Skeletal System
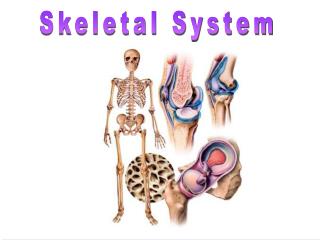
Skeletal System. Skeletal System. ADVANTAGES OF ENDO SKELETON Allows for continual growth. Provides site of attachment for muscles. Skeletal Organization. Axial Skeleton head, neck, trunk skull, vertebral column, rib cage body’s central framework Supports central axis of body

Skeletal System
E N D
Presentation Transcript
Skeletal System ADVANTAGES OF ENDOSKELETON • Allows for continual growth. • Provides site of attachment for muscles.
Skeletal Organization • Axial Skeleton • head, neck, trunk • skull, vertebral column, rib cage • body’s central framework • Supports central axis of body • Protects organs • Appendicular Skeleton • upper limbs • lower limbs • pectoral girdle • pelvic girdle
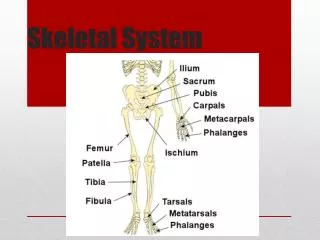
Skull Axial Skeleton Appendicular Skeleton Clavicle Sternum Scapula Humerus Ribs Radius Vertebral column Pelvis Ulna Carpals Metacarpals Phalanges Femur Patella Fibula Tibia Tarsals Metatarsals Phalanges The Skeletal System Skeleton
Bone Function • Support, Movement & Protection • gives shape to head, etc. • supports body’s weight • protects lungs, etc. • bones and muscles interact • when limbs or body parts move • Inorganic Salt Storage • calcium • phosphate • magnesium • sodium • potassium • Blood Cell Formation • hematopoiesis • red marrow
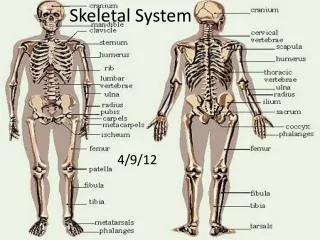
Cranium Cervical Vertebrae (Atlas) Clavicle (ventral) Scapula (dorsal) Sternum True ribs (7 pairs) Humerus False ribs (3 pairs) Radius (thumb side) Ulna (little finger side) Ilium Pubis (ventral) Ischium (dorsal) Carpals (wrist) Metacarpals (palm) Phalanges Femur Patella Tibia (shin) Fibula Tarsals (ankle) Metatarsals (instep) Phalanges Cervical vertebrae (7) Thoracic vertebrae (12) Lumbar vertebrae (5) Sacral vertebrae (5) Coccygeal vertebrae (4) Ligament – connects bones Tendon – connects muscle to bone True ribs – (7prs) attach to vertebrae and sternum False ribs – (3prs) attach to vertebrae and true ribs Floating ribs – (2prs) attach to vertebrae 120 of the 206 bones are in the hands and feet!! CRANIUM Suture (immovable joint – cartilage) Parietal bone 9. maxilla Frontal bone 10. mandible Temporal bone Occipital bone Sphenoid bone Nasal bone Zygomatic bone Bones – ORGANS206 in Skeletal SystemNote Correct Spelling!
Skeletal System Bone Classification • Long Bones • Short Bones • Flat Bones • Irregular Bones • Sesamoid (Round) • Bones
Classification of BonesClassified in THREE ways • SHAPE: bones are either long (eg. Extremities), short (wrist, ankle, & sesamoid), or flat (cranium, scapula, & ribs). Some are irregular (eg. Vertebrae). • EMBRYONIC ORIGIN: bones are either membranous (develop from connective tissue membrane) or cartilaginous (develop from cartilage). In later life, sesamoid bones may develop in tendons or in joint capsules. • STRUCTURE: bone tissue is either compact (hard, dense outside layer of all bones – strongest, giving most support) or spongy (aka cancellous – containing many cavities which are filled w/ marrow and are generally enclosed by compact bone).
Spongy bone Haversian canal Compact bone Compact bone Periosteum Bone marrow Spongy bone Osteocyte Artery Periosteum Vein Figure 36-3 The Structure of Bone Bone Structure – Haversian System Section 36-1
Parts of a Long Bone • epiphysis • distal • proximal • diaphysis • compact bone • spongy bone • articular cartilage • periosteum • endosteum • medullary cavity • marrow • red – blood cells • yellow - fat
OSTEON/HAVERSIAN SYSTEM(concentric circles) – living cells producing a rigid inorganic matrix. How do the osteocytes get food & water (surrounded by bone!)?
LONG BONE CONTINUED PERIOSTEUM: MEMBRANE COVERING BONES. • PROTECTS BONES • CONTAINS BLOOD VESSELS & NERVES • HELPS CONNECT MUSCLES TO BONES
CELL OF THE SKELETAL SYSTEM - OSTEOCYTE • OSTEOCYTES ARE EMBEDDED IN A BONE MATRIX (OSTEON). • THEY ARE FOUND IN THE LACUNA, LINING THE HAVERSIAN CANALS, & ON THE SURFACES OF COMPACT AND SPONGY BONE. • OSTEOBLASTS BUILD BONE; OSTEOCLASTS BREAK BONE DOWN AND REABSORB IT
Microscopic Structureof Compact Bone • osteon • central canal (Haversian canal) • perforating canal • osteocyte • lacuna: cavity where osteocytes found. • lamella: ring of bone matrix • canaliculus: canals connecting osteocytes (blood & nerve supply)
Bone Development • Intramembranous Ossification • bones originate within sheetlike layers of connective tissues • broad, flat bones • skull bones (except mandible) • intramembranous bones • Endochondral Ossification • bones begin as hyaline cartilage • form models for future bones • Cartilage does not BECOME bone – is destroyed and replaced by bone. (fetal skeleton is initially cartilage) • most bones of the skeleton • endochondral bones
Endochondral Ossification • hyaline cartilage model • primary ossification center • secondary ossification centers • epiphyseal plate • epiphyseal line • osteoblasts vs. osteoclasts
Factors Affecting Bone Development, Growth, and Repair • Deficiency of Vitamin A – retards bone development • Deficiency of Vitamin C – results in fragile bones • Deficiency of Vitamin D – rickets, osteomalacia • Insufficient Growth Hormone – dwarfism • Excessive Growth Hormone – gigantism, acromegaly • Insufficient Thyroid Hormone – delays bone growth • Sex Hormones – promote bone formation; stimulate ossification of epiphyseal plates • Physical Stress – stimulates bone growth • Osteoporosis: loss of bone density that may occur in later years of life. More in women-smaller bones, sex hormones decrease in menopause, lose Ca w/ child bearing. • Prevention of bone loss?? Balanced diet, exercise, & calcium
3 FUNCTIONS MOVEMENT MAINTAINS POSTURE GENERATES HEAT 2 CLASSIFICATIONS VOLUNTARY---UNDER CONSCIOUS CONTROL---CEREBRUM--- SKELETAL INVOLUNTARY---NO CONSCIOUS CONTROL---MEDULLA---CARDIAC & SMOOTH 2 CELL TYPES STRIATED---CROSS- STRIATIONS IN EACH CELL (FIBER). DUE TO PARALLEL ARRANGEMENT OF THICK & THIN PROTEIN FILAMENTS A. SKELETAL MUSCLE TISSUE- ATTACHED TO BONES B. CARDIAC MUSCLE TISSUE- ONLY IN THE HEART NON-STRIATED---LACKS CROSS-STRIATIONS A. SMOOTH MUSCLE TISSUE- VISCERA (INTERNAL ORGANS) AND ARTERY AND VEIN WALLS MUSCLE
Figure 36-7 Skeletal Muscle Structure SKELETAL MUSCLE STRUCTURE Section 36-2
Skeletal Muscle Fibers • Fiber- a single muscle cell with fibrils inside. • myofibril-gives muscle cells ability to change shape. Small unit of muscle that shows alternate light/dark bands. • actin-muscle protein of small molecular weight. Slides over and under myosin, forming actomyosin (protein formed during muscle contraction) • myosin-muscle protein of high molecular weight • sarcomere- smallest unit of contraction in skeletal muscle. (a cross-striation)
Sarcomere • I bands- area of Actin • A bands-area of overlapping actin & myosin • H zone-area of myosin (w/in A band) • Z lines-dark zone at center of I band-boundaries of sarcomere. Attached to actin • M line
Video 1 Video 1 • Click the image to play the video segment. Muscle Contraction, Part 1
Video 2 Video 2 Muscle Contraction, Part 2 • Click the image to play the video segment.
Sliding Filament Model of Muscle Contraction • When sarcromeres shorten, thick and thin filaments slide past one another • H zones and I bands narrow (H disappears!) • Z lines move closer together • During contraction each sarcomere contracts. Actin slides over and under Myosin, sarcomere shortens. Length of filaments does not change!
Myofilaments • Thin Filaments • composed of actin • associated with troponin and tropomyosin • Thick Filaments • composed of myosin • cross-bridges
Cross-bridge Cycling • myosin cross-bridge attaches to actin binding site • myosin cross-bridge pulls thin filament • ADP and phosphate released from myosin • new ATP binds to myosin • linkage between actin and myosin cross-bridge break • ATP splits • myosin cross-bridge goes back to original position
Figure 36-8 Muscle Contraction MUSCLE CONTRACTION Section 36-2 Relaxed Muscle Z line Myosin Actin Z line Movement of Actin Filament Actin Cross-bridge Sarcomore Binding sites Myosin Contracted Muscle During muscle contraction, the knoblike head of a myosin filament attaches to a binding site on actin, forming a cross-bridge. Powered by ATP, the myosin cross-bridge changes shape and pulls the actin filament toward the center of the sarcomere. The cross-bridge is broken, the myosin binds to another site on the actin filament, and the cycle begins again. Cross-bridges Z line
Cycle Diagram MUSCLE CONTRACTION Section 36-2 1 Myosin forms cross-bridge with actin 5 2 Myosin returns to original shape Cross-bridge changes shape 4 3 Cross-bridge releases actic Actin pulled
Relaxation • acetylcholinesterase – rapidly decomposes Ach • remaining in the synapse • muscle impulse stops • stimulus to sarcolemma and muscle fiber membrane • ceases • calcium moves back into sarcoplasmic reticulum • myosin and actin binding prevented • muscle fiber relaxes
SOURCES OF ENERGY FOR MUSCLE CONTRACTION • ATP-Adenosine Triphosphate. Found in muscle cells, regenerated from stores of Creatine Phosphate. • CP – Creatine Phosphate • Glycogen-a starch (polysaccharide) made of glucose. Small amount in muscle cells, most stored in liver. ** These 3 reactions can occur anaerobically, creating lactic acid. Aerobic occurance of these reactions is much more efficient at making ATP – no lactic acid!! ENERGY FOR MUSCLE CONTRACTION FROM ATP!
Oxygen Debt Oxygen debt – amount of oxygen needed by liver cells to use the accumulated lactic acid to produce glucose • oxygen not available • glycolysis continues • pyruvic acid converted to lactic acid (which is toxic to muscle cells, causes fatigue) • liver converts lactic acid to glucose in series of enzymatic rxns called the CORI cycle (needs oxygen!) • Oxygen debt is resolved during RECOVERY PERIOD. Glycogen is resythesized as oxygen is used to break down lactic acid (in liver!)
Neuromuscular Junction • also known as myoneural junction • site where an axon and muscle fiber meet • motor neuron • motor end plate • synapse • synaptic cleft • synaptic vesicles • neurotransmitters
Stimulus for Contraction • acetylcholine (ACh) • nerve impulse causes release of ACh from synaptic vesicles • ACh binds to ACh receptors on motor end plate • generates a muscle impulse • muscle impulse eventually reaches sarcoplasmic reticulum • and the cisternae
Skeletal Muscle Actions • origin – immovable end • insertion – movable end • flexors – muscles that bend a joint. • extensors – muscles that extend/straighten a joint. • *flexors and extensors are opposing pairs. When one is contracted, the other is relaxed. Ex. biceps and triceps • antagonistic action – a muscle acting in opposition to another muscle.
Figure 36-11 Opposing Muscle Pairs OPPOSING MUSCLE PAIRS Section 36-2 Movement Movement Biceps (relaxed) Biceps (contracted) Triceps (relaxed) Triceps (relaxed)
Muscle Fatigue • inability to contract • commonly caused from • decreased blood flow • ion imbalances across the sarcolemma • accumulation of lactic acid • cramp – sustained, involuntary muscle contraction
MORE ON MUSCLES • THE FORCE OF MUSCULAR CONTRACTION IS DETERMINED BY THE NUMBER OF INDIVUDUAL MUSCLE FIBERS STIMULATED. • AEROBICACTIVITY- MORE EFFICIENT; INCREASES CARDIAC ENDURANCE. • STEROIDS – SERIOUS SIDE EFFECTS. 1. PREVENT FROM REACHING FULL HEIGHT. 2. HEART DISEASE 3. CANCER 4. PSYCHOLOGICAL DISORDERS
Life-Span Changes • myoglobin, ATP, and creatine phosphate decline • by age 80, half of muscle mass has atrophied • adipose cells and connective tissues replace muscle tissue • exercise helps to maintain muscle mass and function
Clinical Application Myasthenia Gravis • autoimmune disorder • receptors for ACh on muscle cells are attacked • weak and easily fatigued muscles result • difficulty swallowing and chewing • ventilator needed if respiratory muscles are affected • treatments include • drugs that boost ACh • removing thymus gland • immunosuppressant drugs • antibodies
Integumentary System • Composed of several tissues • Maintains homeostasis • Protective covering (uv rays, microbes, scrapes, burns, water loss) • Retards water loss • Regulates body temperature • Houses sensory receptors • Contains immune system cells • Synthesizes chemicals • Excretes small amounts of waste • Cushions the body(shock absorber)
Skin functions as a is made up of the Regulator of body temperature Protector against UV radiation Remover of waste products Barrier to infection Dermis Epidermis which is the which is the Inner layer Outer layer
SKIN • LARGEST ORGAN IN THE BODY!!! • 15% IF TOTAL BODY WEIGHT.
SKIN Figure 36-13 The Structure of Skin Section 36-3