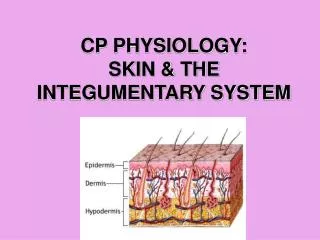
Chapter 8 Skin Physiology
Chapter 8 Skin Physiology. Key Terms . Skin Physiology- study of the skins function Skin Histology- microscopic study of the skin’s tissue Dermatology- study of skin Dermatologist- MD who specializes in the skin, hair and nails. Functions of the Skin.


Chapter 8 Skin Physiology
E N D
Presentation Transcript
Key Terms • Skin Physiology- study of the skins function • Skin Histology- microscopic study of the skin’s tissue • Dermatology- study of skin • Dermatologist- MD who specializes in the skin, hair and nails
Functions of the Skin • Protection- shields internal tissues from external elements • Absorption- certain types of ingredients are allowed to enter the skin • Secretion- sebum is secreted through the hair follicle giving us an acid mantle • Excretion- sweat allows our body to rid itself of waste • Regulation- 98.6 by goosebumps, shivering, blood flow increases and sweat production • Sensation - nerve ending that contain stimuli
Mitosis Steps: 1.Nucleus Splits 2. Cytokinesis 3.Cell Membrane split Resulting: in 2 daughter cells
What makes up the skin? • A Protein Called KERATIN • Hard Keratin – Hair and Nails • Soft Keratin – Skin Keratin is made of these Chemical Elements: C – Carbon O- Oxygen H- Hydrogen N- Nitrogen S- Sulfur
Keratin • Keratincytes produce large amounts of the protein keratin, once that is made is forms fibers. The tightly interlocked cells filled with keratin fibers are surrounded by keratohyalin (a protein substance that forms keratin)
The Epidermis • Outermost layer of the skin • NO blood vessels in this layer • Epidermis cells are called epithelial cells • Is composed of keratinocytes, which consist of the protein keratin • Like the shingles on a roof • Made up of 5 layers
Stratum Corneum • “Horny Layer” • Toughest layer of the epidermis • Keratinization ends. (The chemical process of living cells into dead protein cells) • Desmosomes keep these dead cells connected • These dead protein cells remain in this layer for about 28 days. • Squamous Cells- these serve as protection and aids in moisture balance by acting as a barrier
Stratum Lucidum • Clear transparent layer • Thickest on the palms and soles • Epidermal ridges and whorls (fingerprints and traction) • Prism
Stratum Granulosum • “Granular Layer” • Keratinization begins ( the nucleus and other organelles begin to disintegrate and die as they are traveling up through this layer and those above) • Cells continue to move upward through this layer
Stratum Spinosum • “Spiny Layer” • 8-10 cell layers thick • Langerhans cells – these cells alert the T-cells of antigens by displaying a key part of the antigen material on it’s cellular membrane • Not present in all areas of skin
Stratum Germinativum • “Basal Layer” • Mitosis occurs and cells take 25-30 days to travel from this layer to the stratum corneum. • Only living layer in the epidermis • Hemidesmosomes – help the epidermis attach the dermis, intercellular cement. Which is called the basement membrane • Merkel Cells – touch and sensory receptors • Melanin present in this layer
Melanin vs. Pigment • Melanin is the body’s natural coloring • Pigment refers to natural or artificial coloring • 3 things impact a persons skin color: • The amount of melanin • The type of melanin (eumelanin and pheomelanin • The distribution of melanin
The Dermis • “True Skin” • 25 x thicker than the epidermis • Connective tissue • Fibroblast cells – formation of collagen (Structure) and elastin (Stretch) • 70% of the dermis is made up of collagen • Elastin should stretch to 2x its size • Mast cells- produce histamines
Papillary Layer • Rich in Blood Vessels • Provides nutrients to the epidermis with fingerlike projections • House sensory nerve ending • Thermo receptors- hot or cold • Mechano receptors- movement • Tactile receptors- gentle touch or pressure
4 main receptors for sensation • Meisner’s Corpuscles- Light pressure and cold • Ruffini’s Corpuscles – Longterm pressure and heat • Pacinian Corpuscles – Deep pressure and pain • Krause’s End Bulbs – Pressure and pain receptors
Reticular Layer • Contains fewer blood vessels • Contain the sweat and oil glands
Sudoriferious Glands • Produce sweat (H2O, urea, electrolytes, and lactic acid) • Controlled by the nervous system • Has its own pore opening • 2 types • Apocrine – arms, genitals and nipples, odorless substance triggered by emotion • Eccrine- throughout the body, influenced by the sympathetic nervous system which produce physiological responses • What causes body odor then?
Sebaceous Glands • Produce sebum (oil) • All over the body except the palms and soles • Attached to the hair follicle • Influenced by the male hormone androgen • Helps create Acid Mantle
The Subcutaneous Layer • Composed of adipose tissue (fat) • Body’s shock absorber • Gives contour and shape • Serves as an emergency reservoir for nutrients, water and energy
CTR – Cell Turnover Rate • Factors: • Age • Sun Exposure • Use of exfoliating agents • Skin conditions
Exfoliation • Manual – physical process of removing dead cells from the surface of the skin • Chemical- using a chemical reaction to remove the dead cells from the surface of the skin.
Transdermal Penetration • The process of skin absorption • 4 ways products are absorbed: • Pores • Follicles • Intercellular cement • Oil and sweat glands • Factors affecting skin absorption: • Condition of the stratum corneum • Hydration level • Oiliness of the skin • Size of the products molecules • Temperature of the skin
Primary Lesions • Macule- large freckle • Wheal- raised pink swelling, caused by an allergic reaction • Papule- does not contain pus, red and elevated • Pustule-(zit) filled with bacterial fluid and pus • Vesicle- blister • Nodule- solid mass within the skin • Cyst- abnormal membrane sac containing a gaseous liquid or semi solid substance
Secondary Lesions • Crust- scab • Excoriation- scratches to surface of the skin • Scale- shedding of dead skin cells • Scar- formation resulting from lesion • Fissure- crack or line in the skin • Ulcer- open lesion
Dermatitis “inflammation of the skin” • Atopic- genetic, have sensitivities, temp changes aggravate, avoid hot showers and baths • Contact- rash caused by allergic reaction • Seborrheic- form of eczema, pink, yellow patches
Psoriasis • Genetic • Excess of thick, scaly, silvery skin • Caused by increased growth of skin cells • Can become thick requiring exfoliation
Eczema • Dry or moist lesions • Eruption of small vesicles and watery discharge and then dries • Not contagious but refer to MD
Infections • Herpes simplex – viral, no cure, contagious • Herpes Zosters- Shingles
Infections • Impetigo- staph infection, honey yellow crusted lesion • Tinea- ringworm, contagious fungal disease
Infections • TineaCorporis- fungal infection on the arms, trunk and legs • TineaVericolor- tricolor yeast infection
Infections • Verruca- most common tumor, Warts, (HPV) • Candida Albicans – yeast infection • Pink Eye- inflammation of the membrane of the eyelid
Sebaceous Disorders • Asteatosis- reduced sebum production • Seborrhea- excess secretion of sebum • Steatoma-harmless cyst filled with sebum • Furnucle- boil • Carbuncle- group of boils
Rosacea • Chronic inflammatory condition • Couperose dilated and inflamed • Can be accompanied with acne type papules and pustules • Prevalent in fair skin types and women • A more severe type is rhinophyma • Condition worsened by acidic and spicy food, temp changes, alcohol and stress • Cause is unknown • Topical Vit C therapy can be helpful
Acne • Hormonal changes and genetics are 2 major causes • Can be caused by stress, medications, humid environment, and surface irritation • Is always caused by excessive androgen • The follicle lining sheds more rapidly and the production of sebum increases, the combination plugs the opening of the follicle and blocks oxygen from entering • Bacteria contributes to the inflammation • Retention hyperkeratosis- accumulation of cells that adhere to the follicle
Types of Acne • Open Comedone- blackhead, has been oxidized • Closed comedone- whitehead, not exposed to oxygen • Papule- does not contain pus • Pustule- contains pus • Milia- pearly white enclosed cyst, can be lanced. • Nodular Cystic Acne- hard lesions found deep in the skin. Severe form