Airway Pressure Release Ventilation
280 likes | 693 Vues
Airway Pressure Release Ventilation. APRV review and indications in paediatrics. APRV. Terminology How it works Indications Advantages/disadvantages Review of paediatric studies Set-up (paed specific) Weaning Discussion. APRV.

Airway Pressure Release Ventilation
E N D
Presentation Transcript
Airway Pressure Release Ventilation APRV review and indications in paediatrics
APRV • Terminology • How it works • Indications • Advantages/disadvantages • Review of paediatric studies • Set-up (paed specific) • Weaning • Discussion
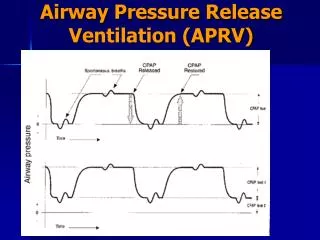
APRV • Continuous positive airway pressure with regular, brief releases in airway pressure to facilitate alveolar ventilation and CO2 removal • Time triggered, pressure limited, time cycled mode • Allowing unrestricted spon. Breathing throughout the ventilatory cycle
Terminology • P high = the baseline airway pressure level, • P low = airway pressure resulting from airway release (PEEP) • Time high = the length of time that P high is maintained • Time PEEP = time spent in airway release at P low
How does it work? • The constant airway pressure at P high facilitates alveolar recruitment and therefore enhances gas diffusion • The long time at P high allows alveolar units with slow time constants to open • The timed releases in pressure T PEEP allows alveolar gas to be expelled via natural lung recoil not with repetitious opening of alveoli
Indications • Recruitable low compliance lung disorders • Lung dysfunction secondary to thoracic restriction i.e.. obesity, acites • Inadequate oxygenation with FiO2 > .60 • PIP> 35 cmH2O and /or PEEP>10 cmH2O • Lung protective strategies (high PEEP, low Vt) are failing • Can be used with other interventions i.e.. INO therapy, prone positioning
Advantages • Significantly lower peak Paw and improved oxygenation when compared to conventional ventilation • Requires lower min. vol. suggesting decreased dead space ventilation • Avoids low volume lung injury by avoiding repetitious opening of alveoli
Advantages • Allows for spontaneous breathing at all points in the respiratory cycle • Spon. breathing tends to improve V/Q matching • Decreased need for sedation and near eliminating need for neuromuscular blockade
Disadvantages • Volumes affected by changes in compliance and resistance and therefore close monitoring required • Integrating new technology • Limited research and clinical experience
Paediatric Studies • Studies in the paediatric population are few and small • Several are ongoing • 3 published • Most evidence is extrapolated from the adult studies
Airway pressure release ventilation in paediatricsSchultz T, et al. Pediatric Crit Care Med. 2001 jul;2(3):24 3-6 Airway pressure release ventilation in paediatricsSchultz T, et al. Pediatric Crit Care Med. 2001 jul;2(3):24 3-6 • a prospective, randomized, cross-over trial of 15 PICU pt. >8kg • Randomized to either VCV (9) or APRV (6) • APRV had lower PIP and Pplat than VCV in all patients • No sig. differences in physiologic variables e.g.. EtCO2
Airway Pressure Release in a Paediatric PopulationJones R, Roberts T, Christensen D. St.Luke’s Reginal Medical Center, Boise, ID AARC open Forum 2004 • A case series of 7 paediatric patients aged 3 to 13 with ALI • All failing conventional PPV with severe hypoxemia • 2 failed HFOV with severe hypoxemia • 6/7 lower PIP, all had higher MAP, all had improved oxygenation, all had lower FiO2 requirements
Airway Pressure Release Ventilation: A Pediatric Case SeriesKrishnan,J. ,Morrison, M.: University of Maryland, Pediatric Pulmonology 42:83-88. 2007 • retrospective review of 7 pediatric cases • Approved by the University of Maryland institutional review board • All pt.s failed on conventional ventilation • Implemented similar starting parameters as to be described later
Case 1 • 9 y.o. leukemia with septic shock, ARDS and MSOF • SIMV PC , FiO2 = 1.0, PIP/PEEP= 38/14 cmH2O, PaO2= 91 mmHg • Failed HFOV secondary to hypotension • APRV – Phigh 37 cmH20, Plow 0cmH2O with Pmean of 32 cmH2O • PaO2 improved over 84 hrs and required no NMB • Weaned and d/ced home
Case 2 • 5 y.o. 60% body area burns with development of sepsis and ARDS • Failed convention ventilation (39/19) and was placed on HFOV with intractable hypercarbia (PaCO2= 121mmHg) • APRV of 40/0 PaCO2 improved to 78mmHg • MSOF worsened and pt. made limited resuscitation
Case 3 • 8 y.o. CF with development of ARDS • Pt. required heavy sedation with CV with 30/13 and FiO2 = .50 • APRV settings 28/0 and sedation was decreased and pt. was extubated to NIV • No NMB was required
Case 4 • 4 y.o. with fever, jaundice, hepatomegaly, pancytopenia and hypofibrinogenemia • Requiring CRRT for MSOF and ARDS • CV with 40/10 cmH20 and FiO2 = 1.0 • APRV 34/0 and O2 weaned to .6 and NMB was lifted • Weaned to CPAP and septic shock resolved but pt suffered an intracranial haemorrhage which led to his death • Autopsy revealed hemophagocytic lymphohistiocytosis
Case 5 • 1 y.o. leukemia post bone marrow transplant with sepsis and neutropenia and graft vs host disease and tracheotomy • Difficult to ventilate with PaCO2 of 64mmHg and tachypnea and distress • APRV 30/0 cmH20 and was rapidly weaned with noted increase in comfort • Weaned to FiO2 to .45 and PaCO2 = 39mmHg • Later exacerbation of leukemia resulted in renal failure
Hints for set-up • P high = same as plateau or 125% of mean Paw • PEEP = 0 cmH2O • T PEEP = long enough to get returned Vt but not long enough to derecruit – titrate to end at 25 -50% of the PEF • T high = manipulated to achieve RR • PS = set to avoid flow hunger with spon. resps.
Set-up Set-up • Be patient • The change to APRV may not provide instant improvement in oxygenation • The effects may take hours to be realized • Has been shown that the maximum benefit occurred at approx. 8 hours after implementation
Weaning • Decrease FiO2 first and then P high is small increments • As compliance improves the TCs lengthen and T PEEP may need adjustment to allow for adequate Vt • When P high is weaned to a low level consider extubation • Lengthen T high and therefore decreasing the # of pressure releases per minute
Lets talk! Any questions?