ABO Blood Groups
ABO Blood Groups. Brian Poirier, MD UCDavis Medical Center. Topics. Basic genetics of ABO blood groups Formation of H, A, and B antigens ABO antigens and antibodies ABO testing ABO discrepancies. Objectives.

ABO Blood Groups
E N D
Presentation Transcript
ABO Blood Groups Brian Poirier, MD UCDavis Medical Center
Topics Basic genetics of ABO blood groups Formation of H, A, and B antigens ABO antigens and antibodies ABO testing ABO discrepancies
Objectives Describe the inheritance of the ABO Blood Groups and predict the ABO phenotypes and genotypes of offspring from various ABO matings Explain the roles of Secretor and H genes in the formation of H, A, and B antigens on the red cells Describe the reciprocal relationship between ABO antigens and antibodies for blood types O, A, B, and AB.
Objectives (Continued) Describe the procedures on ABO forward and back typings; interpret the results; and resolve any discrepancies if present. Describe the quantitative and qualitative differences between the A1 and A2 antigens. Correctly identify all the ABO compatible blood components for each blood type
Co-Dominance • A “Big” letter doesn’t mean dominant • A “small” letter doesn’t mean recessive • The exceptions to #1 and #2 are: • The Secretor genes: Se and se • The Lewis genes: Le and le • The H genes: H and h
Inheritance of the ABO Blood Groups First described by Bernstein in 1924. A, B, O genes on chromosome #9 The expression of antigens are based on the combination of three gene alleles: A, B, and O.
Phenotypes vs Genotypes PhenotypesGenotypes Group O OO Group A AA or AO Group B BB or BO Group AB AB
ABO Phenotype Frequencies in U.S. Populations Phenotype White Blk Mexican Asian O 45 49 56 43 A1 33 12 22 27 A2 8 8 6 Rare B 10 19 13 25 A1B 3 3 4 5 A2B 1 1 Rare Rare
Exercises Mother is type A and father is type O: What are the possible blood types for their offspring? Mother is type A and father is type B: What are possible blood types for their offspring?
Basic Biochemistry Type I and Type II chains Se gene H gene Formation of the H antigen Formation of the A and B antigens
Type I and Type II chains Type I: primarily glycoproteins in secretions and plasma • Saliva, clostrum, mothers’ milk, gastric fluid, bile, urine, serum, plasma, ovarian cyst Type II: primarily glycolipids on RBCs • RBC, WBC, platelets, normoblast, sperm, epidermal and epithelial cells
Se Gene and Formation of the H Antigen Secretor = SeSe, Sese; Nonsecretor = sese 80% of random population is either SeSe or Sese Secretor gene codes for fucosyl transferase Enzyme (FUT2) adds fucose to type I chains at terminal galactose; product is H antigen.
H Gene and Formation of the H Antigen Phenotypes: HH, Hh, hh Virtually 100% of random population is either HH or Hh; hh genotype (lack of H =“Bombay phenotype”) is rare. H gene also codes for fucosyl transferase (FUT1) Enzyme (fucosyl transferase) adds fucose to terminal galactose of type II chains Final product is H antigen
Type 2: H, A, and B Antigens • H Ag: Gal–GlcNAc–Gal-X | Fuc • A Ag: GalNAc–Gal–GlcNAc–Gal-X | Fuc • B Ag: Gal–Gal–GlcNAc–Gal-X | Fuc
“A” Gene and Formation of the A Antigen • H antigen is required for A antigen formation on RBCs or in secretions/plasma • Formation of A antigen: N-acetylgalactosamine is added to H antigen to make A antigen. • A Ag
“B” Gene and Formation of the B Antigen • H antigen is required for B antigen formation on RBCs or in secretions/plasma • Formation of B antigen: D-galactose is added to H antigen to make B antigen.
The Residual H Antigen • The more A or B antigen is made, the less H remains • Relative amounts of H by blood group O>A2>B>A2B>A1>A1B
The Use of Lectins for Antigen Confirmation Dolichos biflorus = anti-A1 Ulex europaeus = anti-H
Questions? • How is H antigen formed? • Relationship of Type I chain and Se gene • Relationship of Type II chain and H gene • How are A and B antigens formed? • What blood type has the highest amount of H antigen? What blood type has the least amount of H antigen? How would you determine that?
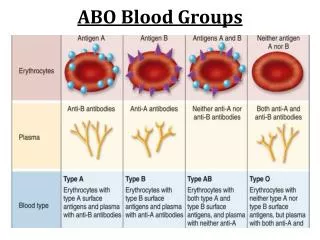
ABO Antigens and Antibodies • ABO antigens based on combinations of three genes: A, B, and O • Antibodies are clinically significant and “naturally occurring” • causing most fatal acute HTRs • some causing HDFN • ABO antibodies neutralized with secretor saliva.
Group O • Generally the most common blood group • Genotype: OO • Antigen: H • Antibodies: anti-A, anti-B, and anti-A,B • Antibodies are naturally occurring and very strong • Anti-A,B (mostly IgG) may cross placenta to cause HDFN
Group A • Genotype: AA, AO • Antigen: A, H • Antibodies: anti-B (primarily IgM) • A subgroups • A1 (80%) and A2 (20%) most important • A1 has more A than A2 (quantitative difference); qualitative differences, too. • ~25% of A2B’s form anti-A1 • 1-8% of A2’s form anti-A1 • Lectin of Dolichos biflorus agglutinates A1
Group B Genotype: BB, BO Antigen: B, H Antibodies: anti-A (primarily IgM) B subgroups: Not important
Group AB Genotype: AB Antigen: A, B, very little H Antibodies: None B subgroups: Not important A2B: 25% of A2B individuals produce anti-A1
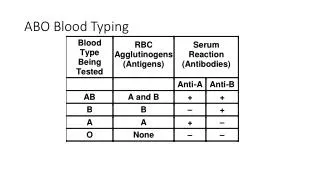
ABO Testing • Cell typing (forward grouping) to determine antigen types on RBCs • Serum/plasma typing (reverse grouping or backtyping) to determine type of antibody in serum: • Note the opposite reactions • If the forward reactions are opposite of reverse, an ABO discrepancy is not present.
ABO Grouping Reagents Forward Grouping Reagent Reverse or Back Tying Cells
Forward Grouping • Reagent: Monoclonal antibody • Highly specific • IgM • Expected 3+- to 4+ reaction • 1 drop • Anti-A=Blue; anti-B=Yellow (Acroflavin dye) • A and B antigens on patient red cells are agglutinated by known sera (anti-A, anti-B)
Reverse or Back Typing • Reagent Cells: Human Source • Expected 2+ to 4+ reaction • 4-5% cell suspension • 1 drop • Anti-A or anti-B antibodies in patient serum (or plasma) agglutinate with A1 and B antigens on Reagent cells
Forward Typing Procedures To determine what antigens are present on RBCs.
Step 4: Add one drop of 2-5% suspension of patient RBC to each tube.
Group A: 4+ Agglutination with Anti-A0 Agglutination with Anti-B