC Circulating EPC Allogenic EC Embryonic stem cell Non-thromgenicity Immune response Remodeling In vivo implantation American Journal of Transplantation 2004; 4 (Suppl. 6): 36–42
How to Build a Beating Heart http://channel.nationalgeographic.com/series/explorer/4828/Photos/3671755be79cd210VgnVCM1000000100007fRCRD#tab-Videos/09347_00 http://channel.nationalgeographic.com/series/explorer/4828/Photos/3671755be79cd210VgnVCM1000000100007fRCRD#tab-Videos/10008_00 http://channel.nationalgeographic.com/series/explorer/4828/Photos/3671755be79cd210VgnVCM1000000100007fRCRD#tab-Videos/09346_00
Artificial skin • skin substitute • Adhere to the substrate, • Durable and sufficiently elastic • Tolerate some deformation • Allow evaporative water loss • Provide a microbial barrier • Promote homeostasis • Easy to use • Readily available immediately after injury, and elicit a • Regeneration-like response from the wound bed without evoking an inflammatory, foreign-body, or non- self immunologic reaction.
MSC (mesenchyma stem cells) Proliferate in cultures Differentiate into multiple mesenchyma lineage ie. correction of genetic disorder of , i.e bone cartilage
Preparation of 3-D mesenchyma cells Cell seeding on cotton gauze framed collagen substratum Formation of multilayer mesenchyma cells Physical detachment 3D culture
Preparation of 3-D mesenchyma cells Seeding of mesenchyma cells confluent mesenchyma cells Seeding of epithelial cells Coculture of epithelial and mesenchyma cells Detachment of epithelial cells –attached mesenchyma cell sheet Formation of hetero-spheroid
Osteoblast • Arise from mesenchyma cells( MSC) • MSC may be differentiate into osteoblast in vitro • Cultured osteoblast may form extracellular matrix in culture
Bone marrow derived osteoblast Cultured bone Transplantation of cultured bone cells T. Uemura et al. / Biomaterials 24 (2003) 2277–2286
Bone marrow derived osteoblast Cultured bone Transplantation of cultured bone cells T. Uemura et al. / Biomaterials 24 (2003) 2277–2286
Elastomeric PGS Scaffolds in Arterial Tissue Engineering http://www.jove.com/details.php?id=2691 Tissue Engineering -- Building Body Parts http://www.youtube.com/watch?v=ofiLcTs7_Ys&feature=related