Bone Tissue
Bone Tissue. Ch. 6. Objectives: Identify main functions of osseous tissue Identify the major parts of a long Describe the cells found in osseous tissue Describe the components of an osteon Compare and contrast intramembranous and endochondral ossification.


Bone Tissue
E N D
Presentation Transcript
Bone Tissue Ch. 6
Objectives: • Identify main functions of osseous tissue • Identify the major parts of a long • Describe the cells found in osseous tissue • Describe the components of an osteon • Compare and contrast intramembranous and endochondral ossification.
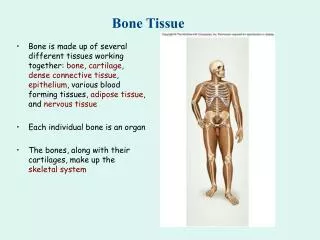
Osteology: study of osseous structures. Support Protection Movement Mineral homeostasis Hemopoiesis: blood cell formation Storage of adipose tissue: yellow marrow
Long bone anatomy • Diaphysis: long shaft of bone • Epiphysis: ends of bone • Epiphyseal plate: growth plate • Metaphysis: b/w epiphysis and diaphysis • Articular cartilage: covers epiphysis • Periosteum: bone covering (pain sensitive) • Sharpey’s fibers: periosteum attaches to underlying bone • Medullary cavity: Hollow chamber in bone - red marrow produces blood cells - yellow marrow is adipose. • Endosteum: thin layer lining the medullary cavity
Histology of bone tissue Cells are surrounded by matrix. - 25% water - 25% protein - 50% mineral salts 4 cell types make up osseous tissue Osteoprogenitor cells Osteoblasts Osteocytes Osteoclasts
Osteoprogenitor cells: - derived from mesenchyme - all connective tissue is derived - unspecialized stem cells - undergo mitosis and develop into osteoblasts - found on inner surface of periosteum and endosteum.
Osteoblasts: - bone forming cells - found on surface of bone - no ability to mitotically divide - collagen secretors • Osteocytes: - mature bone cells - derived form osteoblasts - do not secrete matrix material - cellular duties include exchange of nutrients and waste with blood.
Osteoclasts - bone resorbing cells - bone surface - growth, maintenance and bone repair Abundant inorganic mineral salts: - Tricalcium phosphate in crystalline form called hydroxyapatite Ca3(PO4)2(OH)2 • Calcium Carbonate: CaCO3 • Magnesium Hydroxide: Mg(OH)2 • Fluoride and Sulfate
These salts are deposited on the collagen fiber framework (tensile strength) and crystallization occurs. - calcification or mineralization
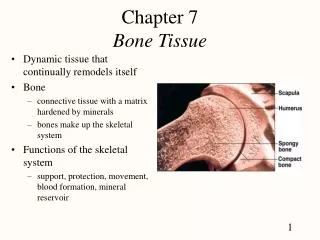
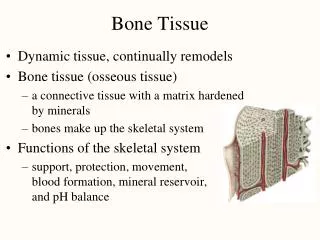
Compact bone: (Osteon) external layer - called lamellar bone (groups of elongated tubules called lamella) - majority of all long bones - protection and strength (wt. bearing) - concentric ring structure - blood vessels and nerves penetrate periosteum through horizontal openings called perforating (Volkmann’s) canals.
- central (Haversian) canals run longitudinally. Blood vessels and nerves. - around canals are concentric lamella - osteocytes occupy lacunae (“little lakes”) which are between the lamella - radiating from the lacunea are channels called canaliculi. (finger like processes of osteocytes)
Lacunae are connected to one another by canaliculi. • Osteon contains: - central canal - surrounding lamellae - lacunae - osteocytes - canaliculi
Spongy bone (cancellous bone): internal layer - latticework of bone tissue (haphazard arrangement). - made of trabeculae (“little beams”) - filled with red and yellow bone marrow - osteocytes get nutrients directly from circulating blood. - short, flat and irregular bone is made up of mostly spongy bone
Bone formation (ossification) occurs in two ways 1- Intramembranous ossification 2- Endochondral ossification Both methods above lead to the same bone formation but are different methods of getting there. Ossification (osteogenesis) begins around the 6th -7th week of embryonic life. At this time the embryonic skeleton is made of fibrous membranes and hyaline cartilage.
Hyaline Cartilage Review a. Most abundant b. Provides support, flexibility and resilience c. Located: a. forming nearly all the fetal skeleton b. articular cartilage: ends of moving bones c. costal cartilage: ribs to sternum d. tip of nose e. respiratory cartilage
Skeletal Cartilage: 1. Chondrocytes: cartilage producing cells. 2. Lacunae: small cavities where the chondrocytes are encased. 3. Extracellular matrix: jellylike ground substance. 4. Perichondrium: layer of dense irregular connective tissue that surrounds the cartilage. 5. No blood vessels or nerves
Intramembranous (within the membrane) ossification: Bone develops from a fibrous membrane. - flat bones of skull - mandible - clavicles -mesenchymal cells become vascularized and become osteoprogenitor cells and then osteoblasts. - organic matrix of bone is secreted - osteocytes are formed - calcium and mineral salts are deposited and bone tissue hardens. - trabeculae develop and spongy bone is formed - red marrow fills spaces
Replacement of hyaline cartilage with bone is called .Endochondral (intracartilaginous) ossification Most bones are formed this way (i.e. long bones). Where bone is going to form: 1- mesenchymal cells differentiate into chondroblasts (immature cartilage cells) which produces hyaline cartilage. Perichondrium develop around new cartilage 2- Chondrocytes (mature) mitotically divide increasing in length This pattern of growth: interstitial growth. - growth from within
Growth of cartilage in thickness occurs from the deposition of new matrix to the periphery formed by chondroblasts within the perichondrium. Appositional growth. Chondrocytes undergo hypertrophy, swell and burst. pH of the matrix changes and calcification is triggered. Ultimately, cartilage cells die. Lacunae are now empty.
Nutrients are supplied by way of the nutrient artery passing through the perichondrium through the nutrient foramen. Osteoprogenitor cells are stimulated in the perichondrium to produce osteoblasts. A thin layer of compact bone is laid down under the perichondrium called the periosteal bone collar. Perichondrium becomes periosteum
Osteoblasts begin to deposit bone matrix forming spongy bone trabeculae. In the middle of the bone, osteoclasts break down spongy bone trabeculae and form a hollowed out cavity called the medullary cavity. This cavity will be filled with red bone marrow for hemopoiesis. The shaft of the bone is replaced (was hyaline cartilage) with compact bone.
Physiology of bone growth: - epiphyseal plate (bone length) - 4 zones of bone growth under hGH. 1- Zone of resting cartilage: - no bone growth - located near the epiphyseal plate - scattered chondrocytes - anchors plate to bone 2- Zone of proliferating cartilage - chondrocytes stacked like coins - chondrocytes divide
3- Zone of hypertrophic (maturing) cartilage - large chondrocytes arranged in columns - lengthwise expansion of epiphyseal plate 4- Zone of calcified cartilage - few cell layers thick - occupied by osteoblasts and osteoclasts and capillaries from the diaphysis - cells lay down bone - dead chondrocytes surrounded by a calcified matrix. Matrix resembles long spicules of calcified cartilage. Spicules are partly eroded by osteoclasts and then covered in bone matrix from osteoblasts: spongy bone is formed.
Age 18-21: Longitudinal bone growth ends when epiphysis fuses with the diaphysis. - epiphyseal plate closure - epiphyseal line is remnant of this - last bone to stop growing: clavicle
Bone width: increase in diameter of bone occurs through appositional growth . - Osteoblasts located beneath the periosteum secrete bone matrix and build bone on the surface - Osteoclasts located in the endosteum resorbs (breakdown) bone.
Bone Remodeling: - bone continually renews itself - never metabolically at rest - enables Ca to be pulled from bone when blood levels are low - osteoclasts are responsible for matrix destruction - produce lysosomal enzymes and acids - spongy bone replaced every 3-4 years - compact bone every 10 years