Perform and interpret Respiratory Function Tests
E N D
Presentation Transcript
Perform and interpret Respiratory Function Tests • Devangna Bhatia
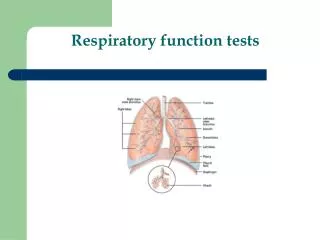
Lung Function Tests • Lung function tests measure: • How much air you can take into your lungs. This amount is compared to that of other people your age, height, and sex. This allows the doctor to see whether you're in the normal range. • How much air you can blow out of your lungs and how fast you can do it. • How well your lungs deliver oxygen to your blood. • The strength of your breathing muscles.
Peak flow meter Test This measures the fastest speed you can blow out. To do the test you take the biggest breath in that you can and then blow out as fast as you can. The results are useful in diagnosing asthma and deciding on its treatment.
Spirometry Test Most common lung function test Tests the amount (volume) and/or speed of air that can be inhaled and exhaled Results are displayed in pneumotachographs Helpful in assessing conditions, such as - asthma, COPD, pulmonary fibrosis and cystic fibrosis.
FEV1/FVC (FEV1%)= In healthy adults = 75–80%. Obstructive diseases (asthma, COPD, chronic bronchitis, emphysema) FEV1 is diminished because of increased airway resistance to expiratory flow and the FVC may be decreased (for instance by premature closure of airway in expiration). This generates a reduced value (<80%, often ~45%). In restrictive diseases (pulmonary fibrosis) the FEV1 and FVC are both reduced proportionally and the value may be normal or even increased as a result of decreased lung compliance. FEV1= Forced Expiratory Volume in 1 second. Expiration after max. inspiration. FVC= Forced Vital Capacity, volume of air that can forcibly be blown out after full inspiration, measured in liters.
Other values: FEF = Forced Expiratory Flow - flow/speed of air coming out of the lungs during the middle portion of a forced expiration. The usual intervals at which it is measured are 25%, 50% and 75% (FEF25, FEF50 and FEF75), or 25% and 50% of FVC FIF= Forced Inspiratory Flow - similar to FEF but measured during inspiration! PEF= Peak Expiratory Flow - the maximal flow/speed achieved during the maximally forced expiration initiated at full inspiration, measured in litres per minute. TV= Tidal volume - specific volume of air drawn into, and then expired out of, the lungs during normal tidal breathing. TLC= Total Lung Capacity - maximum volume of air present in the lungs
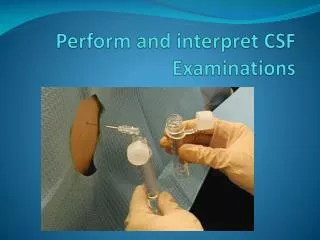
Blood Gas Test A.k.a - Arterial blood gas (ABG) It involves using a needle to draw blood from the radial artery OR the brachial artery OR the femoral artery. In rare cases, blood from veins can be used. Function of the test: Used to measure the CO2 and O2 levels blood Can also determine the acidity (pH) of the blood Aims: To make sure patients are receiving the right amount of O2, to check if the current treatment is effective and to measure the acid-base level in patients with heart or kidney failure, uncontrolled diabetes, severe infections or sleeping disorders.
Indications 1) If patients show signs of an oxygen/carbon dioxide or pH imbalance 2) Respiratory, kidney or metabolic disease and are suffering from respiratory distress 3) Have head or neck trauma 4) Have just undergone prolonged anaesthesia for procedures such as cardiac bypass or brain surgery. Preparation Generally, there are no special steps that patients must take in preparation for a blood gas test. The only exception applies to patients receiving oxygen therapy, whose oxygen concentration must not change during the 20 minutes before the test.
Pulse Oximeters Device to measure indirect oxygen saturation of patient’s blood. Very useful, since it is non-invasive. When used in hospitals, it is linked up to a medical monitor to allow continuous oxygenation. Portable devices are also available - use at home. Acceptable normal range: 95-100% Situations/locations where it’s highly useful: Intensive Care (ICU) Operating room and Recovery Emergency and hospital ward settings