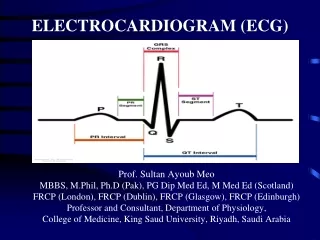
A 12-lead electrocardiogram
A 12-lead electrocardiogram. By Dr Abdul- Monim Batiha Dr Ibrahim Bashayreh. A 12-lead electrocardiogram (ECG). ECG is a graphic record of electric currents that are generated by the heart muscles.

A 12-lead electrocardiogram
E N D
Presentation Transcript
A 12-lead electrocardiogram By Dr Abdul-MonimBatiha Dr Ibrahim Bashayreh
A 12-lead electrocardiogram (ECG) ECG is a graphic record of electric currents that are generated by the heart muscles. Electrical impulses are picked up by the surface electrode which are placed at various points on the body and connect the ECG machine to the body.
Objectives • To diagnose the presence of MI. • To diagnose the presence of cardiac dysrrhythmias. • To diagnose the presence of cardiac enlargement and size of cardiac champers. • To detect the electrolyte abnormalities especially K and Ca.
To evaluate the effect of therapeutic interventions on the heart ( e.g. drugs, fluid, and mechanical support)
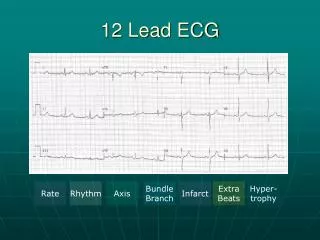
The 12-lead ECG provides “views” of cardiac electrical activity from 12 different vantage points on the body surface.
ASSESSMENT 1. Assess age, gender, and current medication history for any medications with possible cardiac or hemodynamic effects. Gather other data that may be required by unit/institution protocol (height, weight, recent blood pressure, operator identification).
A 15-lead ECG adds 3 additional chest leads across the right precordium and is a valuable tool for the early diagnosis of right ventricular and posterior left ventricular infarction. The 18-lead ECG adds 3 posterior leads to the 15-lead ECG and is very useful for early detection of myocardial ischemia and injury
Determine that the client is able to tolerate a supine position and that adequate exposure of chest and limbs is possible for electrode placement. Correct sitting of electrodes is enhanced by comfortable, stable position.
Determine presence of neck, arm, jaw, or other pain with possible cardiac origin. Chest or other pain may provide additional information useful in serial comparison of ECGs.
Assess client need for information about the procedure purpose and requirements and ability to cooperate: that client should lie still and refrain from talking, electrode attachment, procedure lasts only a few minutes and is painless. Anxiety may be relieved by simple explanation of intent, duration, and purpose.
Equipment Needed • Twelve-lead ECG machine with charged battery, cables and leads, graph paper • Disposable electrodes (12) • Electrode paste or gel • Alcohol wipes • Pillows • Sheet or drape • Towel and washcloth • Disposable razor
Each of the 12 leads represents a particular orientation in space, as indicated below (RA = right arm; LA = left arm, LF = left foot): • Bipolar limb leads (frontal plane): Lead I: RA (-) to LA (+) (Right Left, or lateral) Lead II: RA (-) to LF (+) (Superior Inferior) Lead III: LA (-) to LF (+) (Superior Inferior)
Continuous Electrocardiographic Monitoring • Continuous ECG monitoring is standard for patients who are at high risk for dysrhythmias.
Two continuous ECG monitoring techniques • hardwire monitoring, found in critical care units and specialty step-down units, and • telemetry, found in specialty step-down units and general nursing care units.
Patients who arereceiving continuous ECG monitoring need to be informed of its purpose and cautioned that this monitoring method will not detect symptoms such as dyspnea or chest pain. Therefore, patients need to be advised to report symptoms to the nurse whenever they occur.
HARDWIRE CARDIAC MONITORING • The patient’s ECG can be continuously observed for dysrhythmias and conduction disorders on an oscilloscope at the bedside or at a central monitoring station by a hardwire monitoring system.
Objectives of cardiac monitor • Monitor more than one lead simultaneously • Monitor ST segments (ST-segment depression is a marker of myocardial ischemia; ST-segment elevation provides evidence of an evolving MI)
• Provide graded visual and audible alarms (based on priority, asystole would be highest) • • Computerize rhythm monitoring (dysrhythmias are interpreted and stored in memory) • • Print a rhythm strip • • Record a 12-lead ECG
Two leadscommonly used for continuous monitoring are leads II and V1 or a modification of V1 Lead II provides the best visualization of atrial depolarization (represented by the P wave). Leads V1 and II best visualize the ventricle responsible for ectopic or abnormal ventricular beats.
Following the guidelines for electrode placement will ensure good conduction and a clear picture of the patient’s rhythm on the monitor: •
Cleanthe skin surface with soap and water and dry well (or as recommended by the manufacturer) before applying the electrodes. If the patient has much hair where the electrodes need to be placed, shave or clip the hair.
Apply a small amount of benzoin to the skin if the patient is diaphoretic (sweaty) and the electrodes do not adhere well.
PULSE OXIMETRY • Is a noninvasive method of continuously monitoring the oxygen saturation of hemoglobin (SpO2 or SaO2). Although pulse oximetry does not replace arterial blood gas measurement, it is an effective tool to monitor for subtle or sudden changes in oxygen saturation.
It is used in all settings where oxygen saturation monitoring is needed, such as the home, clinics, ambulatory surgical settings, and hospitals.
It is used in all settings where oxygen saturation monitoring is needed, such as the home, clinics, ambulatory surgical settings, and hospitals.
A probe or sensor is attached to the fingertip, forehead, earlobe, or bridge of the nose. The sensor detects changes in oxygen saturation levels by monitoring light signals generated by the oximeter and reflected by blood pulsing through the tissue at the probe.
naloxone :a drug resembling morphine, used in the diagnosis of narcotics addiction and to reverse the effects of narcotics poisoning
Physiologic Limitations. • Elevated levels of abnormal hemoglobins, • Presence of vascular dyes, • Poor tissue perfusion. The pulse oximeter cannot differentiate between normal and abnormal hemoglobin.
Elevated levels of abnormal hemoglobin falsely elevate the Spo2. • Vascular dyes such as methylene blue, indigo also interfere with pulse oximetry and can lead to falsely low readings. • Poor tissue perfusion to the area with the probe leads to loss of pulsatile flow and signal failure.
Technical Limitations. • Technical limitations include • Bright lights, • Excessive motion, • Incorrect placement of the probe. Bright lights may interfere with the photodetector and cause inaccurate results. The probe must be covered to limit optical interference.
Excessive motion can mimic arterial pulsations and can lead to false readings. Incorrect placement of the probe can lead to inaccurate results, because part of the light can reach the photodetector without having passed through blood (optical shunting).
Interventions to limit these problems include • Using the proper probe in the appropriate spot (e.g., not using a finger probe on the ear), • Applying the probe according to the directions, and ensuring that the area being monitored has adequate perfusion.
Equipment • Pulse oximeter • Sensor (permanent or disposable) • Alcohol wipe(s) • Nail polish remover, if indicated