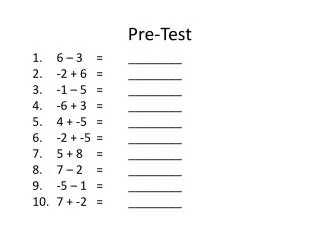
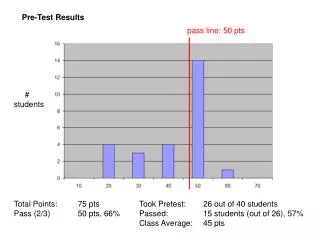
Pre-test
Pre-test. 1.Regargind latest guideline on initiation of ARV start at CD4 of A. <200cc/ml B.>200cc/ml C..<350cc/ml D.<500cc/ml E. non of the above 2.Best ARVs combination for PMTCT should contain at least A. AZT B. 3TC C.TDF D.LPV/r E. NVP. 3.Best option advocated by the WHO IS


Pre-test
E N D
Presentation Transcript
Pre-test • 1.Regargind latest guideline on initiation of ARV start at CD4 of • A. <200cc/ml • B.>200cc/ml • C..<350cc/ml • D.<500cc/ml • E. non of the above • 2.Best ARVs combination for PMTCT should contain at least • A. AZT • B. 3TC • C.TDF • D.LPV/r • E. NVP
3.Best option advocated by the WHO IS • A.Option a • B. Option b • C.Option c • D. Option a+ • E. option b+ • 4. Factors associated with MTCH include • A.low viral load • B.infections • C. prolong rupture of membranes • D.cracked nipples • E. antepartumhaemorrhage
5.concerning choice of ARVs for PMTCT • A.NVP should be avoided in the first trimester • B.EFZ can be use in the first trimester • C.NVP is safe in TB/HIV Co infection • D.AZT IS unsafe throughout pregnancy • E. EFZ Is teratogenic hence avoid in 1st trimester
CURRENT TREND In management of MATERNAL TO CHILD TRANSMISSION OF HIV BY DR ZAINAB ABDULAZEEZ UMAR DEPARTMENT OF FAMILY MEDICINE
SYNOPSIS • OBJECTIVES • INTRODUCTION • SCOPE OF HIV • MTCT • PMTCT • HAART AND PMTCT • INFANTS FEEDING • CONCLUSION • REFERENCES
Learning Objectives • To become familiar with factors affecting the transmission of HIV from mother-to-child • To become familiar with interventions to prevent the transmission of HIV from mother-to-child • To be familiar with current guidelines in managing MTCT
INTRODUCTION • HIV the aetiological agents of AIDS have been identified as HIV-1 and HIV-2. These viruses belong to the Lentivirus group of Retroviridae family. • HIV continues to be a major global public health issue, having claimed more than 36 million lives so far. • The Human Immunodeficiency Virus (HIV) targets the immune system and weakens people's surveillance and defense systems against infections and some types of cancer.
As the virus destroys and impairs the function of immune cells, infected individuals gradually become immunodeficient • Immunodeficiency results in increased susceptibility to a wide range of infections and diseases that people with healthy immune systems can fight off • . The most advanced stage of HIV infection is Acquired Immunodeficiency Syndrome (AIDS), which can take from 2 to 15 years to develop depending on the individual • . AIDS is defined by the development of certain cancers, infections, or other severe clinical manifestations
The transmission of HIV from an HIV-positive mother to her child during pregnancy, labour, delivery or breastfeeding is called mother-to-child transmission. • In the absence of any interventions transmission rates range from 15-45%. • This rate can be reduced to levels below 5% with effective interventions. • These can be achieved by setting global norms and standards for HIV prevention, care and treatment of pregnant women, mothers and their children,
with nearly 1 in every 20 adults living with HIV. 69% of all people living with HIV are living in this region.
, down from 3.4 New HIV infections among children have declined by 52% since 2001.
SCOPE IN NIGERIA • HIV Prevalence in Nigeria is 4.6% • Nigeria now has the second highest number of plwhivin the world after South Africa. • Over 90% of HIV infection in children are as a result of MTCT. • An estimated 220,000 exposed children born each year. • Without PMTCT about 88,000(40%) of these are infected. • With PMTCT about 2% (4,400) infected. • Nigeria has 30% of the global burden of MTCT.
SCOPE IN KANO In 2009 with 372 HIV infected pregnant women detected out of 3470 ANC clients There were 4922 deliveries out of which 125 were HIV positive, giving a prevalence rate of 2.54%. the transmission rate from mother to child amongst those who accessed PMTCT services was about 2-3 % .
Scope of HIV/AIDS in women • HIV spreads rapidly, particularly among young women. • These women are in their most productive and reproductive years. • There are various factors that make women vulnerable to HIV infection, These factors include: • Biological factors • Socio-cultural factors
Biological factors • Women have larger surface area of the genital mucosa • Semen infected with HIV contains higher concentrations of virus than vaginal fluid. • Young women have immature cervix and scanty vaginal secretion hence barrier to infection is reduced • Women become more vulnerable again after menopause • Tearing and bleeding during intercourse further increased predisposition to infection. This can occur during rough vagina sex, anal sex, dry sex or rape • Untreated STIs multiplies the risk of HIV infection by 300-400%.
Socio-cultural factors • Economic and societal approved dependency on men • Rights of women are abused and often violated. • Condom use by stable partners is often frowned at. • Cultural practices often expose women to multiple partners e.g polygamy, widow inheritance, wife hospitality • Gender inequalities which negatively impacts on and their effect on seeking care and prevention efforts • Burden of being the care provider in the home may supercede the need to care for herself
Mother-to-Child Transmission MTCT of HIV can occur during: • Pregnancy • Labour and delivery • Breastfeeding
Mother-to-Child Transmission 100 infants born to HIV-infected women who breastfeed, without any interventions 60 to 75 infants will not be HIV-infected About 15 infants infected during labour and delivery 5–15 infants infected during breast-feeding 5–10 infants infected during pregnancy 25–40 infants will be HIV-infected
Timing of Transmission: Targeting Prevention (In an Untreated Non-Breastfeeding Population, Total Transmission Rate is up to 25%) • Pregnancy ---------- (5 - 10%) • Delivery ------- (10 -15%) • Breastfeeding ----- (10 - 15%)
Risk Factors for MTCT • Labour and Delivery • High maternal viral load • Prolonged rupture of membranes • Invasive delivery procedures • Chorioamnionitis • Breastfeeding • High maternal viral load • Duration • Early mixed feeding • Breast fissures, infections • Poor maternal nutrition • Oral disease in infant • Pregnancy • High maternal viral load • Infection • STIs • Malnutrition • Haemorrhage
PMTCT Prevention Of Mother To Child Transmission • Best practice for antenatal, intrapartum and postpartum care of the HIV-positive mother to reduce mother-to-child transmission
Elements of a successful programme for Prevention of HIV Infection in Infants and Young Children • Element 1 Primary prevention of HIV infections • Element 2 Prevention of unintended pregnancies among women infected with HIV • Element 3 Prevention of HIV transmission from women infected with HIV to their infants • Element 4 Provision of treatment, care and support to women infected with HIV, their infants and their families
Element 1: Prevention of Primary HIV Infection ABCs of primary HIV prevention for parents-to-be: A = Abstain B = Be faithful to one HIV-uninfected partner C = Condom use – use condoms consistently and correctly Adapt approach to local culture and target groups at risk
Element 2: Prevention of Unintended Pregnancies Among Women Infected with HIV • Access to counselling and referral for family planning • Safe, consistent, effective contraception
Element 3: Prevention of HIV Transmission from Women Infected with HIV to Their Infants Core Interventions • HIV testing and counselling • Antiretrovirals • Safer delivery practices • Safer infant-feeding practices Combination interventions can reduce the MTCT rate to as low as 2% in the absence of breastfeeding.
Element 4: Treatment, Care and Support for Women Infected with HIV and their Families • Prevention and treatment of OIs • ARV treatment • Treatment of symptoms • Palliative care • Nutritional support • Reproductive healthcare • Psychosocial and community support
Specific Interventions to Reduce Mother-to-Child Transmission • HIV testing and coucelling in pregnancy • Antenatal care • Antiretroviral agents • Obstetric interventions • Avoid amniotomy • Avoid procedures: Forceps/vacuum extractor, scalp electrode, scalp blood sampling • Restrict episiotomy • Elective cesarean section • Remember infection prevention practices • Newborn feeding: Breast milk vs. formula
Testing and Counseling for PMTCT • Offered in the following settings • Antenatal care • Labour and delivery • Postnatal • Family planning and other services • Information offered are the following: • HIV Infection and mode of transmission • Safer sex practices • Prevention and treatment of sexually transmitted infections (STIs) • Prevention of HIV in infants and young children including interventions for PMTCT • HIV testing, post-test counseling, and follow-up services
INFORMATIO OFFERED TO HIV +VES (POST TEST) • Antiretroviral treatment/prophylaxis • Infant-feeding counseling and support • Information and counseling on family planning • Receive education on the importance of delivering in a setting where universal precautions and safer obstetric practices are implemented. • Secure early access to HIV treatment, care and support services. • Receive information and counseling on the prevention of HIV transmission to others. • Receive follow-up and ongoing health care for themselves and their HIV-exposed infants. • Disclose their results to partners and family members.
Lab. Testing for HIV infections • Detectable components or products of viral infection for diagnosis • Antibodies- • Rapid tests • ELISA(reactive/non-reactive), • Western blot (positive, negative, Indeterminate.) • Antigen- antigen P24 • Nucleic acid- polymerase chain reaction • Whole(viable)virus- viral culture
Laboratory testing(4) CD4 lymphocyte count. • Normal laboratory ranges 500-1400/mm. • Most useful for assessing immune function. • Degree of immuno-suppression determines staging of HIV infection, recommendations for ARV and prophylaxis against OIs. Viral Load estimation • goal is to reduce viral load to undetectable (<400 copies/mL)
Other Tests: Baseline Labs tests • FBC (anemia with ZDU) • LFTs (mitochondrial disease with NRTI, elevated ALT w/ NNRTI and PI) • amylase (pancreatitis with NRTI) • early 1-hr OGT (GDM with PI) • creatinine • Hep B & C, CMV, toxo
Antenatal Care • Most HIV-infected women will be asymptomatic • Watch for signs/symptoms of AIDS and pregnancy-related complications • Treat STDs and other coinfections • Counsel against unprotected intercourse • Avoid invasive procedures and external cephalic version • Give antiretroviral agents • Counsel about nutrition HIV and Pregnancy
Principles of ARV use • Strict adherence critical but a challenge in pregnancy • ARVs have side effects that need clinical and lab monitoring • Beware of drug interactions • Resistance may develop if adherence is not excellent or if drug interactions affect drug levels, resistance may occur • Resistance may be spread to baby and to partner With excellent adherence and monitoring, risks of ARV are minimised and benefits are maximised
HIV in Pregnancy: Drug Treatment • The goal in pregnancy is to reduce viral load to undetectable to minimize perinatal transmission. • However, the woman should be counselled and willing to adhere to the regimen • She should be counselled on the risks and benefits of the ARVs
Evolution of the efficacy of the ARV prophylaxis: 1994-2004 % Transmission Transmission Rate (%)
OTHERS Fusion Inhibitor • Enfuvirtide (ENF, T-20) CCR5 Antagonist • Maraviroc (MVC) Integrase Inhibitor • Raltegravir (RAL)
FIRST - LINE AND SECOND-LINE REGIMEN • A first-line regimen is a combination of drugs that will be used in a patient who has no prior ART experience. This means that the patient has never taken ARV drugs before. • Most commonly, a first-line regimen will consist of two NsRTI's and one NNRTI. • Many patients will eventually develop failure of therapy: the first-line therapy will not be effective anymore (often because the drugs were not taken correctly). In that case, the doctor may decide to switch to a second-line regimen. • Usually, the second-line regimen will consist of 2 NRTI + 1 PI.
ART INITIATION ART should be initiated in all pregnant women based on the following criteria. • CD4 count of less than or equal to 350 irrespective of WHO clinical staging. • WHO stages III and IV irrespective of CD4 cell count. • Nigerian guideline Recognizes pregnancy as an indication for prophylactic ART irrespective of CD4 count, viral loads or clinical staging