References
Macroporous Monolithic Poly (2- Hydroxyl ethyl Methacrylate) Cryogels as a matrix for cytapheresis W. Akande* 1 , L. Mikhalovska 1 , I. Savina 1 , H. Kirsebom 2 ,S. James 1 , B. Mattiasson 2 , S. Mikhalovsky 1

References
E N D
Presentation Transcript
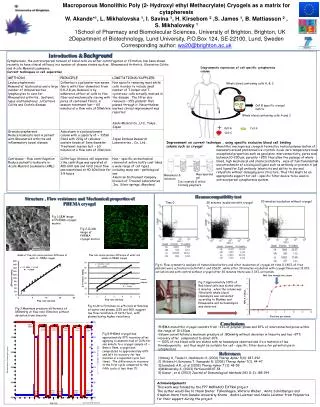
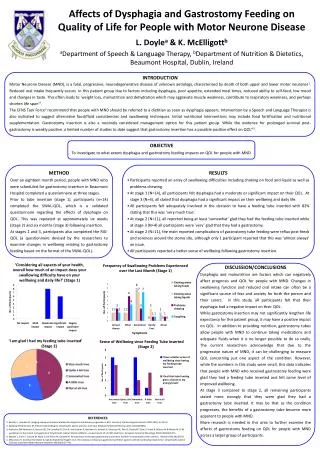
Macroporous Monolithic Poly (2- Hydroxyl ethyl Methacrylate) Cryogels as a matrix for cytapheresis W. Akande*1, L. Mikhalovska 1, I. Savina 1, H. Kirsebom 2 ,S. James 1, B. Mattiasson 2 , S. Mikhalovsky 1 1School of Pharmacy and Biomolecular Sciences, University of Brighton, Brighton, UK 2Department of Biotechnology, Lund University, P.O.Box 124, SE-22100, Lund, Sweden Corresponding author: wa20@brighton.ac.uk Introduction & Background Cytapheresis, the extracorporeal removal of blood cells via either centrifugation or filtration, has been shown recently to have clinical efficacy in a number of disease states such as , Rheumatoid Arthritis, Ulcerative Colitis and Acute Myeloid Leukaemia . Current techniques in cell separation Diagrammaticexpression of cell specific cytapheresis column Whole blood containing cells A, B, C Cell B specific cryogel matrix Whole blood containing cells A and C Cell A Cell B Cell C Improvement on current technique , using specific exclusive blood cell binding column such as cryogel Monolithic macroporous cryogels formed by radical polymerisation of monomers around preformed ice crystals in sub zero temperature have exceptional properties such as good pore interconnectivity, pores size between 10-200 µm, porosity > 85% thus allow the passage of whole blood, high mechanical and chemical stability , ease of functionalisation and attachment of a biological ligand such as antibody or protein A (an avid ligand for IgG antibody )elasticity and ability to dry and rehydrate without damaging pore structure. Thus this might be an appropriate support for cell – specific filter device to be used in extracorporeal cytapheresis system. Macroporous gel Monomers & initators Ice crystals & initial forming polymers Heamocompatiblity test Structure , Flow resistance and Mechanical properties of PHEMA cryogel 30 minutes incubation without cryogel Time 0 30 minutes incubation with cryogel Fig 1;SEM image of PHEMA cryogel matrix Fig 2;CLSM image of PHEMA cryogel matrix Fig 6; Flow cytometric analysis of human blood before and after incubation of cryogel.At time 0 1.40% of free platelet were activated in both PAC-1 and CD62P , while after 30 minutes incubation with cryogel there was 13.10% activation and with control without cryogel after 30 minutes there was 3.33% activation, Fig 7;Approximately 100% of Red blood cells was eluted after 6 minutes , when the column was filled with whole blood. Heamolysis was calculated according to Blankey and Dinewoodie and no haemolysis was observed Fig 4;Ultra filtration co-efficient at 5ml/min of water and plasma 1225 and 909, suggest low flow resistance of both fluid , with plasma having higher resistance Fig 3;Maximum pressure difference of 180mmHg at flow rate 15ml/min without deviation from linearity • PHEMA monolithic cryogel consists from ~13% of polymer phase and 87% of interconnected pores within the range of 10-120µm • Column can withstand a maximum pressure of 180mmHg without deviation in linearity and has ~97% recovery after compressed to about 60% • ~ 100% of red blood cells are eluted with no haemolysis observed and it’s a material of low thrombogenicity and thus might be suitable for cell – specific filter device for potential use in cytapheresis Conclusions Fig 5;PHEMA cryogel had approximately 97% recovery after applying a constant load of 0.2N for one minute to a cryogel sample of ~ 8mm x 9mm, cryogel was compressed to approximately 60% and left to recovery for two minutes in a repeated cycle five times . The difference in recovery in the first cycle compared to the fifth cycle is less than 1%. 1)Yamaji K, Tsuda H, Hashimoto H. (2001) TherapApher 5(4): 287-292 2) Shibata H, Kuriyama T, Yamawaki N. (2003) TherapApher 7(1): 44-47 3)Saniabadi A.R., et al (2003) TherapApher 7 (1): 48-59 4)Mikhalovsky S, (2003) Perfusion18:47-54 5) Kumar , et al (2003) Journal of Immunological Methods 283 (1-2): 185-194 References Acknowledgements This work was funded by the FP7 MONACO EXTRA project The author would like to thank Dieter Falkenhagen, Viktoria Weber , Anita Schildberger and Stephan Harm from Danube University Krems , Andre Leistner and Aneila Leistner from Polymerics for their support during the project