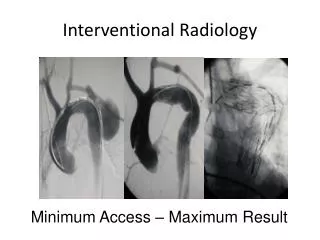
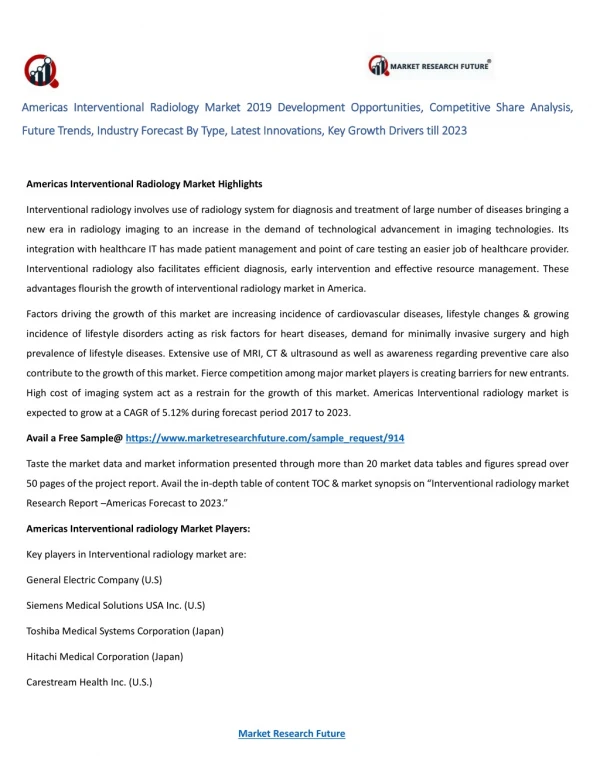
Interventional radiology for the diagnostician
Interventional radiology for the diagnostician. Jon Kirkland, DO. General. Coagulation parameters SIR guidelines Antibiotics SIR guidelines. Paracentesis. Location- Right or left lower quadrant most often. Consider image guidance, in particular for diagnostic.

Interventional radiology for the diagnostician
E N D
Presentation Transcript
Interventional radiology for the diagnostician Jon Kirkland, DO
General • Coagulation parameters • SIR guidelines • Antibiotics • SIR guidelines
Paracentesis • Location- Right or left lower quadrant most often. Consider image guidance, in particular for diagnostic. • How much? I personally will take up to 4-5 liters on the first time. Patients should be monitored by RN if first paracentesis. • If large volume, administer albumin (8G/L over 5L). • http://www.aasld.org/practiceguidelines/Documents/Bookmarked%20Practice%20Guidelines/ascites%20Update6-2009.pdf
M/M- <1%. Deaths is documented as RARE. • 8/9 patients who bled in a large study- renal failure. • No guidelines for routine checking INR or platelets. • Relative contraindications- DIC or fibrinolysis.
Thoracentesis • Ultrasound guided. OVER the rib. • First time- about 1.5 L. If more than that, chest tube. • Coagulation- See guidelines. (A lot more serious than Paracentesis). • M/M- low risk. Bleeding, PTX. Expansion pulmonary edema.
When to consider further treatment • Patients who have frequent paracentesis or thoracentesis need to be considered for more definitive treatment. • In the setting of recurrent paracentesis- liver transplant, TIPS, Pleurx catheter should be considered. • In the setting of malignant pleural effusion- pleurx catheter.
Biopsy • Coagulation parameters- See guidelines. • Consider having pathology on site- difficult lesion with necrosis on imaging. • Know what you are biopsing and why. • What to put the sample in- RPMI, formalin, sterile containter, renal solution, etc. If you don’t know, call pathologist.
Lung Biopsy • Shortest track without crossing unneccessary pleura. • Special care when in the hilum. • Avoid entering lung if at all possible for pleural based lesions. • Use a coaxial needle.
I like to biopsy the patient with the biopsy lung DOWN if at all possible (keeps the lesion from moving as much AND keeps hemorrhage in that lung if it happens). • Avoid additional pleural surfaces. • Take samples quickly, but cautiously. Extra time in increases your risk for bleeding and PTX.
Always scan for PTX and hemorhage upon completion. • If there is a instant PTX of significant size (>20-30%)- place a chest tube immediately. • Post-procedure monitoring for 2-4 hours. • High risk- CXR immediately and at 1-2 hours post op. • Lower risk- CXR 1-2 hours post op. • Always have patients on oxygen monitor and O2. • Use a AIRTIGHT dressing (tegaderm).
M/M • PTX- documented at 5-60%. I tell patients 1/3 get a PTX and 1/3 of them require chest tube. • Always talk to the patient about chest tube/admission prior to the procedure. • Hemorrhage- some hemorrhage is expected. Always tell patients about coughing up blood after procedure • Large hemorrhage- bleeding lung down and if necessary contralateral intubation. • Rare- air embolus, bronchopleural fistula, tract seeding, massive hemoptysis.
Chest tube placement • Use CT guidance if still in room. Can use fluoro. • Place a DART or a pigtail. Needle decompress if necessary. If using a pigtai, you can place a Yueh, wire and then put a small pigtail (7-8 Fr). • I like to use an atrium (-20mmHg suction). • Management- Admission, suction overnight. Clamp at 0600 and CXR at 0800. Keep clamped. CXR at noon and pull if clear. CXR 1 hour after pulling. If clear, consider additional CXR in 2 hours.
Liver biopsy • Either lesion or random. • Consider US or CT guidance. US is real-time and is preferred if possible. • For random- strongly consider left lobe ( use sandbag after procedure). • Avoid intercostal if possible ( anywhere intercostal can be transpleural!!) • Coagulation- See guidelines. Be strong! Transfuse during procedure if iffy. Consider trans-Jug. • Respiration suspension if possible. • Go through some normal liver prior to entering lesion.
Post-procedure CT advised- look for blood or other complications (PTX). • Right side down or sandbag (for left lobe) for 2 hours while hemodynamic monitoring. • Coach patients on signs/symtoms of volume loss.
M/M • Approximately 2% • BLEEDING!!! Know how to get out- Gelfoam, clot. • Needle tract seeding (exceedingly rare) • Infection • Damage to local structures (colon, stomach, bile ducts).
Pancreas • Eat when you can, sleep when you can, don’t f&*@ with the pancreas. • Consider other non-radiology biopsy methods (EUS). • M/M- Bleeding, infection, pancreatic necrosis, pancreatitis. • Consider amylase/lipase after pancreas biopsy if patient has N/V or new abdominal pain.
Adrenal • RESPECT THE ADRENAL GLAND • Always look at imaging. Could this be a pheo (consider urinary metabolic assessments and correlate with clinical symptoms). • Have hydralazine in the room. • Strongly consider phentolamine ( 1mg IV with titration of 5mg for BP control) Sodium nitroprusside for hypertensive crisis. Consult medicine.
Plan your route- Consider transhepatic if necessary (gelfoam the liver tract). • Risks- PTX, hemorrhage, adrenal crisis
Spleen • Get real- consult IR.
Renal • Lesion or random • Stay at one of the poles- avoid the hilum. • US or CT- depending on goal, comfort, etc. • Know what solution is needed. • High risk of bleeding- retroperitoneal hemorrhage can be very hard to diagnose. • Consider Gelfoam or clot. • Risks- Bleeding (significant), hematuria, infection, Tract seeding.
MSK biopsy • Talk to ortho first. If it is malignant, they are going to have a preferred surgical route and that will dictate how you biopsy.
Spine biopsy • Either under Fluoro (consider IR) or under CT. • Know your solutions. • Risks- Bleeding, infection, nerve damage (temporary or permanent), epidural hemorrhage. • Try and get a coaxial needle- Second biopsy is generally not as good as first biopsy. • Bone biopsy- often poorly touches off.
Abscess drainage • Know your path • Know your access options (Yueh, Hawkins, micropuncture) • Antibiotics! • Place atleast an 8Fr. Have a low threshold for 10-12 Fr. Use fascial dilators to make life easier. • Flush the catheter- place a three way stopcock and ensure the patient or family knows how to flush. Atleast daily- more is better.
Persistent high drainage- consider fistula. • Failure of resolution- TPA injection 2-4 mg TPA in 10-20mL sterile water. Inject and let dwell for 30-60 minutes. • Ready to remove- <10mL daily output, no fevers, no white count. • If the output goes from 100mL daily to nothing, consider failure to resolve. Image.
PICC • Order in which I consider veins- • Basilic • Cephalic • Lateral brachial • Median brachial
Myelogram • Lumbar- 12 mL Isovue M 200 • Cervical- 8mL Isovue M 300 • Access at L2-L3 (try and avoid areas with prior surgery if possible). • Know your approaches- Intraspinal, paraspinal, parasagittal. • For cervical- tilt the table and watch the column go cephlad. Catch the contrast at C6. • Myelogram images- Frontal. Laterals and flex/extend (standing). Consider obliques. • Cervical- Frontal. Laterals and obliques (cross table).
Risks- lowers seizure threshold, post-spinal headache. • Post-op- monitor for 2 hours while patient lays flat or HOB<30. • 24 hours of laying around. • If they get a headache- lay down. • If it persists- blood patch via anesthesia.
Sedation • Pain relievers- Fentanyl, Dilaudid, Morphine (longer acting). • Sedatives- Versed, Xanax, Ativan, Valium. • Benadryl. • Don’t be afraid of Marcaine with epi in appropriate location. • For me- one round to start (1mg Versed, 50mcg fentanyl). • Can always give more- can never take it back
Reversal • Romazicon for benzos. Benzo antagonist. Rapid onset. 0.2-1mg IV slowly (0.2mg/minute supposedly). Can repeat every 20 minutes. Lowers seizure threshold. • Narcan for fentanyl, etc. Competitive blocker of the opiate receptors, allowing liver to metabolize. 0.4 mg. repeat as necessary.
Conclusion • Own up to your complications- Noone is perfect. • Learn from your mistakes- Never make the same mistake twice. • You will have to leave your comfort zone- ALOT. • Know when to say no- Don’t kneejerk. • Practice now- sooner or later, it gets very real, very quick.