Gene diagnosis (Gene testing)
370 likes | 433 Vues
Gene diagnosis (Gene testing). Medical Genetics. Gene diagnosis. Detection of gene mutation by DNA analysis to diagnose genetic disorder

Gene diagnosis (Gene testing)
E N D
Presentation Transcript
Gene diagnosis(Gene testing) Medical Genetics
Gene diagnosis • Detection of gene mutation by DNA analysis to diagnose genetic disorder • The positive result of gene diagnosis is more objective evidence with respect to history, signs, symptoms and pedigree analysis in diagnosis of single gene disorder • However, the disorder diagnosis can not be excluded with the negative result of gene testing due to the complexity and limited detection rate of gene mutation Master
In 1978, Dr.Yuet Wai Kan first successfully fulfill prenatal genetic diagnosis of sickle cell anemia, which represents the birth of clinical gene diagnosis The history of gene diagnosis
The necessity of gene diagnosis • More than 6000 single gene disorders have been found. Most of them can not be treated effectively • While the disorders can be prevented by prenatal gene diagnosis
Typing gene diagnosis according to clinic purpose • Clinical diagnosis • Object: patient (proband of a pedigree) • Method: direct analysis of relevant gene for seeking mutation responsible for disorder • Purpose: rendering diagnosis, guiding treatment and preventing recurrence • Disease spectrum: all genetic diaorders Master
Presymptomatic disgnosis • Object: asymptomatic individual with high risk for disorder in a pedigree of autosomal dominant inherence showing delayed onset • Method: direct analysis of relevant gene for seeking mutation responsible for disorder • Purpose: predicting the occurrence of disorder and avoiding vertical transmission of disease-causing mutation • Disease spectrum: genetic disorders showing delayed onset, e.g. Huntington chorea
Prenatal diagnosis • Object: fetus with high risk for getting severe disease-causing mutation • Method: direct analysis of relevant gene for seeking mutation responsible for disorder, or indirect diagnosis by gene linkage analysis • Purpose: avoiding birth of patient with severely genetic disorder • Disease spectrum: severe and untreatable genetic disorders
Typing gene diagnosis according to analysis method • Direct gene diagnosis • Object: patient (proband of a pedigree), or asymptomatic individual, or fetus with high risk for genetic disorder • Method: direct analysis of relevant gene for seeking mutation responsible for disorder • Gene spectrum: relatively small genes prone to analysis with quick, inexpensive and reliable method. And the relationship between gene and disorder is explicit Master
Indirect gene diagnosis • Object: a pedigree of genetic disorder compulsorilyincluding the proband • Method: gene linkage analysis with SNPs or/and STRs in relevant gene to speculate the transmission status of risk chromosome carrying disease-causing gene • Gene spectrum: large gene difficult to analysis with quick and inexpensive method, or the mutation of proband is undetectable
More definition • Mutation spectrum: a collection including all mutations published in a gene • Known mutation testing: analyzing mutations published previously, especially the common mutations in a population • Unknown mutation testing: analyzing the complete sequence of a gene to detect mutation. the found mutations may be published previously, also may be novel Master
Gene diagnosis of β-Thalassemia • Known mutation testing • In Chinese, about 11 known mutations of HBB gene are responsible for more than 95% of patients with β-Thalassemia • That is, more than 95% of patients may be diagnosed by analyzing the 11 mutations of HBB gene.
Gene diagnosis of Hemophilia A • X-linked recessive inheritance, and thus mainly occurs in males (OMIM 603700) • General symptoms are internal or external bleeding episodes involved in joints, muscles, digestive tract and even brain in patients with severe hemophilia. While patients with mild haemophilia suffer minor symptoms except after surgery or serious trauma Familiar
Unknown mutation testing • There is no mutation hotspot found in F8 gene • Complete sequence is analyzed by DNA sequencing to seek mutation. • A important step: analyzing the property of the base substitution found, polymorphism variation or disease-causing mutation
c.138 TGG>TCG Trp>Ser Missence mutation
Gene diagnosis of Huntington’s disease • Autosomal delayed dominant inheritance (OMIM 143100) • A neurodegenerative genetic disorder that affects muscle coordination and leads to cognitive decline and dementia. It typically becomes noticeable in middle age • HD is the most common genetic cause of abnormal involuntary writhing movements called chorea and is much more common in people of Western European descent than in those from Asia or Africa Familiar
Direct gene diagnosis • Dynamic mutation disease caused by the expanded trinucleotide repeatof (CAG)n in HTT gene
Gene diagnosis of Duchenne muscular dystrophy (DMD) • X-linked recessive inheritance (OMIM 310200) • Severe muscular dystrophy leading to difficulty walking, breathing, and death • Most DMD patients become wheelchair-dependent early in life, and the gradual development of cardiac hypertrophy resulting in premature death in the first two or three decades of life Familiar
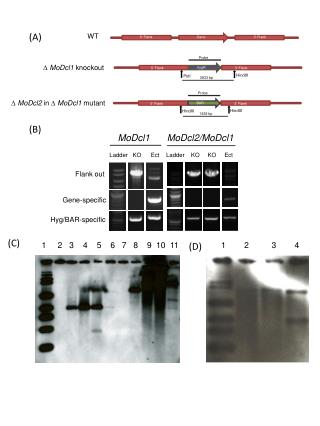
Direct gene diagnosis for gene deletion • There are 79 exons in DMD gene, which is the largest gene found in human genome • There are two regions prone to deletion as exon2~exon20 and exon44~exon53 in DMD gene, which is responsible for 65~70% of patients • That is, the deletion testing can detect the mutation of 65-70% of patients and render diagnosis
Indirect gene diagnosis for prenatal testing • 30~35% of probands do not result from large gene deletion, but small deletion, insertion or base substitution. The latters are difficult to detect since too much regions need be analyzed • In this case, prenatal testing is carried out by gene linkage analysis with STRs in DMD gene
Fetus 3 Father Mother Proband Fetus 1 Fetus 2 Female carrier Normal male Male patient
Notes in gene diagnosis • Relatively determined clinic diagnosis • Gene analysis in view ofpedigree • Pay attention to ethical issues • Correct understanding of the risk of gene testing Master
General procedures of gene diagnosis • Determining target gene based on symptomatic diagnosis, pedigree analysis and other laboratory tests • Determining the method for mutation analysis • Detection of the mutation of target gene in laboratory • Reporting the results of DNA testing and putting forward the interpretation to the finding
How to understand the report of gene diagnosis • Positive result: determining the location and property of the mutation, as well as the relationship with disorder occurrence • Negative result: it is failed to detect the mutation of target gene. In this case, the clinic diagnosis should not be excluded due to the limited detection rate and genetic heterogeneity Master
Prenatal gene diagnosis • Indications • Severe genetic disorders: lethal, untreatable and seriously reduced quality of life • Severe genetic disorders with delayed dominant inheritance • Severe genetic disorders with explicit etiology Master
Sample type • Chorionic villus: obtained during pregnant 6~9 weeks • Amniotic fluid: obtained during pregnant 16~22 weeks • Cord blood: obtained in pregnant ~28 weeks Master
The risk of prenatal gene diagnosis • The contamination of exogenous gene • The accuracy of clinic diagnosis of proband • The occurrence of novel germline mutation • The occurrence of gene recombination • The accuracy of pedigree analysis Master