Adrenaline (Epinephrine)
Adrenaline (Epinephrine). It is the major constituent of the adrenal medulla secretion (80%). Hydrochloride aqueous solutions are hydrolyzed rapidly in alkaline or neutral media but are stable at low pH and in the presence of reducing agents (ascorbic acid). Absorption and Fate:

Adrenaline (Epinephrine)
E N D
Presentation Transcript
It is the major constituent of the adrenal medulla secretion (80%). • Hydrochloride aqueous solutions are hydrolyzed rapidly in alkaline or neutral media but are stable at low pH and in the presence of reducing agents (ascorbic acid).
Absorption and Fate: • It is not effective orally because: • Poor absorption from the GIT • Rapid destruction by digestives juices • Rapid metabolism by the liver
Absorption and Fate: • It is absorbed slowly from s.c. tissues due to local vasoconstriction (α-effect). • It is more rapidly absorbed from i.m. sites (β2-mediated vasodilatation). • Inhaled solutions have a restricted action to the respiratory tract. • Intracardiac: emergency. • Infusion: adrenaline and noradrenaline.
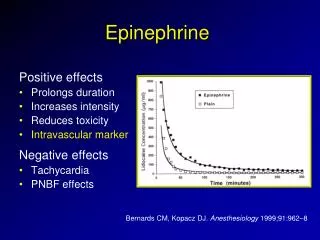
Pharmacological actions: • Local actions: • On mucous membranes or abraded surfaces vasoconstriction • Added to local anesthetics to prolong their durationof action. • A haemostatic action when applied to bleeding surface. • A delay in the absorption of associated drugs when injected subcutaneously
Local application of adrenaline to the eye: • It has a limited effect on the size of the pupil because: • It is partly destroyed by the alkalinity of tears. • It causes v.c. of the conjunctival blood vessels hinders its own absorption. • In patients with open angle glaucoma, it helps to the formation of the A.H. & its drainage the IOP.
Adrenaline causes mydriasis in the following conditions: • Acute hemorrhagic pancreatitis. • Postganglionic sympathetic denervation of the dilator pupillae muscle. • Some cases of glaucoma. • Hyperthyroidism. • Diabetic coma.
Systemic actions: • Cardiovascular system: • Heart (β1 receptors) • Heart rate (+vechronotropic action, tachycardia). • Force of contraction (+veinotropic action). • Cardiac output. • Heart work and O2 consumption.
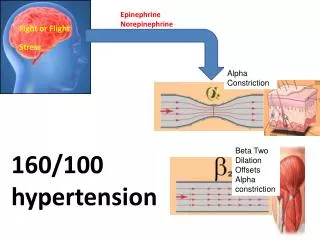
Blood vessels (α and β2) • α-Stimulation v.c. of the blood vessels of the skin, mucous membrane and kidney. • β2-Stimulation v.d. of the skeletal muscle and coronary blood vessels.
Blood pressure (B.P.): • SBP (due to COP) while DBP changes up or down depending on the final effect on the PVR. • Therapeutic doses PVR due to the dominant action on β2 receptors DBP. • Experimentally, epinephrine (low dose) B.P. because of its β effects. Gradual epinephrine doses B.P. (marked α effects) and ergotamine (α-adrenergic blocker) administration B.P. (epinephrine reversal) as epinephrine would act only on β-receptors.
The pressor effect of phenylephrine (a selective α1-stimulant) is abolished by ergotamine. • The pressor effect of NE is partially blocked by ergotamine [the pressor effect of NE is partly due to its v.c. (α1-receptors) and partly due to a cardiac stimulant action (β1-receptor) that remains in effect after α-receptors blockade].
Effect on Eye: • Active mydriasis (α1-receptors )!!! • No loss of light reflex & accommodation.
Effect on bronchi: • It stimulates β2-receptors in the bronchioles bronchodilatation. • Adrenaline acts also on α-receptors of blood vessels v.c. bronchial mucosal congestion.
Gastrointestinal tract: • The GIT contains both αand βreceptors. • Stimulation of either types of receptors leads to inhibition of tone and motility.
Urinary bladder • Adrenaline relaxes the detrusor muscle (β2-receptors) and contracts the sphincter (α1-receptors) urine retention.
Uterus: • Adrenaline relaxes the pregnant human uterus (β2).
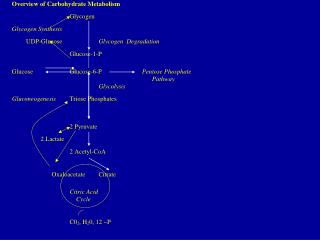
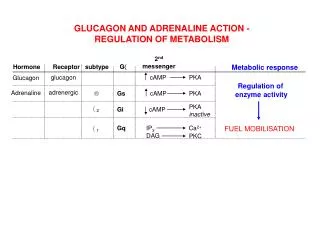
Metabolic Actions: • Blood glucose through: • Enhancement of hepatic glycogenolysis (β2). • Glucose uptake by peripheral tissues. • Blood lactate ( breakdown of glycogen to lactate in skeletal muscles).
Metabolic Actions: • Blood concentration free fatty acids (due to lipolysisβ1 & β3). • ( Breakdown of TGs in adipose tissues) • O2 consumption (20-30%) due to metabolism. • A transient in plasma K+ level followed by a prolonged fall.
Action on the CNS: • Adrenaline has a weak stimulant effect restlessness, headache & tremors.
Skeletal muscle action: • It facilitates neuromuscular transmission by sensitization of the motor endplate and hastens recovery from fatigue by increasing blood flow to the muscles.
Antihistamine and antiallergic action. • Adrenaline is the physiological antagonist of histamine.
Therapeutic Uses: • Acute bronchial asthma bronchodilatation & bronchial mucosal congestion and edema. • Allergy, urticaria, edema and anaphylactic shock. • Insulin hypoglycemia. • Cardiac resuscitation (intracardiac injection of adrenaline in cardiac arrest).
Adrenaline is given with local anesthetics (s.c.) v.c. • Prolong their durations of action. • Bleeding from the operation sites. • Local hemostatic(stop hemorrhage from the nasal mucosa, epistaxis). • As eye drops in some cases of glaucoma.
Contraindications: • Coronary heart diseases ( anginal attacks) • Hypertension ( cerebral hemorrhage). • Cardiac arrhythmias. • During anesthesia with halogenated inhalational anesthesia. • In patients receiving digitalis • Hyperthyroidism. • With local anesthetics in fingers and toes.