Belarus
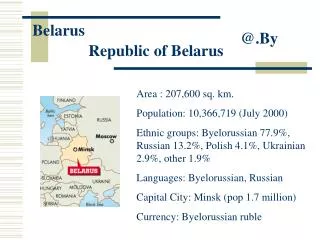
Belarus. @.By. Republic of Belarus. Area : 207,600 sq. km. Population: 10,366,719 (July 2000) Ethnic groups: Byelorussian 77.9%, Russian 13.2%, Polish 4.1%, Ukrainian 2.9%, other 1.9% Languages: Byelorussian, Russian Capital City: Minsk (pop 1.7 million) Currency: Byelorussian ruble.


Belarus
E N D
Presentation Transcript
Belarus @.By Republic of Belarus Area : 207,600 sq. km. Population: 10,366,719 (July 2000) Ethnic groups: Byelorussian 77.9%, Russian 13.2%, Polish 4.1%, Ukrainian 2.9%, other 1.9% Languages: Byelorussian, Russian Capital City: Minsk (pop 1.7 million) Currency: Byelorussian ruble
Belarus @.By Republic of Belarus
Belarus @.By Republic of Belarus Red Catholic church in Minsk
Belarus @.By Republic of Belarus Castle in the Mir Settlement, Minsk Region
Belarus @.By Republic of Belarus Farny Catholic church in Grodno
Belarus @.By Republic of Belarus Street in Grodno
Belarus @.By Republic of Belarus Grodno Dramatic theater
Belarus @.By Republic of Belarus Zubr (bison) In Belovezhskaja virgin forest
Dr. Serguey A Khoruzhik MD, Computed Tomography Unit, Grodno Regional Clinical Hospital, Grodno, Belarus CT Imaging of Radiotherapy Induced Pulmonary Changes Hammersmith Hospital, London, October 18th, 2001
1990 1994 1999 Number of new lung cancer cases 26 627 30 290 33 152 Incidence rates per 100 000 population 37,7 44,2 42,7 Cancer mortality rates per 100 000 population 29,5 31,3 34,5 Lung Cancer Statistics in Belarus
Lung Cancer Statistics in Belarus (continued) Distribution of new cancer cases according to the disease stage in 1999: I - 13,6%, II - 23,7%, III - 33,5%, IV - 20,2%, ? - 9,0% • Lung cancer treatment in 1999: • Surgery alone - 39,4 % • Chemotherapy alone or in combined regimens - 19,6% • Radiotherapy (RT) alone - 41,0%
Radiotherapy regimen Split-course (Sp-RT): • First RT stage: 28 Gy in 2 Gy fractions twice daily 5 days a week • 4 weeks of rest • Second RT stage: 30 in 1 Gy fractions twice daily 5 days a week
Computed tomography of the thorax Dynamic CT scans: • First CT - before RT • Second CT scan - before second RT stage • Follow-up CT scans - from 4 weeks to 1 year after RT To study: • Tumor response • Radiation-induced lung injury
Radiation-induced lung injury - timing • Before 3 months - acute (radiation pneumonitis) • Before 9 month - late (organizing) pneumonitis or fibrosis • 9-12 month - established fibrosis but... it still may evolve before 2 years • After 2 years - no any change usually observed
Radiation-induced lung injury - CT patterns (1) A homogeneous slight increase in attenuation, uniformly involving irradiated portion of the lung (2) Patchy consolidation within irradiated lung, not necessarily conforming to the shape of the portal (3) Discrete consolidation, conforming to the shape of the portal, but not uniformly outlining it (4) Solid consolidation, conforming and totally involving the irradiated region of the lung Libshitz HI et al. JCAT 1984; 8: 15-19
Radiation pneumonitis after first RT stage (35 patients) • Slight increase in attenuation - in 1 patient • Minimal patchy consolidation - in 1 Earliest radiation-induced lung injury was seen 4 weeks after 28 Gy delivered Khoruzhik SA et al. Proceedings of Republican Conference "Modern Diagnostic Technologies in Medicine", Minsk 2000. - p. 40
Radiation pneumonitis after first RT stage (continued) 4 weeks after 28 Gy Earliest radiation-induced diffusely increased attenuation in lung tissue
Radiation pneumonitis after first RT stage (continued) 4 weeks after 28 Gy Minimal patchy consolidation
Radiation pneumonitis after the end of RT (16 patients) • No radiation-induced lung injury were detected - in 5 • Slight increase in attenuation - 6 patients • Patchy consolidation - 2 patient • Discrete consolidation - 2 patients Pneumonitis was seen in 10 of 16 patients (63%) 4 to 11 weeks after Sp-RT Khoruzhik SA et al. Lung Cancer 2000; 29 (Supplement 1): 249
Radiation pneumonitis after the end of RT(continued) 8 weeks after RT Patchy consolidation in the left lung
Radiation pneumonitis after the end of RT(continued) 5 weeks after RT Discreet consolidation with clearly defined lateral margin and mediastinum border traction from the left
Radiation pneumonitis after the end of RT(continued) Other radiotherapy induced pulmonary changes seen before 3 months after RT: • Solid consolidation - 2 patients • Fluid collection in pleural cavity – 1 • Pleural thickening - 1 Khoruzhik SA et al. European Society of Thoracic Imaging 8th Annual Meeting, Salzburg 2000. - Final Program and Abstracts. - p. 69
Radiation pneumonitis after the end of RT (continued) 5 weeks after RT Both discrete and solid consolidations seen in the left lung
Radiation pneumonitis after the end of RT (continued) 4 weeks after RT Streaky densities in left near-mediastinum region along with minimal fluid accumulation in the main pleural fissure from the left
Evolution of radiation pneumonitis 3 to 8 months after RT (11 patients) In 8 patients who presented with pneumonitis initially: • Fibrosis starts to develop - in 5 patients • Pneumonitis changed it`s radiological appearance - in 3 In 3 patients who had no pneumonitis initially: • No radiation-induced lung injury was seen - in 1 • Pneumonitis developed - in 1 • Fibrosis starts to develop - in 1 patient KhoruzhikSA et al. International Conference on Non-Small Cell Lung Cancer, Bialystok 2001, Proceedings, p. 56
Evolution of radiation pneumonitis (continued) A B (A) Slight increase of lung attenuation from the right 4 weeks after RT. (B) 4 months later fibrosis starts to develop in the right lung. Gross tumor recurrence is seen from the left.
Late radiation changes in the lungs Radiation fibrosis 7 months after RT
Conclusions • Radiation pneumonitis might be seen on CT in more then half of patients treated with radiotherapy • Some changes in attenuation values of lung tissue may be seen as early as 4 weeks after 28 Gy • Radiation pneumonitis may change its radiological appearance and in most of cases evolve to fibrosis
Contact Dr. Serguey A. Khoruzhik MD, Computed Tomography, Grodno Regional Clinical Hospital, BLK 52, 230025 Grodno, Belarus Phone: + (375 152) 772156, 331320 khoruzhik@grsmi.unibel.by http://nld.unibel.by/e/personal/cv.htm