Endocarditis
Endocarditis. Lobna AL Juffali December2014. Introduction. 3-4 cases per 100,000 population per year Platlet – fibrin complex becomes infected with microorganisms (vegetation). Definition.


Endocarditis
E N D
Presentation Transcript
Endocarditis Lobna AL Juffali December2014
Introduction • 3-4 cases per 100,000 population per year • Platlet –fibrin complex becomes infected with microorganisms (vegetation)
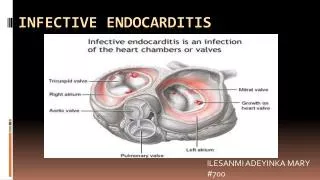
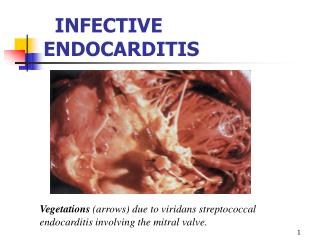
Definition • Endocarditis is an inflammation of the endocardium, the membrane lining the chambers of the heart and covering the cusps of the heart valves. • Infective endocarditis (IE) refers to infection of the heart valves by microorganisms, primarily bacteria.
Risk factors • Presence of a prosthetic valve (highest risk) • Previous endocarditis (highest risk) • Complex cyanotic congenital heart disease (e.g., single ventricle states) • Surgically constructed systemic pulmonary shunts • Acquired valvular dysfunction (e.g., rheumatic heart disease) • Hypertrophic cardiomyopathy • Mitral valve prolapse with regurgitation • IV drug abuse
Clinical Presentation Symptoms • fever, chills, weakness, dyspnea, night sweats, weight loss, and/or malaise. Signs • Fever • heart murmur • The patient may or may not have embolic phenomenon, • splenomegaly,
Clinical Presentation (skin manifestations) Osler’s nodes
Clinical Presentation (skin manifestations) Splinter hemorrhage
Laboratory Findings • The hallmark laboratory finding • is continuous bacteremia; (+ve blood culture) • three sets of blood cultures should be collected over 24 hours. • Leukocytosis • Anemia (normocytic, normochromic) • ESR • C-reactive protein • altered urinary analysis (proteinuria/microscopic hematuria
Duke criteria for the diagnosis of infective endocarditis and proposed modifications • Pathological criteria • Microorganisms demonstrated by culture or histological in a vegetation • Active endocarditis demonstrated by histological examination • Major criteria • Positive blood cultures • Evidence of endocardial involvement
Duke criteria for the diagnosis of infective endocarditis and proposed modifications Minor criteria • predisposing heart disease • fever >38°C • vascular phenomena • immunological phenomena • microbiological evidence (no major criterion) • suspect echocardiography (no major criterion
Duke criteria for the diagnosis of infective endocarditis and proposed modifications • Categories Definite: • Pathological criteria positive • or 2 major criteria positive • or 1 major and 2 minor criteria positive • or 5 minor criteria positive Possible: All cases which cannot be classified as definite or rejected • 1 major and 1 minor criterion positive • 3 minor criteria positive Rejected: • Alternative diagnosis • Resolution of the infection with antibiotic treatment for 4 days • No histological evidence
Other diagnostic tests • An electrocardiogram, • chest radiograph, • echocardiogram (valvular vegetations)
Streptococci Viridans Other streptococci Staphylococci Coagulase positive Coagulase negative Enterococci Gram-negative aerobic bacilli Fungi Miscellaneous bacteria Mixed infections “Culture negative” 60–80 30–40 15–25 20–35 10–27 1–3 5–18 1.5–13 2–4 <5 1–2 <5–24 Causitive microorganism %
DESIRED OUTCOME • Relieve the signs and symptoms of disease. • Decrease morbidity and mortality associated with infection. • Eradicate the causative organism with minimal drug exposure. • Provide cost-effective antimicrobial therapy. • Prevent IE in high-risk patients with appropriate prophylactic antimicrobials.
Factors associated with increased mortality include the following: • Congestive heart failure • Culture-negative endocarditis • Endocarditis caused by resistant organisms such as fungi and gram- negative bacteria • Left-sided endocarditis caused by Staphylococcus aureus • Prosthetic valve endocarditis (PVE)
GENERAL PRINCIPLES • The most important approach to treatment of IE includes • isolation of the infecting pathogen • determination of antimicrobial susceptibilities • followed by high-dose, bactericidal antibiotics for an extended period. • Treatment usually is started in the hospital, but in selected patients, it may be completed in the outpatient setting.
GENERAL PRINCIPLES • Large doses of parenteral antimicrobials usually are necessary to achieve bactericidal concentrations within vegetations. • An extended duration of therapy is required, even for susceptible pathogens, because microorganisms are enclosed within valvular vegetations and fibrin deposits.
Nonpharmamcological Therapy • Surgery is an important adjunct to management of endocarditis in certain patients. • valvectomy and valve replacement • The most important indications for surgical intervention in the past have been • heart failure in left-sided IE • persistent infections in right-sided IE.
Treatment • In patients with endocarditis of prosthetic valves or other prosthetic material caused by • viridans streptococci and Streptococcus bovis, treatment courses are extended to 6 weeks
Treatment The following conditions should all be present to consider a 2-week treatment regimen • The isolate is penicillin sensitive. • There are no cardiovascular risk factors. • No evidence of thrombotic disease. • Native valve infection. • No vegetation greater than 5 mm diameter. • Clinical response is evident within 7 days.
Staphylococci endocarditis • Endocarditis caused by staphylococci is becoming more prevalent,mainly because of • increased IVDA • more frequent use of peripheraland central venous catheters • increased frequency of valve replacement surgery. • Staphylococcus aureus is the most common organism causing IE among those with IVDA and persons with venous catheters. • Coagulase-negative staphylococci (usually S. epidermidis) are prominent causes of PVE
Staphylococci endocarditis • Is the organism methicillin resistant? • Should combinationtherapy be used? • Is the infection on a native or prosthetic valve? • Does the patient have a history of IVDA? • Is the infection on the left or right side of the heart?
Treatment * In patients with endocarditis of prosthetic valves or other prosthetic material addition of aminoglycosides is must for the first two weeks
HACEK Infective Endocarditis • Haemophilus spp. • Actinobacillus actinomycetemcomitans • Cardiobacterium hominis • Eikenella corrodens • Kingella kingae • Slow growing, fastidious Gram negatives likely • cause of Culture Negative Endocarditis
Treatment the treatment of HACEK infective endocarditis • ceftriaxone • ampicillin-sulbactam • oral ciprofloxacin for selected patients • Treatment is usually for 4 weeks, but it should be extended to 6 weeks in PVE caused by one of these organisms.
Aminoglycosides and Endocarditis • Aminoglycosides are ototoxic and nephrotoxic • Want to limit therapy to as short a period of time as possible to avoid toxicity – Staphylococci < 5 days – Enterococci will require 4-6 weeks
Aminoglycosides and Endocarditis • Control peak and trough concentrations • Elderly and/or renally impaired patients treated for extended periods of time are at greatest risk • Maintain gentamicinCpmax 3-5 mg/L & Cpmin < 1 mg/L • Present data would not support SDD
Vancomycin • Trough serum vancomycin concentrations are the most accurate and practical method for monitoring efficacy. • just before the fourth dose • trough level Above 15-20mg/dl • Red neck syndrome • Ototoxicity • nephrotoxicity
EVALUATION OF THERAPEUTIC OUTCOMES • assessment of signs and symptoms • Persistence of fever beyond 1 week may indicate ineffective antimicrobial therapy, emboli, infections of intravascular catheters, or drug reactions. • In some patients, low-grade fever may persist even with appropriate antimicrobial therapy.
EVALUATION OF THERAPEUTIC OUTCOMES • blood cultures should be negative within a few days, although microbiologic response to vancomycin may be unusually slower. • blood cultures should be rechecked until they are negative. During the remainder of the therapy, frequent blood culturing is not necessary.
EVALUATION OF THERAPEUTIC OUTCOMES • For all isolates from blood cultures, MIC should be determined. • When aminoglycosides are used for endocarditis caused by gram-positive cocci with a traditional three-times daily regimen, peak serum concentrations are recommended to be on the low side of the traditional ranges (3 to 4 mcg/mL for gentamicin). • Serum concentrations of the antimicrobial should generally exceed the MBC of the organism; however, in practice this principle is usually not helpful in monitoring patients with endocarditis.
Endocarditis prophylaxis Conditions in which prophylaxis is necessary • Prosthetic cardiac valves • Previous infective endocarditis • Congenital heart disease (CHD) • Unrepaired cyanotic CHD • Completely repaired congenital heart defect with prosthetic material or device, during the first 6 months after the procedure • Repaired CHD with residual defects at the site or adjacent to the site of a prosthetic patch or prosthetic device • Cardiac transplantation recipients who develop cardiac valvulopathy
Prophylaxis in Dental procedures • Endocarditis prophylaxis is recommended for all dental procedures that involve manipulation of the gingival tissue of the periapical region of teeth or perforation of the oral mucosa. • When antibiotic prophylaxis is appropriate, a single 2-g dose of amoxicillin for adult patients at risk, given 30 to 60 minutes before undergoing procedures associated with bacteremia.
Other procedures that require prophylaxis • Respiratory tract: • Tonsillectomy and or adenoidectomy • Surgical operations that involve an incision or biopsy of the respiratory mucosa
Case T.S. is a 48-year-old man who presents to the emergency department complaining of fever, chills, nausea/vomiting, anorexia, lymphangitis in his right hand, and lower back pain. He has no significant medical history except for kidney stones 4 years ago. He has no known drug allergies. He is homeless and an IV drug abuser (heroin) for the past year but quit 2 weeks ago. On physical examination, he is alert and oriented, with the following vital signs: temperature 100.8ºF (38ºC); heart rate 114 beats/minute; respiratory rate 12 breaths/minute; and blood pressure 127/78 mm Hg. He has a faint systolic ejection murmur, and his right hand is erythematous and swollen.
Case His laboratory values were all within normal limits. He had an HIV test done a year ago, which was negative. One blood culture was obtained that later grew MSSA. Two more cultures were obtained that are now growing gram-positive cocci in clusters. A transesophageal echocardiogram shows vegetation on the mitral valve.
Case Which one of the following therapeutic regimens is appropriate for T.S.? A. nafcillin IV therapy—antibiotic duration: 2 weeks. B. nafcillin IV plus rifampin therapy—antibiotic duration: ≥ 6 weeks. C. nafcillin IV plus gentamicin IV therapy—antibiotic duration: 2 weeks of both antibiotics. D. nafcillin IV plus gentamicin—antibiotic duration: 6 weeks (nafcillin) with first 3-5 days of gentamicin.