Endocarditis
Endocarditis. Dr. Gehan Mohammed Dr. Abdelaty Shawky. Endocarditis. * Types: (1). Non-infective endocarditis A. Rheumatic endocarditis. B. Verrucous ( libman sack) endocarditis: with SLE. C. Non-Bacterial thrombotic endocarditis. (2). Infective endocarditis

Endocarditis
E N D
Presentation Transcript
Endocarditis Dr. Gehan Mohammed Dr. Abdelaty Shawky
Endocarditis • * Types: • (1). Non-infective endocarditis • A. Rheumatic endocarditis. • B. Verrucous (libman sack) endocarditis: with SLE. • C. Non-Bacterial thrombotic endocarditis. • (2). Infective endocarditis • A. Acute Infective endocarditis • B. Sub-acute Infective endocarditis
RHEUMATIC HEART DISEASE • Rheumatic fever is a post-streptococcal immune-mediated inflammatory disease affect heart and extra-cardiac sites e.g. joints, skin, brain…. • The incidence and mortality of rheumatic fever has declined over the past 30 years (due to improved socioeconomic condition and rapid diagnosis and treatment of strep. pharyngitis).
* Pathogenesis: • An acute attack of streptococcal pharyngitis by group A beta-hemolytic streptococci. • Within 2-4 weeks after this attack anti-streptococcal antibodies are formed and attack the heart and the extra-cardiac sites. • The mechanism of this immune reaction is not yet understood, however, the most accepted hypothesis is antigenic similarity hypothesis.
Strep throat Antibody production Antibody cross-reaction with heart vegetations Aschoff body pericarditis
* Pathological features of Rheumatic Heart disease: • The characteristic lesion of acute rheumatic fever is the Aschoff body, consisting of a focus of necrosis (representing the site of antigen – antibody reaction) surrounded by activated histiocytes and lymphocytes. The histiocytes may be mononuclear or multinuclear, and are referred to as Anitschkow's or Aschoff cells.
These foci may be found in the pericardium, the myocardium, or uncommonly in the valves. • They ultimately "heal" by fibrosis.
- The disease passes into two phases; A. Acute phase: acute rheumatic pancarditis(inflammation of endocardium, myocardium and pericardium) • Myocarditis. • Pericarditis: "bread and butter", due to fibrinous inflammation • Endocarditis: edema, inflammation and fibrin deposits on valve leaflets (vegetations) along lines of closure. Mostly mitral and aortic valve. Aschoff nodules are uncommon in the valves.
B. Chronic phase: Acute changes may resolve completely or progress to scarring and development of chronic valvular deformities many years after the acute disease.
* Extra-caerdiac lesions of rheumatic fever: • These lesions are acute and resolve completely without disability. 1. Migratory polyarthritis: It causes "fleeting arthritis" in the large joints, self limited, no chronic deformities. 2. Skin: skin rheumatic nodules, erythema marginatum. 3. Sydenham chorea: a neurologic disorder with involuntary purposeless, rapid movements.
* Clinical features of Acute Rheumatic Fever: • Occurs 10 days to 6 weeks after pharyngitis • Peak incidence: 5-15 years. • Cardiac manifestations: pericardial friction rubs, weak heart sounds, tachycardia and arrhythmias. • Extra-cardiac: fever, migratory polyarthritis of large joints, arthralgia, skin lesions, chorea. • Pharyngeal culture may be negative, but anti streptolysin O (ASO) titer will be high.
* Jones criteria: A. Major criteria: • Carditis. • Polyarthritis • Sydenham’s chorea. • Erythema marginatum. • Subcutaneous nodules. B. Minor criteria: • Previous history of rheumatic fever. • Arthralgia. • Fever. • Lab tests indicative of inflammation : ESR (erythrocyte sedimentation rate), CRP (C-Reactive protein), leukocytosis. • ECG changes.
* Diagnosis of rheumatic fever: • Need 2 major criteria or 1 major and 2 minor criteria.
CHRONIC RHEUMATIC HEART DISEASE - Endocarditis heals by progressive fibrosis. Chronic scarring of the valves constitutes the most important long-term sequelae of rheumatic fever, and usually becomes clinically manifest decades after the acute process. • Left sided valves (mitral and aortic) are more commonly involved than the right. • Fibrosis of valve leaflets --> stenosis.
Fibrosis of chordae tendonae --> regurgitation (improper closure). • Other cardiac complications: • Subacute bacterial endocarditis. • Arrhythmia. • Chronic heart failure.
In valve stenosis: • Leaflets are thickened, fibrotic, shrunken with fusion • Dilatation and hypertrophy of left atrium (atrial fibrillation). • secondary deposition of Ca++ • fish mouth (button hole) stenosis - i.e. the stenosed valve looks like a fish's mouth • Lungs are firm and heavy (chronic passive congestion).
Pulmonary hypertension • Right side of the heart may be affected later (right ventricular hypertrophy). • In valve incompetence (regurgitation): • Retracted leaflets. • Left ventricular hypertrophy and dilatation.
* Mitral valve stenosis: • Leads to left atrial dilatation and failure, chronic venous congestion of the lung, lung fibrosis, pulmonary hypertension and chronic right sided heart failure.
* Mitral valve incompetence: • Leads to left ventricular dilatation and failure, left atrial dilatation and failure, chronic pulmonary congestion, lung fibrosis, pulmonary hypertension and chronic right sided heart failure.
Characterized by the deposition of small masses of fibrin, platelets, and other blood components on the leaflets of the cardiac valves. There is no infective organism (sterile). • Aortic valve is most common site. • Clinically: asymptomatic, if large: may embolize. * Pathogenesis/ association: • Subtle endothelial abnormalities. • Hypercoagulability. • Association with malignancy (50%).
Less common, non-infective endocarditis attributable to elevated levels of circulating immune complexes may occur in patients with systemic lupus erythematosus
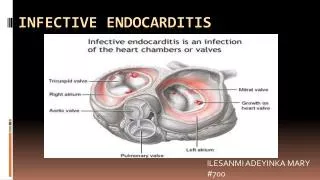
* Definition: infection of the cardiac valves or mural surface of the endocardium, resulting in the formation septic vegetations (thrombi). * Divided into: a. Acute infective endocarditis. b. Subacute infective endocarditis.
Acute infective endocarditis * Etiology: • Acute suppurative inflammation that affects healthy valves. • Organisms: Highly virulent as staph. Aureus, strept.hemolyticus and gonococci.
* Lesions: • Mitral & aortic valves are most commonly affected. Tricuspid is affected in IV drug abusers. • The mural endocardium may be also affected. • The affected valve and mural endocardium show acute suppurative inflammation + vegetations.
Vegetations are: * N/E: multiple, large, yellowish, friable found anywhere on the cusps. * M/P: the vegetations consist of platelet, fibrin, bacteria, numerous neutrophils & pus cells. • Myocardial shows microabscesses. • The pericardial sac is filled with pus.
* Complications: 1. Embolic complications: • Detached septic vegetations leads to systemic pyemia. 2. Toxemic complications: • Severe toxemia
* Prognosis: • Rapidly fatal due to; • Severe toxemia (septicemia). • Cusp perforation (acute heart failure).
Subacuteinfective endocarditis * Etiology: • Subacute inflammation that affects abnormal valves in; • Rheumatic valvulitis • Congenitally abnormal valves. • Prosthetic valves. • Caused by Less virulent bacteria as strept.viridans.
* Lesions: • Mitral & aortic valves are commonly affected. • The mural endocardium may be also affected • The affected valve and the mural endocardium show; the lesion of the corresponding disease (e.g. rheumatic, congenital) + vegetations.
Vegetations are: * N/E: multiple, large, gray, friable found anywhere on the cusps. * M/P: the vegetations consist of platelets, fibrin, bacteria and some inflammatory cells mainly histiocytes. • The Myocardium shows degenerative changes.
* Complications: 1. Embolic complications: • Infarctions: in kidney, spleen and brain, retina, heart. • Mycotic aneurysms: mainly in cerebral and mesenteric. • Petechial hemorrhage: in skin, mucous membranes and serous membranes. • Osler’s nodules: small. tender, intracutaneous nodules in pulps of fingers & toes.
2. Toxemic complications: • Moderate toxemia: fever, anemia, clubbing of fingers, splenomegaly, petechial hemorrhage and focal glomerulonephritis (flea bitten kidney)
* Prognosis: • Heal by fibrosis leads to valve lesion either stenosis or incompetence.
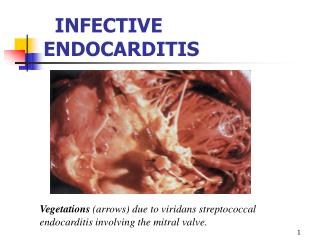
Endocarditis of the mitral valve (subacute, caused by Streptococcus viridens). vegetations are denoted by arrows.
C. Histologic appearance of vegetation of endocarditis with extensive acute inflammatory cells and fibrin. Bacterial organisms were demonstrated by tissue Gram stain. Slide 13.42