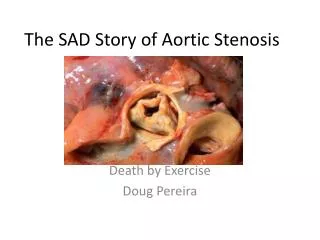
Aortic Stenosis
Aortic Stenosis. Clinical Case Study Ema Thake University of Utah June 8, 2012. Aortic Stenosis. As the aortic valve becomes more narrow, the pressure increases inside the left heart ventricle. causes the left heart ventricle to become thicker, decreasing blood flow

Aortic Stenosis
E N D
Presentation Transcript
Aortic Stenosis Clinical Case Study EmaThake University of Utah June 8, 2012
Aortic Stenosis • As the aortic valve becomes more narrow, the pressure increases inside the left heart ventricle. • causes the left heart ventricle to become thicker, decreasing blood flow • Can lead to chest pain and shortness of breath. • Severe forms of aortic stenosis prevent enough blood from reaching the brain and rest of the body. This can cause light-headedness and fainting Aortic Stenosis. http://www.ncbi.nlm.nih.gov/pubmedhealth/PMH0001230/
Aortic Stenosis • Symptoms • Breathlessness • Chest pain • Fainting, dizziness • Treatment • Stop smoking • Treatment for high cholesterol • Surgery to replace or repair the valve • Medications • Diuretics • Nitrates • Beta blockers
Patient GH • 71 year old male • Admitting diagnosis: for pre-op consultation for Aortic stenosis with aortic root dilation and ascending aorta dilation, with coronary artery disease • On admit: • Wt: 113.2 kg; Height: 173 cm • BMI: 37.82 (obese – grade II) • Extensive medical history
Medical/Nutritional History • PAST MEDICAL HISTORY: • Aortic stenosis with bicuspid aortic valve. • Aortic root and ascending aorta dilation • Coronary artery disease, status post CABG in 2001 • Type 2 diabetes, non-insulin dependent. • COPD • Hypertension • Hyperlipidemia • Renal insufficiency • Lung disease • The patient complains of irregular heartbeats or palpitation • Peripheral vascular disease • Obstructive sleep apnea, for which he does not use a CPAP machine • GERD • Osteoarthritis in his shoulders • Chronic low back pain, status post fusion. • Pancreatitis • Non-union of his sternum with broken sternal wires
Medical/Nutrition History • PAST SURGICAL HISTORY: • Coronary artery bypass grafts in 2001 • Angioplasty x 3 with stents to his circumflex • Cholecystectomy • Right knee surgery • Lower back fusions in 1999
Medical/Nutrition History FAMILY HISTORY: Significant for coronary artery disease. Father died from an MI at the age of 52. The patient has 3 brothers, who have had coronary artery bypass grafts in the past. Another sister had coronary disease, who is now deceased. SOCIAL HISTORY: The patient reports approximately 50-pack-year smoking history. The patient quit 1-1/2 years ago. The patient quit using alcohol 2 years ago and denies any drug history. The patient is married, lives with his wife in Green River, Wyoming and is retired.
Biochemical Piper and Kaplan, 2012
Medications Furosemide Atorvastatin Metaprolol Metformin Omeprazole Warfarin Sitagliptin Potassium Chloride
Clinical • No apparent skin breakdown • Edema on legs caused some broken skin • No pressure ulcers • Swallowing Evaluations • POD #12 - First attempt failed by patient • POD #19 – Passed eval., advanced to dysphagia 3 diet
Nutrition Diagnosis Inadequate oral intake related to intubation and sedation as evidenced by need for nutrition support. Obesity as evidenced by BMI 37.82.
Nutrition Intervention • DHT placed • 5/6 – trophic feeds • 5/7 – Promote @ 75 ml/hr • 5/10 – Promote @ 90 ml/hr • 5/15 – DHT accidentally pulled out • 5/16 – Promote @ 25 ml/hr after DHT replacement • 5/18 – Promote @ 90 ml/hr – resp. failure, intubated again • 5/19 – Promote @ 40 ml/hr • 5/20 – Promote @ 75 ml/hr – IDC indicated underfeeding • 5/25 – DHT accidentally pulled out, diet advanced to dysphagia 3
Nutrition Intervention • Tube feed initiated - Promote • Adjusted based on needs • Estimated needs and IDC • 2025-2430 kcal/day (25-30 kcal/kg AdjBW) • 97-122 g protein/day (1.2-1.5 g/kg AdjBW) • SLP evaluation • Advanced diet
Monitoring & Evaluation • IDC to monitor adequacy of the tube feeds • Calorie counts to assess oral intake when diet was advanced • Notes • Percentage of meals eaten
Reflection/Personal Assessment I had the opportunity to assist in the placement of a DHT in this patient. I found that experience to be very valuable. It was good to see the patient through each stage of recovery. Would have liked to gain more information about the education he received for discharge diet.
References Svagzdiene M, Sirvinskas E, Benetis R, Raliene L, Simatoniene V. Atrial fibrillation and changes in serum and urinary electrolyte levels after coronary artery bypass grafting surgery. Medicina (Kaunas). 2009;45(12):960-70. Piper GL, Kaplan LJ. Fluid and electrolyte management for the surgical patient. SurgClin North Am. 2012 Apr;92(2):189-205, vii. Epub 2012 Feb 9 Atrial Fibrillation/Flutter. http://www.ncbi.nlm.nih.gov/pubmedhealth/PMH0001236/ Aortic Stenosis. http://www.ncbi.nlm.nih.gov/pubmedhealth/PMH0001230/