Understanding the Urinary System: Functions and Physiology
520 likes | 607 Vues
Explore the essential functions, anatomy, and physiology of the urinary system, including regulation of blood volume, waste excretion, and hormone synthesis. Discover the role of nephrons, renal corpuscles, and glomerular filtration in maintaining homeostasis. Learn about GFR regulation mechanisms and renal physiology processes.

Understanding the Urinary System: Functions and Physiology
E N D
Presentation Transcript
The Urinary System Chapter 26
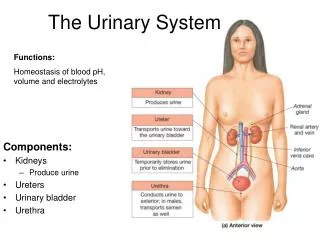
Functions figure 26.1 • ___________- • Excrete waste in urine • Regulate blood volume & composition (ions, pH) • Help regulate blood pressure • Synthesize glucose • Release erythropoietin • Participate in vitamin D synthesis • ___________ – transport urine from kidneys to urinary bladder • Urinary bladder– stores urine, capacity≈ 700-800mL • ____________ – discharges urine from the body
Kidney • Regulates ___________________ composition • Na+, K+, Ca2+ , Cl-, and HPO42- • Regulate _______________ • Excrete H+ • Conserve HCO3– • Reg. __________________ – conserve or elim water • blood volume bp, blood vol bp • Regulating ___________ • Secrete: renin bp, or adjust blood volume • Maintaining blood osmolarity- reg water & solute loss • Hormones: calcitrol (active Vit D), ________________________ • Regulate blood glucose- use glutamine in gluconeogenesis • Excreting waste and foreign substances
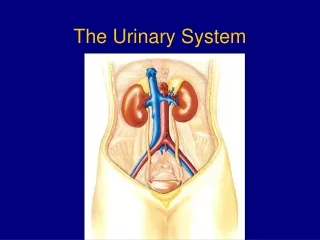
Kidney anatomy figure 26.3 • Retroperitoneal • 3 layers surrounding • Renal capsule – deepest • Adipose capsule • Renal fascia – superficial, anchors to ab wall • _______________- fissure where following emerge: • Renal aretery • Renal vein • Ureter • Internally, 2 distinct regions: • Renal _________ – superficial • Renal _________ – deep, arranged in renal pyramids
Nephron figure 26.5 a & b • Functional unit of the kidney, 2 parts: • _________________ – where blood plasma is filtered • Glomerulus – capillary network • Glomerular (Bowman’s) capsule – epithelial cup • _________________ – into which the filtrate is passed • Proximal convoluted tubule (PCT) • Loop of Henle (LOH) • Distal convoluted tubule (DCT) • Types: • __________ nephron- short LOH, blood from peritubular cap • __________________ nephron- close to medulla, long LOH • Long loops enable excretion of very dilute or very [ ]
Renal corpuscle fig 26.6 • __________________- capillary network • Glomerular (Bowman’s) capsule- double walled epithelial cup that surrounds the capillaries • Blood plasma is filtered & collected in capsule • Filtered fluid then passes thru renal tubule • _____________- visceral, modified simple squamous cells, wrap around glomerular capillaries & form inner wall of capsule • Outer wall (parietal) is simple squamous
Renal physiology, 3 processes • _______________________ • Water & most solutes: capillary renal capsule • _______________________ • Filtered fluid move thru tubule • Cells reabsorb 99% of water & useful solutes • Returns to blood via • Peritubular capillaries • Vasa recta • ________________________ • Removes substances from blood • Urine contains these excreted substances: wastes, drugs, excess ions
Glomerular filtration fig 26.8 • Filtration fraction- amt of plasma in ______________ that becomes glomerular filtrate = 16-20% of plasma • Daily volume of glomerular filtrate: • 150L female,180L male • >99% returned to blood, 1-2 L urine/day • Substances pass _________________: • Glomerular endothelial cells = fenestrated • Between capillaries mesangial cells – regulate GF • Basal lamina • Podocytes w/ pedicel create filtration slits • ____________ & ______________________ • Most plasma proteins, blood cells & platelets DO NOT
Net filtration pressure, figure 26.9 • Glomerular filtration dependent on these 3: • Glomerular blood hydrostatic pressure • Blood pressure in glomerular capillaries • Promotes filtration • Capsular hydrostatic pressure • Hydrostatic P exert by fluid in capsular space • Opposes filtration • Blood colloid osmotic pressure • Presence of proteins in blood plasma • Opposes filtration
Glomerular filtration rate (GFR) • Filtrate formed in renal corpuscles of both kidneys each minute • 125 mL/min male, 105 mL/min female • Homeostasis req it to be ≈ constant • If too ↑, substance not reabsorbed, lost in urine • If too , not enough waste excreted • Directly related to P determining NFP • Regulation: • Adjusting _______________ to glomerulus • Alter glomerular capillary __________- filtration
Regulation of GFR, table 26.2 • 1. _____________________ • Myogenic mechanism- smooth muscle contraction – wall of afferent arteriole • ↑ bp, stretch wall, smooth mus contracts, narrow lumen renal blood flow GFR • Tubuloglomerular feedback- macula densa provide feedback to glomerulus • If GFR ↑ due to ↑ bp, filtered fluid flows faster, less time for reabsorption nitric oxide not released & ________________ constricted
Regulation of GFR (2) • 2. _____ regulation- kidney bv supplied by SympNS • Release NE vasoconstrict (exercise, hemhorrrage) • Blood flow , GFR • urine output, conserve blood volume • ↑ blood flow to other body tissues • At rest, bv dilated & autoregulation occurring • 3. ___________ regulation- • Angiotensin II- GFR by vasoconstriction • Atrial natriuretic peptide (ANP) secreted when ↑ blood vol relax mesangial cells ↑ SA ↑ GFR
Tubular reabsorption • PCT • ______ & _______ reabsorbed in large quantities • ≈65% of filtered water reabsorbed • Na+/glucose (phosphate, sulfate, aa) symporters • Na+/H+ antiporter • _________ (HCO3-) reabsorbed- fac diffusion • _________ of water • Concentrates remaining solutes in PCT • Passive reabsorption of other solutes: • Cl-, K+, Ca2+, Mg2+, urea • Urea and ammonia ____________ by PCT
Tubular reabsorption (2) • Loop of Henle • Descending limb: • ___________ is reabsorbed (15% of filtered water) • Ascending limb: • Na+, K+, 2Cl- symporters • most K+ leaks back into tubule thru channels • Ca2+, HCO3-, • ____________- ascending LOH virtually impermeable to water • not automatically coupled to reabsorption of other solutes like in PCT • Filtrate osmolarity as ascend (ions, not water reabsorb)
Tubular reabsorption (3) • DCT: • Na+ Cl- symporter reabsorption • PTH causes reabsorption of Ca2+ • Water 10-15%, (at this point 80% already ab) • * by time fluid reaches end of DCT 90-95% of filtered solutes & water have been returned to bloodstream • Collecting duct: • ______ reabsorb thru leak channel Na+/K+pumpblood • ______ reabsorbed by intercalated cells, secreted in variable amounts thru leak channels of principal cells
Tubular secretion • Secretion of H+ helps control ___________ • Secretion of others for ____________ from body • PCT • H+ and NH4+ ions, urea • DCT • H+ ions, (K+ by principal cells at end of DCT) • Collecting duct • K+/ H+ /NH4+ ions (depending on salt, pH balance)
Hormonal effects table 26.4 • Angiotensin II-(released when blood volume, bp) • GFR • Stim antiporter reabsorb Na+, Cl-, H2O in PCT • Stim release aldosterone • Aldosterone: ( plasma K+) • K+ secretion, Na+, Cl-, H20 reabsorbed • ADH- ( osm of ECF or blood volume) • water reabsorption in DCT • ANP- (stim by atria stretch, blood volume) • secretion of Na+ (natriuresis) • Suppress reabsorption at PCT • urine output (diuresis) • ANP suppresses ADH & aldosterone secretion
Dilute & concentrated, fig 26.18 • Body __________ depends largely on kidney • Large volume, dilute urine when fluid intake • Asc LOH & DCT rel impermeable to water • End of DCT & collecting duct impermeable to water when ADH ________ • Small volume, concentrated: fluid intake • ADH enabled by osmotic gradient • Differences in solute & water permeability along LOH & collecting duct • Countercurrent flow in Des & Asc LOH
Countercurrent mechanism • Hairpin shape of LOH- countercurrent flow • Descending limb: one direction • Very permeable to water • I.F. osmolarity > than inside tube water→ out • As fluid moves down- gradient, osmolarity ↑ • Impermeable to solutes except urea • Ascending limb: opposite direction • Impermeable to water • Symporters reabsorb Na+, Cl- • Fluid osmolarity as ascending
Countercurrent mechanism (2) • ____________: loops working similar to LOH • Descending- renal medulla I.F. more [ ] • More Na+, Cl-, urea diffuse into blood • Blood osmolarity • Ascending- I.F. increasingly less [ ] • Ions diffuse out of Asc vasa recta • Reabsorbed water diffuses from I.F. vasa recta • Osmolarity of blood leaving vasa recta only slightly higher than what entered • O2 & nutrients dropped off w/out gradient
ORGANIC Urea Creatinine Uric acid INORGANIC Chloride Sodium Potassium Sulfates Phosphates Ammonia Calcium Magnesium Constituents of urine (lab, p60)
Diuretics • ______________ – elevated urine flow rate • Substances slow renal reabsorption of water • Often prescribed for _________________ • Lower blood volume lower bp • Most interfere w/mechanism for Na+ reabsorption • Naturally occurring: • Caffeine- inhibits Na+ reabsorption • Alcohol- inhibits ADH secretion
Dialysis- “to separate” • _________ of large solutes from smaller ones by diffusion thru selectively permeable mem • Kidneys so impaired that unable to function • __________dialysis- filter patient’s blood by removing wastes, excess electrolytes & fluids and return blood to patient • Hemodialyzer, dialysis membrane • Dialysate- solution formed to maintain diffusion gradients & add needed substances • Peritoneal dialysis- catheter & dialysate
Flow from nephron to urethra • (Nephron: Bowman’s capsulePCTLOHDCT) • Collecting duct • Papillary duct • Minor calyx • Major calyx • Renal pelvis • Ureter • Urinary bladder • Urethra
Micturition • Urination or voiding • Discharge of urine from urinary bladder • Voluntary (SNS) & involuntary (ANS) muscle contractions • When 200-400mL stretch receptors trigger ________________- S2-S3 spinal reflex • Contraction of detrusor • Relaxation- internal urethral sphincter muscle • Filling causes sensation before reflex occurs • _______________- lack of voluntary control