Endometriosis:
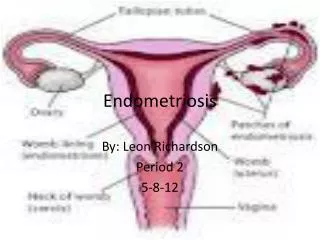
Endometriosis:. In this condition, tissue normally found only in the uterus starts to grow outside the uterus — in the ovaries, fallopian tubes, or other parts of the pelvic cavity. It can cause abnormal bleeding, dysmenorrheal, and general pelvic pain. Treating Menstrual Problems;.

Endometriosis:
E N D
Presentation Transcript
Endometriosis: In this condition, tissue normally found only in the uterus starts to grow outside the uterus — in the ovaries, fallopian tubes, or other parts of the pelvic cavity. It can cause abnormal bleeding, dysmenorrheal, and general pelvic pain.
Treating Menstrual Problems; • -To determine whether a problem requires treatment, the doctor will ask several questions and do a thorough physical exam. The doctor may do a pelvic exam, a Pap smear, blood tests (to check hormone levels), or urine tests. If there might be a structural problem or some sort of growth, an ultrasound or CT scan may be performed. Together, these tests can help the doctor determine how a condition should be handled.
-Growths such as polyps or fibroids can often be removed and endometriosis can often be treated with medications or surgery. If a hormone imbalance is to blame, the doctor will likely suggest hormone therapy with birth control pills or other hormone-containing medications.
-And for menstrual pain with no underlying medical cause, anti-inflammatory medicines are the most effective treatment. Conditions like clotting disorders or thyroid problems may require treatment with medications as well.
When to Call the Doctor? • -Although most period problems aren't cause for alarm, certain symptoms do call for a trip to the doctor. This is particularly true if a girl's normal cycle changes. So take your daughter to her doctor if she: • hasn't started her period by the time she's 15 or her period hasn't become regular after 3 years of menstruating. The most likely cause is a hormone imbalance (which may need treatment), but this also might point to another medical problem.
stops getting her period or it becomes irregular after it has been regular. Also let your daughter's doctor know if her cycle is less than 21 days or more than 45 days, or if she doesn't get a period for 3 months at any time after first beginning to menstruate. • has heavy or long periods, especially if she gets her period frequently. In some cases, significant blood loss can cause iron-deficiency anemia. Also, heavy bleeding could be a sign of a growth in the uterus, a thyroid condition, an infection, or a blood clotting problem.
has very painful periods. Having cramps for a couple of days is normal, but if your daughter isn't able to participate in her normal activities, let the doctor know. She might have a medical problem, such as endometriosis, causing the pain.
-Helping Your Daughter…. • -When your daughter's experiencing a particularly bad bout of PMS or cramps, you can help make her more comfortable. Suggest that she: • eat a balanced diet with lots of fresh fruit and vegetables • reduce her intake of salt (which can cause water retention) and caffeine (which can make her jumpy and anxious) • include foods with calcium, which may reduce the severity of her PMS symptoms • try over-the-counter pain relievers like acetaminophen or ibuprofen for cramps, headaches, or back pain • take a brisk walk or bike ride to relieve stress and aches
soak in a warm bath or put a hot water bottle on her abdomen, which may help her relax • -If you notice that your daughter's usual periods are causing her great discomfort and interfering with her life, talk to her doctor to make sure nothing else is causing the problem and to see if anything can help. Sometimes, hormone treatment, usually in the form of birth control pills, can help ease many symptoms associated with uncomfortable periods.
-But the most important way you can help your daughter feel more at ease about her period is to talk to her and explain that most annoying or uncomfortable conditions that accompany menstruation are normal and may improve over time. And be understanding when she's cranky and unhappy. After all, no one's at her best all the time — including you.
Toxic shock syndrome (TSS) • - is a serious but uncommon bacterial infection. TSS was originally linked to the use of tampons, but is now also known to be associated with the contraceptive sponge and diaphragm birth control methods. TSS has also resulted from wounds secondary to minor trauma or surgery incisions where bacteria have been able to enter the body and cause the infection.
-The symptoms of TSS include sudden high fever, a faint feeling, watery diarrhea, headache, and muscle aches. There are two types of this condition. The first, toxic shock syndrome, is caused by Staphylococcus aureus bacteria and has been associated with the use of tampons. (TSS was initially linked to a particular type of tampon, which has since been taken off the market.) Although the exact connection is still not clear, researchers suspect that certain types of high-absorbency tampons provided a moist, warm home where the bacteria could thrive.
-TSS can affect anyone who has any type of staph infection, including pneumonia, abscess, skin or wound infection, a blood infection called septicemia, or a bone infection called osteomyelitis. • -The second type of related infection, streptococcal toxic shock syndrome, or STSS, is caused by streptococcus bacteria. Most often STSS appears after streptococcus bacteria have invaded areas of injured skin, such as cuts and scrapes, surgical wounds, and even chickenpox blisters.
Toxic shock syndrome from staphylococcus starts suddenly with vomiting, high fever (temperature at least 102° Fahrenheit [38.8° Celsius]), a rapid drop in blood pressure (with lightheadedness or fainting), watery diarrhea, headache, sore throat, and muscle aches. • Within 24 hours, a sunburn-like rash appears. There also may be bloodshot eyes and an unusual redness under the eyelids or inside the mouth (and vagina in females). After that, broken blood vessels may appear on the skin. Other symptoms may include: confusion or other mental changes; decreased urination; fatigue and weakness; thirst; weak and rapid pulse; pale, cool, moist skin; and rapid breathing.
Prevention: • -The bacteria that cause toxic shock syndrome can be carried on unwashed hands and prompt an infection anywhere on the body. So hand washing is extremely important. • -Girls can reduce their risk of TSS by either avoiding tampons or alternating them with sanitary napkins. Girls who use only tampons should choose ones with the lowest absorbency that will handle menstrual flow and change the tampons frequently. Between menstrual periods, store tampons away from heat and moisture (where bacteria can grow) — for example, in a bedroom rather than in a bathroom closet.
-Because staphylococcus bacteria are often carried on dirty hands, it's important for girls to to wash their hands thoroughly before and after inserting a tampon. If your daughter is just starting her menstrual period, she should know about taking these precautions. Any female who has recovered from TSS should check with her doctor before using tampons again
Diagnosis and Treatment: • -Doctors typically diagnose TSS and STSS by doing a physical exam and conducting blood tests that assess a child's liver and kidney function. In toxic shock syndrome, doctors may want to rule out conditions like measles or Rocky Mountain spotted fever, which can produce similar symptoms. A doctor may also take samples of fluid from an abscess, boil, or infected wound to look for a possible source of staphylococcus or streptococcus infection.
-Doctors typically treat TSS with antibiotics. If there is a pocket of infection, like an abscess, a doctor also may need to drain the infected area. A child who has TSS is monitored for signs of shock until the condition has stabilized and seems to be improving. Steroids are also sometimes used to treat severe cases of TSS. • -As with TSS, doctors typically treat STSS with antibiotics and give intravenous fluids and medications to maintain normal blood pressure. Surgery is sometimes necessary to remove areas of dead skin and muscle around an infected wound.
When to Call the Doctor: • Call your doctor immediately if your child has any of the following signs and symptoms: • 1-Signs of shock: • - Go to the emergency department immediately or call an ambulance if your child has cold hands and feet; a pulse that is fast and weak; confusion or other mental changes; pale, moist skin; shortness of breath; abnormally fast breathing; or a strong feeling of anxiety or fear.
2-Signs of TSS: • - Look for fever; rash (especially a rash that looks like sunburn); nausea and vomiting; watery diarrhea; confusion or other mental changes; and decreased urination. If your daughter uses tampons, ask her to tell you immediately if she notices any unusual vaginal discharge, especially if it smells strange or bad. Most of the time that will be due to other causes, but no matter the cause, it still rates evaluation.
Signs of STSS: Look for the symptoms of shock listed above, plus a fever; blotchy rash; and an area of infected skin that is red, swollen, and painful. • -Once you realize that something is wrong, it's important to get medical attention right away. The sooner your child gets treatment, the quicker the recovery will be.