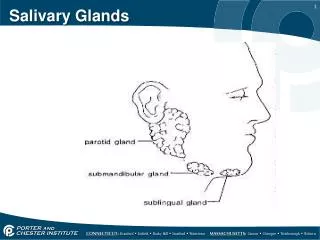
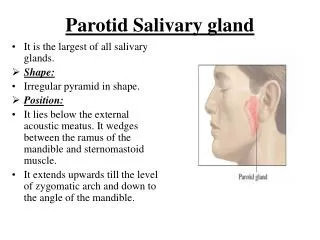
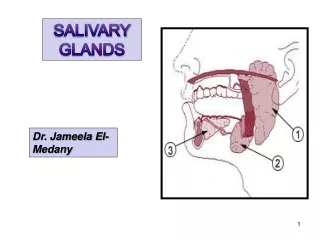
Salivary Infections
270 likes | 1.39k Vues
Salivary Infections. Viral endemic Parotitis (Mumps) Bacterial Sialadenitis. Mumps (Viral endemic parotitis). Mumps is an acute sialadenitis which caused by an RNA virus This RNA virus is the “paramxovirus” Other virus which can cause salivary infections are: Cytomegalovirus

Salivary Infections
E N D
Presentation Transcript
Salivary Infections Viral endemic Parotitis (Mumps) Bacterial Sialadenitis
Mumps (Viral endemic parotitis) • Mumps is an acute sialadenitis which caused by an RNA virus • This RNA virus is the “paramxovirus” • Other virus which can cause salivary infections are: Cytomegalovirus Coxsackieviruses Echovirus
Mumps (Viral endemic parotitis) CLINICAL FEATURES: • Airborne droplets transmit mumps virus • It mainly effects the parotid gland. • Children between the ages of 5-18 years are infected the most. • Once exposed the patient will develop the disease within 2-3 weeks • There is rapid swelling of the parotids bilaterally • There is an acute pain while salivation. cont……d
Mumps (Viral endemic parotitis) • The ear lobe is elevated as there is glandular enlargement. • There may be a purulent discharge from the parotid duct but it is clear and unremarkable. • As the acini become infected the salivary amylase leaks into the interstitium and is absorbed in the blood stream raising the serum amylase levels • Severe form of parotitis can lead to sterility.
Mumps (Viral endemic parotitis) HISTOPATHOLOGY: • The acini develop cloudy swelling making the connective tissue edematous • There is infiltration with plasma cells and the lymphocytes • The ductal lumens contain desquamated cell debris and leukocytes .
Mumps (Viral endemic parotitis) TREATMENT: • There no effective antiviral therapy available for the treatment of mumps. • Analgesics and antipyretics are given to control pain and fever • Liquid diet with vitamins should be considered • There should be complete bed rest.
Bacterial Saladenitis • Bacterial saladinitis usually occurs after surgery most commonly abdominal surgery. • The possible reason may be temporary lack of ductal flow which can develop while atropine sulphate is administered while delivering general anesthesia which allows ascending infections and thus pyogenic bacteria can inhibit the ducts. • Due to this there is pain and swelling . • Purulent exudate can be expressed from the orifice of the duct.
Immune Mediated Salivary Gland Diseases Lymphoepithelial saladenitis Sjogren syndrome
Sjogren syndrome • It is a group of autoimmune conditions with a marked predilection for woman, it has an intense T lymphocyte – mediated autoimmune process in salivary and the lacrimal glands as on of its most prominent component . • Sjogren syndrome exhibits T cells infiltration and replaces the glandular parenchyma .
Sjogren syndrome CLINICAL FEATURES: • It usually occurs in 0.5 – 1.0 % of the population. • This disease is not hereditary but certain genotypes have been identified. • Primary sjogren syndrome only effects the salivary glands and the lacrimal glands • Patients show kerato conjunctivitis. • Secondary sjogren syndrome exhibits other signs of autoimmune disease , of which the common are: cont…..d
Sjogren syndrome Rheumatoid arthritis. Collagen vascular disease Lupus erytmatosis Systemic sclerosis Mixed connective tissue disease . • The risk of developing extra salivary malignant lymphoma is increased.
Sjogren syndrome • 45% of SS patients have bilateral parotid swellings and the gland feels firm. • Some patients have involvement of the parotid gland and as well as the submandibular gland. • The most significant feature of SS is the dry mouth (xerostromia) and dry eyes (xeropthalmia) • Dry mouth and dry eyes have there own implications which are quite annoying.
Sjogren syndrome INVESTIGATIONS: • Blood complete picture will show raised ESR • Serological test for rheumatoid arthritis • Schirmer’s test for lacrimation. • Contrast sialography • MRI of the gland • CT scan • Finally biopsy for conclusive diagnosis.
Sjogren syndrome HISTOPATHOLOGY: • Immuno- marker studies shoe the presence of the B and the T lymphocytes. • The T lymphocytes are more in number • As the is increased infiltration of the lymphocytes the is more acinar destruction. • There is hyperplasia of the myoepithelial cells resulting in islands which no longer contain ductal lumens
Sjogren syndrome TREATMENT: • There is no effective therapy for SS. • Xerostromia become worse with time artificial saliva may be used to reduce the discomfort. • Usage of chewing gums to increase salivation has also shown some promise. • Dry eyes are managed by using eye drops (pilocarpine) • Root caries is managed by fluoride applications and filling materials. • Candidasis is managed by using anti-fungal drugs.