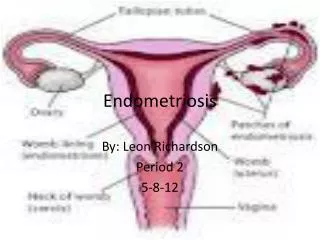
Endometriosis
Endometriosis. Endometriosis is defined as the presence of endometrial glands and stroma outside the endometrial cavity and uterine musculature. The pelvis is the most common site of endometriosis, but endometriotic implants may occur nearly anywhere in the body.


Endometriosis
E N D
Presentation Transcript
Endometriosis • Endometriosis is defined as the presence of endometrial glands and stroma outside the endometrial cavity and uterine musculature. • The pelvis is the most common site of endometriosis, but endometriotic implants may occur nearly anywhere in the body. • Endometriosis is a common gynecologic problem in reproductive-age women who have pelvic pain, dyspareunia, or infertility.
Pathogenesis • Several theories have been proposed to explain the histogenesis of endometriosis. The implantation theory proposes that endometrial tissue desquamated during menstruation passes through the fallopian tubes, where it gains access to and implants on pelvic structures. (Sampson’s) • The incidence of retrograde menstruation is similar in women with and without endometriosis.
Conti…. • Thus, the development of endometriosis could depend on the quantity of endometrial tissue reaching the peritoneal cavity, specific factors enhancing attachment of endometrial cells to the peritoneum and ovary, or the capacity of a woman's innate immune system to remove the refluxed menstrual debris. • The direct transplantation theory is the probable explanation for endometriosis that develops in episiotomy, cesarean section, and other scars following surgery. • Endometriosis in locations outside the pelvis likely develops from dissemination of endometrial cells or tissue through lymphatic channels or blood vessels.
The coelomicmetaplasia theory proposes that the coelomic (peritoneal) cavity contains undifferentiated cells or cells capable of dedifferentiating into endometrial tissue. • This theory is based on embryologic studies demonstrating that all pelvic organs, including the endometrium, are derived from the cells lining the coelomic cavity. • The induction theory, an extension of the coelomicmetaplasia theory, postulates that the refluxed endometrial debris releases a product that activates undifferentiated peritoneal cells to undergo metaplasia.
Anatomic alternations of the pelvis that increase tubal reflux of menstrual endometrium increase a woman's chance of developing endometriosis. The incidence of endometriosis is increased in young women with genital tract obstructions that prevent expulsion of menses into the vagina and increase the likelihood of tubal reflux. • Studies have suggested that deficient cellular immunity results in an inability to recognize the presence of endometrial tissue in abnormal locations. Decreased natural killer cell activity resulting in decreased cytotoxicity to autologous endometrium has been reported in women with endometriosis.
The presence of increased concentrations of leukocytes and their cytokine products in peritoneal fluid of women with endometriosis may play a role in the initiation and growth of the ectopic implants. The immune system clearly has an important, albeit unclear, role in the pathogenesis of endometriosis • The possibility of a familial tendency for endometriosis has been recognized for several decades. If a patient has endometriosis, a first-degree female relative has a 7% likelihood of being affected similarly. Studies are ongoing to determine the major susceptibility gene(s) involved.
Epidemiology • The true prevalence of endometriosis in the general population is unknown. Estimates of its prevalence are based on visualization of the pelvic organs. • Pelvic endometriosis is present in approximately 1% of women undergoing major surgery for all gynecologic indications, 6% to 43% of women undergoing sterilization, 12% to 32% when laparoscopy is performed to determine the cause of pelvic pain in reproductive-age women, and 21% to 48% of women undergoing laparoscopy for infertility. • Endometriosis is found in 50% of teenagers undergoing laparoscopy for evaluation of chronic pelvic pain or dysmenorrhea.
The influence of age, socioeconomic status, and race on the prevalence of endometriosis remains controversial. • The age at time of diagnosis is commonly 25 to 35 years, and endometriosis rarely is diagnosed in postmenopausal women. • Many believe that endometriosis is more common in women of upper economic classes because they delay pregnancy, which is postulated to increase the risk of developing endometriosis.
Pathology • The most common sites of endometriosis, in decreasing order of frequency, are the ovaries, anterior and posterior cul-de-sac, posterior broad ligaments, uterosacral ligaments, uterus, fallopian tubes, sigmoid colon, appendix, and round ligaments. Other sites less commonly involved include the vagina, cervix, and rectovaginal septum. • Uncommon locations include the inguinal canal, abdominal or perineal scars, ureters, urinary bladder, umbilicus, kidney, lung, liver, diaphragm, vertebrae, and extremities.
Symptoms • The common signs and symptoms of endometriosis are pelvic pain, dysmenorrhea, dyspareunia, abnormal uterine bleeding, and infertility. • The type and severity of symptoms are dependent on the extent of disease, the location, and the organs involved. Even limited amounts of disease may cause significant Symptomatology. • About 30% of patients are asymtomatic.
Pelvic pain : • Endometriosis is present in approximately one third of patients with chronic pelvic pain. The pain may be described as crampy, dull, or sharp and usually increases around menses. The discomfort may be unilateral or bilateral, and many patients complain of rectal pressure or low backache. Acute abdominal pain may result from hemorrhage secondary to a ruptured endometrioma.
Dysmenorrhea : • Dysmenorrhea is a more frequent complaint than dyspareunia. There is some correlation between the extent of disease and the severity of pain. • The pain begins before the onset of menstruation,builds up continously until the flow begins and declines gradually. • The pain variable from dull ache to grinding or crushing pain, colicky pain or a bearing down pain. Deeper lesions cause more pain than superficial ones. • Dyspareunia is more common in women with invasive endometriotic nodules in the cul-de-sac, uterosacral ligaments, rectovaginal septum, and vagina.
Abnormal uterine bleeding occurs in up to one third of women with endometriosis with symptoms of oligomenorrhea, polymenorrhea, and midcycle or premenstrual spotting. The abnormal bleeding likely results from conditions associated with endometriosis: • oligoanovulatory luteinized unruptured follicles, luteal phase defects, and other pathology such as uterine fibroids.
Bladder involvement is associated with frequency and urgency. Invasion of the mucosa results in hematuria. Ureteral and rare cases of renal endometriosis occasionally cause flank pain or gross Hematuria. • Symptoms suggestive of gastrointestinal involvement include, in decreasing order of frequency, diarrhea, rectal bleeding, constipation, and dyschezia. All symptoms usually are exacerbated catamenially
There are numerous case reports of extrapelvic endometriosis. • Pulmonary endometriosis causes catamenialhemoptysis and dyspnea. • Cutaneous lesions are associated with catamenial bleeding, tenderness, and swelling. • It is estimated that 25% to 50% of infertile women have endometriosis and that 30% to 50% of women with endometriosis are infertile. Although the association of endometriosis and infertility is well recognized, the path physiologic mechanisms are poorly understood.
Proposed Mediators and Mechanisms of Infertility : • Anatomic distortion and tubal obstruction • Anovulation, luteal phase defects, and hormonal abnormalities • Galactorrhea or hyperprolactinemia • Autoimmunity • Peritoneal leukocytes and the peritoneal inflammatory response • Peritoneal fluid prostaglandins • Peritoneal fluid cytokines • Embryo implantations defect and spontaneous abortions
Classification: • A number of classifications have been developed for staging endometriosis. The most widely used system was introduced by the American Society for Reproductive Medicine (ASRM) in 1979 and revised in 1985 and In 1996. • This system assigns a point score for the size and location of endometriotic implants and associated adhesions. • The new ASRM endometriosis classification for infertility includes the morphologic appearance of the implant.
Endometriosis is classified as minimal, mild, moderate, and severe. • Mild disease is characterized by superficial implants <5 cm2 in aggregate scattered on the peritoneum and ovaries. Minimal or no adhesions are present. • Moderate forms are characterized by multiple implants, both superficial and invasive. Peritubal and periovarian adhesions may be evident. • Severe forms are characterized by multiple superficial and deep implants, including large ovarian endometriomas. Filmy and dense adhesions usually are present.
Diagnosis:: • Endometriosis usually is diagnosed during the third and fourth decades of life. It has not been found in prepubertal girls and rarely is diagnosed in postmenopausal women unless they are taking replacement hormones. • Endometriosis should be suspected in any woman having the classic symptoms of pelvic pain, dysmenorrhea, dyspareunia, abnormal menstrual bleeding, and infertility. • Many women with endometriosis are completely asymptomatic, and endometriosis should be considered in all reproductive-age women with infertility or an adnexal mass.
Localized tenderness in the cul-de-sac or uterosacral ligament • Palpable tender nodules in the cull-de-sac, uterosacral ligament, or • rectovaginal septum • Pain with uterine movement • Tender, enlarged adnexal masses • Fixation of adnexa or uterus in retroverted position
Investigations : • Laparoscopic findings : should be used not merely for the diagnostic purpose , but the should be able to proceed with minimal invasive surgery. The diagnosis should be validated by peritoneal and tissue biopsy. • CA-125 :glycoprotein and cell surface antigen, is raised to more than 35U/ml in 80% cases, and the level is directly proportional to the extent of the disease. • USG and MRI :Transvaginal USG • Cystoscopy • Sigmoidoscopy
Treatment • The treatment of endometriosis is dependent on • (a) the severity of symptoms, • (b) the extent of disease, • (c) the location of disease, • (d) the patient's desire for pregnancy, and • (e) the age of the patient.
Expectant ManagementMedical therapyProgestinsLevonorgestrel-releasing intrauterine deviceDanazolGnRH analoguesAromatase inhibitorsSurgical therapy (laparoscopy or laparotomy) Conservative: retains uterus and ovarian tissue Definitive: removal of uterus and possibly ovariesCombination therapy Preoperative medical therapy Postoperative medical therapy
Expectant Management • Avoiding specific therapy is considered when patients have minimal or no symptoms and have suspected minimal or mild endometriosis. Patients in this category may benefit from nonsteroidal anti-inflammatory drugs (NSAIDs) and/or cyclic or continuous oral contraceptives to retard progression of the disease and protect against unwanted pregnancy. • One study suggests that surgical treatment of mild endometriosis results in higher pregnancy rates than expectant management. • If pregnancy occurs, regression or complete resolution of the disease is common.
Medical Therapy: • Endometriotic implant growth is highly dependent on ovarian steroids. • Medical therapy attempts to induce pseudo pregnancy or menopause, the two physiologic states believed to inhibit or delay progression of endometriosis by interrupting cyclic ovarian hormone production. • Progestin alone or in combination with estrogen hormonally mimic pregnancy. Danazol and gonadotropin-releasing hormone (GnRH) analogues induce a state of pseudomenopause. • Medical therapy has the following advantages over surgery: • (a) avoidance of the surgical risks of damaging pelvic organs and causing postoperative adhesions.
(b) treatment of implants that are not visible at surgery. • Disadvantages of medical therapy are the associated side effects, high recurrence rates following discontinuation of treatment, lack of an effect on endometrioma and adhesions, and inability to conceive because of medically induced an ovulation. • Medical therapy never has been shown to enhance fertility. Thus, it is not appropriate for women with advanced stages of endometriosis and adhesions causing symptoms or women desiring pregnancy. • The medications used most commonly to treat endometriosis are continuous oral contraceptives, progestins, danazol, and GnRH analogues.
Progestins inhibit endometriotic tissue growth by a direct effect on the implants, causing initial decidualization and eventual pseudodecidual necrosis or atrophy. They also inhibit pituitary gonadotropin secretion and ovarian hormone production. • Treatment may consist of medroxyprogesterone acetate (10 mg three times a day) or norethindrone acetate (5 mg daily for 2 weeks), increased by 2.5 mg per day every 2 weeks until a daily dose of 15.0 mg is reached. • Side effects include irregular menstrual bleeding, nausea, breast tenderness, fluid retention, and depression.
The effectiveness of continuous oral contraceptives or progestin in eliminating implants and the risk of recurrent endometriosis following treatment are not precisely known. Over 80% of women have partial or complete pain relief. • Low-dose cyclic oral contraceptives are effective in relieving dysmenorrhea in women with endometriosis
Danazol is the isoxazole derivative of 17-ethinyltestosterone and has the following three mechanisms of action: • (a) inhibition of pituitary gonadotropin secretion, • (b) direct inhibition of endometriotic implant growth, and • (c) direct inhibition of steroidogenic enzymes. • Danazol is given orally in divided doses, from 400 to 800 mg daily, generally for 6 months. Most women taking danazol have side effects, but only a small percentage of patients discontinue the drug because of unwanted effects. • Side effects, in decreasing order of frequency, include weight gain, muscle cramps, decreased breast size, acne, hirsutism, oily skin, decreased high-density lipoprotein levels, increased liver enzyme levels, hot flashes, mood changes, and depression.
The GnRH analogues profoundly suppress ovarian estrogen production by inhibiting pituitary gonadotropin secretion. • These medications are administered by nasal spray or depot injections. The usual dosage is 400.00 to 800.00 mg daily for nasal nafarelin, 3.60 mg for monthly subcutaneous goserelin, and 3.75 mg for monthly intramuscular leuprolide. • Side effects of the hypoestrogenemia are common and include hot flashes, vaginal dryness, decreased libido, insomnia, breast tenderness, depression, headaches, and transient menstruation. • GnRH analogue treatment for the recommended 6-month period decreases bone density and total body calcium, but most of the bone loss is reversible.
Aromatase inhibitors are a novel approach to inhibiting estrogen production in the endometriotic lesions themselves as well as in the ovary. • The two most widely used aromatase inhibitors are anastrozole (1.0 mg) and letrozole (2.5 mg) daily. • Aromatase inhibitors cause significant bone loss over time, and they should not be used alone, as they stimulate multiple ovarian follicular development. • They have been used successfully in combination with daily progesterone (200.0 mg) or norethindrone acetate (2.5 mg), GnRH analogues, or oral contraceptives.
Surgical Management • Surgery for endometriosis is considered conservative when the uterus and as much ovarian tissue as possible are preserved. • Definitive surgery involves hysterectomy with or without removal of the fallopian tubes and ovaries. • Surgery is indicated when the symptoms are severe, incapacitating, or acute and when the disease is advanced. • Surgery is preferred over medical therapy for advanced stages of disease with anatomic distortion of the pelvic organs, endometriotic cysts, or obstruction of the bowel or urinary tract.
Women who are older than 35 years, infertile, or symptomatic following expectant or medical management should be treated surgically. • Laparoscopy is the preferred approach to perform conservative surgery. Treatment of endometriosis is possible during the initial laparoscopy, which is used to diagnose the condition. • This offers the advantage of ablating the implants and adhesions while avoiding possible progression of disease or symptoms and the expense and side effects of medical therapy.
Disadvantages include possible damage to the bowel and bladder, infection, and mechanical trauma that may result in adhesion formation. • Conservative surgery involves excision, fulguration, or laser ablation of endometriotic implants and removal of associated adhesions. The goal is to restore normal pelvic anatomy. Surgery effectively removes pathology and restores normal anatomy in most cases. • The disease recurrence risk is estimated to be as much as 40% with 10 years of follow-up. Pain relief is achieved in 80% to 90% of patients. • Approximate pregnancy rates after surgery in patients with mild, moderate, and severe endometriosis are 60%, 50%, and 40%, respectively.
. Definitive surgery for treatment of endometriosis is indicated when significant disease is present and pregnancy is not desired, when incapacitating symptoms persist following medical therapy or conservative surgery, and when coexisting pelvic pathology requires hysterectomy. • The ovaries may be conserved in younger women to avoid the need for estrogen replacement therapy. • Removal of both ovaries is appropriate when the ovaries are damaged extensively by endometriosis or when menopause is approaching.
Combination Medical and Surgical Therapy • Medical therapy is used before surgery to decrease the size of endometriotic implants and thus reduce the extent of surgery. • When complete removal of implants is not possible or advisable, postoperative medical therapy is used to treat residual disease. • Progestin, danazol, or GnRH analogues may be used in conjunction with conservative or definitive surgery.