Gastrointestinal Bleeding
Gastrointestinal Bleeding. Rajeev Jain, M.D. GI Bleeding. Background Acute Upper GI Bleed Acute Lower GI Bleed . Clinical Presentation Definitions. Hematemesis: bloody vomitus (bright red or coffee-grounds) Melena: black, tarry, foul-smelling stool

Gastrointestinal Bleeding
E N D
Presentation Transcript
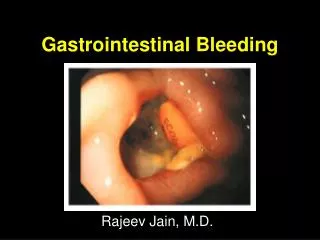
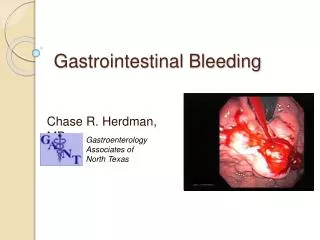
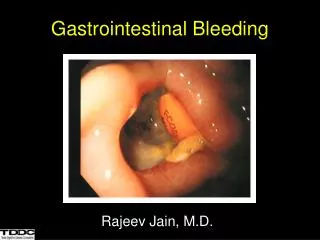
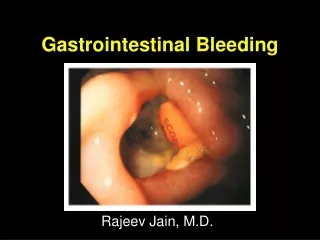
Gastrointestinal Bleeding Rajeev Jain, M.D.
GI Bleeding • Background • Acute Upper GI Bleed • Acute Lower GI Bleed
Clinical PresentationDefinitions Hematemesis: bloody vomitus (bright red or coffee-grounds) Melena: black, tarry, foul-smelling stool Hematochezia: bright red or maroon blood per rectum Occult: positive guaiac test Symptoms of anemia: angina, dyspnea, or lightheadedness
Clinical Presentation • Reflection of bleeding: • Site • Etiology • Rate
Resuscitation • 2 large bore peripheral IV’s • Colloid (normal saline or lactated Ringer’s) • Transfuse packed RBCs • In elderly, goal Hct 30% • In young, goal Hct 20-25% • In cirrhotics, goal Hct 25-28% • Correct coagulopathy • Reassess hemodynamics
History • Prior history of bleeding • Previous gastrointestinal illnesses • Previous surgery • Other medical conditions (ie, cirrhosis) • Medications • Aspirin, NSAIDs, & anti-platelet agents • Anticoagulants • ? SSRIs • Abdominal pain, weight loss
Physical Exam & Labs • Focused but thorough • Look for markers of liver disease • Laboratory studies • CBC • INR • Electrolytes • Type and crossmatch RBCs
Acute BleedingChanges Before and After 2 Liter Bleed 45% 45% 27%
Location of Bleeding • Upper • Proximal to Ligament of Treitz • Melena (100-200 cc of blood) • Azotemia • Nasogastric aspirate • Lower • Distal to Ligament of Treitz • Hematochezia
Acute UGIBDemographics • Annual incidence of hospitalization: 100/100,000 persons • 80% self-limited • Mortality stable at 10% • Continued or recurrent bleeding - mortality 30-40%
Acute UGIBPrognostic Indicators • Cause of bleeding • Severity of initial bleed • Age of the patient • Comorbid conditions • Onset of bleeding during hospitalization
Acute UGIBPrognostic Indicators Tedesco et al. ASGE Bleeding Survey. Gastro Endo. 1981.
Peptic ulcer disease Gastric ulcer Duodenal ulcer Mallory-Weiss tear Portal hypertension Esophagogastric varices Gastropathy Esophagitis Dieulafoy’s lesion Vascular anomalies Hemobilia Hemorrhagic gastropathy Aortoenteric fistula Neoplasms Gastric cancer Kaposi’s sarcoma Acute UGIBDifferential Diagnosis
Acute UGIBFinal Diagnoses of the Cause in 2225 Patients Tedesco et al. ASGE Bleeding Survey. Gastro Endo. 1981.
Acute UGIBCauses in CURE Hemostasis Studies (n=948) Savides et al. Endoscopy 1996;28:244-8.
Acute UGIBCORI Database: 7822 EGDs b/n 1999-2001 Boonpongmanee S. et al. Gastrointest Endosc 2004;59:788-94.
Acute Peptic Ulcer BleedingPrognosis by SRH Laine and Peterson. New Eng J Med 1994;331:717-27.
Thermal Bipolar probe Monopolar probe Argon plasma coagulator Heater probe Mechanical Hemoclips Band ligation Injection Epinephrine Alcohol Ethanolamine Polidocal Endoscopic Therapy of PUD
Endoscopic Therapy of PUD Laine and Peterson New Eng J Med 1994;331:717-27.
Peptic Ulcer BleedingAdjuvant Medical Therapy • Erythromycin • 250 mg IV 30 minutes before endoscopy decreases blood in stomach • Proton pump inhibitor therapy • 80 mg IV bolus followed by 8 mg/hr continuous infusion for 72 hrs • Reduced risk: • Rebleeding (NNT 12) • Surgery (NNT 20) Leontiadis, G. et al. BMJ 2005;330:568
MEDICAL THERAPYAcute Variceal Bleeding • Octreotide • Cyclic octapeptide analog of somatostatin • Longer acting than somatostatin • Equivalent to sclerotherapy and improves endoscopic results
Transjugular Intrahepatic Portosystemic Shunt (TIPS) Coronary Vein IVC Splenic Vein Portal Vein
Aortoduodenal Fistula Aorta Duodenum Fistula Graft
Acute UGIBSurgery • Recurrent bleeding despite endoscopic therapy • > 6-8 units pRBCs
Diverticulosis Colitis IBD (UC>>CD) Ischemia Infection Vascular anomalies Neoplasia Anorectal Hemorrhoids Fissure Dieulafoy’s lesion Varices Small bowel Rectal Aortoenteric fistula Kaposi’s sarcoma UPPER GI BLEED Acute LGIBDifferential Diagnosis
Acute LGIBDiagnoses in pts with hemodynamic compromise. Zuccaro. ASGE Clinical Update. 1999.
Etiology of Acute LGIB Strate LL. Gastroenterol Clin North Am. 2005 Dec;34(4):643-64.
Outcomes of Acute LGIB Strate LL. Gastroenterol Clin North Am. 2005 Dec;34(4):643-64.
Urgent Colonoscopy for the Diagnosis and Treatment of Severe Diverticular Hemorrhage • 121 pts with severe bleeding (>4 hrs after hospitalization) • 1st 73 pts: no colonoscopic tx • Last 48 pts eligible for colonoscopic tx • Colonoscopy w/in 6-12 hrs
Urgent Colonoscopy for the Diagnosis and Treatment of Severe Diverticular Hemorrhage Jensen DM, et al. New Eng J Med 2000:342:78-82.
Ischemic Colitis • Most common form of intestinal ischemia • Transient and reversible • Abdominal pain • Watershed areas • Splenic flexure • Rectosigmoid junction
Acute LGIBMeckel’s Diverticulum • Incidence 0.3 - 3.0 % • Etiology Incomplete obliteration of the vitelline duct. • Pathology 50% ileal, 50% gastric, pancreatic, colonic mucosa • Complications • Painless bleeding (children, currant jelly) • Intussusception
Acute LGIBEvaluation Zuccaro. ASGE Clinical Update. 1999.
Acute LGIBKey Points • Annual incidence of hospitalization: • 20-30/100,000 persons • Resuscitation • Exclude an UGI source • Most bleeding ceases • Colonoscopy • No role for barium studies