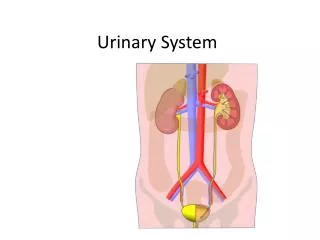
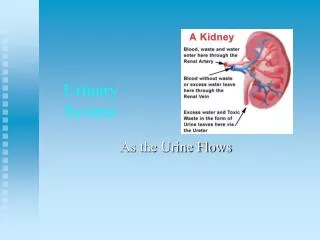
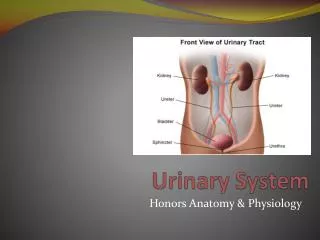
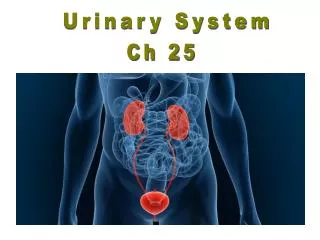
URINARY SYSTEM 2
E N D
Presentation Transcript
URINARY SYSTEM 2 PHYSIOLOGY OF THE KIDNEYS
RENAL CLEARANCE • Renal clearance – the kidney removes molecules from the blood plasma by excreting them in the urine. • Renal clearance is accomplished by • Filtration – moves most things out. • Secretion – the opposite of reabsorption; moves molecules from the blood back to the filtrate.
Secretion is the reverse of reabsorption Secretion increases renal clearance Excretion rate = (filtration rate + secretion rate) – reabsorption rate.
Removal of Xenobiotics • Xenobiotics – substances foreign to the body • Organic anion transporter (OAT) family – Na+-independent transport that secretes some endogenous compounds as well as many xenobiotics • Located in the basolateral membrane of the proximal tubule • Larger xenobiotics are removed by OATs in the liver bile • Organic Cation transporters (OCTs)- secrete particular xenobiotics, e.g. metformin (for Diabetes type II)
INULIN CAN BE USED TO MEASURE GFR • Inulinis filtered but not reabsorbed or secreted • A great marker of GFR only • Found in garlic, onion, dahlias, and artichokes.
Calculating GFR Using Inulin: If: V = rate of urine formation (ml/min) U = inulin concentration in urine (mg/ml) P = inulin concentration in plasma (mg/ml) V x U GFR = ---------- P
Example: If: V = rate of urine formation is 2 ml/min. U = inulin concentration in urine is 30 mg/ml P = inulin concentration in plasma is 0.5 mg/ml V x U 2 ml/min x 30 mg/ml GFR = ---------- = ---------------------------- =120 ml/min P 0.5 mg/ml
Renal Plasma Clearance Calculation Renal Plasma Clearance= Volume of plasma from which a substance is completely removed by the kidneys in 1 minute (ml/min) • Inulin is filtered only. Therefore, Clearance = GFR • Anything that can be reabsorbed has a clearance < GFR. • If a substance is filtered and secreted, it will have a clearance > GFR. • Renal plasma clearance uses same formula as GFR. • Clearance of ureais less than GFR – means some is reabsorbed (see next slide)
EXAMPLE: Clearance of Urea The urea concentration in urine (U) is about 7.5 mg/ml, and the amount of urea in the blood is 0.2 mg/ml (P). If the rate of urine formation is 2 ml/min, then… Urea clearance = (2ml/min)(7.5 mg/ml) = 75 ml/min 0.2 mg/ml This is LESS than 120ml/min (the clearance rate for INULIN), and therefore, some of the urea is reabsorbed.
USE OF PAH TO MEASURE TOTAL RENAL BLOOD FLOW • PAH in glomerulus, • some PAH is filtered, • all PAH in peritubular capillaries is secreted. Therefore, PAH can be used to measure total renal blood flow. Normal PAH clearance = 625 ml/min Glomerular filtration is only 120 ml/min, or only 20% of plasma is filtered/80% is secreted.
Mechanism of Reabsorption in the proximal tubule • Glucose and amino acids • not found in urine. • filtered out in the capsule • Reabsorbed in PCT STEPS: 1) 2◦active transport of glucose and Na+ into cyto 2) 1◦ active transport of Na+ by Na+/K+ pump. 3) Glucose facilitated diffusion
Glucose Carriers Can Become Saturated • Transport maximum (Tm) is when the glucose carriers are saturated. • Occurs at 375 mg/min of glucose in the filtrate • Normal glucose levels are about 125 mg/min • Glycosuria– glucose appears in the urine.
What causes GLYCOSURIA? • Glucose spills into the urine when plasma concentrations reach 180-200 mg/100 ml • This is well below the Transport Maximum (Tm). • Therefore, some nephrons may have lower Tm values than average • Renal Plasma Threshold – a more convenient term • Is the minimum plasma concentration of a substance that results in the excretion of that substance in the urine. Hyperglycemia – when glucose exceeds renal plasma threshold; (fasting hyperglycemia = diabetes mellitus)
Electrolyte Excretion The kidneys match electrolyte (Na+, K+, Cl−, bicarbonate, phosphate) excretion to ingestion. • Control of Na+ levels is important in blood pressure and blood volume. • Control of K+ levels is important in healthy skeletal and cardiac muscle activity. • Aldosterone plays a big role in Na+ and K+ balance.
Reabsorption and Secretion of Na+ and K+ • In PCT: 90% of Na+ and K+ is reabsorbed at a constant rate early in the nephron. • occurs at constant rate, not subject to hormonal regulation. In DCT and cortical region of collecting duct: Na+(into blood) and K+(out of blood) regulation occurs by aldosterone.
SODIUM REABSORPTION Without Aldosterone: • 90% is reabsorbed (aldosterone-independent) in PCT • Of the 10% remaining, 80% is reabsorbed in the DCT and 20% is excreted (about 30 g/day). • Cl- is also passively reabsorbed, following Na+ With Aldosterone: • No Na+ is excreted • Aldosterone raises blood pressure
Aldosterone raises blood pressure Aldosterone stimulates Na+/K+ Pumps
Potassium Secretion • Purpose: to maintain a set-point [K+] in the blood • A rise in blood K+ leads to the following… • Stimulates adrenal cortex to secrete aldosterone. • Aldosterone causes K+ to be secreted into the filtrate • Aldosterone-independent secretion of K+ • Synthesis of K+ channels in the apical membrane of the cortical collecting duct. • When blood K+ falls, these channels are removed.
Aldosterone raises blood pressure Aldosterone-dependent Secretion of K+
Relationship Between Na+ and K+ • Increases in Na+absorption drive extra K+secretion. • Due to: • Potential difference created by Na+reabsorption, which drives K+ secretion through K+ channels. • Stimulation of Renin-angiotensin-aldosterone system by water and Na+ in filtrate. • Increased flow rates in tubule bend cilia on the cells of the distal tubule, resulting in activation of K+channels.
Student Activity Diuretics (drugs that increase urine volume) inhibit Na+ transport in the nephron loop and increase delivery of Na+ to the collecting duct, and increased Na+ reabsorption in the collecting duct. Why would a person who is taking diuretics might have to take K+ supplements?
Student Activity ANSWER Diuretics (drugs that increase urine volume) inhibit Na+ transport in the nephron loop and increase delivery of Na+ to the collecting duct. Why would a person who is taking diuretics might have to take K+ supplements? ANSWER: Increased delivery of Na+ to the collecting duct increases secretion of K+ and excretion of K+ into the urine.
Control of Aldosterone Secretion • A rise in blood K+directly stimulates (depolarizes) the adrenal cortex produce aldosterone. • A fall in blood Na+indirectly stimulates production of aldosterone via the renin- angiotensin-aldosterone system. aldosterone
Location of Juxtaglomerular Apparatus Located where the afferent arteriole comes into contact with the distal tubule.
SECRETION OF RENIN When there is a fall in blood volume, due to a fall in plasma Na+, Renin is secreted by the granular cells. RENIN is an enzyme.
Renin converts angiotensinogen to angiotensin I Angiotensin I is converted to angiotensin II by ACE ACE = angiotensin converting enzyme Angiotensin II stimulates the adrenal cortex to secrete aldosterone. Aldosterone raises blood pressure by causing Na+ reabsorption in the DCT and cortical collecting duct, and increases secretion of K+Angiotensin II also stimulates vasoconstriction of afferent and efferent arterioles, lowering Na+ excretion.
Regulation of Renin Secretion • Low salt leads to lower blood volume • Reduced blood volume is detected by granular cells that act as baroreceptors. • They then secrete renin. 2) Granular cells are also stimulated by sympathetic innervation from the baroreceptor reflex POINT – If b.p. is low renin is secreted Na+ reabsorption b.p. goes up
Macula Densa Sensor for tubuloglomerular feedback needed for regulation of GFR: • High Na+ and H2O in the filtrate, cause macula densa to release ATP, which constricts the afferent arteriole. 2) constriction lowers GFR, which lowers Na+ and H2O (negative feedback) b. ALSO – High Na+ and H2O in the filtrate causes the granular cells to lower their production of renin. • This results in less reabsorption of Na+, allowing more to be excreted. • This helps lower Na+ levels in the blood.
ANP DECREASES BLOOD PRESSURE • Increases in blood volume also increase the release of ANP hormone from atria of the heart when atrial walls are stretched. • Stimulates kidneys to excrete more salt and therefore more water • Decreases blood volume and blood pressure ANP IS OPPOSITE TO RENIN
Reabsorption of Na+ stimulates the secretion ofother positive ions, such as K+ and H+ • Acidosisstimulates the secretion of H+and inhibits the secretion of K+ ions; acidosis can lead to hyperkalemia. • Alkalosis stimulates the secretion and excretion of more K+. Increases reabsorption of H+ • Hyperkalemia stimulates the secretion of K+ and inhibits secretion of H+; can lead to acidosis
ACID BASE REGULATION • Proximal tubule uses Na+/H+ pumps to exchange Na+ out and H+ in. • Some of the H+ brought in is used for the reabsorption of bicarbonate. • Antiport secondary active transport
ACID BASE REGULATION • Kidneys maintain blood pH by reabsorbing bicarbonate and secreting H+; urine is thus acidic.
ACID BASE REGULATION Bicarbonate cannot cross the inner tubule membrane so must be converted to CO2 and H2O using carbonic anhydrase. • Bicarbonate + H+ carbonic acid • Carbonic acid (w/ carbonic anhydrase) H2O + CO2 • CO2 can cross into tubule cells, where the reaction reverses and bicarbonate is made again. • This diffuses into the interstitial space.
ACID BASE REGULATION Aside from the Na+/H+ pumps in the proximal tubule, the distal tubule has H+ ATPase pumps to increase H+ secretion.
pH Disturbances • Kidneys can help compensate for respiratory problems b. Alkalosis: Less H+ is available to transport bicarbonate into tubule cells, so less bicarbonate is reabsorbed; extra bicarbonate secretion compensates for alkalosis. • Acidosis: Proximal tubule can make extra bicarbonate through the metabolism of the amino acid glutamine. • Extra bicarbonate enters the blood to compensate for acidosis. • Ammonia stays in urine to buffer H+.
Urinary Buffers • Nephrons cannot produce urine with a pH below 4.5. • To increase H+ secretion, urine must be buffered. • Phosphates and ammonia buffer the urine. • Phosphates enter via filtration. • Ammonia comes from the deamination of amino acids.
Use of Diuretics • Used clinically to control blood pressure and relieve edema (fluid accumulation) • Diuretics increase urine volume, decreasing blood volume and interstitial fluid volume. • Many types act on different portions of the nephron.
Types of Diuretics Loop diuretics: most powerful; inhibit salt transport out of ascending loop of Henle • Example: Lasix • Can inhibit up to 25% of water reabsorption
Types of Diuretics b. Thiazide diuretics: inhibit salt transport in distal tubule • Can inhibit up to 8% of water reabsorption
Types of Diuretics • Carbonic anhydrase inhibitors: much weaker; inhibit water reabsorption when bicarbonate is reabsorbed • Also promote excretion of bicarbonate
Types of Diuretics d. Potassium-sparing diuretics: Aldosterone antagonists block reabsorption of Na+ and secretion of K+.
Types of Diuretics, cont. e. Osmotic diuretics: reduce reabsorption of water by adding extra solutes to the filtrate • Example: Mannitol • Can occur as a side effect of diabetes
Renal Function Tests • PAH and inulin clearance • Can diagnose nephritis or renal insufficiency • Urinary albumin excretion rate: detects above-normal albumin excretion • Called microalbuminuria • Signifies renal damage due to hypertension or diabetes • Proteinuria: overexcretion of proteins; signifies nephrotic syndrome