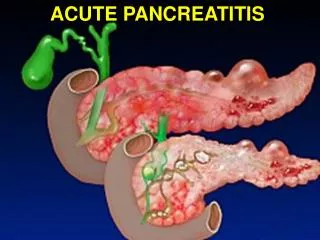
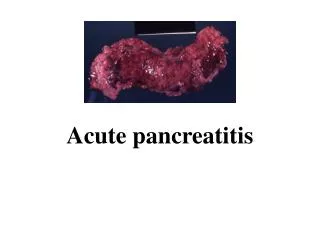
Acute Pancreatitis Evidence Based Approach
940 likes | 2.18k Vues
Acute Pancreatitis Evidence Based Approach. Pankaj Singh MD Director of Gastrointestinal Endoscopy Central Texas VA Health System, TX Assistant Professor Texas A&M University. Clinical Case. 32-year-old man c/o acute onset abdominal pain (presumed pancreatic origin) h/o alcohol intake.

Acute Pancreatitis Evidence Based Approach
E N D
Presentation Transcript
Acute PancreatitisEvidence Based Approach Pankaj Singh MD Director of Gastrointestinal Endoscopy Central Texas VA Health System, TX Assistant Professor Texas A&M University
Clinical Case • 32-year-old man • c/o acute onset abdominal pain (presumed pancreatic origin) • h/o alcohol intake
What do you think? • Amylase or lipase • Ultrasound or CT scan • If yes, When? • ICU or medical ward • Enteral nutrition or TPN • Antibiotics • ERCP • Surgery
Evidence • A. Proven • > 2 well designed trials, randomized • B. Possible/ Probable • 1 well designed study, randomized • C. Consensus • agreed opinion with no supportive evidence
Guidelines • Atlanta • British Society of Gastroenterology • International Association of Pancreas • Santorini Conference • World Congress of Gastroenterology
Background • Potentially fatal • Mortality – 0-25% • Necrosis determines the prognosis Panreas 1998 307-11
Background • Mild AP (no necrosis) – 0% • Sterile necrosis – 10% • Infected necrosis – 25%
Diagnosis • Laboratory • Amylase • Lipase • Radiological • US • CT scan
Blood tests • Amylase and lipase • Plasma level peak within 24 hours • t1/2 of amylase << lipase Gut 1997,41:431-35; Br J Surg 1998,84:1665-69.
Lipase has slightly higher sensitivity and specificity and greater overall accuracy than amylase (Evidence category A)
Ultra Sound (US) • Little part in the diagnosis of the acute pancreatitis • Role in biliary pancreatitis • Stones in gallbladder • Common Bile Duct dilation Br J Surg 1982;69:369-72
US findings should be examined in all patients with possible acute pancreatitis on admission (Evidence category B)
CT scan • Not necessary for the diagnosis • Diagnostic doubt • Atypical presentations • Asymptomatic hyperamylasaemia or hyperlipasemia Gastroenterol Clin N Am 1990;19:811-42
Routine use of CT scan within 24-48 hours of admission (Evidence category C)
Initial Management • Monitoring – temp., pulse, blood pressure, and urine output • Treatment – • Cardiopulmonary care • Sufficient fluid resuscitation • Pain control
Severity Stratification Rationale • Differentiate mild from severe acute pancreatitis
Desirable features of Markers of Severity • Accuracy - High sensitivity & PPV • Predictability within 24 hours of admission • Easy to use
Clinical Features • Clinical examination • Age > 70 years • Abdominal findings • increased tenderness • rebound • distension • hypoactive bowel sounds • In first 24 hours of admission - unreliable • After 48 hours- as accurate as Ranson score
Multiple Factors Scoring System • Ranson • Separate for alcohol and gallstone etiology • Score > 3 = severe acute pancreatitis • Glasgow • valid in all types of pancreatitis Both of these systems require 48 hours from the admission for full assessment Can J Gastroent 2003 325-328
APACHE II • Acute Physiology and Chronic Health Evaluation • as good as the Ranson or Glasgow at 24 and 48 hours of the admission • APACHE II score > 8 = Severe acute pancreatitis • Cumbersometo use if one does not use a pc or palm - where the formula is easily downloaded Br J Surg 1997,84:1665-69
If a multiple factor scoring system is to be used, the best choice at present appears to be APACHE II calculated at 24 hours - Evidence category A
Tests • Trypsinogen Trypsinogen activation peptide (TAP) I • Trypsin • Inflammatory cascade (IL6, IL-8, TNF-) II C - reactive proteinIII • Pancreatic injury • Amylase, Lipase, Trypsinogen IV
Markers for Leakage of Pancreatic Enzymes • Amylase/ Lipase • Degree of elevation shows little correlation with disease severity and prognosis • May have an inverse relationship with severity • Trypsinogen 2 • Excreted into the urine • Used as a screening test for acute pancreatitis
Trypsinogen activation peptide (TAP) • Small peptide • Advantage • Appear very early during the disease • Disadvantage • Limited "diagnostic window". • decrease very quickly irrespective of the course of the disease • Not suitable for rapid simple analysis
Markers of Inflammation • TNF-alpha • Major role in mediating inflammatory response • Conflicting reports as a predictor of severity • Interleukin-6 and 8. • Principal cytokine mediator • Measured in serum and urine • Discriminate severe from mild cases on day 1
C-reactive protein (CRP) • Acute phase reactant • Synthesized by the hepatocytes • Synthesis is induced by the release of interleukin 1 and 6 • Peak in serum is three days after the onset of pain • Most popular single test severity marker used today Isenmann et al Pancreas 1993;8:358-61
C-reactive protein (CRP) • Gold standard for the prediction of the necrotizing course of the disease • Accuracy of 86% • Readily available
C-reactive protein (CRP) Advantage • Used to monitor the clinical course of the disease Disadvantage • Not always present on admission • Lack specificity
Recommendations • CRP is currently the gold standard • Amylase and lipase of no value • High likelihood that IL-6/ TAP will replace the CRP
CT Scan • Normal • Homogeneous enhancement of the whole pancreas • Abnormal • Non-visualization of a part of the pancreas • Sensitivity of 90-95% • Specificity – 100%
Recommendation • A dynamic CT scan should be performed in all (predicted) severe cases between 3 and 10 days after admission (Evidence grade B)
Is It Possible to Predict Severity Early in Acute Pancreatitis? • Good clinical judgment • Specificity - 80% • Sensitivity - 40% • Scoring or biochemical methods • Specificity – 60% • Sensitivity – 95%
Etiological Assessment • Needed in all patients • Differentiate biliary from alcoholic pancreatitis • Early abdominal US is recommended in all patients (Evidence category A)
Initial Management of acute pancreatitis • Nutrition • Prophylactic Antibiotics • Acid suppression • ERCP • Surgery
Nutrition - Rationale • Hyper metabolic state • Total energy expenditure 1.5 x resting energy requirement • Nutrition depletion • Starvation • Preexisting protein-calorie malnutrition & micronutrient deficiency Crit care Med 1991;19:484-90; J parenter Enter Nutr 1989;13:26-29.
Nutrition – who needs it? • Mild AP • 70-80% recover within 4-7 days • Moderate to severe AP • Ranson score > 3 • APACHE II > 8 • Necrotic pancreas • Organ failure Windsor et al. Gut 1998,42:431-35; Kalfatentzos et al. Br J Surg 1997,84:1665-69
Parenteral nutrition Rationale for - • Pancreatic rest • Inability to tolerate enteric feeding
Parenteral Nutrition Rationale against • Pancreatic rest • Poorly defined • Increased risk of sepsis • Gut atrophy - increased bacterial translocation • Hyperglycemia • Greater costs
Parenteral Nutrition • Nine uncontrolled retrospective studies • Safe, well tolerated with few complications • No impact on the outcome
TPN Prospective randomized controlled trial 54 TPN IV F • Duration of hospital stay 16 10 • Line sepsis 10 1 Sax et al. Am J Surg 1987,153:117-22
Enteral Nutrition Rationale for • Minimal effect on pancreatic secretions • Prevention of gut mucosal atrophy • Avoid TPN related complications • Line sepsis • Hyperglycemia Arch Surg 1999;134:287-292
Enteral Nutrition Rationale against • Small degree of pancreatic stimulation • Proximal displacement of the feeding tube may worsen the disease outcome
Enteral nutrition • 4 prospective randomized controlled trials Significantly lower • Line sepsis • Infections per patients • Hyperglycemic episodes Cost was significantly higher in TPN No difference in mortality, ICU admissions, multi-organ failure Gut 1998,42:431-35; Br J Surg 1997,84:1665-69 JPEN 1997,21:14-20; J Submicrosc Cytol Pathol 1996,28:61-74.
Enteric feeding • Enteral nutrition is feasible, well tolerated and improves nutritional status • Enteral nutrition is certainly no worse than TPN and is less costly
How about Nasogastric feeding ? Aim • Assess the safety and practicability of NG feeding in severe acute pancreatitis Methods • Prospective study • 26 patients with severe acute pancreatitis • NG feeding within 48 hours of admission Eatock et al. International Journal of Pancreatology, 2000
Result • Pancreatic necrosis – 15 patients • Severe organ failure - 11 patients • Feeding • Well tolerated in 22 patients • No evidence of clinical or biochemical deterioration on commencing NG feeding
NG feeding appears safe, is well tolerated and is possible in severe acute pancreatitis