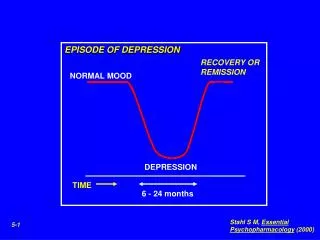
Depression
Depression. Dr. Aubrey H. Fine. For many years, children and adolescents were thought incapable of experiencing depression. It was considered an adult disease. 1975- National Institute of Mental Health met and discussed depression among children.

Depression
E N D
Presentation Transcript
Depression Dr. Aubrey H. Fine
For many years, children and adolescents were thought incapable of experiencing depression. It was considered an adult disease. • 1975- National Institute of Mental Health met and discussed depression among children. • 1977- Diagnosis and existence of depression in children and adolescents is recognized.
Major Depression Disorder (MDD) • Age of first onset of major depression is in adolescence and young adulthood • Adolescent depression is a chronic, recurrent and serious illness. • Children of depressed parents vs. children of non-depressed parents have 2 to 4 fold increased risk of depression. • Symptoms: twice as common in females, substance abuse, suicidal behaviors, social, occupational and educational disability.
Diagnosis 5 or more of the following symptoms must be present nearly every day during the same 2-week period to diagnose an adolescent with MDD • Depressed or irritable mood most of the day • Markedly diminished interest or pleasure in almost all activities, most of the day • Significant weight loss or gain, or change in appetite; failure to gain expected weight • Sleep disturbance • Psychomotor agitation or retardation
Diagnosis – con’t • Fatigue or loss of energy • Feelings of inappropriate guilt or hopelessness • Indecisiveness or diminished ability to concentrate • Recurrent thoughts of death or suicidal ideation, suicide attempt.
At least one of the following two symptoms must be present: depressed or irritable mood, or markedly diminished interest or pleasure in almost all activities. • MDD can be rated as mild, moderate, severe. • Diagnosed s chronic when episodes last more than 2 years.
An undetected diagnosis in adolescents is dysthymia- depressed or irritable mood that must be present for a year or longer and never be symptom free for more than 2 months. • 2 or more symptoms must be present: change in appetite, change in sleep, decrease in energy, low self-esteem, difficulty making decisions or poor concentration, feelings of hopelessness. • Adolescents with dysthymic disorder and who develop a major depressive episode are considered to have a “double depression”
Comoribidity • When depression is tied up with any number of other childhood mental illnesses • Anxiety disorders are the most common, with over 60% of depressed adolescents having a history or a concomitant anxiety disorder. • Social phobia (pathological self-consciousness) • Separation anxiety disorder (marked by fears about the well-being of the family) • Generalized anxiety disorder (a fear of the future and constant worries about one’s performance) • Of those who have both anxiety and depression, research indicates that 85% experience anxiety first.
One study at the New York University Child Study Center found that among children with anxiety disorder as preadolescents, 30% went on to have depression later on. • Peer relationships is a predictive factor in adolescent depression- not so much anxiety about relating with one’s friends but about whether they have friendships.
Conduct disorder or juvenile delinquency is frequently comorbid with depression in young people but the relationship between the two is controversial. Is the teenager depressed because he’s been caught doing something illegal or improper and is now facing consequences? Or is he depressed or demoralized about life, and this in turn leads to outrageous, illegal or oppositional-defiant conduct? • Some young people simply have both disorders at the same time.
Posttraumatic stress disorder (PTSD) also has an association with depression. • Occurs when a person witnesses or experiences a traumatic, fatal, or life-threatening event and later relives it, either in his thoughts or dreams. • Can bring extreme distress-intense fear, agitated behavior, flashbacks, and even physical reactions that might include re-experiencing smells. • A person experiencing PTSD might be jumpy, has trouble sleeping, and will take pains to avoid anything associated with the trauma.
Substance abuse in late adolescence with MDD is common. • Some people feel that depressed adults “medicate” themselves with drugs and alcohol, and that the same holds true for teenagers • Studies have found an association between adolescent depression and obesity, headaches, and asthma.
Risk Factors for Depression in Adolescence • Having a parent who has depression. Rates of depression are 2-4 times higher in children of depressed parents. • Having an anxiety disorder, especially in preadolescence, or a childhood history of depression • Being a female • Having a serious negative life event or an accumulation of damaging experiences (e.g. loss of social support systems, loss of a parent, a childhood history of physical or sexual abuse) • Poverty • Exposure to violence
Cognitive Vulnerability • Negative beliefs about themselves, the world and their future • Tend to make global, stable and internal attributions for negative events. • When confronted with stressful life events, these individuals will appraise the stressors and their consequences negatively and hence are more likely to become depressed than are individuals who do not have such cognitive styles.
Stress • Environmental conditions that threaten to harm the biological or psychological well-being of the individual • May occur either as an acute event or as chronic adversity, and as a major life event or as minor events with accumulated effects. • Events may be normative (school, transition) or pathological (abuse) • May be independent of, or directly related to an thus dependent on, and individual’s actions.
Link between stressful life events and depression in children and adolescents. • Depressive symptoms and disorders are highly associated with minor and major undesirable life events in children. • Negative life events are more prevalent among depressed than non-depressed children. • Stress that occurs as early as at conception likely contributes to an increased vulnerability to depression.
Examples of Stressors That are Associated with Depression • Childhood abuse or maltreatment • Sexual assault • Poverty (depression among low-income mothers is twice as high as in the general population) • Events such as disappointments, loss, separation, and interpersonal conflict
Interpersonal Relationships • Families with a depressed member are characterized by less support and more conflict. • Family dysfunction increases children’s risk of developing depression. • Depressed individuals are themselves more interpersonally difficult, which results in greater problems in their social network. • Family dysfunction, parent-child conflict, peer difficulties, and interpersonal rejection show that social problems precede depression and depression contributes to interpersonal difficulties. • Link between interpersonal vulnerability and depression is bidirectional
Mood Disorders • Bipolar disorder belongs to the category of mental-health experiences called mood disorders. • Primary feature is a significant change or disturbance in mood. • Mood disorders fall into four groups: • Depressive disorders • Bipolar disorders • Mood disorder due to a general medical condition • Substance-induced mood disorder
Diagnosis • Pediatric mania tends to be chronic and continuous rather than episodic and acute • Childhood-onset mania is a non-episodic, chronic, rapid-cycling, mixed manic state • Early-onset manics are more likely to have comorbid behavior disorders in childhood, and compared to adult-onset cases of mania, to have fewer episodes of remission over a 2 year period
“mixed mania” affects 20-30% of adults with mania • High rate of suicide • Poor response to treatment • Early history of neuropsychological deficits highly suggestive of ADHD
Criteria to diagnose bipolar disorder: • A distinct period of abnormally and persistently elevated, expansive, or irritable mood lasting at least 1 week • During the period of mood disturbance, 3 or more of the following symptoms have persisted and have been present to a significant degree:
Inflated self-esteem or grandiosity • Decreased need for sleep • More talkative than usual or pressure to keep talking • Flight of ideas or subjective experience that thoughts are racing • Distractibility • Increase in goal-directed activity • Excessive involvement in pleasurable activities that have a high potential for painful consequences
Comorbidity • Another mental-health experience overlapping or separate from bipolar disorder. • May share similarities with bipolar, making them challenging to pinpoint or diagnose. • It is critical to focus on symptoms, not behaviors
The systematic overlap of childhood mania with ADHD is one major source of diagnostic controversy. Rates of ADHD range from 60% to 90% in pediatric patients with mania. • Although ADHD has a much earlier onset than pediatric mania, the symptomatic syndromatic overlap between pediatric mania and ADHD raises a fundamental question- do children presenting with symptoms suggestive of mania and ADHD have ADHD, mania, or both?
With Conduct Disorder (CD) • CD is strongly associated with pediatric mania • Comorbidity between CD and major depression because pediatric depression often presages mania • CD includes violent behavior that may be categorized as mild, moderate, or severe. • Childhood-onset type (before age 10) • Adolescent-onset type (after age 10)
CD behaviors can start out slowly and build over an individual’s lifetime, ranging from lying, stealing, and physical fights to drug use, burglary, rape, and mugging. • 20-40% of kids with ADHD have CD • One way to distinguish CD from bipolar disorder is to determine if outbursts or episodes of manic symptoms can seen with other indicators of mania. To be diagnosed with CD, your child must be significantly sidetracked by the symptoms and must have an impaired ability to function throughout each day.
For a diagnosis of CD, your child needs to show a regular persisting pattern of violating rules and the rights of others • 3 of the following must have happened within the past year and one must have occurred in the past 6 months:
Physical cruelty to people or animals • Theft from someone in person • Forcing someone to engage in sexual activity • Violent use of a weapon to cause serious harm • Instigating physical fights • Bullying or threatening others • Arson • Destroying others’ property • Breaking into someone’s house, car, or other building • Conning or manipulating others • Shoplifting, credit card identity theft, forging checks • Breaking curfew • Running away from home overnight at least twice • Skipping school before age 13
With Anxiety Disorders • Pediatric studies of youth with panic disorder and youth with mania document a bidirectional overlap. • Subjects with panic disorder and agoraphobia had very high rates of mania • More panic and other anxiety disorders in children with mania. • Mania at any age is frequently comorbid with severe anxiety that requires additional clinical and scientific scrutiny.
With Substance Use Disorders (SUD) • Bidirectional overlap between mania and SUD in youth as well as adults • Juvenile-onset mania may be a risk factor for SUD
Risk Factors • Risk factors have not been clearly identified from community-based studies. • The most consistent risk factor for bipolar disorder is family history. • Offspring of adult bipolar patients has an increased risk, over 3-fold, of bipolar disorder as well as mood disorders, compared to offspring of controls.
Gender Gender is well known to be an important but poorly understood factor influencing the risk of MDD. The prevalence of MDD, while equal between boys and girls prior to puberty, doubles in young women after puberty. This increase in females has been hypothesized to be secondary to hormonal changes occurring during puberty.
Psychosocial Treatments for MDD • Behavior therapy • Cognitive therapy • Interpersonal therapy
Behavior Therapy • Primary goal is to increase the frequency of pleasant activities in the patient’s life • Found to be significantly better than psychotherapy, relaxation therapy, and medication • An efficacious, but not uniquely effective, acute treatment for MDD
Cognitive Therapy • Most widely studied psychotherapy for MDD • Treatment is based on the model that the cognitions of depressed individuals are negatively biased. Negative beliefs about the self, the world, and the future. • Typically 16-20 sessions over a period of 12-16 weeks
Involves both behavioral and cognitive techniques • Behavioral techniques serve to help patients engage in activities that give them pleasure, while cognitive techniques are used to evaluate the veracity of their beliefs. • An efficacious acute-phase treatment for MDD
Interpersonal Therapy • Depression is usually triggered by problems in four interpersonal domains: role transition, grief, interpersonal deficits, and interpersonal disputes. • In IPT, the interpersonal problem that triggered the current depressive episode is addressed and the person is helped to build communication and interaction skills to resolve it. • The acute phase of IPT typically lasts for 16-20 sessions.
Psychopharmacological Treatment for MDD • Monotherapy • Bupropion- blocks noradrenergic and dopamine reuptake. • Side effects: nausea, insomnia, increased anxiety, restlessness, increased incidence of seizures. No weight gain or sexual dysfunction.
SSRIs (Prozac, Zoloft, Luvox, Celexa, Lexapro and Paxil) • Make the most of the serotonin the body is producing at this time • The neurotransmitter (serotonin) lingers longer on the neuron receptors, giving it more of a chance to effectively complete the message it needed to send. • Rarely associated with fatalities and given its safety profile provides an easy treatment option for the clinician. • Side effects: headaches, nausea, dry mouth, insomnia, nervousness, sexual dysfunction, diarrhea, tiredness, and agitation
FDA issued an advisory to physicians that the use of antidepressant may lead to suicidal thinking or attempts in depressed youths. • FDA requested that a warning be added to the product label of these antidepressants
Antidepressant medications were not originally developed with children and adolescents in mind (nor were they tested on this population) • In addition to relieving symptoms of depression, antidepressants may also be prescribed for treating kids who grapple with other issues. • Phobias (often-school related) • Anxiety • Panic attacks • Eating disorders • ADHD • Bedwetting • OCD • Post-traumatic stress disorder
Dosages • Need to remember that the brains and bodies of children and teenagers are still growing and developing • Because bodies are often smaller than adults, the concentration of any medication in their systems is much greater • May lead to amplified side effects that are more intense than those found in adults if great care is not exercised
Careful Monitoring • Monitoring and follow-up is critical • Each medication has the potential to react differently in each child • May take weeks before you see any noticeable improvement in mood • Maintain careful communications with doctor
Pharmacotherapy for Bipolar Disorders • Mood Stabilizers • Lithium • Side effects: tremor, diarrhea, weight gain, increased urinary frequency, and gastrointestinal distress • Divaloproex and Carbamazepine • Lamotrigine • Antidepressants- should only be used with in combination with a mood stabilizer for the treatment of bipolar disorder
Prevention of Depression and Bipolar Disorder • The term prevention refers only to interventions that occur before the initial onset of a disorder • Efforts to identify cases and provide care for known disorders is called treatment • Efforts to provide rehabilitation and reduce relapse and reoccurrence of a disorder were called maintenance/interventions.
Universal mental health prevention interventions are defined as efforts that are beneficial to a whole population or group. • They are targeted to the general public or a whole population group that has not been designated or identified as being at risk for the disorder being prevented. • The goal at this level of prevention is the reduction of the occurrence of new cases of the disorder.
Selective mental health prevention interventions are defined as those efforts that target individuals or a subgroup of the population whose risk for developing the mental health disorder is significantly higher than average. • Indicated prevention interventions are defined as those efforts that target high-risk individuals who are identified as having minimal but detectable signs or symptoms that predict the mental disorder or biological markers indicating predisposition to the disorder.