Airway Pressure Release Ventilation (APRV)
1.27k likes | 4.2k Vues
Airway Pressure Release Ventilation (APRV). Objectives. Provide the definition and names for APRV Explain the four set parameters. Identify recruitment in APRV using exhaled CO 2 . Recommend appropriate initial settings for APRV Make adjustments based on arterial blood gas results

Airway Pressure Release Ventilation (APRV)
E N D
Presentation Transcript
Objectives • Provide the definition and names for APRV • Explain the four set parameters. • Identify recruitment in APRV using exhaled CO2. • Recommend appropriate initial settings for APRV • Make adjustments based on arterial blood gas results • Discontinue ventilation with APRV
Introduction • Airway pressure release ventilation (APRV) is a relatively new mode of ventilatory support that, although outlined in 1987, did not become available in the United States until the mid-1990s. • APRV augments alveolar ventilation. Airway pressure is released from an elevated baseline pressure to produce an expiration. The elevated pressure facilitates oxygenation, while the pressure release increases minute ventilation.
Introduction • APRV has been successfully used in neonatal, pediatric, and adult forms of respiratory failure. Experimental and clinical use of APRV has been shown to facilitate spontaneous breathing and is associated with decreased peak airway pressures and improved oxygenation/ventilation when compared with conventional ventilation. Additionally, improvements in hemodynamic parameters, splanchnic perfusion, and reduced sedation/neuromuscular blocker requirements have been reported.
Introduction • APRV may offer potential clinical advantages for ventilator management of acute lung injury/acute respiratory distress syndrome and may be considered as an alternative “open lung approach” to mechanical ventilation. Whether APRV reduces mortality or increases ventilator-free days compared with a conventional volume-cycled “lung protective” strategy will require future randomized, controlled trials • http://www.youtube.com/watch?v=BIT2Gy9nxp4
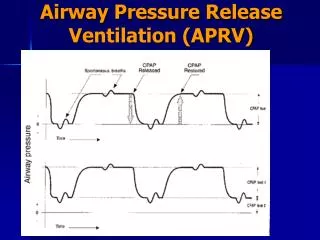
APRV Description • A mode of ventilation along with spontaneous ventilation to promote lung recruitment of collapsed and poorly ventilated alveoli. • The CPAP is released periodically for a brief period. • The short release along with spontaneous breathing promote CO2 elimination. • Release time is short to prevent the peak expiratory flow from returning to a zero baseline.
APRV (Airway Pressure Release Ventilation) • Provides two levels of CPAP and allows spontaneous breathing at both levels when spontaneous effort is present • Both pressure levels are time triggered and time cycled
AKA • BiVent – Servo • APRV – Drager • BiLevel – Puritan Bennett • APRV – Hamilton • Etc.
Lung Protective Strategies • Acute lung injury (ALI) and acute respiratory distress syndrome (ARDS) • Keep plateau pressures < 30 cm H2O • Use low tidal volume ventilation (4-6 mL/kg IBW) • Use PEEP to restore the functional residual capacity (FRC)
Lung Protective Strategies • As recently as 1993, the American College of Chest Physicians (ACCP) consensus conference failed to agree on an optimal mode of ventilation for any disease state or an optimal method of weaning patients from mechanical ventilation. The ACCP agreed that well-controlled clinical trials that defined the indications and uses of specific modes of ventilation were lacking. Now, quite a few years later, the hard science out there is still a bit scarce, but, we have learned a few things.
Lung Protective Strategies • Recently, discovery of the potential for mechanical ventilation to produce ventilator-associated lung injury has resulted in the development of new lung protective strategies. Lung protective strategies include those described in the open lung approach promoted by Amato et al. The open lung approach uses reduced tidal volumes (6 mL/kg or less) to prevent high-volume lung injury and over-distension of alveoli. • In addition, Amato et al. used elevated end expiratory pressure (average positive end-expiratory pressure [PEEP] 16 cmH2O), to prevent low volume lung injury from cyclic airway closure and re-opening.
Open the Lung and Keep it Open • ARDSNet study compared conventional tidal volume (mL/kg) to reduced tidal volume (6 mL/kg). • The results of the ARDSNet trial and a study conducted by Amato et al. suggest an association between reduced tidal volume and improved outcome. • Improved outcomes seen in the ARDSNet study were a result of not only reduced tidal volumes, but also increased PEEP • As a result, ARDSNetAssessment of Low tidal Volume and Elevated end-expiratory volume to Obviate Lung Injury (ALVEOLI) study was conducted to evaluate the role of higher levels of PEEP on survival, results were inconclusive
Lung Recruitment • Complete recruitment exceeds the lower inflection point used by Amato et al. to determine optimal PEEP levels. Recruitment begins at the lower inflection point and continues to the upper inflection point. • Therefore, elevated baseline airway pressure during APRV may produce near complete recruitment, thus minimizing low volume lung injury from cyclic recruitment. • APRV is less likely to produce over-inflation or high-volume lung injury, as airway pressures are lowered (released) in order to accomplish ventilation.
Lung Recruitment • Maintaining a constant airway pressure may be advantageous for several reasons. Constant airway pressure facilitates alveolar recruitment; enhances diffusion of gases; allows alveolar units with slow time constants to fill, preventing over-distension of alveoli; and augments collateral ventilation. Van Allen et al. noted that complete obstruction of an airway unit did not always result in collapse of the alveoli and, therefore, hypothesized that alternative pathways must exist.
Lung Recruitment • The pores of Kohn, located in the septa of the alveoli and open only during inspiration, first were believed to be responsible. However, two additional pathways were later credited with playing a role: (1) Lambert's canals connect terminal and respiratory bronchioles with adjacent peribronchial alveoli, and (2) channels of Martin interconnect respiratory bronchioles and serve to bypass the main pathway
Keeping Plateau Pressure < 30 cm H20 • What do you do if CO2 is rising and the plateau pressure is at 30 cm H2O? • Change to pressure control/increase rate/sedation • Permissive hypercapnia? • Low VT/high rates? • HFVO? • APRV…
Goals with APRV include the following: • Avoiding extension of lung injury • Minimal oxygen toxicity with high mean airway pressure • Recruiting alveoli & preventing de-recruitment • Minimizing peak airway pressure • Preventing atelectasis • Using sedation and paralysis conservatively
Why APRV • Clinicians have learned that cyclical opening and closing of injured lung units damages them (particularly if tidal volumes are large). We would prefer if the patient could be ventilated at the top of the volume pressure curve, at high lung volumes, without phasic changes. This can be achieved using high frequency oscillation, but adult oscillators are not widely available. For the majority of patients, increasing mean airway pressure without increasing peak pressure means prolonging the inspiratory time in a pressure control mode. The longer the inspiratory time (Ti), the better the oxygenation benefit
Indications • Primarily used as an alternative ventilation technique in patients with ARDS. • Used to help protect against ventilator induced lung injury.
Indications • The main causes of hypoxemia associated with ALI are shunting due to alveolar collapse and reduction in functional residual capacity. Therefore, a primary goal of the treatment of ALI is recruitment of alveoli and prevention of de-recruitment. Sustained plateau pressure is used to promote alveolar recruitment, while being maintained at an acceptable level [no more than 30 cmH2O, if possible]. • In addition, the number of respiratory cycles is minimized to prevent both the repetitive opening of alveoli and alveolar stretch that may result in lung injury. Patients in early-phase ALI often do not have impaired respiratory muscle strength or inadequate respiratory drive. Frequently, CPAP alone is sufficient to restore lung volume and increase lung compliance. However, when assistance with ventilation is required, APRV can be used. Intermittent airway pressure release allows alveolar gas to be expelled via natural lung recoil.
Goal To provide the lung protective ventilation supported by the ARDSnet research. Use an “Open lung” approach. Minimize alveolar overdistension. Avoid repeated alveolar collapse and reexpansion. Restore FRC through recruitment and, Maintain FRC by creating intrinsic PEEP.
Consider APRV when the Patient Has -- • Bilateral Infiltrates • PaO2/FIO2 ratio < 300 and falling • Plateau pressures greater than 30 cm H2O • No evidence of left heart failure (e.g. PAOP of 18 mm Hg or greater) • In other words, persistent ARDS
Possible Contraindications • Unmanaged increases in intracraneal pressure. • Large bronchopleural fistulas. • Possibly obstructive lung disease. • Technically, it may be possible to ventilate nearly any disorder.
Terminology • Four commonly used terms include: pressure high (P High), pressure low (P Low), time high (T High), and time low (T Low). • P High– the upper CPAP level. Analogous to MAP (mean airway pressure) and thus affects oxygenation. P High is the baseline airway pressure level and is the higher of the two airway pressure levels. Other authors have described P High as the CPAP level, the inflating pressure, or the P1 pressure (P1), also called High Peep.
P-High p-High is the upper CPAP or pressure setting when utilizing APRV. p-High regulates end-inspiratory lung volume & is analogous with mean airway pressure
Terminology • PEEP (Also called Plow or Low Peep) is the lower pressure setting. • P Low is the airway pressure level resulting from the pressure release. Other authors may refer to P Low as the PEEP level, the release pressure, or the P2 pressure (P2).
P-Low Servo I: Bi-Vent Draeger Evita The p-Low setting, sets the lower level of CPAP during the release phase. The term "p-Low" is used in Draeger & Hamilton medical ventilators. PB 840 BiLEVEL
T-High • T High-is the inspiratory time IT(s) phase for the high CPAP level (P High). • T High corresponds with the length of time for which P High is maintained
T-High Allows for sustained recruitment allowing for improved gas exchange by increasing alveolar surface area.
T-Low • T Low is the length of time for which the P Low is held (i.e. for which the airway pressure is released) • T High plus T PEEP (T low) is the total time of one cycle. • I:E ratio becomes irrelevant because APRV is really best thought of as CPAP With occasional releases
T-Low The t-Low sets the time interval for the low pressure/CPAP phase (p-Low). Allows for intermittent release in airway pressure, providing paCO2 removal. Partially unloads the patients work of breathing associated with pure CPAP breathing. The name "t-Low" is used in both Draeger and Hamilton ventilators. note- t-Low should not be considered "expiratory time" as the patient may exhale throughout the entire inspiratory phase. When using Bi-Level on the PB 840 there is no setting to set the low pressure interval. The operator must change frequency & "TH" to set a t-Low. This can become problematic when trying to precisely set a t-Low interval.
APRV: Setting P-High based on the Static Pressure Volume Curve Some newer mechanical ventilators provide the operator with automated tools to obtain a static Pressure Volume (P/V) Curve in the ventilated patient. These tools provide the clinician a simple, safe, and reproducible method to assess the P/V curve for various pulmonary conditions.
APRV: Setting P-High based on the Static Pressure Volume Curve For example many Respiratory care practitioners utilize the P/V to identify the lower and upper inflection points. “The lower section of the P/V curve, where the compliance is less favorable, corresponds to a condition in which a given number of alveolar units are collapsed” It is common for the practitioner to set Positive End-Expiratory Pressure (PEEP) 1-to-2 cmH2O above the lower inflection point to prevent de-recruitment and minimize injury related to shear stress from the repetitive opening and closing of the alveoli. The upper inflection point indicates a decrease in lung compliance and may specify over-distention of the lung units. The assessment of the static P/V curve can provide insight on how well a patient will respond to the application of Airway Pressure Release Ventilation. Evaluation of the “hysteresis” (difference between the inflation and the deflation limb) can indicate the extent of potential lung units that may be recruited. If the patient has very little probability for alveolar recruitment then APRV is less likely to be beneficial and unjustified.
APRV: Setting P-High based on the Static Pressure Volume Curve If the patient meets indications for utilizing APRV, the operator can use points on the P/V to safely set P-High. P-High should be set always below the pressure which generated the “Upper Inflection Point”. P-High can be set 1-to-2 cmH2o above the “Lower Inflection Point”. The practitioner can calculate “Best Compliance” and set P-High according to the pressure that generated the best compliance (some P/V tools automatically calculate this). The static P/V curve provides a more diagnostic and patient tailored approach to setting P-High.
P/V Tool for more intelligent patient assessment The automated P/V Tool uses an empirical and repeatable method to find best PEEP, based on respiratory mechanics.It also enables sophisticated lung recruitment maneuvers and therapy assessment. This maneuver records the static pressure/volume curve quickly and easily at the bedside. It employs an adjustable pressure ramp, in which airway pressure is slowly increased to an upper limit as resultant volume and pressure are recorded.After the maneuver, the cursor function lets you inspect inflection points so that you can easily visualize the linear portion of the compliance curve.
Advantages of APRV • Uses lower PIP to maintain oxygenation and ventilation without compromising the patient’s hemodynamics(Syndow AJRCCM 1994, Kaplan, CC, 2001) • Shown to improved V/Q matching(Putensen, AJRCCM, 159, 1999) • Required a lower VE suggesting reduced VD/VT(Varpula, Acta Anaesthesiol Scand 2001)
APRV vs. PCIRV • Although both modes increase PAW, PCIRV usually requires higher PIP and heavy sedation/paralytic, whereas APRV allows for spontaneous breathing • Increases cardiac index • Decreases central venous pressure
Additional Advantages - Compared to PCIRV • APRV increases oxygen delivery and • Reduces the need for sedation and paralysis • APRV also improves renal perfusion and urine output when spontaneous breathing is maintained. (Kaplan, Crit Care, 2001; Hering, Crit Care Med 2002)
Advantages of Spontaneous Breathing • The benefits of APRV may be related to the preservation of spontaneous breathing. • Maintaining the normal cyclic decrease in pleural pressure, augmenting venous return and improving cardiac output. (Putensen, AJRCCM, 1999) • The need for sedation is decreased.
Preserve Spontaneous Breathing • The dashed line in each figure represents the normal position of the diaphragm. • The shaded area represents the movement of the diaphragm. (Froese, 1974)